Chapter 3
Bleaching and Microabrasion
Aim
Bleaching is a minimally interventionist means of improving the brightness of vital and non-vital teeth. Microabrasion is a useful (often adjunctive) technique for removing localised enamel discoloration from anterior teeth. In carefully selected cases microabrasion can be usefully combined with vital bleaching procedures to improve anterior aesthetics. The aim of this chapter is to consider different non-vital and vital bleaching procedures along with the technique of microabrasion.
Outcome
Practitioners will be familiar with the advantages, disadvantages, indications and contraindications for various methods of bleaching vital and non-vital teeth. Equally, practitioners will be familiar with the technique of microabrasion.
Introduction
The colour of teeth is very subjective. It means different things to different people. For example, a patient may be convinced that their teeth are too dark and yet to the practitioner they appear to be within the normal colour range. This commonly occurs with canines, which are wronr teeth. Canines are darker than incisors, but this is the natural result of the canine being thicker buccolingually than the other anterior teeth. Differences in the assessment of the colour of teeth between patient and clinician can be an important consideration when obtaining informed consent for bleaching procedures, as it is not possible to guarantee that the technique will be successful, let alone how long the bleaching effect will last.
Common Causes of Tooth Discoloration
The causes of tooth discoloration can be classified as follows:
Localised
Trauma:
-
permanent teeth
-
developing teeth.
Superficial staining:
-
extrinsic causes – dietary, smoking or plaque-related
-
caries
-
discoloured restoration.
Generalised
Acquired:
-
age-related
-
tetracycline
-
fluorosis.
Hereditary:
-
amelogenesis imperfecta
-
dentinogenesis imperfecta.
It is clear that there are a number of causes for tooth discolouration and the diagnosis is important, as this will determine how an individual case is managed.
Trauma
Damage to the blood supply of fully developed teeth may result in the loss of vitality. The pulpal tissues degenerate, sometimes acutely, producing a non-vital tooth. The blood pigments left behind following pulp degeneration include haemoglobin, which infiltrates the dentinal tubules, leading to significant tooth discoloration when this breaks down. This stain can vary in intensity from very dark to almost imperceptible. The intensity of the discoloration will in general determine the time needed to bleach the tooth and in some cases the likelihood of success.
Infrequently, trauma to a deciduous tooth will damage the developing permanent replacement. The result might be a change in colour and shape of the permanent tooth. The discoloration, provided it is not too intense, may be corrected. The change in shape may necessitate the provision of a veneer or crown in adult life.
Superficial staining
Superficial extrinsic staining can be removed by a thorough scaling and polishing. Common dietary supplements – for example, tannin – will cause a superficial stain to develop on the exposed surfaces of teeth. Smoking can also cause extensive extrinsic staining of teeth – in particular, in heavy smokers. Such stains, although superficial, can be quite resistant to routine cleaning and polishing techniques. Whitening toothpastes, containing emulsifiers and titanium dioxide, may remove superficial stain and appear to whiten the teeth. They are particularly useful for removing dietary stains, tobacco tars and for shade maintenance after bleaching.
Occasionally, a chromogenic-type bacterium colonises the gingival crevice of patients with poor oral hygiene. This causes a green/black stain along the cervical margin of the teeth. Typically, a routine prophylaxis fails to remove such surface stain and either bleaching or tooth reduction is required.
Age-related changes
As people age their teeth darken or appear darker. This may be a result of the enamel wearing, exposing the underlying darker dentine, and/or the effect of age-related sclerosis of dentine: consequently the tooth appears darker. This apparent change must be balanced against the patient’s age, as the actual colour change with age might not be so prominent. Equally the tooth colour may appear to be natural while lighter teeth would appear unnatural when framed by an older face.
Tetracycline
Prescribing tetracycline for non-critical infections in patients with developing teeth is now considered to be indefensible. Consequently, the incidence of tetracycline discoloration is decreasing, notably in the UK. This is in contrast to other parts of the developing world. The tetracycline molecule becomes incorporated into developing tooth tissues, changing the colour of dentine from which teeth get their inherent colour (Fig 3-1). The degree of yellow to blue-grey discoloration depends on the nature and concentration of tetracycline administered to the patient and the exposure of the tetracycline-containing tooth tissues to ultraviolet light following eruption. Some brown/yellow tetracycline stains are relatively easy to overcome using vital bleaching techniques. Blue-grey tetracycline stains often remain resistant to bleaching.
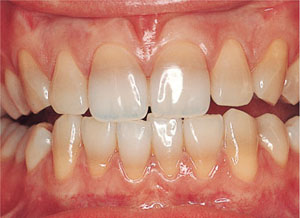
Fig 3-1 Tetracycline staining.
Fluorosis
The intake of excessive amounts of fluoride during tooth crown formation may result in brown and white speckled mottling of the tooth – fluorosis. Concentrations of more than 1ppm of fluoride in drinking water increase the risk of fluorosis – in particular if large amounts of toothpaste or other dietary supplements of fluoride are taken at the same time.
Bleaching or removing the superficial layer of enamel with microabrasion normally eliminates brown mottling. The surrounding white speckled opacity is more difficult to remove but usually responds favourably to vital bleaching. These less interventive management techniques are usually preferred to crowns or veneers, since no tooth tissue needs to be sacrificed.
Hereditary causes
Dentinogenesis imperfecta and amelogenesis imperfecta are relatively rare conditions. It can be difficult to differentiate these conditions clinically. Dentinogenesis imperfecta (hereditary opalescent dentine) is characterised by bulbous root formation and an absence of root canals. Radiographs are invaluable in confirming a diagnosis of dentinogenesis imperfecta. Amelogenesis imperfecta is more difficult to diagnose, as the condition has a variable presentation. Confusing amelogenesis imperfecta with marked fluorosis is not unusual.
Vital Bleaching
Hydrogen Peroxide (H2O2)
Hydrogen peroxide has been used to bleach teeth for over a century. Bleaching (lightening or brightening) teeth is an effective treatment for stained and discoloured sound teeth. Vital tooth-bleaching has the added advantages of being both less interventive and conservative of tooth tissues. Alternative treatments, such as veneers, all-ceramic crowns and metal-ceramic crowns, by necessity require extensive tooth-tissue removal. Vital tooth-bleaching, in common with most clinical procedures, is not without some risk. This risk is, however, low. Balanced against the risk of a tooth becoming non-vital after crowning, bleaching remains the initial treatment of choice to improve the appearance of discoloured teeth. Although veneers and crowns can improve the appearance of discoloured teeth, they can never reproduce the translucency and vibrancy of the intact tooth.
Mode of action
Hydrogen peroxide is a minute molecule. As a consequence, it is able to penetrate enamel and dentine, effecting a change that results in bleaching. Hydrogen peroxide, or those products that degrade to produce it, dissociates to form the superoxide ion and water. It is the high reactivity of the superoxide ion which is thought to be responsible for the bleaching process. The reactive ion removes the stains from teeth by oxidising pigments trapped in the structures of enamel and dentine. Most clinical techniques for bleaching rely on this effect but vary the speed by either extending the periods of contact, using higher concentrations or, as previously practised, heating the bleaching agent.
Carbamide Peroxide
Carbamide peroxide, otherwise known as urea peroxide, breaks down to form hydrogen peroxide and urea. In the oral environment the hydrogen peroxide forms the superoxide ion and water, while the urea forms ammonia and carbon dioxide. The amount of urea formed as part of the breakdown is too small to have any biological consequence. Most research on the safety and efficacy of carbamide peroxide has been on a 10% concentration. More recently, higher concentrations have been produced that increase the speed of reaction and so the bleaching process. A 10% solution of carbamide peroxide produces 3.35% hydrogen peroxide, a 15% solution of carbamide peroxide produces 5% hydrogen peroxide and a 35% carbamide peroxide (chair-side bleaching) gives 10% hydrogen peroxide. To avoid any adverse reactions care must be taken to use solutions and gels of carbamide peroxide according to manufacturer’s directions.
Safety
In the past, bleaching has been used to lighten non-vital teeth. Only in the past 15 years or so has the bleaching of vital teeth become more common. There are risks associated with any operative procedure: using hydrogen peroxide to bleach teeth is no exception. In the early days the technique carried a relatively high risk of subsequent resorption because heat was used to activate the hydrogen peroxide. More recently, the potential for systemic effects has raised concerns, none of which has, to date, found any scientific support. The main concern with hydrogen peroxide is its potential to cause cellular damage. Most of the studies undertaken to investigate this effect have used animal models, with high concentrations per body weight applied for extended periods of time. It is difficult to extrapolate the effects of hydrogen peroxide under such situations to the clinical situation. Hydrogen peroxide is a by-product of human enzymatic action, which is then naturally degraded by enzymes to reduce its potentially damaging effect. Despite the results from animal studies suggesting toxic effects on small mammals, the likely risk to human beings is very low. The consensus of opinion based on research is that the risk of damaging side-effects from hydrogen peroxide or other associated products used to bleach vital or non-vital teeth is small. In essence, the benefits of the treatment far outweigh the theoretical risks of the procedure.
Effects on Teeth and Restorative Materials
Findings from laboratory studies suggest that bleaching has no adverse effect on tooth tissues. Studies on enamel hardness and the bond strength of resin composites to bleached enamel have failed to demonstrate any clinically significant effects of bleaching. There is less research available on the effects of bleaching on dentine bonding but the effect, as with enamel, would appear to be negligible.
When restoring bleached teeth it is generally recommended to delay the provision of restorations of resin composites or glass ionomer cements for at least 24 hours following completion of bleaching. One of the effects of bleaching is dehydration of the tooth surface. Although rehydration tends to occur quickly (< 24 hours), it is advisable to be satisfied that sufficient time has elapsed before proceeding to provide tooth-coloured restorations. An alternative approach is to place restorations before bleaching, but this has the disadvantage of exposing the surfaces of recently placed restorations to hydrogen peroxide. Furthermore, it is difficult to predict shade following bleaching. A common clinical outcome of bleaching is patients requesting restorations be changed to match the new colour of the teeth. It is helpful, therefore, to warn the patients that anterior restorations may need to be replaced following bleaching.
If new crowns are placed after bleaching the adjacent teeth may gradually revert to their original pre-bleached colour and the crowns will appear too bright. Minimally prepared teeth restored with restorations of translucent porcelain – for example, resin-bonded crowns or laminate veneers – may have a slightly different response to bleaching. The bleaching material may pass through the marginal interface to affect the colour of the underlying dentine, which will, in turn, affect the colour of the restored unit. More likely, if bleached teeth are subsequently crowned or veneered, the core of the tooth may darken over time, resulting in a darkening of the restored tooth. Previous clinical experience with veneers has shown that darkening a veneered tooth can be corrected by rebleaching via the palatal surface, with an appropriately designed bleaching splint. If full-coverage crowns are prescribed post-bleaching it is prudent to use a system that has some form of coping to protect the restoration from changes in the colour of the underlying dentine.
The effects of bleaching materials on amalgams have also been investigated. It is unlikely that the bleaching agents used will result in the release of significant levels of mercury, and any mercury released is within recognised safety limits. Occasionally, amalgam restorations may change from a dark to a more silver appearance.
Stability of Bleaching
The response of vital teeth to bleaching is variable. It is not unknown for bleached teeth to remain whitened for decades. In other cases the effects may be short-lived. In most patients the colour of their bleached teeth will remain stable for periods of up to two to three years after which “top-up” bleaching may be required. If the change occurs more quickly, within months, then another bleaching technique or restorative technique is probably indicated. This problem with the stability of the treatment outcome should be balanced against the choice of other irreversible, more destructive restorative techniques, many of which may often have a similar life expectancy. Either way, the patient should be warned about the risk before starting treatment.
Preservation of Tooth Tissue
Many patients will feel comfortable with bleaching as a conservative technique and will accept this treatment over more invasive ones, such as veneers or crowns. This is especially true of younger patients once they realise that restorations may last only a few years. A restoration placed early in life will in all probability need to be replaced many times, resulting inevitably in the loss of more tooth tissue each time it is replaced. In due course repeated treatments will lead to a loss of vitality and critical weakening of the remaining tooth tissues.
The choice whether to bleach teeth or provide veneers or crowns depends on the restorative status of the teeth to be treated. Generally speaking, bleaching should be undertaken only on sound or minimally restored teeth. Teeth with extensive restorations are probably more appropriately treated with crowns.
The bleaching process lightens the teeth but not restorations. Therefore, if extensive restorations are present they will need to be replaced following bleaching. Over time bleached tooth tissue may darken but the colour of the replaced resin composites will remain stable, resulting in a colour mismatch.
Side-effects
The most common side-effect with vital bleaching is cervical sensitivity, which can have an incidence as high as 50%. In most patients this is tolerable and does not interfere with the quality of life of the patient, nor is it likely to compromise the vitality of the tooth. In others, the symptoms disappear within a few days. In cases in which the sensitivity becomes unbearable for patients treatment should be discontinued. The authors have found that concurrent use of a daily fluoride mouthwash and/or the once-only application of a dentine desensitiser, often pre-treatment, help to reduce sensitivity.
It is important to supervise the bleaching process, providing the patient with advice and support during the procedure. Some practitioners manage this by providing patients with a limited number of tubes of bleaching agent and reviewing the pat/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


