Chapter 6
Technical and Laboratory Considerations
Aim
Many of the factors that determine aesthetic success are dependent on close collaboration between the clinician and laboratory. Problems, as and when they occur, are generally a result of a breakdown in communication. The aim of this chapter is to examine in detail this important area of aesthetic dentistry.
Outcome
On reading this section practitioners will become familiar with the ways in which good aesthetic results are dependent on certain technical factors and vice versa. This understanding will improve the reader’s ability to achieve optimal results.
Introduction
Optimising aesthetic outcomes for patients and operators depends on a variety of interrelated factors. These include the clinical-laboratory interface – in particular, colour communication and material selection, underpinned by appropriate tooth preparation and good-quality impressions. There is a range of ceramic materials available to practitioners today and this has led to considerable confusion. Choosing the right material needs careful consideration of the benefits of the material in terms of the potential aesthetic outcome and its physical properties balanced against the risks (for example, in terms of the amount of tooth tissue that requires removal). Equally, a discussion with the patient regarding cost and longevity is also required.
Having selected the material or materials that will be used, tooth reduction appropriate to the specific material or system must be carefully executed. Noting that both under- as well as over-preparation will affect the aesthetic outcome, it is important for practitioners to appreciate that different materials require subtly different tooth preparation. Research has shown that practitioners will frequently prepare a tooth in a way suitable for a gold inlay or onlay type restoration but request a resin composite or ceramic restoration to restore the unit. This is inappropriate, as gold is strong in thin section whereas resin composite and ceramic are not, and this poses a problem as resin composite will fracture off at the margins as a consequence of its relatively thin section.
Once measured, considered and appropriate tooth preparation has been carried out, of equal importance is how the integrity of the preparation and, not least, its relationship to the periodontal tissues are preserved. These are crucial to the long-term clinical outcome. Unfortunately adequate consideration to the temporisation of cases is rarely given. This frequently results in poorly contoured, leaking provisional crowns and bridges that encourage plaque accumulation and loss of pulp vitality in the long term. In addition to these points, practitioners often come to cement the definitive crowns to find that there has been recession or there is gingival haemorrhage to the extent that effective isolation for resin bonding procedures is well nigh impossible.
Technical Considerations for Full Coverage Restorations
Metal Ceramic Crowns
A metal ceramic crown unites two disparate materials, namely a metal alloy and porcelain. Both materials have markedly different physical and aesthetic properties. The success of this type of restoration relies on the strength of the underlying metal coupled with the aesthetic properties of the overlying porcelain. Of particular importance is the interface between the two materials.
The technician needs to mask the underlying non-reflective metal core with porcelain. This can be problematic. If this stage of the crown build-up process is not completed successfully, metal ceramic crowns can look very dark or, if over-opaqued, very high in value or “bright”. To ensure that the aesthetics of the crown are optimal, the clinician needs to complete sufficient tooth reduction to create space for the different porcelains required to mask the underlying metal substructure. Insufficient space results in a crown with a relatively high proportion of core porcelain, which is bright, and so the crown appears to be too bright or too high a value. Appropriate preparation with sufficient tooth reduction provides the technician with the space necessary to build up an aesthetic crown of the same hue but with different chroma to provide depth to the colour of the crown, while still maintaining the labial contour of the tooth. The result is a natural-looking restoration. Under-preparation – in particular, in the cervical third – is a common occurance that results in a crown with a dark neck, given the lack of space for the technician to mask the underlying metal core effectively (Fig 6-1).
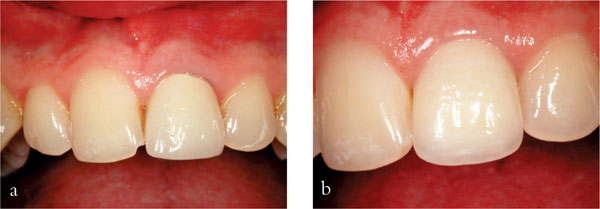
Fig 6-1 (a) Metal ceramic crown with insufficient depth of preparation in the cervical third. (b) After a Procera™ crown and resin composite addition to tooth 11. Note the excellent gingival response
All-Ceramic Crowns
With all-ceramic crowns there is no need to mask an underlying metal coping, as the restoration is metal free. As a consequence, all-ceramic crowns are increasing in popularity, offering good aesthetics and meeting patients’ increasing demands for more biocompatible restorations (Fig 6-2). However, all-ceramic crowns have a limitation in that the strength of these restorations is dependent on the strength of the core or coping used. Most copings or cores have a high value and are therefore comparatively bright. All-ceramic crowns require greater depth of preparation than metal ceramic crowns, as the practitioner must make room for the underlying coping and veneering porcelain. Exceptions to this are resin- or dentine bonded crowns and porcelain laminate veneers, which are made from feldspathic porcelain. Typically the depth of preparation is between 0.5–0.8mm for these restorations. As a consequence all-ceramic crowns cannot be described as minimal interventive techniques and in comparison with metal ceramic crowns are necessarily more destructive of tooth tissue. Systems that do not have opaque copings may not obscure the appearance of discoloured remaining tooth tissue or metal posts and cores. In these circumstances more tooth reduction may be needed to stop unwanted colours showing through the restoration. In certain cases the nature and depth of the discoloration may be such that an all-ceramic crown that does not have a coping is contraindicated.
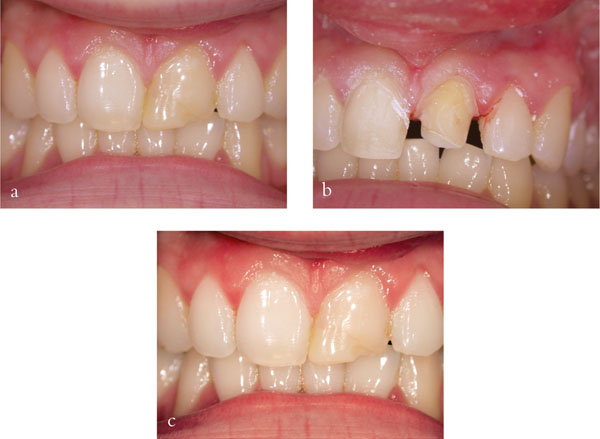
Fig 6-2 (a) Anterior teeth with resin composite build-ups. (b) Patient with the teeth and veneer prepared for Procera™ crowns. (c) Patient with the final crown and veneer in place.
Tooth Preparation
Teeth have a number of naturally occurring anatomical planes. These can be divided on the labial surface into a cervical/gingival, mid-labial and incisal. Removing the optimum amount of enamel and dentine in each dimension will give the technician just the right amount of space to make an aesthetic crown or veneer.
A useful tip is to make a matrix prior to commencing the preparation for a crown or veneer using an addition-cured polyvinyl siloxane putty. This matrix can additionally be used to produce provisional restorations, should this be required. When the operator believes that the preparation has been finished, divide the matrix through its mid-line (sagitally) using a scalpel. Replace the matrix over the prepared tooth and observe the amount of tooth reduced in all the planes along the labial and palatal walls, adjusting the preparation where necessary. Optimal labial reduction is 1.2–1.5mm for metal ceramic crowns, slightly deeper (1.5mm) for an all-ceramic crown and 0.5mm for a porcelain laminate veneer. It is not suggested that practitioners should routinely use a silicone matrix. It is, however, a useful technique for periodically checking and calibrating an individual practitioner’s preparation technique.
If under-preparation leaves the technician with insufficient space on the buccal surface to produce a crown or veneer with a natural emergence profile, he or she must decide between achieving a matched buccal contour or over-building the crown or veneer buccally to produce the right colour. Either way the result will be an unsatisfactory aesthetic outcome (Fig 6-3). Over-bulking the cervical third of crowns and laminate veneers can lead to plaque accumulation and problems with marginal inflammation, which may result in a less than optimal aesthetic outcome, in particular if the patient has a high smile line. Another area that is often under-prepared is the incisal half of the buccal or labial surface. Under-preparation may require the technician to move or widen the incisal edge to accommodate more porcelain, which would be needed to mask the underlying metal. In either situation, although under-preparation may seem more tooth friendly the converse can be true. In essence a balance must be struck between under- and over-preparation.
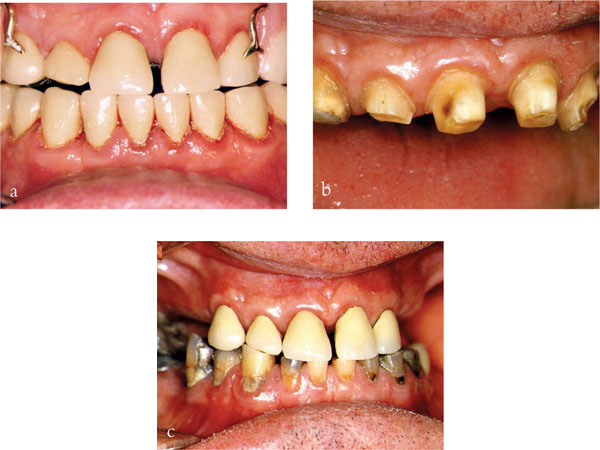
Fig 6-3 (a) Overbulked anterior crowns with marginal gingivitis. (b) Patient with refined preparations. (c) Diagnostic temporaries in place. Note resolution of marginal inflammation.
Stages of Tooth Preparation
The aim of tooth preparation is to provide sufficient space for the technician to make a crown or veneer which is both structurally durable and aesthetic. To achieve this effectively a practitioner must remove enough tooth tissue on the labial, palatal/lingual, incisal/occlusal and proximal surfaces to provide space for the crown without introducing undercuts, yet achieving a near-parallel preparation. Some clinicians prefer a staged process – for instance, occlusal/incisal reduction, then proximal reduction and then finally labial and palatal reduction, in that order.
It is suggested that practitioners proceed as follows:
-
Design the crown – choose the material for the restoration. When choosing a material, it is helpful to consider the amount of preparation each type of material will require. A metal ceramic crown needs more labial/facial reduction than a resin- or dentine-bonded crown. An all-ceramic crown needs an equal amount of tooth reduction on the labial and palatal surfaces and is less conservative of tooth tissue than either resin- or dentine-bonded crowns or metal ceramic crowns.
-
Assess and record the shade prior to tooth preparation.
-
Test the vitality where indicated clinically and check the periapical status of the tooth radiographically.
-
Local anaesthetic is given as appropriate.
-
Obtain a preoperative matrix impression of the tooth or teeth which can be used to produce the provisional crown(s). Periodically take an additional one to check the amount of tooth reduction. Typically this is done with a polyvinyl siloxane or alginate impression, which is put to one side and used to make resin replica provisional crowns after preparation has been completed. It is recommended that if alginate is used it is not put in hypochlorite or wrapped in damp gauze, as excess moisture and, in particular, hypochlorite will retard the set of provisional crown and bridge materials.
-
Another technique is to use modellers’ wax (Fig 6-4) rather then polyvinyl siloxane or alginate. Softened pink wax is moulded around the tooth prior to tooth preparation and then allowed to cool and harden. Sufficient wax is needed to produce strength in bulk. The tooth is prepared and then a provisional crown and bridge resin is dispensed into the wax. The main advantage of the wax is that alterations to the shape of the crown can be readily achieved. For minimally prepared teeth some of the labial aspect of the wax can be removed labially to thicken the provisional crown, making them more durable.
-
Cut grooves into the tooth to achieve the optimum depth for the crown preparation.
-
Retention for crowns, irrespective of the type, is derived from the length of walls and angle of the preparation taper. Ideally, the taper should be around 15–20 degrees; less than this increases the potential for developing undercuts and greater taper reduces the retention of the crown. Most of the retention is obtained from the mesial and distal reduction.
-
Ensure that the proximal contact points are cleared.
-
Follow the natural contour of the tooth.
-
Check the occlusal reduction, in particular in relation to the occlusal contact area, ensuring that adequate space has been produced. It is also important to assess the depth of preparation in relation to excursive movements.
-
Remove sharp-line angles and smooth the preparation. Typically this is done with fine-grade water-cooled finishing burs. Some clinicians find gingival margin trimmers and enamel chisels useful for refining the margins of crown preparations. Such instruments may be found to be especially useful for removing thin flashes of unsupported enamel.
-
Place retraction cord if required. It is recommended that the cord is completely submerged in the crevice and left in situ for the impression and while provisional crowns are made.
-
Make the provisional crowns, taking care to trim the margins appropriately. It is important to avoid any roughness and to ensure that each provisional crown has close/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


