7 Complications Following Implant-Prosthetic Rehabilitations in Edentulous Patients
P. Casentini, D. Wismeijer, M. Chiapasco, G.O. Gallucci
Implant treatment of edentulous patients has become a proven and very predictable treatment option. However, complications associated with implant treatment are not rare. Such complications cannot always be avoided, even if the clinician is well-trained and experienced; nor can long-term biological and mechanical complications always be predicted. For this reason, inserting implants implies the necessity of a strict aftercare regime. After the superstructure has been inserted, patients are expected to report back for periodic inspection of the peri-implant tissues and the superstructure itself. Once the clinician has evaluated the patient and a steady state has been reached, an individual patient-based recall regime can be installed. Systematic and continuous monitoring of the condition of the peri-implant tissues for disease is recommended. Implant superstructures also require continuous monitoring on an individual schedule. The following clinical and radiographic parameters should be evaluated at recall visits:
Peri-implant tissues
Plaque and calculus
Bleeding
Recession
Bone loss (probing)
Radiographs
Superstructures Occlusion/articulation
Wear of occlusal surface
Denture retention
Attachment loosening
Abutment status (with the superstructure removed)
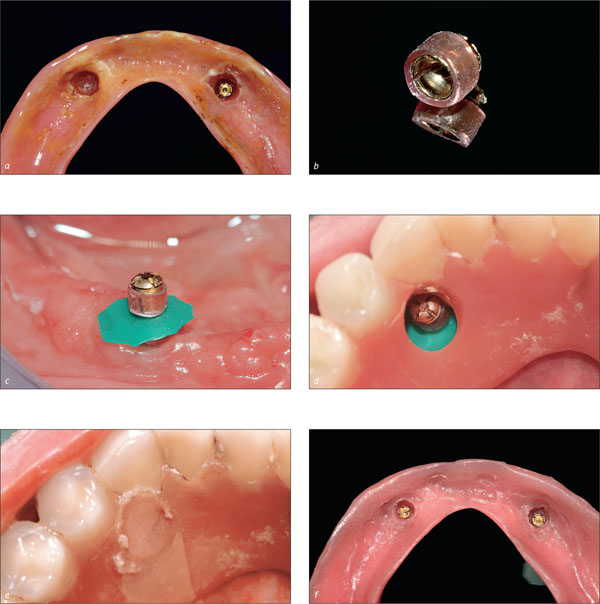
Regular monitoring of the peri-implant tissues is strongly recommended to facilitate early diagnosis of any peri-implant disease. Plaque and calculus must be removed, and sometimes patients will have to be remotivated. Bleeding on probing is evaluated, and probing depths around implants are recorded. Bone loss can be evaluated by probing and the evaluation of periapical radiographs. Such radiographs must be taken every two years, since bone loss can proceed rapidly even in apparently healthy patients. A routine recall visit of a patient treated with an implant-supported overdenture is presented in Figs 1a-f.
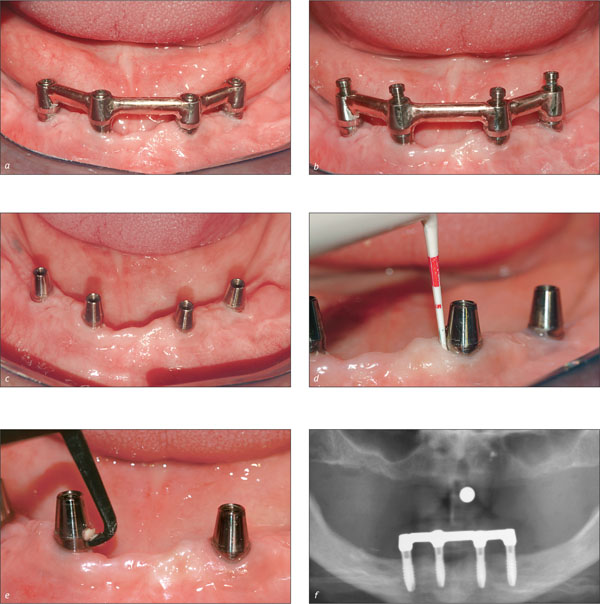
Figs 1a-f Scheduled follow-up of a patient wearing a mandibular implant-supported overdenture. The bar has been disconnected from the implants for cleaning. The peri-implant soft tissues are evaluated by probing with a plastic probe. Plaque and calculus, if present, are removed from the implant surface with plastic or Teflon manual or ultrasonic curettes. In this case, only limited plaque deposits were present, and the peri-implant tissues appeared healthy. A radiographic control confirms the absence of peri-implant bone loss.
The main types of complications are:
-
Soft-tissue complications
-
Maintenance problems
-
Failure of the retentive system
-
Fracture of the dental prosthesis
-
Bone loss due to peri-implant infection
-
Bone loss due to overload or absence of a passive fit
-
Implant fractures
-
Complications due to insufficient planning
7.1 Soft-Tissue Complications
Implants supporting overdentures must be surrounded by a cuff of keratinized tissue. While its presence may have little influence on the long-term prognosis of the implants, it does seem to play an important role for patient comfort. As described in Chapter 3, the absence of keratinized tissue can result in peri-implant pain, which can adversely affect the patient’s oral hygiene and in the long term even lead to the destruction of soft and hard tissues around the implants (Figs 2a-b and 3a-b). The treatment plan must therefore provide for inserting the implants such that the keratinized tissue heals in contact with the implants or keratinized tissue is in place after a grafting procedure. Hence, if no keratinized tissue is present, surgical correction by means of a tissue graft is often required (Fig 4a-g).
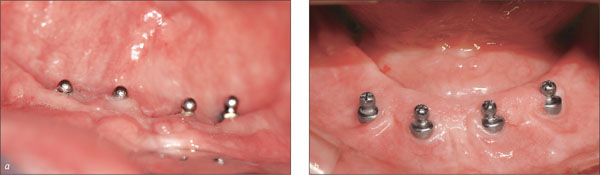
Figs 2a-b Lack of keratinized tissue around the ball attachments.
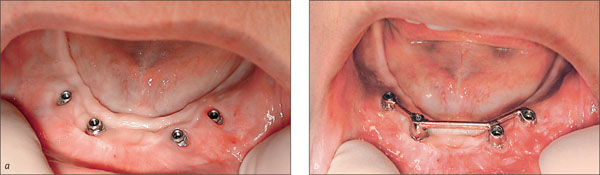
Figs 3a-b Absence of keratinized tissue around four implant abutments supporting a bar.
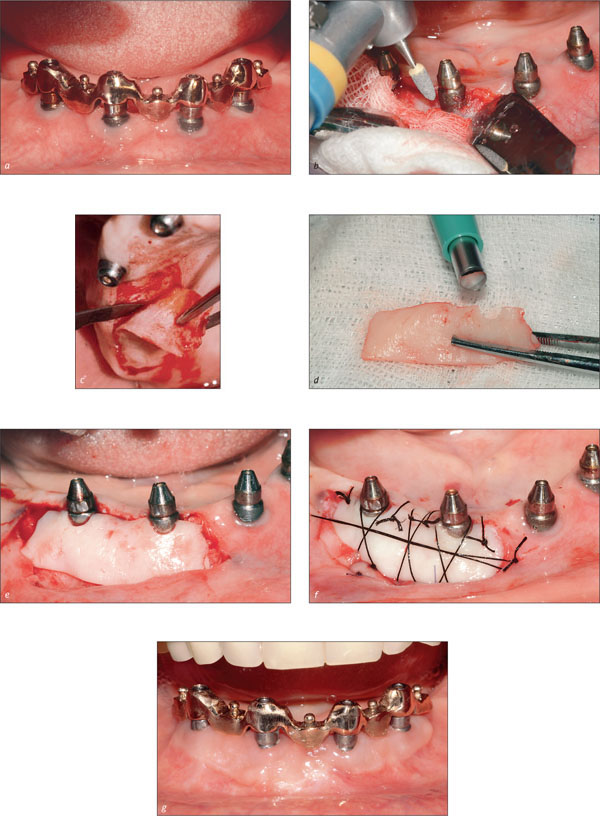
Figs 4a-g Absence of keratinized tissue around two of four implant abutments supporting a bar. The lack of keratinized tissue was associated with horizontal bone loss and exposure of the rough implant surface. The patient was complaining about painful oral hygiene procedures. A graft of keratinized tissue harvested from the palate was combined with remodeling of the implant surface to assist in oral hygiene.
Soft-tissue hyperplasia is sometimes observed beneath overdentures. There are several possible explanations for this phenomenon, including insufficient oral hygiene and insufficient space between the bar and tissue. A comprehensive treatment approach is based primarily on plaque control (Figs 5a-b). In some cases, however, the tissue will have to be reduced surgically and the design of the superstructure modified to prevent recurrence.
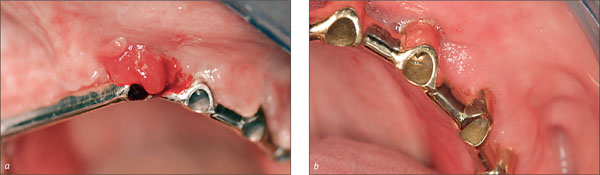
Figs 5a-b Hyperplasia of the soft tissues under a maxillary implant-supported overdenture, before and after treatment. There was no bone loss. Treatment consisted of removing the superstructure, cleaning the implant surfaces, and positioning a flap.
7.2 Maintenance-Related Issues
The design of a superstructure must always allow for adequate dental hygiene. The dental technician must design the superstructure to facilitate access with standard oral-hygiene tools. Sufficient interimplant distance must also be ensured. The pontic areas must be based on the ovate pontic design concept, and no inaccessible concave areas must be present. A ridge-lap design must be avoided wherever possible (Figs 6, 7a-b).
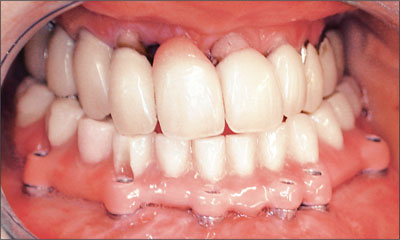
Fig 6 An extremely difficult-to-clean fixed dental prosthesis in an Angle class III patient with a poor periodontal status.
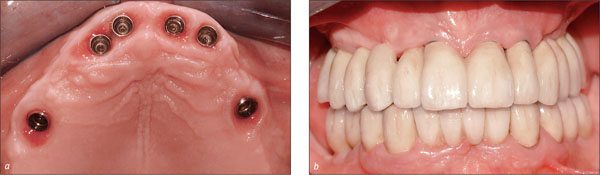
Figs 7a-b Too little distance between implants at the central and lateral right incisor sites may compromise the esthetic result and oral hygiene.
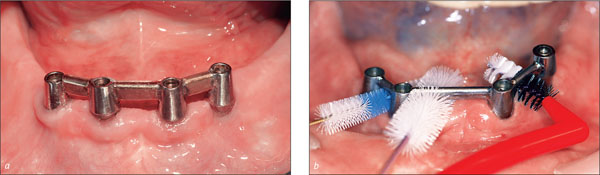
Figs 8a-b Adequately distributed and spaced implants are important for oral hygiene.
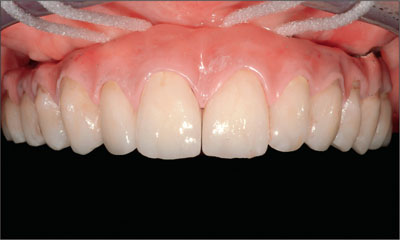
Fig 9 In complex rehabilitations, the framework design should always facilitate adequate oral hygiene.
7.3 Failure of the Retentive System
Over time, the retentive devices of an overdenture will exhibit wear due to use. When clips and matrices loosen, patients will complain about a loss of retention. However, specific instruments can be used to activate the retentive devices (Figs 10a-c).
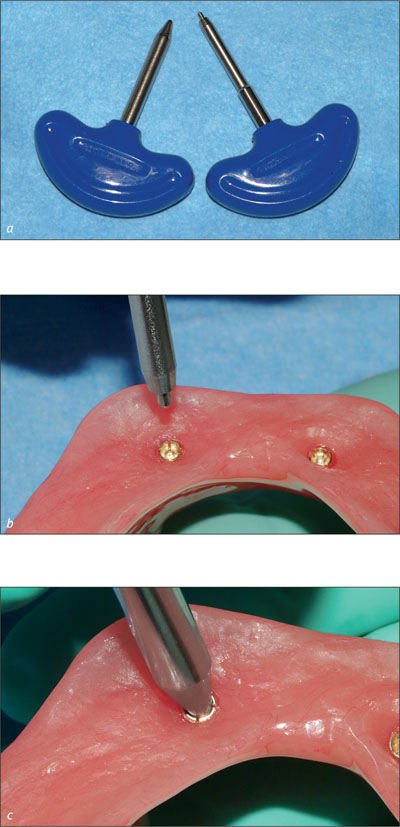
Figs 10a-c If necessary, gold matrices can be activated or deactivated to adapt their retention.
With the introduction of Locator attachments, retention has become adjustable to the patient’s needs by simply replacing the plastic matrices (Figs 11a-c).
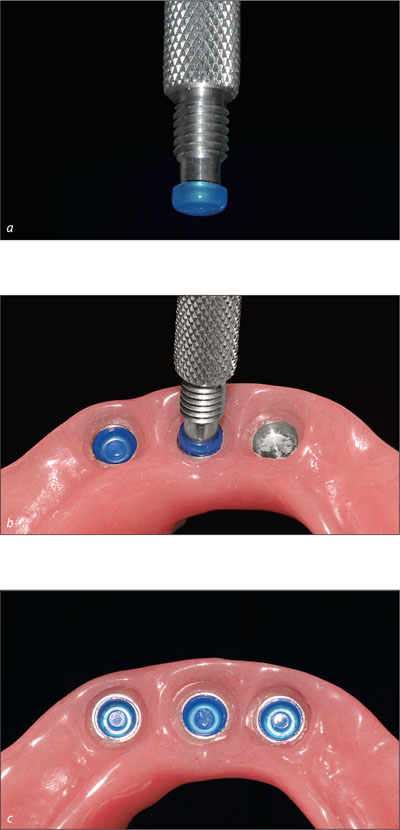
Figs 11a-c Locator retentive devices can be activated by replacing the plastic component of the matrix.
However, there comes a time when the matrices have to be replaced. In most cases, this can be implemented by relining procedure. The matrix is removed from the denture and an impression is made of the denture-bearing area including the abutments. In the dental laboratory, the new matrices are then polymerized into the denture. The matrices must be absolutely parallel, otherwise the clips in the matrix will be bent when the denture is inserted and their retention will deteriorate rapidly. The procedure can also be performed at chairside (Figs 12a-f ). However, this is not the preferred approach, as it is very difficult to position the matrices in parallel with this procedure. There is also a risk of resin polymerizing under the matrix, making it difficult if not impossible to remove the denture without causing damage to the soft tissues or to the denture itself. This approach should only be used in an emergency.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses