Chapter 6
Developing Treatment Algorithms for Restoration or Replacement of the Compromised Tooth
The introduction of newer therapeutic modalities, surgical and restorative techniques, and restorative materials has dramatically expanded available treatment options. While a potential boon for clinicians and patients alike, such expansion places greater demands upon the diagnostic and treatment planning capabilities of the clinician. The challenge is not in mastering available surgical and restorative treatment techniques, but rather in determining when to apply each treatment modality, and how to utilize the chosen therapeutic approach to its maximum benefit for the patient.
Treatment decisions should always be made in consideration of the health of the patient, the appropriateness of the therapy, the informed desires of the patient, and the costs of the therapy. Therapeutic costs to be assessed are not only financial, but also biologic, aesthetic, therapeutic, temporal, and psychological. In addition, the prognosis of each therapeutic option over time must be considered.
When faced with a single compromised tooth, treatment options include restoration of the tooth—in conjunction with endodontic, orthodontic, and/or periodontal therapies where necessary—tooth removal and replacement with an implant supported single crown, or tooth removal and replacement with a three-unit fixed partial denture. It is imperative that selection of a specific treatment approach not be grounded in the clinician’s less-than-thorough understanding of the advantages, disadvantages, and potentials of each treatment option.
A clinician’s lack of understanding or experience with a given treatment approach, or failure to master delivery of such therapy, is a poor excuse for selecting one therapeutic option over another. Rather, treatment outcome expectations, the various risks of each therapeutic option, and the prognosis of each treatment approach should be carefully considered and weighed in the decision-making process.
The challenge is how best to quantify the survival rates of recommended procedures and therapies. While excellent documentation is present regarding success and failure rates of specific therapies, the literature is woefully inadequate in assessing treatment outcomes for other modalities. Many articles poorly define patient selection, the overall patient dental health, criteria for success, and other confounding factors. In addition, a number of published reports utilize materials that are no longer employed on a day-to-day basis. Finally, there is a paucity of literature comparing various treatment approaches in the same patients or clinical practices. As a result, while the goal is to render the decision-making process as scientific as possible, a number of “soft” factors influence this process, including clinician bias and perspective. It is for this reason that clinical dentistry is still a unique combination of art and science.
Diagnostic Requirements
Thorough examination and diagnosis must always be carried out and a comprehensive interdisciplinary treatment plan must be formulated prior to initiation of any active therapy, as discussed in Chapter 1. The components of such an examination will not be repeated here. There are, however, key points that bear mentioning. A thorough examination always begins with an open discussion with the patient, so that the patient’s needs and desires may be determined. Failure to ensure such open avenues of communication increases the risk of patient dissatisfaction, and poor treatment outcomes. Thorough data collection is a must. Examination of hard and soft tissues, models with face-bow mountings, and analysis of the patient’s occlusion in conjunction with a high-quality full series of radiographs provide base line data needed for decision making and treatment recommendations. Three-dimensional imaging is often required. Such imaging provides especially important information when assessing the bone support on the palatal root of a maxillary molar, the precise extent of an endodontic lesion that is present, the assessment of available bone if tooth extraction and implant placement are contemplated, and assurance of the absence of other pathologies which may either influence the course of therapy or pose significant health risks to the patient.
All potential etiologies must be identified and assessed prior to formulating a comprehensive treatment plan, including systemic factors, periodontal status, the presence or absence of parafunction, carious lesions, endodontic lesions, and trauma.
As the available treatment options and ideal treatment plan are being formulated for presentation to the patient, it is important that both the predictability and expected treatment outcome of each therapeutic approach be honestly and openly assessed and discussed. Such an assessment allows the patient to choose the treatment option for which he or she is best suited physically, financially, and psychologically.
Teeth that can be predictably restored to health through reasonable means should always be maintained, if such retention is advantageous to the final treatment plan and addresses the patient’s desires and wishes. Once again, lack of understanding about the predictably attainable results following periodontal and/or endodontic therapy, and the expected long-term prognoses of various approaches, often results in formulation of treatment plans that do a disservice to the patient.
It is inappropriate to remove all teeth that show any degree of compromise and replace them with implant-supported prosthetics. However, it is equally inexcusable to fail to understand and incorporate regenerative and implant therapies into available treatment armentaria, when addressing a patient’s unique situation.
The success rates of procedures that have statistical track records can be presented to patients to help them weigh the pros and cons of each therapeutic option. Such data can also be used to support the treatment decisions of the dentist. Unfortunately, the success rate of a particular procedure performed by the practitioner in question, which is of greatest value, is often unavailable statistically. Usually, the dentist can only state that his/her success with this particular procedure is based on the number of times it has been performed successfully. This history of success and/or failure often shapes the treatment plan.
Assessing the Individual Tooth
Prior to making a determination as to the advantages or disadvantages of retaining a given tooth, a number of parameters must be appropriately assessed. Some of these considerations have been discussed in previous chapters and will be briefly reviewed below. A number of salient points to consider include:
The periodontal status of the tooth in question is an absolute indication or contraindication to attempts at long-term maintenance through periodontal and restorative therapies. There is no question that pocket depths in excess of 4 mm are not maintainable by either the patient or the dental professional. Therefore, except in instances where teeth are being maintained in older or medically compromised patients, pocket elimination must be a feasible treatment outcome in order to consider restoration and retention of a given tooth. Such pocket elimination may proceed through periodontal resective therapy, periodontal regenerative therapy, or a combination of the two.
Pocket elimination also includes resolution of any furcation involvements that are present. Performing extensive restorative therapy on a furcated tooth because it demonstrates only a Class I furcation involvement is ill advised. It is well established that such areas will continue to break down, due to the cul de sac which will continue to trap plaque despite the best professional and patient plaque-control measures. There is no argument in the literature over whether or not furcation involvements progress. The only points to be considered are how quickly a given furcation involvement will progress, the impact of such progression upon the planned therapy, and the influence of overriding patient concerns (age, health, etc.).
As discussed in Chapter 4, a stable band of attached keratinized tissue, and hence an intact fiber barrier system, must be present to help provide adequate defense against the added plaque accumulation and potential periodontal compromise inherent in placement of restorative margins at the gingival crest or intrasulcularly. If such a band of attached keratinized tissue cannot be established due to various anatomic or patient psychological considerations, then the tooth is ill suited for restoration and retention.
The Ability to Safely Perform Crown-Lengthening Surgery
The extent of periodontal attachment loss around the tooth in question, and the expected level of periodontal attachment after necessary periodontal therapy is performed, must be assessed. If a stable periodontal milieu may be established for reception of restorative dentistry without unduly compromising the support of the tooth in question, the argument for retaining the tooth is greatly enhanced. However, should the tooth in question demonstrate extensive periodontal attachment loss, or should performance of necessary preprosthetic crown-lengthening osseous surgery significantly alter the crown-to-root ratio of the tooth, the tooth may be a poor candidate for retention.
A minimum of 3–4 mm of healthy tooth structure must be available crestal to the alveolar bone crest to allow both redevelopment of an appropriate attachment apparatus and establishment of the necessary ferrule in the preparation design. If the restorative margin tooth interface is deep subgingival, patient home care is compromised. The resultant increased plaque accumulation may reinitiate not only the periodontal inflammatory process, but also recurrent caries at the aforementioned interface.
Endodontic Considerations
In addition to determining whether or not endodontic therapy can be carried out on a given tooth, care must be taken to assess the expected residual tooth structure following such endodontic intervention, and the ability of this residual tooth structure to withstand load application over time.
Natural tooth contours may result in a thin isthmus of tooth structure following endodontic therapy. Areas of specific concern are two-rooted maxillary first bicuspids, and the furcal aspect of the mesial root of a lower molar. A study reported from the University of Oregon Dental School found that the teeth with the highest endodontic failure rates were mandibular first premolars, followed by maxillary laterals, maxillary first and second premolars, the mandibular second premolar, and maxillary first molars (1).
While root canal systems are generally predictable in morphology, complicating or unique attributes set many teeth apart. Zillich and Dawson (2) describe mandibular first premolars as either easy or exceedingly difficult to treat. This particular tooth will present with a second or third canal 23% of the time. In addition, these canals may divide at any point within the root. Maxillary premolars exhibit variations similar to mandibular premolars, often making them difficult to successfully treat.
Sjogren et al. report 8–10-year success rates of 96% in teeth with vital pulps and 86% if the pulp was necrotic, following endodontic therapy (3). The manner in which the tooth is obdurated affects success. However, endodontic success does not always equate to restorative success. The factors confounding endodontic therapy make restorative options more challenging. Placement of a post in a maxillary or mandibular first premolar that falls in the 23% complex root canal configuration category may be impossible or result in a compromised prognosis, due to the mechanics of preparing the internal aspect of an irregular cavity with walls of varying thickness using a rotary instrument. The absolute and relative contraindications to retention of a given tooth are listed in Table 6.1.
Table 6.1. Relative fees for various therapies.
| Therapy | Fee |
| Endodontics—Single root | 0.9X |
| Endodontics—Multiple root | 1.3X |
| Core buildup—Natural tooth | 0.6X |
| Crown—Natural tooth | 1.3X |
| Pontic | 1.4X |
| Crown-lengthening periodontal surgery | 1.1X |
| Regenerative periodontal surgery | 1.9X |
| Orthodontic supereruption | 2.8X |
| Extraction | 0.3X |
| Three-unit fixed bridge | 4.3X |
| Implant | 2.1X |
| Implant abutment (stock) and crown | 2.2X |
| Implant abutment (custom) and crown | 2.7X |
| Regenerative therapy at tooth extraction | 0.7–1.4X |
| Sinus augmentation | 2.5X |
| Osteotome sinus lift | 0.9X |
| Osteotome sinus lift at time of implant placement | N/C |
Periodontal stability, defined as no probing depths greater than 3 mm and no horizontal furcation involvements, must be attainable so as to provide a milieu that is accessible to the patient for effective home-care measures. The inability to do so is an absolute contraindication to tooth retention.
The inability to perform the necessary endodontic therapy on the tooth in question must also be seen as an absolute contraindication to tooth retention.
If tooth extraction and implant placement are to be contemplated, it is important to realize that such a treatment choice does not preclude the need for appropriate diagnosis and assessment before carrying out therapy.
Implant Receptor Site Considerations
The implant option is not without its own set of conditions, which need to be evaluated.
A number of site-specific factors must be considered if tooth removal and implant placement are to be entertained. The position of the implant recipient bone is of paramount importance, as are the quantity and quality of the available bone. A malpositioned tooth may result in an extraction socket whose position precludes ideal implant positioning without either regenerative therapy at the time of tooth extraction followed by subsequent implant placement, or concomitant regenerative therapy at the time of tooth removal and implant insertion.
It is crucial that the assessment of bone quantity be carried out in a three-dimensional manner. All too often, such an assessment is limited to evaluating the length of the implant that may be placed, and whether or not the implant will be inserted wholly within an intact extraction socket. Such an assessment is inadequate. A patient with a thin, highly scalloped biotype or one who has undergone buccal orthodontic tooth movement, or has caused hard- and soft-tissue recession through aggressive brushing, will demonstrate a thin, highly labile buccal alveolar bony plate following tooth removal. Placement of an implant in such a situation without concomitant regenerative therapy to protect and increase the bulk of the buccal bone will leave the patient with a situation highly prone to either postoperative bone resorption, or bone resorption upon application of functional load. Any implant placed must be housed in adequate bone to withstand functional forces buccally and lingually/palatally, over time.
Assessing Cost-Benefit Ratios
In dentistry, extrapolation is made from the combined experience of treating many patients and evidence from literature when making treatment decisions. However, it is important to realize that humans are unique, and one case may not have the same outcome as others treated in the same manner. A risk-reward benefits analysis must be undertaken to help determine the most reasonable approach to a given situation. The development of an appropriate treatment algorithm mandates recognition and evaluation of all applicable cost-benefit ratios. These cost-benefit ratios are biologic, esthetic, financial, temporal, psychological and therapeutic in nature. Appropriate assessment must also take into consideration not only the present, but also the future status of the treatment delivered.
BIOLOGIC CONSIDERATIONS
Biologic costs impact both the tooth under direct consideration and adjacent teeth. The tooth being assessed may pay a biologic price in terms of loss of tooth structure following preparation with or without endodontic intervention, loss of supporting bone following preprosthetic periodontal therapy when necessary, or development of furcation involvements following preprosthetic crown-lengthening osseous surgery.
CLINICAL EXAMPLE ONE
A patient presents with a subgingival fracture on the buccal aspect of a mandibular first molar (Fig. 6.1). This tooth has already undergone endodontic therapy. Radiographic examination (Fig. 6.2) demonstrates the short residual root trunk which is present between the root fracture and the entrance to the buccal furcation. Due to the short distance between the subgingival margin of the buccal fracture and the entrance to the furcation (approximately 1.3 mm), performance of the necessary crown-lengthening osseous surgery would result in development of a significant buccal furcation involvement, and a compromised prognosis for the tooth following completion of therapy.
Fig. 6.1 A patient presents with a buccal subgingival fracture of a mandibular first molar.
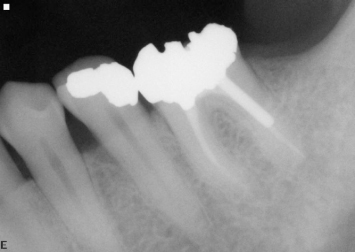
Fig. 6.2 Radiographic examination demonstrates a short residual root trunk between the fracture and the entrance to the buccal furcation. Performance of crown-lengthening osseous surgery would result in a significant buccal furcation involvement on the first molar.
Removal of such a tooth and its replacement by an implant with concomitant regenerative therapy may appear at first to be an overly aggressive treatment approach. The argument might be made that the patient would be better served by placing a crown on the tooth and “trying to hold on to it for as long as possible,” especially as endodontic therapy had been performed some years before. However, such a treatment option is not in the best interest of the patient unless patient health precludes more comprehensive care, or patient age leads the clinician to believe that the tooth will not have to function for much longer.
Post and core build-buildup and a full coverage restoration without periodontal surgical therapy entails significant expense, and will result in a milieu that institutes a periodontal inflammatory lesion almost immediately upon completion of tooth restoration. At best, the disease process will proceed slowly. At worst, the tooth will become significantly compromised and periodontally untreatable in the near future.
Performance of crown-lengthening osseous surgery prior to post and core buildup and full-coverage restoration of the tooth will entail additional expense, and will not provide a periodontal milieu conducive to placement of restorative dentistry without the initiation of an inflammatory periodontal lesion. Conservative therapy is removal of the tooth, placement of an implant, and subsequent restoration so as to provide a healthy, functional situation for the patient.
The biologic costs to the adjacent teeth must also be considered. If crown-lengthening osseous surgery performed around a giv/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


