Chapter 8
Local Anesthesia
One of the most important and challenging aspects of child behavior management is pain control. Children who undergo early painful experiences during dental procedures are likely to carry negative feelings toward dentistry into adulthood. Therefore, it is important that clinicians make every effort to minimize pain and discomfort during dental treatment. The successful children’s dentist must master the skill and art of administering the most painless injection possible. Some clinicians will try to avoid the administration of local anesthesia; however, this often results in poor clinical practice. As a consequence of no local anesthesia, a rubber dam will rarely or never be used and cavity preparations may be left shallow, with the end result far from optimal. In addition, there are times when an anticipated “minor” procedure becomes a major procedure and the patient is placed in a painful situation because of the lack of dental anesthesia.
On the other hand, one of the greatest single fears of the pediatric dental patient is “the needle” (Eichenbaum and Dunn 1971). Childhood fears emanate from many sources, and some can be extremely obscure. One possible cause of general dental anxiety may be previous exposure to invasive medical care in early childhood (Karjalainen et al. 2003). A recent review (Sokolowski et al. 2010) on needle phobia presented several publications suggesting that the fear of needles may result after a negative experience at a physician’s or dentist’s office. Many childhood fears are learned and may be the result of early childhood conditioning (i.e., “shots” administered from infancy). The average child will receive twenty-one vaccines in up to six to seven injections before the age of six. Children may not be voluntarily cooperative during these immunization procedures, and sometimes they may be physically restrained. Ost (1991) examined subjects with injection phobia, and showed that 56% could trace their fear back to negative conditioning from a health care experience. The mean age onset was eight years and often correlated with a first-time health care–related appointment. This study also determined that 24% of the subjects could trace their phobias to having seen another child, often a sibling, have a negative experience to needles.
As a consequence of these conflicting concerns—the dentist wanting to control pain with local anesthesia and the child fearing the pain of the needle—injection procedures present an almost constant challenge to the dentist’s skills. Thus the aims of this chapter, which covers an important aspect of behavior management, are (1) to discuss factors associated with administering injections and (2) to review the most commonly used local anesthetic techniques for children. The chapter will not present every type of local anesthesia, nor will it include detailed techniques. It will focus instead on the most commonly used injections, with an emphasis on how to administer local anesthesia with minimum pain and maximum effect.
Administration of Local Anesthesia
It is extremely important for the dentist to have an effective system for the administration of local anesthesia. Children are very sensitive to body language. Pediatric patients can detect uncertainty or hesitation, which can lead to difficulty. If the dentist’s approach, and that of the assistant, are not confident and well-timed, the child may easily sense their attitude and resist every effort that they make (see Communication in Chapter Six). Considerable skill is needed for administering local anesthesia to children while avoiding behavior problems. Some of the following clinical procedures, which have been developed over the years, are widely accepted and highly successful with children. Others, however, are debatable.
Preparation of Patient
Preparation of the patient prior to injection consists of two components: mental and physical.
Mental preparation begins with explaining the anesthesia administration process to the child in terminology that they can understand. The child may be sitting upright in a non-threatened position. Consider the following narrative:
“Today I’m going to put your tooth to sleep, wash some germs out of your tooth and fix your tooth and make it all better. When your tooth falls asleep your lip and tongue will feel fat and funny for a little while. You will not look funny or fat. You will just feel funny and fat.
To make your tooth fall asleep, I am going to use sleepy juice. Only your tooth will go to sleep, not you! The sleepy juice doesn’t taste so good, so as soon as I put it next to your tooth, I will wash it away with some water. Oh, and while I put the juice next to your tooth I will give you a little pinch. A pinch only hurts a little. Not a lot. Let’s pretend to do it. Not for real, just pretend. I’m going to show you everything I do so you can see how easy this is.”
The dentist asks the child to pinch her arm. Some children may hesitate, but after a little coaxing, they will happily proceed to pinch the dentist. At this point, the dentist may turn around and, with a smile, inform the accompanying parent that kids love this part of the procedure. During the pinch the dentist says: “That hurt me, but not a lot. It hurt very little. I do not need to cry for such a little pinch.”
The dentist now takes the child’s arm and gently pinches the skin. The slight amount of pain created will not upset most children, and the child has now learned an objective association for the expectation of the injection, “the pinch.” The dentist proceeds to gently pinch the cheek or gingiva adjacent to the tooth and immediately spray water, demonstrating the feeling of the intraoral pinch and subsequent washing away of the bitter sleepy juice. The dentist then says, “you are a good boy (or girl) and I am sure you can stand a little pinch like that.” An overwhelming majority of children will agree and will cooperate during the injection.
Chair Position
Some authors have suggested giving injections, particularly mandibular blocks, with the patient in a somewhat upright position, resulting in the patient’s mandible being approximately parallel to the floor and the clinician’s elbow close to the body. Most pediatric dentists prefer to deliver local anesthetics with the patient in a supine position (Figure 8-1). This is especially true for those using custom-made benches, as shown in Chapter Seventeen. The anatomical positions and injections are essentially the same. However, when the child is in the supine position, the mandible is at approximately a thirty-degree angle to the floor, and the clinician’s elbow will be high, with the arm nearly parallel to the floor. The patient is positioned with the head and heart parallel to the floor and the feet slightly elevated. Positioning the patient in this manner reduces the incidence of syncope that can occur as a result of increased anxiety. In addition, the patient’s sudden movements are more easily controlled.
Figure 8-1. Most pediatric dentists prefer to deliver local anesthetics with the patient in a supine position.
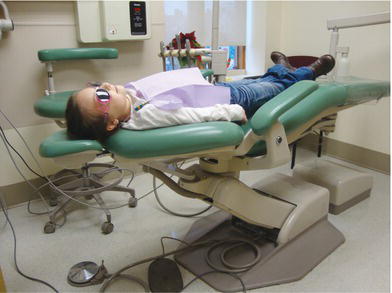
“It will be much easier for me to see your teeth if you lay back, so I will give you a ride and make the chair go back. Before I give you the pinch I will practice with you again and explain everything.” Repeating the explanation and pinch while the child is reclined may not be necessary with all children. In addition, if the child has been holding a hand mirror, it should be taken by the assistant with the promise that it will be shortly returned.
Assembling the Syringe
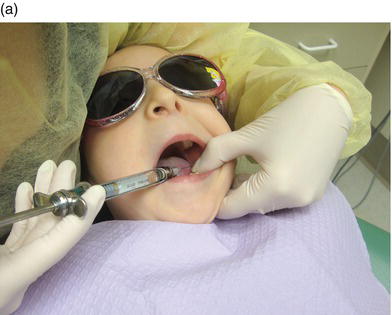
There is debate among clinicians as to whether the syringe and its components should be assembled in or out of view of the patient. The majority of pediatric dentists attempt to keep anesthetic syringes out of the sight of child patients (Starkey 1983). Proponents of assembling the syringe out of the patient’s sight assert that most children have developed a fear of the injection during prior visits to the pediatrician, and the slightest suspicion that they are getting an injection will set them off. This is especially true when told stories by older siblings and friends. In addition, the word “injection” has not been used. From the perspective of the child, he or she is simply getting a special pinch with sleepy juice. Introducing the syringe may complicate the process. In addition, some children may insist on removing the cap, thus exposing the needle. With proper technique the child need not ever see the syringe, which is always passed and held in blind spots, away from the patient’s view (Figure 8-2).
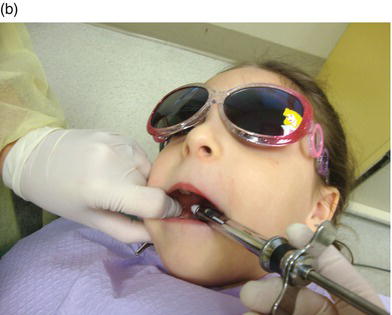
Figure 8-2. With the proper technique, the child need not ever see the syringe. It is always passed and held in blind spots, away from the patient’s view: under the child’s chin (a) and behind her head (b).
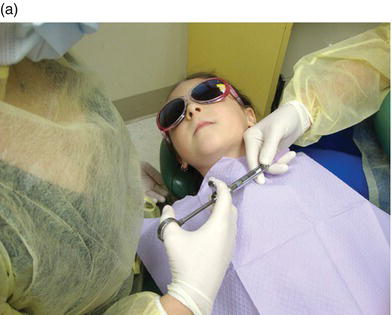
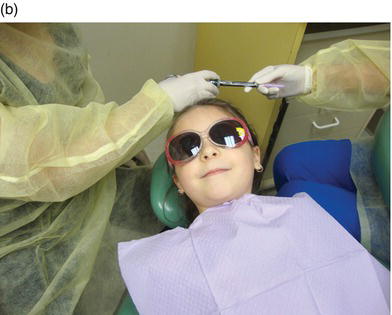
Proponents of assembling the syringe in view of the patient assert that doing so acts as a desensitization technique. The patient has the opportunity to touch and feel the individual, non-threatening components, reducing patient apprehension linked to prior injections. Clinicians who opt to show the syringe and its assembly in view of the patient may use the following narrative during syringe assembly.
“I’m going to make the tooth go to sleep and feel fat and funny with my sleepy juice. The sleepy juice is kept in this little glass jar.” (Allow the child to hold the cartridge.) “We place the jar in a special water sprayer,” (allow the child to hold the syringe) “and we place a plastic straw at the end of the water sprayer.” (Allow the child to hold the covered needle.)
Case 8.1, Discussion: Option 1. The dentist answers: “I am not giving you a shot, only a pinch.” The child suddenly moves and sees the syringe. He screams: “You are a liar! You are giving me a shot!” The boy manages to jump off the chair and run out of the room. A severe behavior problem ensued, and no amount of talk from the dentist made any difference to the child. The parents opted to switch to another dentist.
Option 2. The dentist answers: “As I told you before, I am going to give you a little pinch and put your tooth to sleep. Let’s pretend and pinch your cheek. See? It only hurts a little. Now let’s do it for real.” Jack answers: “How do you squirt the sleepy juice? Show it to me!” Dentist: “I am like a magician. Magicians never reveal their tricks. Maybe later, if you are a good patient, I will show you how I do it.” Most patients will not ask to see the syringe at the end of their treatment.
Option 3. The dentist answers: “Yes, I am going to give to you a shot, if that is what you want to call it. I know how to give a shot in a special way so that it does not hurt a lot, only a little. I don’t call it a shot, I call it a pinch.” Jack answers: “Show it to me!” The dentist shows Jack the covered syringe.
There are unlimited ways to successfully manage the above scenario. However, it is obvious that Option 1 is not one of them. The dentist lied to the child, thereby losing all credibility. In Option 2 the dentist never acknowledged that a shot would be given, yet she did not deny it either. She never stated that she would not be giving an injection. In many instances the child will receive the injection, never aware of it being a “shot”—just an uncomfortable pinch. The child was worried about the shot, not the pinch.
Jack had been adversely preconditioned to injections. His fear of the shot might have emanated from his experience with vaccinations. He disliked them and remembered crying. Although he returned from his first dental appointment excited and pleased, he became very anxious in anticipation of the next visit. He had he told his best friend in kindergarten how much fun the visit was. The friend responded by warning him of his next visit, when the dentist would give him a shot.
Administration of the Anesthetic
There are two important goals which one must accomplish during anesthetic administration; controlling and limiting movement of the patient’s head and body, and communicating with the patient to draw their attention away from the minor discomfort that may be felt during the injection process. Most clinicians prefer to keep the uncapped needle out of the patient’s line of sight. The child should not be asked to close her eyes, as that is usually a sign that something bad or painful is about to occur. In addition, pain perception may be enhanced with eyes closed. Instead, the assistant should pass the uncapped syringe behind the patient’s head (Figure 8-2). Once the assistant has handed the syringe to the dentist and has freed her hands, she positions them over the patient. The assistant should not actively restrain or even touch the child’s arms unless an attempt is made by the patient to lift her arms to reject treatment (Figure 8-3). Just touching the arms, as if to restrain, may cause apprehension in the child and, at that moment, the youngster may attempt to resist physically. Instead, the dental assistant should position her hands above the child’s hands to intercept any untoward movement.
Stabilization
Before placing the syringe in the mouth, the patient’s head should be stabilized. There are two basic positions for stabilizing the patient’s head. A behind-the-patient position is assumed for injecting the quadrants that are contralateral to the clinician’s favored hand and the anterior regions (i.e., right-handed clinicians injecting the left side, left-handed clinicians injecting the right side). The clinician stabilizes the patient’s head by supporting the head against the clinician’s body with the less favored hand and arm. He stabilizes the jaw by resting the fingers against the mandible for support and retraction of the lips and cheek.
Figure 8-3. The assistant should not actively restrain or even touch the child’s arms unless an attempt is made by the patient to lift her arms to reject treatment.
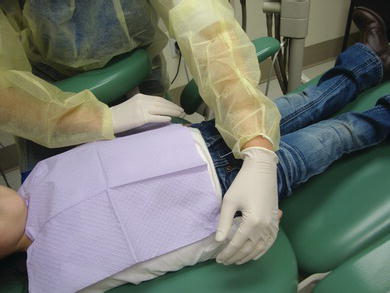
For injections on the same side as the clinician’s favored hand (i.e., right side for right-handed clinicians and left side for left-handed clinicians), the clinician assumes a more forward position—eight o’clock for right-handed clinicians, four o’clock for left-handed clinicians (Figure 8-4a and b). The clinician stabilizes the patient’s head and retracts the soft tissues with the fingers of the weaker hand resting on the bones of the maxilla and mandible.
Communication and Distraction
The clinician speaks with the patient in a reassuring manner during anesthesia administration. The subject matter can range from describing the process in child-friendly terminology, to praise, to storytelling, to singing, or, if the clinician is totally unimaginative, counting. Avoid words like shot, pain, hurt, and injection, and substitute words like cold, warm, weird, fat, and funny.
“The sleepy juice may feel real cold. So what I’ll do is count, and by the time I reach five the water will warm up.”
Two distraction techniques which may be employed are described. The child is asked to say “la, la, la, la” during the pinch. Not “ah, ah, ah, ah” but “la, la, la, la.” The patient also may be asked to raise the left or right leg during the injection. After depositing the desired amount of anesthetic, the syringe is withdrawn and the needle safely recapped.
Finally, the mouth is rinsed with water from the triple syringe, thus eliminating any blood from view: “Does the sleepy juice taste bitter? Let me rinse it away. Here is some water. Swallow the water. Wow, what a great helper you are.” Include a specific compliment: “You were very still.”
Figure 8-4. A behind-the-patient position is assumed for injecting the contralateral quadrants to the clinician’s favored hand (i.e., right-handed clinicians injecting the left side). The clinician stabilizes the patient’s head by supporting the head against the clinician’s body with the less favored hand and arm (a). For injections on the same side as the clinician’s favored hand (i.e., right side for right-handed clinicians), the clinician assumes a forward position of eight o’clock (b).
The assistant may return the hand mirror to the child. “Your tooth and cheek feel fat and funny, but you look the same.” The child looks in the mirror and sees that all appears normal, although the mouth does indeed feel strange.
Topical Anesthesia
Topical anesthetics are available in gel, liquid, ointment, patch, and pressurized spray forms. Topical anesthetics are effective to a depth of 2–3 mm and are limited in their effect to reduce the discomfort of the initial penetration of the needle into the mucosa: they offer little benefit when performing a mandibular block. The benefits of topical anesthetics may not be entirely pharmacological; a psychological advantage may ensue. A number of investigations have compared topical anesthetics with placebo intraorally with conflicting results(Meechan 2008). Some show positive benefits from the use of topical anesthesia before needle insertion and others do not. There is no evidence that topical anesthetics have any value in reducing the discomfort of regional block administrations such as inferior alveolar nerve block injections (Meechan 2002). In addition, their disadvantages include a disagreeable taste that may be a cause of patient discomfort, sometimes eliciting crying even before the actual injection is given. In addition, the length of application time may increase apprehension of the approaching procedure in the pediatric patient. The application duration time is a crucial factor governing effectiveness (beyond a placebo). The onset times of topical anesthetics range between thirty seconds and five minutes. Many clinicians do not wait for the anesthetic to take effect; they proceed with the injection almost immediately after placing the topical. In a survey on local anesthesia, Kohli and colleagues (2001) reported that two-thirds of the responding pediatric dentists waited a minute or less. In addition, most practitioners responded that patients disliked the taste, consistency, and the warm or burning sensation of the topical anesthetics. A majority of the respondents (86%) always used a topical anesthetic, while 9% sometimes used a topical anesthetic, 4% rarely used topical anesthetic, and 1% reported that they never used a topical anesthetic. Another reason for widespread use of topical may be the expectation of the accompanying parent, who presumes that its use is crucial for a painless injection. However, if a child has been referred due to behavior problems and the previous dentist used a topical, it might be best to avoid it.
Benzocaine is a very common topical anesthetic. It is not known to produce systemic toxicity in adults, but can produce local allergic reactions. However, the Food and Drug Administration announced in April 2011 that “Topical benzocaine sprays, gels, and liquids used as anesthesia during medical procedures and for analgesia from tooth and gum pain may cause methemoglobinemia, a rare but serious and potentially fatal condition.” Children younger than two years appear to be at particular risk. In the most severe cases, methemoglobinemia can result in death. Patients who develop methemoglobinemia may experience signs and symptoms such as pale gray- or blue-colored skin, lips and nail beds; headaches; lightheadedness; shortness of breath; fatigue; and rapid heart rate.
Application of Topical Anesthetic
Use a 2 × 2 gauze to dry the tissue and remove any gross debris around the site of needle penetration. The effectiveness of the topical will be enhanced when applied onto dry mucosa. Retract the lip to obtain adequate visibility during the injection. Wipe and dry the lip to make retraction easier. “I’m wiping your tooth and gums with my little washcloth to make sure everything is clean.”
Apply a small amount of topical only at the site of preparation, thus avoiding anesthetizing the pharyngeal tissues. The topical anesthetic should remain in contact with the soft tissue for one to two minutes. “Now I’m rubbing (goofy, cherry, bubble gum) tooth jelly next to your tooth. If it begins to feel too warm or goofy let me know and I’ll wash it away with the special water.”
Needle Selection
Controversy centers on both the gauge and length of needles. The most common gauges are 25-, 27-, and 30-gauge. Needles come in three lengths: long, short, and ultrashort. Gauge refers to the diameter of the lumen of the needle; the smaller the number, the greater the diameter of the lumen. For example, a 30-gauge needle has a smaller internal diameter than a 25-gauge needle. There is a trend among dentists toward the use of smaller-diameter needles on the assumption that they are less traumatic to the patient. Proponents of large gauges claim that these needles yield better aspiration and may cause less pain during initial penetration of the mucosa, believing that needles with a smaller diameter result in less injection pain than wider-diameter needles. Studies have refuted both points. Trapp and Davies (1980) and Delgado-Molina and colleagues (2003) reported that no significant differences existed in the ability to aspirate blood through 25-, 27-, and 30-gauge dental needles. On the contrary, the studies concluded that there is increased resistance to aspiration of blood through a thinner needle (e.g., 30-gauge) compared with a larger-diameter needle (e.g., 27- or 25-gauge). With regard to pain experienced by the patient, numerous studies have reported that patients are unable to differentiate among 23-, 25-, 27-, and 30-gauge needles—no significant differences in the perception of pain produced by them were reported (Reed et al. 2012).
Pain associated with dental anesthesia results mostly from the pressure caused when the anesthetic solution is injected into the mucosa—especially during the first few seconds—and less so from the actual needle penetration. The pressure produced is greater when using high gauges than with lower gauges. Needle deflection along the axis of the bevel and breakage must also be considered when choosing the gauge. The smaller the diameter of the needle, the more it deflects. Thirty-gauge needles deflect significantly, whereas 25-gauge needles essentially do not deflect at all. Likewise, 25-gauge needles very rarely, if ever, break during an intraoral injection. This is an important advantage when treating a child who may make sudden movements. Malamed et al. (2010) reported that 99% of the needles that do break are 30-gauge needles. In his classic textbook, The Handbook of Local Anesthesia, he recommends using the smallest gauge (largest diameter) needle available, which allows for easier aspiration, less deflection of the needle as it perforates the soft tissue, and less chance of breakage at the hub.
Traditionally, clinicians were taught to decide on the length in relation to the type of injection (block or infiltration), the size of the patient, and the thickness of the tissue. Although a long needle has been recommended for inferior alveolar injections, short needles seem to offer better control to the dentist dealing with children. The long needle recommendation relates to the possibility of needle fracture. Proponents of long needles claim that after a needle fracture, a portion of the needle is exposed for easy removal. However, in the event of this rare happenstance, fracture usually occurs at the hub. In addition, it is never recommended to insert a short needle to the hub. Thus, long needles seem to offer little advantage over short ones, and the authors recommend the short needle for all local anesthetics (excluding the intraligamental injection for which extra short needles are indicated) for children, regardless of their age and the type of injection.
Injection Rate
Another aspect of anesthetic technique that is often mentioned but has not been quantified is the injection rate. Most educators recommend slow injections because a rapidly expelled solution causes discomfort. But how slow is “slow?” Based on videotaped procedures, Starkey and Wright (1983) calculated that a slow injection takes approximately 45 seconds, using an entire 1.8 ml cartridge. In most pediatric cases, two-thirds of a cartridge are sufficient, the injection time being 30 seconds or less. Malamed (2012) recommends an injection time of one minute or more. However, the authors’ experience with pediatric patients is not to prolong the injection procedure. Kohli and coworkers (2001) reported in their survey of AAPD members that 56% of the respondents inject a cartridge in less than 30 seconds. The majority (89%) reported their injection time as being under one minute. A more recent study reported the average in/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


