Chapter 6
Ultrasonic instrumentation technique
CHAPTER OBJECTIVES
- On completion of this chapter, the student will be able to:
- Demonstrate the basic principles of ultrasonic instrumentation technique.
- Explain the relationship between each instrumentation technique variable and the removal of deposits and root substance.
- Identify infection control procedures, which will minimize cross-contamination by the aerosol generated during ultrasonic instrumentation.
- Justify the staged approach to ultrasonic periodontal instrumentation.
Manual and ultrasonic instrumentation share the common objective of thorough disruption and removal of biofilm and calculus deposits without over-instrumentation of the root surface; however, the mechanisms by which each instrumentation method achieves this objective significantly differ, are inherent to the design of each instrument, and influence the instrumentation technique utilized.
Hand scaling instruments are designed to mechanically break the bond between the deposit and the tooth at the tooth–deposit interface by manually stroking a bladed cutting edge across the tooth surface (Lea and Walmsley, 2009). As presented in Chapter 3, ultrasonic scaling instruments are designed to ablate and disrupt deposits by vibratory and biophysical forces produced by a blunt metal tip oscillating at a high frequency (Walmsley et al., 1984; Khambay and Walmsley, 1999).
While ultrasonic and manual instrumentation methods are equally effective in removing deposits and improving and maintaining periodontal health as measured by reduction in clinical parameters (BOP, PD, CAL) (Chapter 2), ultrasonic instrumentation is less damaging to the root surface than hand instrumentation (Ritz et al., 1991; Dragoo, 1992; Jacobson et al., 1994; Busslinger et al., 2001; Schmidlin et al., 2001; Kawashima et al., 2007). However, the amount of root substance lost during ultrasonic instrumentation is technique-dependent (Box 6.1).
Box 6.1 Key point
Both the effectiveness of deposit removal and the amount of root surface lost during ultrasonic instrumentation are technique-dependent!
In order to accomplish the objectives of periodontal debridement by means of ultrasonic mechanisms of action, it is prudent for the clinician to have a solid understanding of the ultrasonic instrumentation technique and the variables that influence both deposit removal and root substance loss.
Ultrasonic instrumentation: Principles of technique
A significant error commonly made during ultrasonic debridement is the implementation of principles of manual instrumentation, with clinicians inappropriately utilizing the ultrasonic instrument as a “hand scaler with power.” Such misapplication of the ultrasonic scaling instrument is largely due to a lack of instructional resources specific to ultrasonic instrumentation theory and technique compounded by training curricula historically grounded in hand (manual) instrumentation.
The principles of technique for ultrasonic instrumentation are summarized and differentiated from the principles of technique for manual instrumentation in Table 6.1.
Table 6.1 Comparison of principles: techniques of periodontal instrumentation
| Principle | Ultrasonic instrumentation | Hand instrumentation |
| Adaptation | Adapt any surface of the active tip
|
Adapt lateral surface of toe/tip
|
| Angulation | 0–15° to tooth surface | 45–90° to tooth surface |
| Lateral pressure | Light pressure applied to maintain contact with tooth | Moderate pressure applied to engage cutting edge |
| Working Stroke | Constant and varied in direction | Intermittent and apico-coronal in direction |
| Insertion | At gingival margin or outer edge of deposit | Below deposit |
| Grasp | Light standard pen | Firm modified pen |
| Fulcrum | Established at a distance from treatment site for stabilization | Established in immediate treatment area to leverage working stroke |
Adaptation
The stroke pattern produced by the oscillating ultrasonic tip influences instrumentation technique, specifically the adaptation of the tip to the tooth.
Contrary to popular belief, both piezoelectric and magnetostrictive instruments produce an elliptical stroke pattern (Chapter 3), which allows debridement to be accomplished by adapting any surface of the oscillating tip to the tooth. The ability to utilize any surface of the tip (back, face, or lateral surfaces) facilitates a greater degree of contact between the active area and treatment surface, and thus, a more efficient and predictable debridement. A greater degree of contact results when the shape of the active tip conforms to the anatomy of the treatment surface (Figure 6.1).
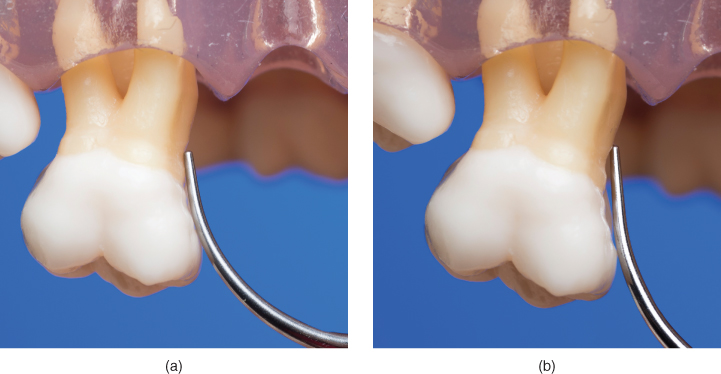
Figure 6.1 Adaptation of the back of a tip to the mesial concavity of tooth #3 (FDI 16). The convex arc of the curved tip (a) conforms to the concave anatomy of the tooth surface, whereas adaptation of a straight tip (b) lacks conformity, leaving a gap between the tip and tooth surface
Achieving a greater degree of contact is dependent upon not just the shape of the tip utilized, but more precisely, which surface of the tip is adapted and the manner in which the surface is adapted. Preferably, the surface of the tip that best conforms to the anatomy of the treatment surface should be utilized; however, at some treatment sites, this will not be possible. Alternatively then, the tip surface most readily available to the treatment surface can and should be used (Figure 6.2).
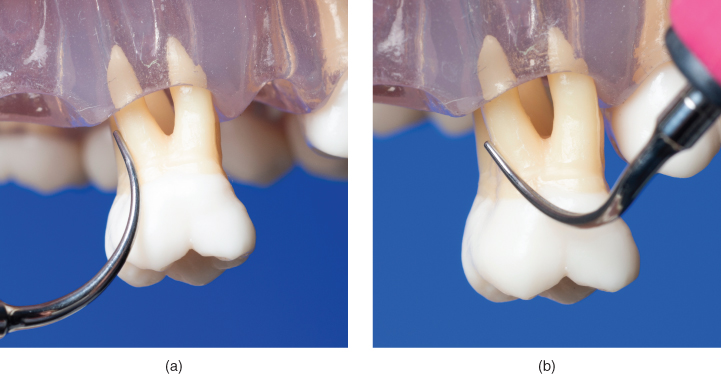
Figure 6.2 In a distal concavity, (a) adaptation of the convex back of the tip is ideal, but impossible to achieve; as an alternative, (b) the lateral surface of the tip is adapted
The preferred surface of the ultrasonic tip may be adapted to the tooth using several orientations: vertical (parallel) adaptation, horizontal (perpendicular) adaptation, and traditional oblique adaptation. Indications for use of each of these orientations are designated in Table 6.2.
- Vertical (parallel) adaptation
Vertical adaptation positions the active area of the ultrasonic tip parallel to the long axis of the tooth, with the point of the tip directed toward the base of the pocket (Figure 6.3). This is the same orientation used during periodontal probing (Figure 6.4).
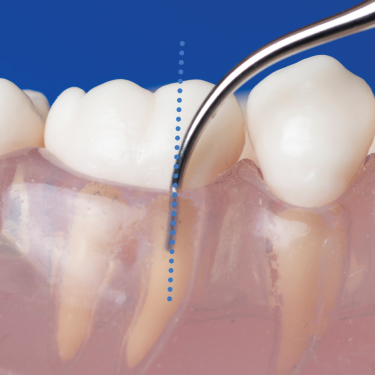
Figure 6.3 Vertical adaptation of the tip. Tip is positioned parallel to the long axis of the tooth with point directed toward the base of the pocket
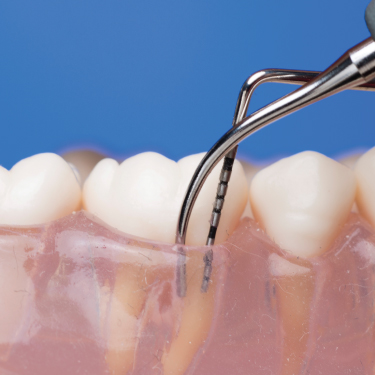
Figure 6.4 Vertical adaptation of an ultrasonic tip is similar to the adaptation of periodontal probe
Vertical adaptation is the primary and preferred approach to be used during ultrasonic debridement for several reasons:
- As accomplished during periodontal probing, vertical orientation facilitates the most direct access to the base of deeper pockets, increasing the predictability of the active area of the tip reaching the full depth of the treatment site (Figure 6.5).
- The extent of biofilm removed by cavitation and microstreaming may be increased with vertical adaptation to the tooth. Walmsley et al (1988) demonstrated that vertical adaptation of the tip resulted in an eightfold increase in biofilm removal, compared to a sixfold increase in biofilm removal when the tip was adapted in the more traditional oblique orientation (Figures 6.6a,b).
- Vertical orientation favors easy adaptation of ANY surface of the tip to any surface of the tooth. From this orientation, the clinician can readily adapt the preferred tip surface to the tooth with minimal repositioning required (Figure 6.7).
- On concave and convex tooth surfaces, positioning the tip parallel to the surface yields contact of a greater portion of the active tip area (2–3 mm vs 1–2 mm if positioned obliquely), maximizing the surface area debrided with each stroke and requiring fewer strokes per treatment surface (Figure 6.8).
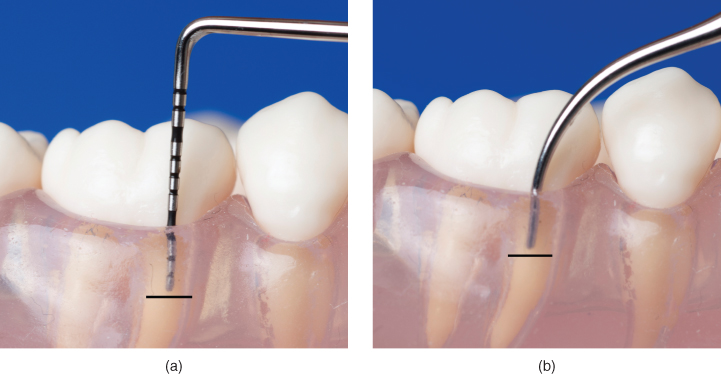
Figure 6.5 Vertical adaptation facilitates direct access to the base of the pocket during (a) periodontal probing and (b) ultrasonic instrumentation

Figure 6.6 Extent of plaque removal by tip and cavitational activity resulting from (a) vertical adaptation of the tip compared to (b) oblique adaptation of the tip. The direction of water flow is indicated by arrows.
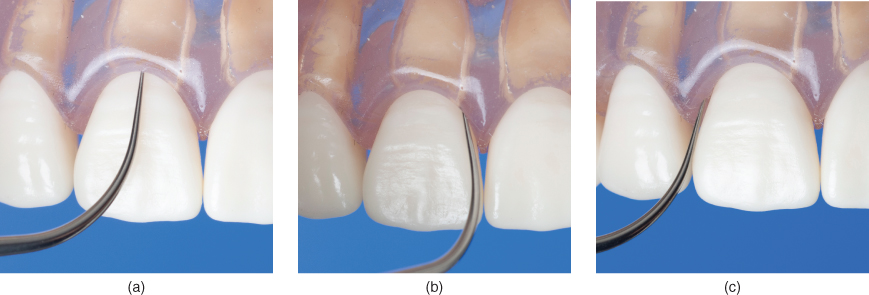
Figure 6.7 From vertical adaptation, the tip can be readily adapted to all tooth surfaces, (a) facial or lingual, (b) mesial, and (c) distal, without changing fulcrum or operator position
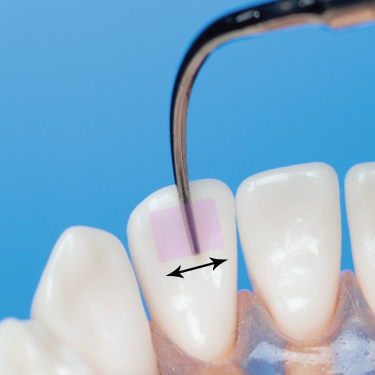
Figure 6.8 On a concave surface, vertical adaptation of the tip allows a greater portion of the active area to contact the tooth, increasing the surface area debrided (shaded area) with each stroke; arrow indicates direction of working stroke
- B. Horizontal (perpendicular) adaptation
Horizontal adaptation, which may also be described as “perpendicular” adaptation, is used primarily for instrumentation in the interproximal space (Figure 6.9). Horizontal adaptation positions the active area of the tip perpendicular, or in a horizontal orientation, to the long axis of the tooth, facilitating use of the BACK and FACE of the active tip.
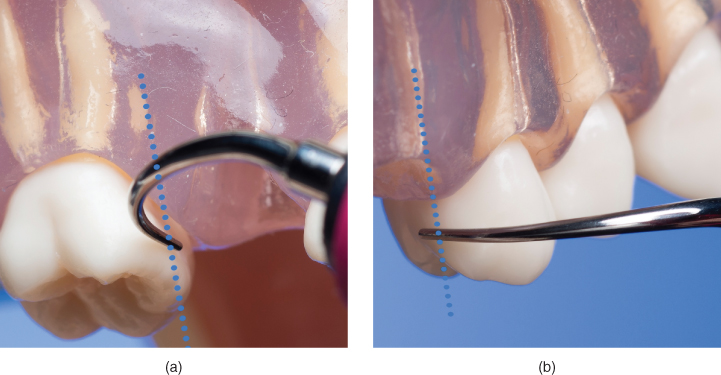
Figure 6.9 Horizontal adaptation of the tip. Tip position is perpendicular to the long axis of the tooth and facilitates use of (a) the back and (b) the face of the tip on interproximal coronal surfaces
Horizontal adaptation to the interproximal surfaces affords the clinician an easier and more ergonomic transition to and from the primary position of vertical adaptation than does traditional oblique adaptation. This transition is fully described in Chapter 7, General Principles of Instrumentation Sequencing.
- C. Oblique adaptation
Oblique adaptation positions the active area of the LATERAL surface of the tip in an oblique orientation to the long axis of the tooth (Figure 6.10). This is the same orientation used with bladed instruments, such as curettes and sickle scalers.
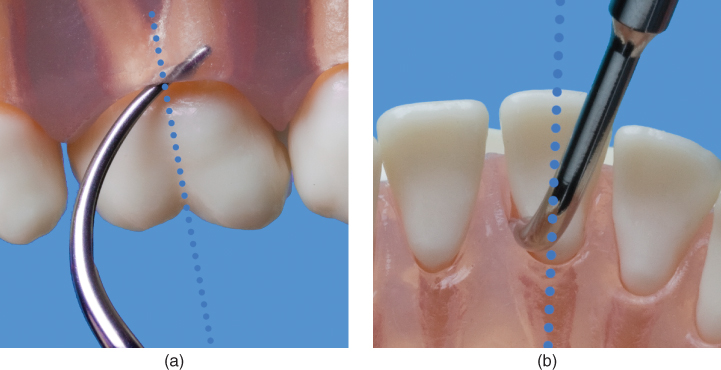
Figure 6.10 (a,b) Oblique adaptation of the tip. Tip position is oblique to the long axis of the tooth to facilitate adaptation of a lateral surface to the tooth
Use of oblique adaptation is one of the common misapplications of the ultrasonic instrument alluded to at the beginning of this chapter. Oblique adaptation is necessary during manual instrumentation in order to keep the cutting edge, located on a lateral surface of the curette or sickle, in contact with the tooth and in a position that enables the clinician to stroke the cutting edge in a direction that will break the bond between the deposit and the tooth. In other words, oblique adaptation is inherent to the mechanism of removal for which hand instruments are designed.
Table 6.2 Ultrasonic instrumentation adaptation techniques
| Image | Adaptation technique | Description | Indication for use |
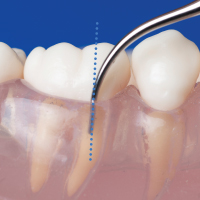 |
Vertical (Parallel) | Active area of tip is parallel to long axis of tooth, with point of tip directed apically, toward base of the pocket | Instrumentation of all subgingival and supragingival surfaces (excluding interproximal spaces) using any surface of the tip |
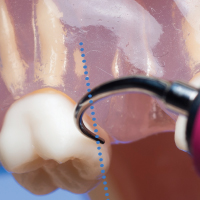 |
Horizontal (Perpendicular) | Active area of tip is perpendicular to the long axis of the tooth | Instrumentation of interproximal space using back or face of the tip |
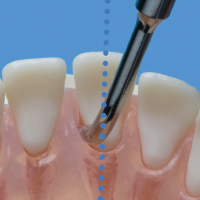 |
Oblique | Active area of a lateral surface is oblique to the long axis of the tooth | Manual instrumentation; not recommended by authors for ultrasonic instrumentation |
As ultrasonic instruments utilize a very different mechanism of deposit removal, oblique adaptation is neither indicated nor recommended by these authors, as it imposes several limitations to implementing an effective and efficient debridement:
- Oblique adaptation limits the clinician to utilizing a lateral surface of the tip.
- Depending on tip design, the lateral surface may not be the surface that best conforms to the anatomy of the treatment site, thereby risking inadequate contact for thorough biofilm debridement.
- The lateral surface may not be readily available to the treatment site, thereby requiring more frequent changes in operator position in order to adapt it, as is necessary when performing manual instrumentation.
- Oblique orientation of the tip may result in less biofilm being removed by cavitation and microstreaming compared to vertical orientation (sixfold vs eightfold), as illustrated previously in Figure 6.6 (Walmsley et al., 1988).
- Oblique orientation may hinder access of the active area to the base of deeper pockets, lessening the predictability of thorough debridement (Figure 6.11).
- Oblique adaptation of the lateral surface limits contact of the active area to the terminal 1–2 mm of the tip on any given surface, minimizing the surface area debrided with each stroke and requiring more strokes per treatment surface (Figure 6.12).
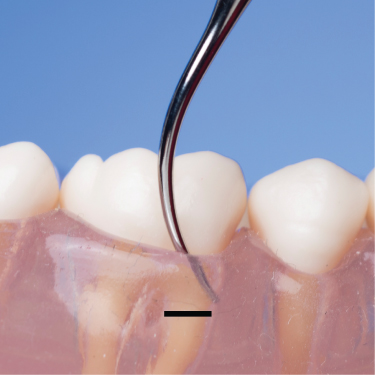
Figure 6.11 Direct access to the base of the pocket is hindered by oblique adaptation of the tip
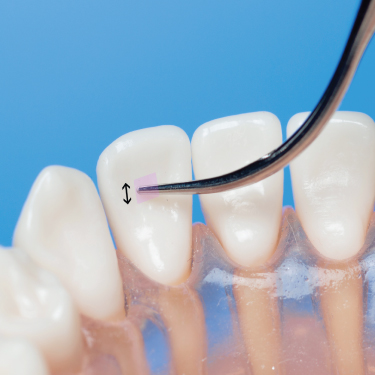
Figure 6.12 On a concave surface, oblique adaptation of the tip limits contact to the terminal 1–2 mm, minimizing the surface area debrided (shaded area) with each stroke; arrow indicates direction of working stroke
Angulation
Angulation of the active area of the oscillating tip to the tooth surface being treated should be maintained between 0 and 15 degrees: as close to 0° as possible, but never exceeding 15° (Figure 6.13). By comparison, this is similar to the degree of angulation maintained during periodontal probing, and significantly less than the 45–90° cutting edge-to-tooth angulation (Nield-Gehrig, 2008) needed to accomplish manual scaling.
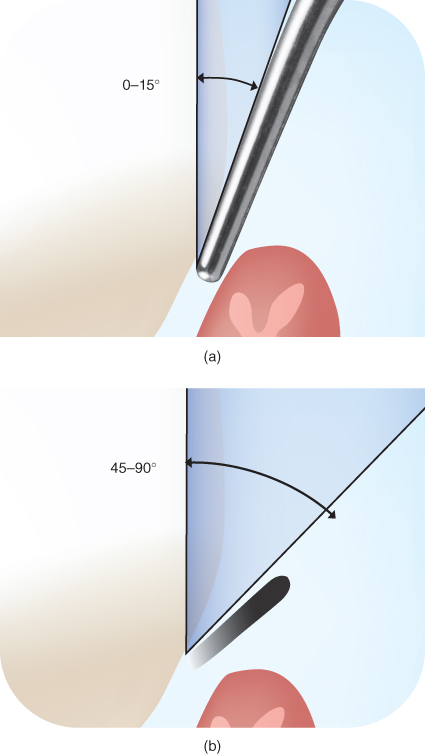
Figure 6.13 Angulation of the active area of the ultrasonic tip to the tooth surface is 0–15° (a), as compared to the 45–90° (b) angulation needed for manual instrumentation
Increasing (opening) this tip-tooth angulation beyond the recommended 0–15° increases the amount of root substance lost during sonic and ultrasonic instrumentation.
Flemmig et al. (1997, 1998a,b) demonstrated a positive correlation between the amount of root surface lost and an increase in tip-tooth angulation. Using magnetostrictive technology (Flemmig et al., 1998b), as angulation of the tip increased from 0° to 45° to 90° to the tooth, so too did the depth of the root surface defect, regardless of power setting or lateral force (Figure 6.14). However, a different pattern of root surface loss was found when piezoelectric technology was evaluated. Using piezoelectric technology (Flemmig et al., 1998a), significantly greater root surface loss occurred at the 45° angulation than at the 90° angulation (Figure 6.15).
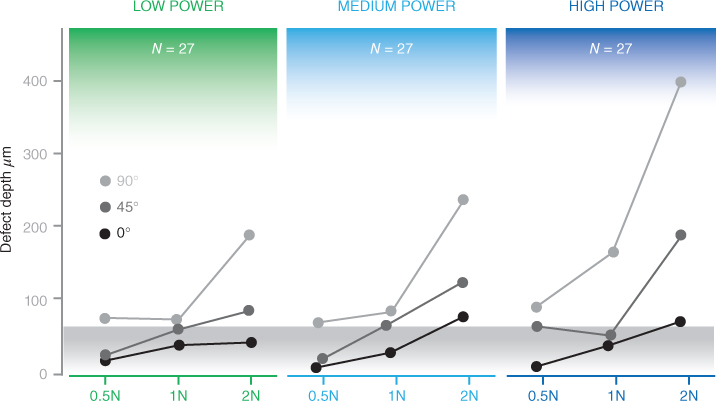
Figure 6.14 Effect of combinations of lateral force and tip angulation at different power settings on root surface defect depth after 40 seconds of instrumentation time using a magnetostrictive scaler.
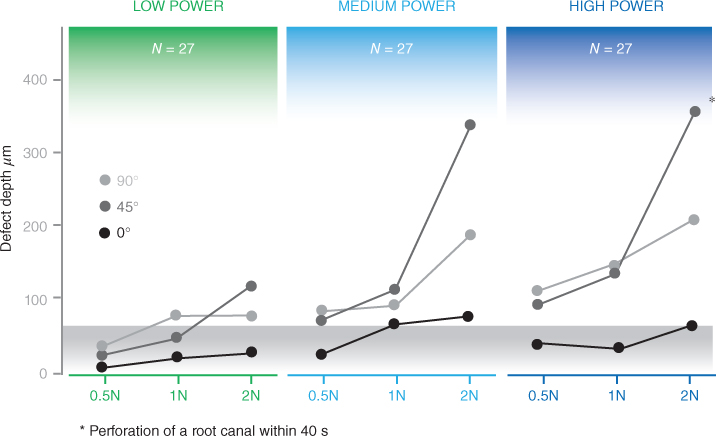
Figure 6.15 Effect of combinations of lateral forces and tip angulation at different power settings on root surface defect depth after 40 seconds of instrumentation time using a piezoelectric scaler.
At that time, the authors concluded that piezoelectric instruments are more technique sensitive in regard to tip angulation and alteration of the root surface than magnetostrictive instruments. In light of the findings of several subsequently published studies, which demonstrated that tip shape is more influential than type of generator on scaling performance (Lea et al., 2009a) and amount of root substance loss (Jepsen et al., 2004; Lea et al., 2009b) (see Chapters 3 and 4), it is likely that the differences between magnetostrictive and piezoelectric units observed by Flemmig et al. in regard to tip angulation and root surface alteration are also due to the differences in the tip shape used with each generator, not the type of generator, with the broad/flat (curette-like) tip used on the piezoelectric unit (Figure 6.16a) being more aggressive and angulation sensitive than the cylindrical (probe-like) tip used with the magnetostrictive unit (Figure 6.16b).

Figure 6.16 Tip designs identical or comparable to those used in the cited studies. Compare the (a) broad and flat (curette-like) design used with the piezoelectric scaling units to the (b) slim and cylindrical (probe-like) design used with the magnetostrictive scaling units
Lateral pressure
The tip is described as oscillating under load when it is adapted to the tooth surface, whereas the term unloaded refers to the tip oscillating freely in air. The degree of lateral pressure applied to adapt the tip is typically measured in Newtons (N), the standard unit of measurement of force.
The amount of lateral pressure to apply to the oscillating tip varies according to the type of deposit to be removed, ranging between 0.5 N and 2.0 N (Figure 6.17). Forces below this range (<0.5 N) may inhibit the clinician’s ability to maintain continuous adaptation of the tip to the tooth. Forces above this range (>2 N) affect the efficiency of deposit removal and the amount of root surface damage.

Figure 6.17 Range of lateral pressure applied during ultrasonic instrumentation
By comparison, this is significantly less than the amount of lateral force applied during manual instrumentation, which has been demonstrated to range between 1.01 and 15.73 N, with a mean of 5.70 N applied by dentists and a mean of 5.38 N applied by dental hygienists (Zappa et al., 1991).
Influence of lateral pressure on deposit removal
When an oscillating tip contacts the tooth, there is a general tendency for displacement amplitude to decrease (or dampen) initially, but not continuously as lateral force increases up to 1.0 N (Lea et al., 2003b; Trenter et al., 2003; Walmsley et al., 2013). Slim diameter tips appear to be more susceptible to dampening under load than wider diameter tips (Lea et al., 2003b; Trenter et al., 2003).
It has been previously established that the amount of cavitational activity is great/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


