Chapter 7
Periodontal Osseous Resective Surgery
INTRODUCTION
Successful treatment of periodontal disease can be achieved today through a number of surgical and nonsurgical procedures, each aiming to control infection and inflammation and reduce pocket depth. Periodontal surgery can still be considered a keystone in the treatment of periodontitis. Osseous resective surgery is defined as a means of changing the diseased tissue contour to reproduce a more physiologic anatomy. Knowledge of the pathogenetic mechanisms of the disease process and identification of the defect characteristics enable the clinician to select the appropriate surgical therapy to correct the deformity and establish a healthy environment.
The degree of destruction of periodontal tissues involving bone, periodontal ligament, cementum, and connective tissue depends on several factors such as type of bacteria, host response, teeth anatomy, hard and soft tissue biotypes, and so forth. Once the lesion has progressed apically, a discrepancy between the gingival margin and bone contour is established, resulting in a pocket. The characteristics of this pocket are determined by gingival biotype, morphology of the osseous crest, and teeth anatomy and location. As the inflammation caused by the periodonto-pathogens moves apically in the periodontal apparatus, a change in the anatomy of the zone takes place. If the bone is thick enough, a funnel-shaped defect is created while the surrounding bone not involved in the demineralization process maintains the gingival tissue in the same position. In the case of thin bone, such as buccal bone or interproximal bone between mandibular incisors, a horizontal pattern of resorption usually takes place, and depending on the soft tissue thickness, a recession or a suprabony pocket is formed.
INDICATIONS AND ENDPOINTS
The goal of osseous resective surgery is to establish minimal or physiologic probing depth and create a gingival contour compatible with good self-performed oral hygiene (Barrington, 1981). Even if regeneration of the lost periodontal apparatus is considered to be the ideal form of treatment, this can be successfully applied only to a limited number of defects according to their infraosseous depth and morphology. There is a clear indication in the literature that regenerative principles should be applied to those defects with an intra-osseous component greater than or equal to 4mm. Therefore, osseous resection is indicated in a number of clinical situations whenever the infra-osseous defect depth is in the 3-mm range or whenever a one-wall defect is present (Ochsenbein, 1986).
Bone re-contouring should be carried out to achieve the so-called positive architecture. This term refers to the physiologic morphology of the alveolar bone that is located in a more coronal position interproximally compared to the radicular buccal and palatal/lingual aspect of the teeth (Figure 7.1). The bone contour follows the cementoenamel junction of the teeth and may be more or less concave, according to the tooth type and genetic biotype (Becker et al., 1997). Therefore, the alveolar crest architecture would have a more pronounced scalloping around incisors and canines, while that toward the molar region would progress in a more flat profile (Figure 7.2).
In a healthy condition, the gingival margin follows the bone architecture so that a consistency between the two entities can be recorded (Matherson, 1988). This is considered during surgical correction of osseous defects to avoid excessive or inappropriate remodelling of the osseous crest. Another field of application for osseous resective surgery is in the case of pre-prosthetic applications. Exposing sound tooth structure, re-establishing a biologic space between alveolar bone and the restoration margin, or correcting an un-esthetic gingival contour can be achieved through osseous resective surgery. In those instances the surgical approach is best known as a crown lengthening procedure (Ingber et al., 1977).
PHYSIOLOGIC AND PATHOLOGIC ALVEOLAR BONE ANATOMY
Unaltered alveolar bone morphology is characterized by the following conditions:
- The interproximal bone peaks are located at a more coronal position compared to the buccal or palatal bone. This is identified as a positive architecture. A negative architecture is considered whenever, due to the effect of periodontal disease, the position of the interdental bone is apical to the one of the buccal or palatal/lingual side. A flat type of architecture is identified whenever interproximal and buccal or palatal bone contour lie on the same line. This can be an effect of periodontal disease or the result of a surgical treatment if an ideal osseous recontouring cannot be achieved.
- The buccal or palatal/lingual bone architecture follows the cementoenamel junction (CEJ) of the related tooth. Therefore, the concavity may be more or less accentuated according to the tooth anatomy. The bone crest appears to be more scalloped at the single-rooted teeth compared to the molars, which present a more flat contour.
- The interproximal bone anatomy reflects the position and root anatomy of the proximal teeth. In the anterior areas, because of the reduced interproximal embrasure and the more or less conical anatomy of the root of the adjacent teeth, this morphology has a knife-edge contour. On the contrary, in the molar area the embrasure is wider and the roots have a more complex anatomy with concavity and convexity leading to a flatter morphology.
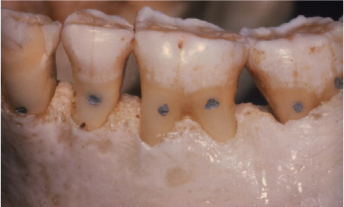
Figure 7.1. An example of positive architecture is shown in this human dry mandible. The buccal alveolar bone is apical to the interproximal crest. Courtesy of Dr. Hyman Smukler, Brookline, MA, USA.
These differences also have an impact from a histologic point of view. A thin knife edge interproximal area usually includes only cortical bone with minimal or no cancellous component (Figure 7.3). This is true, as demonstrated by Tal (1984), any time the distance between two adjacent roots is less than 3mm. In this case, around 1mm on each tooth side of the inter-radicular space is occupied by the periodontal ligament and only about 1mm is left for the alveolar crest that would be made of only cortical bone. In a molar area the embrasure is usually wider and therefore the inter-radicular bone may include both cortical and cancellous bone compartments (Figure 7.4). These above-mentioned anatomical features play a significant role in the pathogenesis of an infra-osseous defect. The inflammatory process, in the case of a narrow interproximal space with a mainly cortical interdental bone, usually determines a horizontal pattern of resorption. Conversely, in the case of a wider embrasure, with thicker cortical and cancellous bone, an infra-osseous defect is more likely to occur. (Figure 7.5)
- The buccal bone is usually thinner than the corresponding palatal or lingual bone according to the biotype. Root prominence, such as in the case of canines or the mesio-buccal root of the first maxillary molars, may determine a further reduction of the bone thickness predisposing to buccal bone dehiscences and fenestrations. Eliot and Bowers (1963), studying human skulls, reported an incidence of bone defects of about 20%. Fenestrations were more frequent in the maxilla, whereas dehiscences occurred at a higher rate in the mandible. The occurrence of one of these defects during periodontal surgery may complicate the osseous recontouring or may determine a significant change in the treatment goals. (Figure 7.6)
Figure 7.2. A, Surgical exposure of the alveolar crest around maxillary incisors during a crown lengthening procedure. Note how the bone architecture follows the CEJ outline, creating a scalloped morphology. B, A full-thickness flap of a maxillary posterior sextant for pocket elimination. The alveolar crest at the molar area runs with minimal scalloping according to the CEJ morphology.
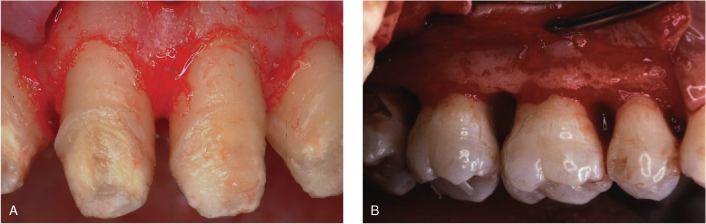
Figure 7.3. Histologic specimen from a monkey (Macaca fascicularis) showing the interproximal bone septum between the canine and incisor. The coronal part of the crest consists of only cortical bone, while cancellous bone becomes evident toward the middle third of the septum. Courtesy of Dr. Morris Ruben, Boston, MA, USA.
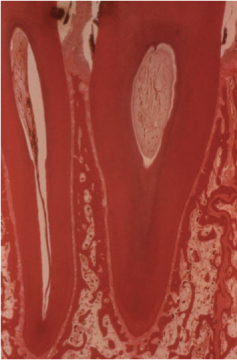
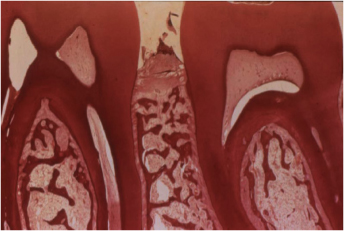
Figure 7.4. Histologic view of a block section taken from a non-human primate at the molar area. The interproximal distance is greater than 3mm and cortical and cancellous bone are well represented. Courtesy of Dr. Morris Ruben, Boston, MA, USA.
PRINCIPLES
The principles of osseous resective surgery, as it is conceived today, date back to Schluger (1949) and Friedman (1955). Those authors reported the need for eliminating osseous defects so that a consistency between osseous topography and gingival tissue could be re-established, but at a more apical level. According to the Glossary of Periodontal Terms, osseous resective surgery includes two different steps: (1) osteoplasty, the reshaping of the alveolar process to achieve a more physiologic form without removing supporting bone, and (2) ostectomy, the excision of bone or portion of a bone that is part of a periodontal defect and includes removal of supporting bone.
Figure 7.5. A large semi-circumferential three-wall defect around the mesio-lingual aspect of a mandibular first molar is exposed during surgery. The thickness of the lingual cortex and the inter-radicular distance account for the defect morphology.
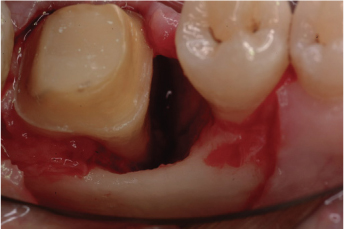
Figure 7.6. After flap elevation for pocket elimination, a dehiscence at the disto-buccal roots of the first molar has occurred. This finding greatly affects treatment strategy and approach. Courtesy of Dr. Alessandro Crea, Viterbo, Italy.
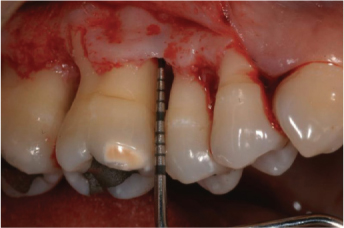
Figure 7.7. A thick buccal bony ledge can be observed after a full-thickness flap is raised. Bony ledges are often accompanied by infra-osseous defects and craters. Their elimination includes a generous osteoplasty to achieve a physiologic osseous anatomy.
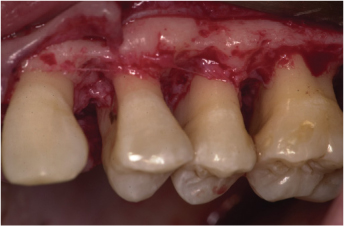
According to Friedman (1955) osteoplasty, is indicated in the case of buccal and/or interpoximal thick bony ledges (Figure 7.7), whereas ostectomy should be used to correct shallow interproximal defects such as craters and hemisepti. This resective approach has several limitations and side effects, and often the application of these principles may determine extraction of involved teeth or an unacceptable esthetic result for the patient. Those limitations have been discussed by Siebert (1976), who reported that the main side effect was the loss of attachment induced by the surgery. He also listed a series of factors that should be taken into account before selecting ostectomy as the surgical treatment modality. Those factors include the length and shape of the roots, location and dimension of the defect, width of investing bone, root prominence, and relationship between the intrabony defects and the adjacent teeth or anatomic structures (maxillary sinus, alveolar nerve, etc). For these reasons, osseous resection underwent a series of modifications through the years, aiming to reduce the amount of bone removal during surgery and thus decreasing the resulting attachment loss.
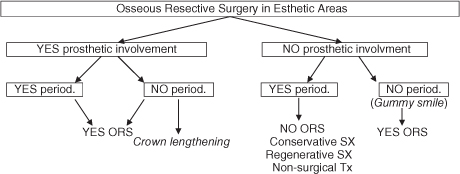
It should be stressed that osseous resective surgery must be used cautiously whenever an area with esthetic concern is involved in the surgical plan. To simplify the surgical approach to esthetic areas, the key to deciding whether or not to use resective surgery is related to the presence of or a need for a prosthetic involvement. In those cases, osseous resection may be ideal. When there is no prosthetic commitment, only limited and selected cases, including patients with a low smile line and with low esthetic expectations, may be appropriate for this technique (Figure 7.8, Tables 7.1, 7.2).
Table 7.1. Indications and contraindications to the surgical therapy in the case of anterior areas with no prosthetic involvement.
| Therapy | Indications | Notes |
| Non-surgical Therapy (SRP) | √ PPD > 4mm √ Horizontal defects |
Attention to thin biotypes for recessions |
| Access Surgery 1. Labial curtain 2. Papilla preservation |
√ PPD > 6mm √ Vertical defects √ Palatal defects |
Attention to the high smile |
| Osseous resective surgery | √ Rarely √ Low lip line √ Low esthetic expectation |
Attention to the post-op teeth sensitivity |
Table 7.2. Indications and contraindications to the surgical therapy in the case of anterior areas with prosthetic involvement.
| Therapy | Indications | Notes |
| Non-surgical Therapy (SRP) | √ PPD 4–5mm √ Horizontal defects |
Attention to thin biotypes for recessions |
| Access Surgery 1. Labial curtain 2. Papilla preservation |
√ Palatal defects √ Severe buccal recessions and extremely long crowns |
No if infrabony defect > 4mm Attention to the high smile |
| Osseous resective surgery | √ PPD > 4mm √ Medium and shallow intrabony defects |
Att.: Crown-to-root ratio Att: Clinical crown length |
TECHNIQUE
If osseous resective surgery is selected as a treatment option, several steps should be followed to correctly apply the technique.
Flap Design
Osseous resective surgery is usually coupled with an apical position of the flap. A para-marginal or sub-marginal incision using a 15 or 15C blade is carried out according to the soft tissue characteristics. A split or combined full-split flap may be used to expose the underlying alveolar bone. Releasing incisions may be necessary to gain better surgical visibility or to easily position the flap at the end of the surgery. Vertical incisions should always be carried out beyond the mucogingival line buccally and lingually, while the palatal aspect should be extended far enough to allow flap mobilization. The main concern in designing the flap is to provide an adequate vascular supply to the margin of the mobilized flap. Therefore, the apical portion of the flap must be wider than the coronal one and should include the major vessel of the area. For this reason vertical releasing incisions should go by the following general principles: (a) must be bevelled, (b) must be divergent toward the apex, (c) should be placed at the mesial and/or distal line angle of the last tooth included in the surgical area, and (d) radicular and interpoximal areas must be avoided due to the major blood supply.
Figure 7.8. Strategic use of resective surgery according to the presence of prosthetic involvement and the diagnosis of periodontal disease.
Degranulation and Root Debridement
Once the flap is reflected, degranulation of the soft tissue must be done with surgical curettes (Goldman-Fox n.2, n.3; Barnhardt n. 1/2, etc.) and with sonic/ultrasonic and hand scalers. Once the degranulation is completed and the defect can be identified thoroughly, the root surfaces should be cleaned and planed. Root preparation must be carried out with great care because it greatly influences the type of healing that will take place at the end of the surgical procedures. Polson and Caton described the factors influencing periodontal repair in a primate model (Polson and Caton, 1982). They showed that root surface alterations and contamination inhibit new connective tissue attachment and they stressed the importance of a complete root surface debridement for periodontal healing.
Identification and Measurement of the Defect
Once the surgical field is cleaned, the defect is measured and identified. This is critical in determining the amount of ostectomy and osteoplasty that is indicated. In addition, location of the furcation entrance, root trunk length, or anatomical characteristics of the surgical area must be identified.
Osteoplasty/Ostectomy
The first step is reducing the interpoximal bone thickness. This procedure, called grooving, determines the amount of osteoplasty that is needed at the radicular bone. In the case of a very thin buccal or palatal/lingual bone, a minimal or no osteoplasty is required. In other instances, a thick bony ledge may be present, requiring aggressive bone re-contouring. This is usually done with diamond coarse or carbide round burs mounted on a hand piece or a high speed hand piece under abundant water cooling irrigation (Figure 7.9). In the case of a bony ledge, a thin cortical layer may be encountered and if care is not taken during the osteoplasty a deep groove into the ledge may be produced as the bur drops into the cancellous bone once the resistance offered by the cortical bone is gone.
Figure 7.9. A diamond coarse round bur (Brassler, USA) can be used to perform osteoplasty. Due to its moderate cutting ability, compared to the carbide bur, it may be indicated whenever minimal osteoplasty must be done.
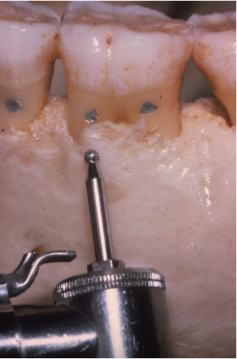
Figure 7.10. A back action (Rhodes 36–37 Hu-friedy, USA) is used in a dry mandible to demonstrate how to perform fine ostectomy. The blade of the instrument is placed on the radicular bone and moved backwards toward the root to eliminate the supporting bone involved in the defect.
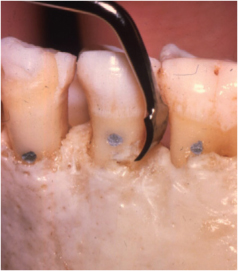
Figure 7.11. An osseous resective surgery bur kit (Brassler, USA), including different sized round burs made of diamond coarse and carbide. The end-cutting bur 957c-H207C is used to remove supporting bone around the tooth without damaging the root surface.

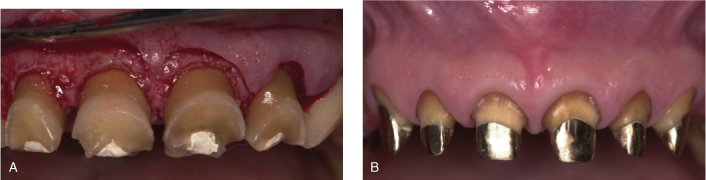
Figure 7.12. A, It may be useful to create a bone ledge in the esthetic area. In this case a crown lengthening has been done and a certain degree of crestal thickness has been intentionally achieved. B, Six months after surgery and before final prosthetic delivery. It is observable that the thickness of crest contributed to the creation of a thick and firm gingival unit.
As soon as the grooving is accomplished, a radicular blending must be done to produce a smooth and blended surface (also known as a sluice-way profile) to enhance flap adaptation. During this step a careful evaluation of root position and anatomy will reduce the risk of causing any fenestration or dehiscence. At this point ostectomy comes into play. One wall, craters, or other defects should be removed and interpoximal and radicular bone designed to achieve a positive architecture. Radicular bone removal is usually carried out with hand instruments. The Ochsenbain chisel (n.1 and 2) and back baction chisel (Rhodes 36–37) (Figure 7.10) are the most popular instruments used for this purpose. Rotary instruments also may be used, but great care must be taken so as to not damage the root while carrying out the ostectomy. Special burs with only an end-cutting head have been designed for this purpose and may be very useful in the interpoximal areas (Figure 7.11).
The more bone that is removed from the radicular or interpoximal areas, the thicker the alveolar margin; this phenomenon is known as ledging. The desired newly established alveolar bone morphology should have a knife-edged profile to allow better flap adaptation and reduce the chance of pocket re-formation. However, there are instances, such as during crown lengthening, in which a certain degree of margin thickness (ledge) is desirable to support soft tissue stability (Figure 7.12).
The last surgical step is the correction of the interdental area. The presence of a crater or a one-wall defect may be managed according to the location and anatomy of the tooth, either by a complete flattening of the crest or by a palatal/lingual approach. This can be done initially with a round bur and completed with bone files (Sugerman file, Kramer and Nevins, etc.). In addition, the removal of the so-called widow’s peak is critical. These peaks consist of residual bone left at the facial and palatal/lingual line angles of the teeth. During the healing process, the persistence of these formations may lead to a soft tissue bridging with a re-pocketing of the area. Their elimination is achieved with hand chisels (Wiedelstadt n.1 and n.2) that are run into the interdental area against the radicular surfaces.
Another important factor that influences the ability to achieve a positive architecture is the amount of the residual attachment apparatus. Performing osseous resection to eliminate pockets and defects should not jeopardize tooth stability. The length and anatomy of the roots and evaluation of the residual periodontal support help determine whether osseous resection may be the treatment of choice. The amount of bone that is removed during osseous surgery may vary according to the defect characteristics, the bone architecture, and the teeth morphology. Selipsky (1976) showed that an average of 0.6mm of support per tooth may be removed with osseous resective surgery. He concluded that although a significant amount of the total bone had to be removed, only a minimal amount of the removed portion would be the supporting apparatus. The increase of mobility following the surgical therapy is transitory and returns to the pre-operative level in about 12 months.
Suturing
Once the osseous re-contour is completed the flap is placed apical to the pre-operative margin. Its position may be apical to or at the osseous crest. In the first case, a small portion of exposed bone, with or without its periosteum, is left exposed. A vertical or horizontal periosteal mattress suture may be used to hold the flap in position; the sutures may be interrupted or continuous. The use of sling sutures is also recommended any time the lingual/palatal or buccal flap must be placed at a different level. A periodontal dressing may or may not be used according to the operator’s preference. In the authors’ experience it seems that periodontal eugenol-free dressing (Coe-pack) may be indicated any time the flap is positioned apical to the osseous crest to improve patient comfort during healing and reduce the risk for flap displacement during healing. However, it is important to remember that the use of a periodontal dressing may delay the healing process and therefore routine use is no longer justified.
MODIFICATIONS TO THE ORIGINAL SURGICAL APPROACH
Palatal Approach
Ochsenbein and Bohannan (1963) were the first to introduce a modification of the original protocols, by describing the palatal approach. This approach was based on the observation that, due to teeth location and alveolar bone anatomy, infraosseous defects in the maxillary arch were located mainly interproximally and palatally. The palatal approach has several advantages: (a) the presence of an abundant amount of keratinized tissue on the palatal side, (b) an increased thickness of the alveolar bone compared to the buccal aspect, (c) a wider embrasure area between the molars, facilitating the surgical access, and (d) the cleansing effect of the tongue in the post-operative period.
By using this approach a palatally inclined ramp is created with minimal ostectomy. The majority of the osteoplasty and ostectomy are carried out from the palatal aspect and only minimal osseous contour is done buccally, preserving furcation entrance integrity in the molars and reducing the amount of root exposure in esthetically sensitive areas. In 1964, the same authors classified the interproximal defects (craters) in four different entities. Class I defect was characterized by a 2-mm to 3-mm deep component with thick facial and palatal walls; Class II was 4mm to 5mm deep with thin facial and palatal walls; Class III more than 6mm deep with a sharp drop from the walls to a flat base, and Class IV, the least common situation, was characterized by a crater with a variable depth but extremely thin buccal and palatal walls. The authors associated a treatment option with each defect so that Class I could be managed only with palatal ramping, while Class II and III should be approached with both buccal and palatal ramping, and treatment of Class IV, although very unfavorable, included the elimination of buccal and palatal walls.
Lingual Approach
The same concept used in the maxilla was later introduced for the mandible. Tibbets et al. (1976) reported on how the mandibular molars and premolars should be approached from the lingual aspect. The rationale for this lies in the observation that molars and premolars have a lingual inclination (Wilson’s curve around 29 degrees for the molars and 9 degrees for the premolars) so that the entrance of the lingual furcation is located at a more apical position compared to the buccal one. Furthermore, the lingual bone is thicker compared to the buccal (Figure 7.13) and there is always an adequate amount of keratinized tissue on this side. As for the palatal approach, this technique should be used to minimize the amount of ostectomy carried out in the buccal area, preserving the furcation integrity and reducing the total amount of attachment loss (Figure 7.14 a–b).
Fiber Retention Osseous Resective Surgery
Another and more recent modification of the osseous resective sur/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


