Chapter 6
Oral Cancer and Premalignant Lesions
Aim
This chapter describes the diagnosis and management of oral cancer.
Outcome
After reading this chapter you should have an understanding of the management of oral cancer and be familiar with those conditions that are premalignant.
Introduction
Squamous cell carcinoma arising from the surface epithelium accounts for approximately 90% of all malignant disease affecting the mouth. On a global basis it is the sixth most common cancer to affect humankind. There are marked variations, with the highest incidence in the developing countries, where it is up to the third most common malignancy. In the West it accounts for approximately 4.2% of all cancers, although there are some regional variations, such as a relatively high level in the Bas-Rhin region of France. These variations probably reflect underlying aetiological factors. There is a slightly lower incidence in the US, where it accounts for 2% of all cancers. In the UK there are approximately 3,500 new cases per annum, with a five-year survival rate of around 50%. The survival rate of oral cancer is lower than for many other malignancies, which often have a higher public profile and awareness.
In addition to being the primary site for a malignancy to arise the mouth can also be an area where metastatic disease appears (Fig 6-1).
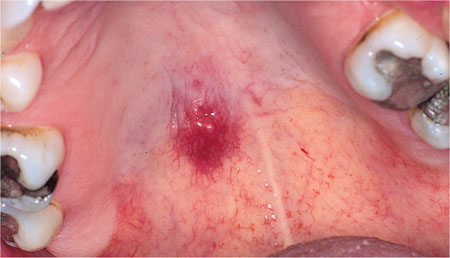
Fig 6-1 Exopytic, highly vascular lesion on palate, which suddenly appeared in a patient with a history of renal carcinoma. This lesion transpired to be a metastasis.
Risk Factors
Although oral cancer can arise in a variety of ‘pre-cancerous conditions’, the majority of cases appear to arise de novo in clinically normal tissue. The aetiology is almost certainly multi-factorial, but there are a number of apparent risk factors:
Age – the prevalence of oral cancer increases with age. In the UK 90% of patients are over 40, although alarmingly there is a rising incidence in those under 35 years old, which may reflect changes in social habits.
Tobacco – tobacco usage in all its forms, whether smoked or chewed, increases the risk of developing oral cancer. There is a smoking history in over 60% of affected patients and in 80% of those where the disease is in the floor of the mouth.
Alcohol – consumption of alcohol above the recommended safe drinking limits (21 units for a male and 14 units for a female) is found in 24% of all patients with oral cancer and in 41% of those whose disease is in the floor of mouth. The combination of heavy tobacco usage and alcohol consumption appears to operate in a multiplicative (synergistic) fashion, producing a 40 times increased risk over those who do not smoke and stay within safe drinking limits.
Areca (Betel nut) – the use of areca nut often in combination with tobacco and other constituents (paan-quid-gutkha) placed in the buccal sulcus and left for considerable periods of time is a relatively common habit among various Asian communities. It is associated with an increased risk of developing squamous cell carcinoma in the mouth.
All the above factors depend, to some degree, on the frequency and duration of use by having a direct local effect. In the case of alcohol and tobacco there may be additional systemic effects.
Other Possible Risk Factors
Other risk factors for oral malignancy include:
-
dietary deficiencies, particularly of vitamins A, C and E and iron, and trace elements such as selenium and zinc
-
viral infections – for example, certain types of human papilloma viruses (HPVs)
-
candidal infection
-
excessive exposure to sunlight or UV radiation (for lip cancer)
-
immune deficiency disease or immunosuppression
-
possible familial or genetic predisposition
-
environmental pollutants
-
mutation of p53 cancer suppression gene – possibly as a result of smoking or HPV infection
-
chronic oral sepsis – this factor may be the result of local irritation to adjacent tissues but also reflects a general poor health awareness.
Clinical Features
Squamous cell cancer of the mouth can present in many ways and can occur at any site, with the most frequent being floor of mouth and ventral/lateral margins of tongue (Fig 6-2). The following clinical signs should be regarded with great suspicion:
-
any ulcer of the mucosa that fails to heal within two to three weeks
-
any area of firmness (induration) of the oral tissue
-
fungation/growth of the tissues to produce an elevated, cauliflower surface or lump
-
fixation of any lesion to underlying tissues with loss of normal mobility
-
failure to heal of a tooth socket, or any other wound
-
tooth mobility with no apparent cause
-
pain/paraesthesia with no apparent cause
-
difficulty in swallowing (dysphagia) for which no other diagnosis can be made
-
white/red patches of the mucosa – these are commonly considered as potentially malignant lesions, but occasionally may represent an early-phase squamous cell carcinoma
-
lymphadenopathy – any large, particularly asymptomatic lymph node in the submental, submandibular and cervical chain area should be regarded with suspicion, and if persistent referred for either surgical removal or fine-needle aspiration cytology.
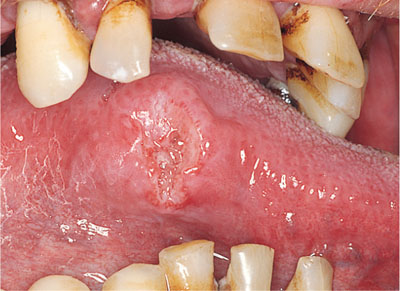
Fig 6-2 Squamous cell carcinoma on lateral margin of tongue.
It should be emphasised, however, that the majority of early oral carcinomas are often entirely asymptomatic.
Management
Squamous cell carcinoma is probably the most life-threatening disorder to affect the mouth and the dental practitioner is in a key position to advise on prevention, its early recognition and appropriate referral for treatment.
As a routine all health care workers should be prepared to give advice regarding known risk factors, in particular smoking and alcohol consumption. A thorough oral examination should always be undertaken and any suspicious lesions noted. Biopsy is obligatory to confirm the diagnosis. If a malignancy is suspected it is best to refer to the appropriate specialist as a matter of u/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


