Rotation Flaps
Introduction
Although rotation flaps are pivotal flaps in their movement, most are also advanced by stretching of the flap. Depending on the degree of stretching, the vector of greatest wound closure tension may be along a line extending from the base to the apex of the distal flap. When no advancement is used in movement of rotation flaps, the greatest wound closure tension is perpendicular across the distal border of the flap, not across the long length of the flap.1,2
Studies by Larrabee and Galt have demonstrated minimal benefit at the defect site of extending the arc of rotation flaps beyond 90° from the axis of the defect.2 This is to say, wound closure tension is not reduced at the defect site by increasing the pivotal movement of the flap by more than 90° from the axis of the defect. However, there is often some benefit in extending the incision to accommodate redraping of skin.
The secondary defect created by rotation flaps represents a transformation and a translocation of the primary defect.3 The surface area encompassed by the primary defect is equivalent to the surface area of the secondary defect.3 The geometry of the secondary defect is determined by the size of the flap. The larger the flap, the longer and narrower is the secondary defect. The narrower the width of the secondary defect, the less is the tension required to close the wound and the less is the secondary movement of tissue adjacent to the donor site. Another way of stating this is that the greater the length of the arc and thus the larger the flap, the less is the wound closure tension across the repair of the secondary defect.
Rotation flaps are best suited for repair of defects that are triangular. Design of the classic rotation flap is seen in Figure 7-1. A standing cutaneous deformity will develop at the base of the flap. A Burow triangle can be removed to facilitate repair of the donor site wound. A back cut4 at the base of the flap shifts the position of the pivotal point and changes the location of the standing cutaneous deformity.5–7 When a rotation flap is converted to a two-dimensional form, it appears as in Figure 7-2. As can be seen in the illustration, a problem encountered with rotation flaps is the unequal length of the flap’s border, labeled B in the drawing, compared with the width of the primary and secondary defects, labeled A in the drawing. A common method to equalize this discrepancy is to excise an equalizing Burow triangle at some point along the periphery of the curvilinear incision. The triangle’s base is equal in width to the width of the base of the defect, labeled C in Figure 7-2. Excision of the triangle of skin results in equalizing of the length of the two sides of the incision. An alternative solution to the management of the discrepancy in length of wound margins is to modify the movement of the flap from one that is purely pivotal to one that is both pivotal and advancement. By advancing the flap while at the same time rotating it around its pivotal point, the flap is stretched to equalize the discrepancy (Fig. 7-3). In so doing, the surgeon takes advantage of the distensibility (Fig. 7-4, side B) and the compressibility (Fig. 7-4, side A) of the skin along the wound margins. Repair is then accomplished by use of the principle of halving by suturing on the bias (Fig. 7-4C, D). This is accomplished by placing a suture to appose the two borders of the wound at the halfway point along the length of the flap. Succeeding sutures are placed in a manner that continues to equally divide the remaining distances along the flap’s border. An experienced surgeon will learn to suture on the bias from one end of the flap to the other without resorting to planned halving sutures.
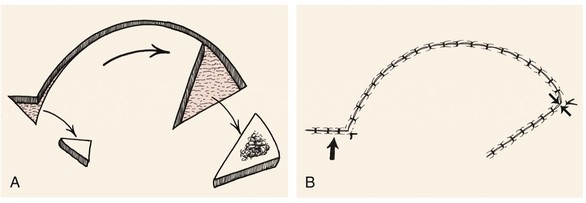
FIGURE 7-1 A, Rotation flap with excision of an equalizing Burow triangle. B, Opposing arrows indicate point of greatest wound closure tension. Large arrow indicates closure site of the equalizing Burow triangle excision.
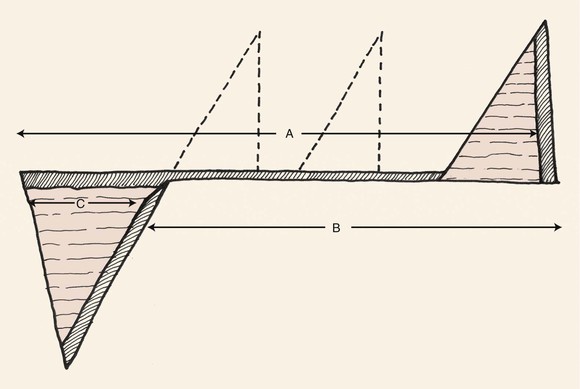
FIGURE 7-2 Rotation flap converted to two-dimensional form. Discrepancy between border of rotation flap (side B) and width of primary and secondary defects (side A) is equalized by excision of a triangle of skin (Burow triangle) at some point along curvilinear periphery of incision (side A) with base equal in width to maximum width of defect (side C).
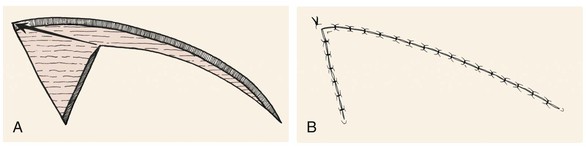
FIGURE 7-3 A, B, Need for excision of a Burow triangle is often avoided by advancement of distal tip of rotation flap and repair of wound by suturing on bias.
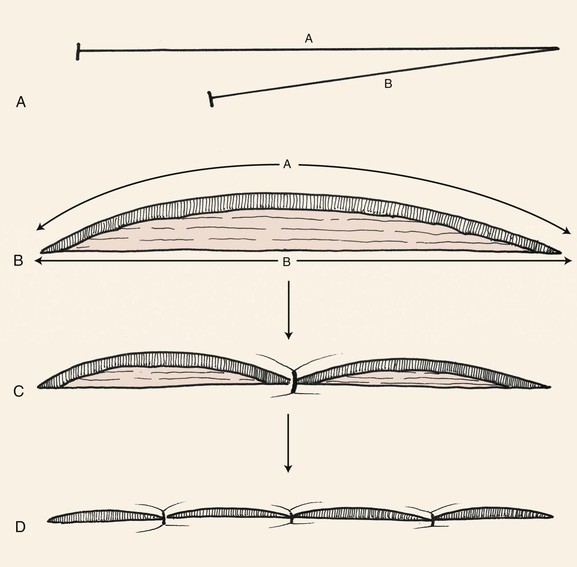
FIGURE 7-4 A, B, Surgeons take advantage of distensibility of side B and compressibility of side A to achieve wound closure without excision of an equalizing Burow triangle by advancing and stretching side B to reach most distal border of defect. C, D, Wound is repaired by principle of halving sutures.
As a general rule, in designing rotation flaps on the face, the length of the flap (Fig. 7-2, side B) should be four times the width of the base of the triangular defect (Fig. 7-2, side C). When this ratio is used, excision of an equalizing Burow triangle is usually not required. Undermining of the base of the flap along with its pivotal point enables advancement of the flap toward the defect during wound closure. Advancement reduces wound closure tension and often necessitates a smaller flap with less movement about its pivotal point than when the flap’s pedicle is not widely undermined and advanced. In addition to reducing the overall size of the flap, undermining limits the development of a standing cutaneous deformity by advancing a portion of the deformity peripherally away from the flap’s base.
Increasing the degree of undermining of the flap without lengthening the border of the flap does not significantly decrease wound closure tension. Likewise, enlarging the flap beyond the length of four times the width of the defect does not significantly decrease wound closure tension.8 When a single flap is used for wound repair, the arc of the flap may be adjusted for a number of considerations. For instance, the arc of the flap may be shortened to maintain the incision along or inside hair-bearing tissue. The arc may be extended more than four times the width of the defect when the defect is located in areas of limited skin mobility.
To avoid a standing cutaneous deformity at the base of a rotation flap used to repair a defect, the defect should ideally assume the configuration of an inverted triangle. The triangle should have the height-to-width proportion of 2 : 1 (Fig. 7-5). In addition, if the arc of rotation of the flap is to be a completely symmetric curve, the height of the triangular defect should be 0.5 to 1 times the radius of the curve of the flap (Fig. 7-6). To create the ideal condition for use of a rotation flap, the defect can be enlarged by removing normal tissue and converting the defect into a triangle with a height-to-width ratio of 2 : 1 (Fig. 7-7).9
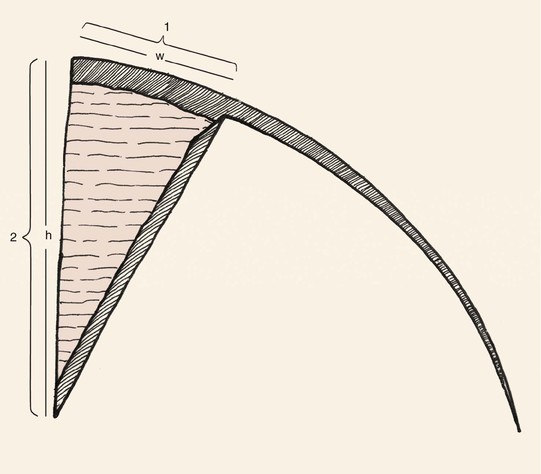
FIGURE 7-5 To minimize standing cutaneous deformity that develops at base of rotation flap, most ideal configuration of triangular defect has height-to-width ratio of 2 : 1.
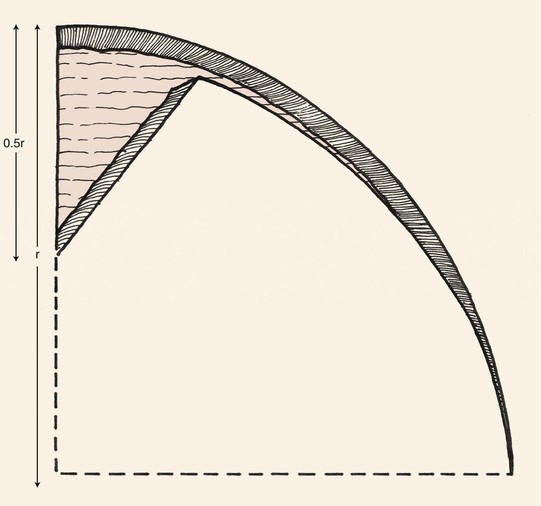
FIGURE 7-6 For symmetric rotation flap, height of triangular defect should be 0.5 to 1 times the radius of curvature of flap’s border.
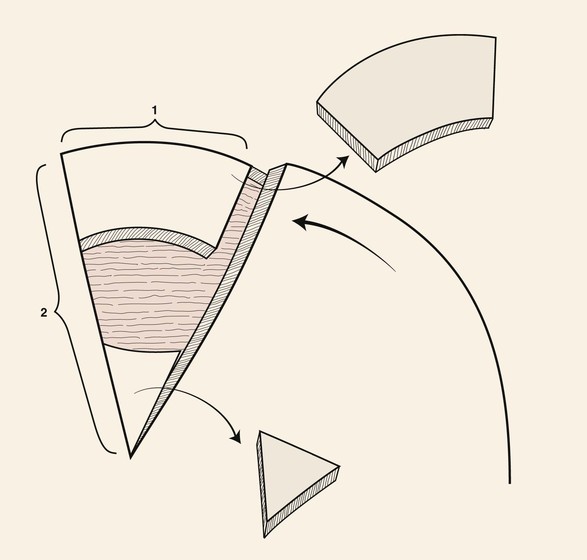
FIGURE 7-7 To create ideal condition for use of rotation flap, defect enlarged by removing normal tissue and converting defect into triangle with height-to-width ratio of 2 : 1.
There are several advantages of using rotation flaps. The flap has only two sides; as a result, the surgeon can sometimes position the arced incision in an aesthetic border. The flap is broad based, and therefore its vascularity tends to be reliable. There is great flexibility in design and positioning of the flap.10–12 Design of inferiorly based rotation flaps promotes lymphatic drainage and reduces flap congestion and edema. Similarly, arterial and venous disruptions may be minimized and sensory innervation may be maximized by appropriately positioning the base of the flap.
Rotation flaps should not be selected as a first option in situations in which design of the flap will necessitate placement of incisions that cross RSTLs or aesthetic borders at right angles. This will likely result in an inadequately camouflaged scar along a portion of the donor site. Rotation flaps are not a good choice to repair central upper cheek skin defects in men because hair-bearing skin of the sideburn is moved medially into the non–hair-bearing area of the cheek covering the malar eminence. Except for the dorsal nasal flap, rotation flaps are not often used in repair of nasal defects because donor site scars do not follow the boundaries separating the nasal aesthetic units. The skin of the nasal tip is inelastic, making the use of rotation flaps difficult. Small defects over the dorsum of the nose are best repaired with transposition flaps, such as a bilobe or rhombic flap. Furthermore, rotation flaps transferred from the cheek to the sidewall of the nose usually have an unacceptable result because of the necessary bridging of the flap across the nasofacial sulcus. This partially obliterates this important landmark. Similarly, rotation flaps from the cheek are inappropriate for reconstruction of lateral lip defects because the arc of the flap must extend across the melolabial fold and crease at right angles. The melolabial crease is a prominent aesthetic border, and incisions crossing it perpendicularly often create unsightly scars.
Applications
Scalp
Rotation flaps are the preferred method to repair most scalp defects with use of local tissue. Because of its spherical topography, the scalp accommodates curvilinear incisions well and the flaps can be constructed sufficiently large without the need to regard RSTLs or aesthetic borders. Rotation flaps are transferred by a pivotal motion rather than depending on stretching of tissue for movement as required by advancement flaps. Because of the inelasticity of scalp tissue, any movement of tissue by advancement is limited. Whenever possible, multiple rotation flaps are preferred to the use of a single flap for scalp reconstruction. Each flap is designed to pivot on an independent pivotal point. When two rotation flaps are used, the flaps may be designed to pivot in opposite directions, creating a T configuration of the wound repair. Most defects left after micrographic surgery are round or oval. When this configuration is present, it is best to use two flaps that pivot in the same direction, either clockwise or counterclockwise. Each flap is designed with an opposite orientation on either side of the defect. The two flaps are apposed with a Z-shaped repair. This type of repair is known as an O-Z repair. In designing a double rotation flap in an O-Z pattern, the optimum design for wound closure is an acute-angled flap with a length equal to four times the radius of the defect being closed. Use of more than one rotation flap is advantageous because it recruits scalp tissue for reconstruction from different locations and the burden of closing the secondary defect is shared by the number of flaps used. Two or three rotation flaps work best for reconstruction of scalp defects. When three flaps are used, each is responsible for repair of one-third of the surface area of the defect. Wound closure is accomplished by pivoting all three flaps in the same direction. Repair of the defect has the appearance of a pinwheel, and wound closure configuration resembles the closing of a camera lens.13
Face
Rotation flaps work extremely well in repair of cheek defects larger than 3 or 4 cm in the lower preauricular area, where recruitment of the upper posterior cervical skin is required for wound closure. The curvilinear incision is positioned juxtaposed to the earlobe and along the hairline of the postauricular scalp. If necessary, the incision extends along the border of the trapezius muscle. An incision in this area of the neck produces a favorable scar even though it does not follow RSTLs. A Z-plasty at the base of the flap often facilitates closure of the secondary defect without the need for excision of an equalizing (Burow) triangle. In cases in which patients use tobacco or have been irradiated in the region of the defect, cervical rotation flaps may be elevated beneath the superficial fascia and the platysmal muscle. This will enhance the vascularity of the flap.14
Nose: Dorsal Nasal Flap
The dorsal nasal flap is a modified rotation flap that recruits redundant skin from the glabella. The flap can be used to repair skin defects of the nasal tip, dorsum, and sidewall. Elliott15 detailed the banner and bilobe flaps for nasal repair, designing them as interpolated flaps that require inset. Rieger16 described the basic design of the dorsal nasal flap used currently. The flap uses the entire dorsal nasal skin to facilitate repair. Further refinements of the flap were offered by Rigg,17 who introduced the concept of limiting the area of nasal skin used for construction of the flap. He advocated a back cut of the flap toward the medial canthus. Marchac and Toth18 designed the flap with an axial vascular pattern by incorporating a constant branch of the angular artery in the pedicle. This enabled a longer descent of the glabellar back cut to the level of the medial canthus. The greater back cut facilitates flap transfer, reducing wound closure tension and distortion of the nostril margin.
The dorsal nasal flap enables the surgeon to repair caudal and midnasal defects measuring 2.5 cm in diameter or less with matching adjacent tissue. There is insufficient nasal skin to repair larger defects in this manner. The flap is ideally suited for elderly patients with skin defects located centrally on the tip. By necessity, the flap is designed with a large surface area to maximize tissue movement and to decrease wound closure tension at the donor site. Excessive cephalic rotation of the nasal tip and alae is prevented by the large size of the flap, which incorporates the majority of the remaining nasal skin. It is imperative to assess nasal skin laxity when use of the flap is being considered and to plan for some degree of secondary movement at the margins of the nasal alae and tip. Skin laxity in the glabella and dorsal nasal regions is best determined by the “pinch test.” This test consists of grasping the skin between the surgeon’s thumb and index finger and determining the degree of redundancy.19 For success, sufficient skin laxity is present when the surgeon can gather 1 or 2 cm of skin on the nasal bridge and glabella. Greater laxity is necessary as the size of the defect increases.
Commonly, the dorsal nasal flap is designed as a laterally based rotation flap with a back cut (Fig. 7-8). The pedicle is centered in the region of the medial canthus. A curvilinear line is drawn laterally from the defect to the junction of the cheek and the nose. From this point, the line is directed superiorly, passing 0.5 cm medial to the medial canthus and extending to the superior aspect of the glabella within a glabellar crease. Because the flap is transferred primarily by pivoting, the effective length of the flap diminishes progressively as the flap rotates about its pivotal point (medial canthus). The height of the flap and thus the arc of pivotal movement must be sufficient to compensate for this shortening. Supplemental flap height is gained from the glabellar extension. The higher the extension, the greater the height of the flap, and the easier it will be to close the primary defect. From the nasofrontal angle, the glabellar extension is approximately 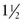 to 2 times the vertical height of the nasal defect. From the superior point of the glabellar extension, a line angles inferiorly toward the contralateral medial canthus, creating a 30° to 45° angle back cut. The back cut remains just superior to the level of the medial canthal tendon to protect the axial vessels from the angular artery located inferior to the tendon. In designing the flap, it is helpful to triangulate the defect by excising the standing cutaneous deformity in such a manner that the exci/>
to 2 times the vertical height of the nasal defect. From the superior point of the glabellar extension, a line angles inferiorly toward the contralateral medial canthus, creating a 30° to 45° angle back cut. The back cut remains just superior to the level of the medial canthal tendon to protect the axial vessels from the angular artery located inferior to the tendon. In designing the flap, it is helpful to triangulate the defect by excising the standing cutaneous deformity in such a manner that the exci/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


