Chapter 6
Restorative dentistry
Contents
Relevant pages in other chapters Caries diagnosis, p. 26; amalgam, p. 608; resin composite, p. 610; the acid-etch technique, p. 614; dentine adhesive systems, p. 616; glass ionomers, p. 618; cermets, p. 623; cements, p. 624; impression materials, p. 626; casting alloys, p. 630; acid-etch tip, p. 100.
Principal sources and further reading Operative Dentistry. Dental Update. The British Dental Journal. B. G. N. Smith 1997 Planning and Making Crowns and Bridges, Dunitz. P. A. Brunton 2002 Decision Making in Operative Dentistry, Quintessence. J. L. Gutmann et al. 1997 Problem Solving in Endodontics, 3rd edn, Mosby. E. A. M. Kidd et al. 2003 Pickard’s Manual of Operative Dentistry, 8th edn, OUP. S. J. Davies and R. J. Gray 2002 A Clinical Guide to Occlusion, British Dental Association. J. M. Whitworth 2002 Rational Root Canal Treatment in Practice, Quintessence.
To attempt to resolve the problem of caries by preparing and restoring teeth is comparable to trying to resolve the problem of poliomyelitis by manufacturing more attractive and better quality crutches, more quickly and more cheaply.
Treatment planning
A proper treatment plan can only result from a thorough patient assessment, which must include a history, an examination, relevant special tests, and ultimately, a diagnosis.
Under ideal circumstances an integrated treatment plan is formulated for each patient at the start of every course of treatment. Very often, however, the treatment plan will need to be revised in the light of clinical findings as the treatment progresses, e.g. patient cooperation, response to periodontal therapy, investigation of teeth of doubtful prognosis, etc. When dealing with patients with a range of problems it is therefore wise to formulate a treatment plan which has a number of achievable goals, and then on completion of this to reassess the patient to decide on what further treatment is necessary.
Sequence of treatment
This list is obviously an oversimplification but should serve as a general guide to the order in which treatment should be carried out.
Practical points
Stabilization or caries control
In patients with multiple carious lesions it may take several weeks/months to complete the permanent restorations necessary to secure OH. In these cases it may be advisable to prevent any symptomless large lesions increasing in size by placing temporary dressings. The cavities should be rendered caries-free at the margins, and temporarily restored with a strong cement, e.g. traditional or resin-modified GI cement.
Dental pain
When a patient attends the surgery and complains of toothache, pain may be arising from a variety of different structures and may be classified as follows:
Dental pain can be very difficult to diagnose, and the clinician must first gather as much information as possible from the history, clinical and radiographic examinations, and other special tests (see Chapter 1).
Pulpal pain
The pulp may be subject to a wide variety of insults, e.g. bacterial, thermal, chemical, traumatic, the effects of which are cumulative and can ultimately lead to inflammation in the pulp (pulpitis) and pain. The dental pulp does not contain any proprioceptive nerve endings, therefore a characteristic of pulpal pain is that the patient is unable to localize the affected tooth. The ability of the pulp to recover from injury depends upon its blood supply, not the nerve supply, which must be borne in mind when vitality (sensibility) testing is carried out (p. 14).1 It is impossible to reliably achieve an accurate ∆ of the state of the pulp on clinical grounds alone; the only 100% accurate method is histological section.
Although numerous classifications of pulpal disease exist, only a limited number of clinical diagnostic situations require identification before effective treatment can be given.
Reversible pulpitis
Symptoms
Fleeting sensitivity/pain to hot, cold or sweet with immediate onset. Pain is usually sharp and may be difficult to locate. Quickly subsides after removal of the stimulus.
Signs
Exaggerated response to pulp testing. Carious cavity/leaking restoration.
Rx
Remove any caries present and place a sedative dressing (e.g. ZOE) or permanent restoration with suitable pulp protection.
Irreversible pulpitis
Symptoms
Spontaneous pain which may last several hours, be worse at night, and is often pulsatile in nature. Pain is elicited by hot and cold at first, but in later stages heat is more significant and cold may actually ease symptoms. A characteristic feature is that the pain remains after the removal of the stimulus. Localization of pain may be difficult initially, but as the inflammation spreads to the periapical tissues the tooth will become more sensitive to pressure.
Signs
Application of heat (e.g. warm GP) elicits pain. Affected tooth may give no or a reduced response to electric pulp tester. In later stages may become TTP.
Rx
Extirpation of the pulp and RCT is the treatment of choice (assuming the tooth is to be saved). If time is short or if anaesthesia proves elusive then removal of the coronal pulp and a Ledermix® dressing can often control the symptoms until the remaining pulp can be extirpated under LA at the next appointment.1
Dentine hypersensitivity
This is pain arising from exposed dentine in response to a thermal, tactile, or osmotic stimulus (but not all exposed dentine gives rise to symptoms). It is thought to be due to dentinal fiuid movement stimulating pulpal pain receptors. Prevalence is ~1:7 adults with a peak in young adults, then ↓ with age.2 ∆ is by elimination of other possible causes and by evoking symptoms.
Rx Involves ↓ aetiological factors (i.e. OHI, possibly including tooth- brushing technique and intrinsic and extrinsic dental erosion) and by ↓ permeability of dentinal tubules (e.g. by toothpaste containing strontium &/or fluoride; placement of varnishes, dentine desensitizers, dentine adhesive systems, or, if indicated, a restoration).
Cracked tooth syndrome
Symptoms
Sharp pain on biting—short duration.
Signs
Often relatively few, therefore ∆ difficult. Tooth often has a large restoration. Crack may not be apparent at first but transillumination and possibly removal of the restoration may aid visualization. Positive response to vitality (sensibility) testing and pain can normally be elicited by getting the patient to bite with the affected tooth on a cotton-wool roll or a ‘tooth slooth’. May be associated with bruxing habit.
Rx
An adhesive resin composite restoration may be appropriate in teeth which are minimally restored, but in some cases a cast restoration with full occlusal coverage will be needed. Occasionally RCT may be required.
Periapical/periradicular pain
Progression of irreversible pulpitis ultimately leads to death of the pulp (pulpal necrosis). At this stage the patient may experience relief from pain and thus may not seek attention. If neglected, however, the bacteria and pulpal breakdown products leave the root canal system via the apical foramen or lateral canals and lead to inflammatory changes and possibly pain. Characteristically the patient can precisely identify the affected tooth, as the periodontal ligament, which is well supplied with proprioceptive nerve endings, is inflamed.
Pulpal necrosis with periapical periodontitis
Symptoms
Variable, but patients generally describe a dull ache exacerbated by biting on the tooth.
Signs Usually no response to vitality testing, unless one canal of a multirooted tooth is still vital. The tooth will be TTP. Radiographically the apical PDL may be widened or there may be a periapical radiolucency (granuloma or cyst).
Rx
RCT or extraction.
Acute periapical abscess
Symptoms
Severe pain which will disturb sleep. Tooth is exquisitely tender to touch.
Signs
Affected tooth is usually extruded, mobile, and TTP. May be associated with a localized or diffuse swelling. Vitality (sensibility) testing may be misleading as pus may conduct stimulus to apical tissues. Radiographic changes can range from a widening of the apical PDL space to an obvious radiolucency. It is important to differentiate this condition from a periodontal abscess.
Rx
Drain pus and, if indicated, relieve occlusion. Drainage of pus can often be achieved by entering the pulp chamber with a high-speed diamond bur, steadying tooth with a finger to prevent excessive vibration. After drainage has been achieved it is preferable to prepare the canal and place a temporary dressing. Avoid ‘open drainage’ if possible, but if absolutely necessary for <24h, as after this time further bacterial contamination of the root canal makes subsequent RCT very difficult. If a fluctuant soft tissue swelling is present, this should be incised to achieve drainage. Antibiotics should be prescribed if there is systemic involvement or if the infection is spreading significantly along tissue planes. When the acute symptoms have subsided, RCT must be performed or the tooth extracted.
Chronic periapical abscess
Often symptomless. Possibly associated with persistent sinus. Presentation may be: coincidental finding or acute exacerbation.
Lateral periodontal abscess
Symptoms
Similar to periapical abscess with acute pain and tenderness, and often an associated bad taste.
Signs
Tooth is usually mobile and TTP, with associated localized or diffuse swelling of the adjacent periodontium. A deep periodontal pocket is usually associated, which will exude pus on probing. Radiographs normally show vertical or horizontal bone loss, and vitality (sensibility) testing is usually positive, unless there is an associated endodontic problem (perio-endo lesion).
Rx Achieve drainage of pus. Irrigate with a chlorhexidine solution. If there is systemic involvement or it is a recurrent problem, prescribe antibiotics (metronidazole or amoxicillin). Debride the pocket once acute symptoms have settled.
Non-dental pain
When no signs of dental or periradicular pathology can be detected then non-dental causes must be considered. Other causes of pain that can present as toothache include:
Isolation and moisture control
Isolation is required to aid visibility, prevent contamination during moisture-sensitive techniques, maintain a relatively aseptic environment, and protect the patient from caustic materials or aspiration of foreign material.
High-volume suction,
e.g. an aspirator.
Low-volume suction,
e.g. a saliva ejector.
Compressed air
This tends to redistribute the moisture to somewhere else (e.g. your eye) rather than remove it. Should be used with care in deep preparations as prolonged use can cause pulpal damage, let alone displace adhesive materials when the solvent is being evaporated prior to curing.
Absorbents
Rubber dam
This provides effective isolation and also improves access to operating site. It is indicated where moisture control and airway protection are essential, e.g. RCT (RCT without rubber dam is considered negligent), acid-etch technique. With practice, rubber dam can be applied quickly and often saves time in the long run. The dam must be secured to the teeth; several methods are available:
Types of dam:
Placement: Several regimens have been described; the following is popular:
If using caustic materials, a rubber dam sealer (e.g. OraSeal®) should be used.
Removal:
Protection of the airway
Mandatory when fitting crowns, bridges, inlays, and carrying out RCT. Best provided by rubber dam, but if this is not possible a butterfly sponge or gauze can be used.
Gingival retraction
↓ gingival exudate and exposes subgingival preparations prior to impression-taking. Some retraction cords are impregnated with substances such as adrenaline to ↓ bleeding. The cord should be gently placed into the gingival crevice with a cord packing instrument (leaving no tag hanging out) prior to impression-taking and temporization. Braided cords are better than twisted. Bleeding from the gingival margin can be ↓ by applying an astringent. A paste (Expasyl™) which contains aluminium chloride provides for retraction and haemorrhage control. Expasyl™ is useful for preparations finished within or just below the level of the gingival crevice, otherwise retraction cord is more appropriate.
Electrosurgery
May be indicated where a margin extends subgingivally and gingival overgrowth is hampering restoration placement or impression-taking. Also for crown-lengthening procedures, although bone removal is required too.
(See p. 102 on crown lengthening).
Principles of tooth preparation
Why restore?
However, these reasons need to be evaluated with regard to the patient and the rest of the dentition.
Preparation design
With caries prevalence declining, emphasis has changed from extension for prevention, to minimizing removal of tooth tissue. Tooth preparation should be based on the morphology of the carious lesion and the requirements of the restorative material being used.
General principles of tooth preparation
Helpful hints
Amalgam1
(see also p. 608)
Resin composite,
p. 610.
Glass ionomer,
p. 618.
Gold
It would be foolish to think that experience in tooth preparation can be adequately assimilated from the written text. The purpose of the following pages is to give the reader some practical tips on how to do the procedures considered, as well as to describe recent innovations and techniques.
Nomenclature
Black’s classification of cavities is now not widely used. It has been replaced by the following:
| Occlusal (Class I) | Cavity in pits and fissures |
| Proximal (Class II or III) | Cavity in proximal surface(s) of any tooth |
| Incisal (Class IV) | Proximal in an anterior tooth, but including incisal edge |
| Cervical (Class V) | Cavity in cervical third of buccal or lingual surface of any tooth. |
Occlusal (Class I)
Amalgam
Amalgam is still the most widely used material for occlusal cavities, probably because it is more forgiving of technique than some of the newer materials. It is now widely accepted, however, that resin composite placed in conjunction with minimal preparation techniques has a role in initial lesion management. If enamel margins are cut to an angle of 90° (or, if cusps steeply inclined, >70°) the resultant preparation will be adequately retentive.
Lining
Recently, emphasis has changed, with linings being used to seal the underlying dentine for moderate to deep cavities. Light-cured RMGIs (e.g. Vitrebond™) are now recommended. A preparation sealer (Gluma® Desensitizer) can be used in minimal preparations.
Resin composite
Use of these materials in posterior teeth is increasing as patients request tooth coloured restorations and their concern about amalgam grows. The controversy surrounding posterior resin composites is dealt with on pp. 230 and 612. A technique which has gained more widespread acceptance is:
Preventive resin restoration
Introduced by Simonsen (then by others as the minimal resin composite restoration or sealant restoration!). Preparation is limited to caries removal and the resultant preparation restored using fissure sealant alone if small, or resin composite followed by sealant if larger. Alternatively, GI can be used instead of resin composite. The rationale of this approach is that adjacent fissures are sealed for prevention. It is particularly useful for investigating any suspect areas of a fissure, a technique that is often referred to as an enamel biopsy (obviously coined by an academic). This involves exploring the area with a small bur, and if no caries is found further preparation can be aborted and sealant placed. If carious, a PRR can be carried out. It is often possible to complete preparation of a PRR without LA; however, if the cavity appears larger than originally thought, LA can then be given. If the preparation extends significantly into load-bearing areas, conventional tooth preparation should be carried out and the tooth restored with resin composite or other suitable material.
Technique for medium-sized cavities:
Where possible a related sealant and resin composite should be used to ensure a good bond.
Hints for resin composite restorations
Proximal (Class II)
 Avoid the creation of an overhang at the cervical margin and ensure a good contact point with adjacent tooth with a well-contoured matrix band and wedges.
Avoid the creation of an overhang at the cervical margin and ensure a good contact point with adjacent tooth with a well-contoured matrix band and wedges.
Amalgam
In practice, preparation size is determined by the size of the carious lesion and extension beyond this should be minimal. Proximal preparations comprise a proximal box with vertical grooves. The preparation should only extend occlusally if there is evidence of caries in the occlusal fissures. Retention from occlusal forces is derived from a 2–5° divergence of the walls towards the floor in both parts of the preparation. Amalgam restorations are prone to # at the isthmus in restorations exte-nded occlusally, therefore sufficient depth must be provided in this area. The width of the isthmus should not be overcut (ideally ¼ to 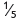 intercusp width). If the cusps are extensively undermined or missing they should be replaced with a bonded restoration (p. 232). A chisel can be used to plane away unsupported enamel from the margins of the completed preparation to produce a 90° butt joint. In molar teeth with mesial and distal caries it is preferable to try and cut two separate cavities, but often a confluent mesio-occlusal-distal preparation is unavoidable. Increasingly the use of resin composite placed in conjunction with a dentine adhesive system is advocated for the restoration of small to moderate proximal preparations in premolar and molar teeth.
intercusp width). If the cusps are extensively undermined or missing they should be replaced with a bonded restoration (p. 232). A chisel can be used to plane away unsupported enamel from the margins of the completed preparation to produce a 90° butt joint. In molar teeth with mesial and distal caries it is preferable to try and cut two separate cavities, but often a confluent mesio-occlusal-distal preparation is unavoidable. Increasingly the use of resin composite placed in conjunction with a dentine adhesive system is advocated for the restoration of small to moderate proximal preparations in premolar and molar teeth.
Tunnel preparations
A ‘tunnel’ approach to interproximal caries has been described.1 Access to the caries is made through either the occlusal or buccal surfaces, leaving the marginal ridge intact. This approach is only suitable for small lesions, as when preparation is completed at least 2mm of marginal ridge must remain. The access cavity may need to be widened buccolingually to complete caries removal. Carisolv™ may have a place here to ensure complete caries removal. A piece of mylar strip wedged into place will act as a matrix. A RMGIC is used to fill the bulk of the preparation and the occlusal access cavity restored with a posterior resin composite. In view of the difficulty of accurately removing all the caries, let alone the incidence of marginal fracture, this technique is rarely used.
Resin composite
Posterior resin composites should be used predominately to restore posterior teeth, but the technique is more demanding, taking ~50% longer. In addition, it is difficult to establish adequate contact points and occlusal stops. Polymerization shrinkage can cause cuspal flexure, post-operative pain, and marginal gaps. Direct posterior resin composites are best avoided in the following situations:
If a resin composite is to be used then a hybrid material with >75% filler is advisable. Pre-wedging one but not both proximal contacts aids creation of a contact point. Resin composite should be placed, and cured, incrementally. If possible, centric stops should be preserved on sound tooth tissue or the restorative material, but never on the marginal interface of the restoration.1 Use of indirect composite inlays may combat some of these problems (see next section).
Proximal (Class II)—resin composite and inlays
Resin composite and porcelain inlays
These inlay techniques appear to overcome some of the problems associated with direct resin composite restorations. When used in conjunction with an acid-etch technique existing tooth tissue can be reinforced. Curing resin composite outside the mouth with the addition of heat (110° for 5mins) or pressure overcomes polymerization shrinkage and possibly ↑ strength. As the inlays are bonded to the tooth with an adhesive, parallel walls are less important, but undercuts must be removed or blocked out with an RMGI cement (not in the proximal box). In general porcelain inlays offer improved aesthetics, surface finish, and bond in comparison to resin composite inlays; however, placement and adjustment can be more difficult. Ceromers (e.g. belleGlass™) may also be used in similar situations.
Technique: preparation
Technique: cementation
Proximal (Class III), incisal (Class IV), cervical (Class V), and root surface caries
Anterior proximal
Resin composite is the most widely used material for anterior proximal restorations.
Access should be gained from either the buccal or lingual aspect, depending on the position of the lesion. As resin composite is adhesive the preparation is just extended sufficiently to remove all peripheral caries. Some unsupported enamel can be retained labially, but the margins should be planed with chisels to remove any grossly weakened tooth structure. Tooth preparation can be almost entirely completed with slow-speed burs and hand instruments. Ideally the margins are bevelled. A slight excess of material should be moulded into the preparation with a mylar strip, wedged cervically. Once the material is set, the excess can be removed. After checking the occlusion the restoration can be polished using one of the proprietary products (e.g. Sof-Lex™ discs, Enhance®) if necessary.
Incisal
The restoration of choice is resin composite, the so-called ‘acid-etch tip’ (p. 100); however, for large incisal cavities in the adult patient, a dentine-bonded crown or porcelain veneer may give better retention and aesthetics.
Cervical
Although cervical cavities are seen less frequently in younger patients, they are an ↑ problem in older age-groups with gingival recession. Resin composite e.g. flowable, compomer, or RMGIC are the preferred materials in this situation. Amalgam should be avoided in this situation due to the possibility of a lichenoid reaction.
Once caries has been removed the occlusal margin should be bevelled. The cervical margin should not be bevelled as it has been shown to ↑ microleakage. The materials are ideally placed incrementally under rubber dam isolation.
Root surface caries
As gingival recession is a prerequisite to root caries, it occurs predominantly in the >40-yr age group. Dentine, which has a critical pH below that of enamel, is thus directly exposed to carious attack. It is sometimes seen secondary to ↓ saliva flow (which reduces buffering capacity and may alter dietary habits) caused by salivary gland disease, drugs, or radiation. Long-term sugar-based medication may also be a factor. Rx requires, first, control of the aetiological factor, and for most patients this involves dietary advice and OHI. Topical fluoride varnishes, high fluoride toothpastes and mouthrinses may aid remineralization and prevent new lesions developing. However, active lesions require restoration, typically with a traditional or RMGIC. See also severe early childhood caries p. 90.
Management of the deep carious lesion
Assessment
Management Depends upon a guesstimate of pulpal condition (p. 220).
Irreversible pulpitis/necrotic pulp—Rx: RCT (p. 276) or extraction. Reversible pulpitis/healthy pulp—aim to maintain pulp vitality by selective removal of carious dentine without pulp exposure. If in doubt Rx as reversible pulpitis. Can always institute RCT later.
There is some evidence that in symptomless teeth with deep carious lesions partial, rather than complete, removal of caries is preferable as it reduces the risk of pulp exposure. It is not known yet whether it is necessary to re-enter and complete excavation at a later date (stepwise excavation of caries)1
Rationale
Bacteria sealed under a restoration that provides a good peripheral seal are denied substrate, therefore lesion arrests. This allows the pulpodentinal complex to lay down reparative dentine.
Exposure
Pulpotomy Is removal of coronal part of pulp in order to eliminate damaged or contaminated tissue. It is indicated for teeth with immature apices, as continued vitality of apical pulp will allow root formation to proceed. Once the apex has closed, conventional RCT can be carried out. The pulp is amputated to the cervical constriction, dressed with non-setting or hard-setting calcium hydroxide or MTA and the tooth temporarily restored.
Materials used in the management of pulp vitality
Calcium hydroxide
has a pH of 11, which makes it bacteriostatic and promotes the formation of a calcific barrier. When calcium hydroxide comes into contact with the pulp a zone of pulpal necrosis is formed. This is subsequently mineralized with calcium ions from the pulp. It is the material of choice for direct pulp caps, particularly the hard-setting type.
Mineral trioxide aggregate is
a very slow setting material. Similar in nature to industrial cement. Very biocompatible.
Ledermix
is a mixture of triamcinolone acetonide (a steroid) and demethyl chlortetracycline in a water-soluble base. It has anti-inflammatory and bacteriostatic properties, but also suppresses pulpal defences, therefore resulting in the rapid spread of any bacteria not affected by the antibiotic it contains. It is a useful compromise for the management of irreversibly inflamed pulps where anaesthesia may be a problem, or when pulp extirpation has to be delayed.
Survival and failure of restorations
Survival of restorations
The results of Elderton’s study into the durability of routine restorations placed in the General Dental Services in Scotland provided both a shock and a stimulus to the profession, as he found that 50% lasted for less than 5yrs.1 This led to debate over both clinical technique and the profession’s readiness to replace restorations. It has been reported that 60% of practitioners’ time is spent replacing restorations. It is also interesting to note that those patients who change dentists frequently are more at risk of replacement restorations than those who are loyal to the same GDP.2 In order to ↑ longevity we need to consider the reasons for the failure of restorations and ∆ of secondary caries.
Reasons for failure of restorations
Before replacing a failed restoration it is important to identify the cause of failure and decide whether this can be dealt with by replacement or repair. When making this decision bear in mind that cavity size is ↑ on average by 0.6mm each time a restoration is removed.3
Secondary caries
Unfortunately, placement of a restoration does not confer caries immunity upon a tooth. When caries occurs adjacent to a restoration it is called secondary or recurrent caries. More correctly it is defined as a new lesion which just happens to be adjacent to an existing restoration, and it should be managed in its own right. While secondary caries is an accepted phenomenon, we as a profession have perhaps been a little too ready in the past to diagnose and treat it. Ditched amalgam margins are not a reason for replacement per se, and active intervention is only required if caries can definitely be demonstrated as active. Secondary caries is difficult to diagnose, but careful observation (clinically and radiographically) rather than intervention, is now advocated. Intervention is only indicated when the lesion is in dentine, and there is evidence of progression &/or cavitation is present.
To prevent secondary caries it is important not only to educate the patient to reduce their caries rate, but also to examine our restorative technique, to ensure good long term-restorations.
Occlusion—1
In a book of this size it is (thankfully) not possible to consider all aspects of occlusion; therefore we will try to concentrate on the practical aspects and leave the more esoteric considerations to other texts. We also suggest that significant occlusal adjustment is rarely indicated and should only be attempted by a specialist.
Definitions
Ideal occlusion
Anatomically perfect occlusion—rare.
Functional occlusion
An occlusion that is free of interferences to smooth gliding movements of the mandible, with absence of pathology.
Balanced occlusion
Balancing contacts in all excursions of the mandible to provide therefore ↑ stability of F/F dentures; not applicable to natural dentition (except rarely in full-mouth reconstruction).
Group function
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


