Chapter 1
Examination and Diagnosis
The periodontal prerequisites for maximization of long-term oral health are well established. Effective home-care efforts, maintainable probing depths (defined as 3 mm or less), no evidence of furcation involvements, and adequate bands of attached keratinized tissue to provide a stable fiber barrier in various clinical scenaria are well-accepted periodontal endpoints of therapy. Combined with appropriate management of carious and endodontic lesions, replacement of missing teeth, control of parafunctional habits, and establishment of a healthy, stable occlusion, such a periodontal milieu will help ensure maximization of patient comfort, function, and aesthetics in both the short and long terms.
It has become popular to speak of paradigm shifts in clinical dentistry. However, these shifts represent nothing more than alterations in the treatment approaches utilized to attain the aforementioned therapeutic goals. In addition, efforts must be made to utilize the least-involved and least-expensive therapies possible for ensuring these treatment outcomes.
Maximizing oral health and ameliorating patient concerns remain essential to ethical practice. When considering the utilization of various treatment approaches, it is important to listen to patient desires, determine patient needs, and ensure that the therapy to be employed is truly in the best interest of the patient. A thorough understanding of the predictability of appropriately performed therapies around natural teeth is crucial to the formulation of an ideal treatment plan for a given patient. This treatment plan is based upon a precise diagnosis of the patient’s condition and recognition of all contributing etiologies. Such a diagnosis takes into consideration the patient’s overall health and the entire dentition, treating each site as both an individual entity and as a component of the masticatory unit.
Establishment of such oral health is dependent upon first carrying out a thorough examination, so as to establish a comprehensive diagnosis of patient etiologies, needs, and required therapies.
Establishing an Appropriate Treatment Plan
A high-quality full series of radiographs must be taken. All full series of radiographs must employ two film/sensor sizes: a #2 film/sensor in posterior regions and a #1 film/sensor in anterior areas. Attempts at utilizing either a #1- or #2-size film/sensor in all areas of the mouth will result in an inability to properly position the film/sensor in the anterior regions, and lead to poorly angulated, nondiagnostic radiographs. Digital radiographs are preferable, due to the ability to manipulate the images and thus gain additional information, and the lesser radiation exposure to the patient. When necessary, three-dimensional images are utilized. Panorex films are not used, since their accuracy is not sufficient for providing useful information for constructing a comprehensive diagnosis.
The components of a thorough clinical examination include periodontal probing depths, assessment of clinical attachment levels, hard- and soft- tissue examination, models, and face-bow records. However, it is important to realize that a thorough examination begins with an open discussion with the individual patient, as a step in determining the patient’s needs and desires. In this way, treatment plans may be formulated that are in the best interest of the patient and represent a greater value for the patient.
Prior to formulating a comprehensive treatment plan, all potential etiologies must be identified and assessed. In addition to systemic factors, these etiologies include, but are not limited to, periodontal disease, parafunction, caries, endodontic lesions, and trauma.
The treating clinician should always formulate an “ideal” treatment plan and present it to every patient. Appropriate and predictable treatment alternatives must be offered to the patient as well, to allow the patient to choose the treatment option to which he or she is best suited physically, financially, and psychologically.
In many situations, initial therapies, such as plaque control instruction, debridement, caries control, and endodontic assessment, must be carried out prior to establishment of the final treatment options.
While it is true that clinicians who fail to incorporate regenerative and implant therapies into their treatment armamentaria are depriving their patients of predictable therapeutic possibilities that afford unique treatment outcomes in a variety of situations, other proven therapies should not be abandoned too quickly.
Teeth that can be predictably restored to health through reasonable means should be maintained, if their retention is advantageous to the final treatment plan. Clinicians who claim to be implantologists, performing only implant therapy while ignoring periodontal and other pathologies, do patients a disservice. Such clinicians include practitioners who either perform inadequate periodontal therapy to predictably halt the disease process, or remove teeth that could be treated through predictable periodontal techniques.
It is inconceivable that any clinician would see only patients who require implant therapy, and demonstrate periodontal, endodontic, restorative, and occlusal health around all remaining teeth that are not to be extracted. Such a clinical outlook is at the expense of ethical, comprehensive care, and must be avoided at all times.
Clinical presentations of different patients may appear similar, despite dramatic differences in etiology and individual patient needs. It is crucial that the conscientious clinician utilize all tools at his or her disposal to differentiate between various clinical entities.
It is also imperative that the periodontal restorative dynamic be understood in its complexity, and managed comprehensively, to maximize treatment endpoints. All periodontal therapies have restorative ramifications. Similarly, all restorative therapies have periodontal ramifications. One of the goals of the conscientious clinician must be to determine the relative influence of each discipline on the treatment considered in a given clinical scenario, and manage all aspects of this interrelationship appropriately.
Most if not all clinicians would agree that reconstructive therapy must be grounded in sound periodontal prosthetic principles. It is important to realize the same is true for a single restoration.
Periodontal procedures cannot be considered without understanding their far-reaching restorative ramifications. All therapies succeed or fail depending upon how periodontal and restorative concerns are managed, both individually and as interdependent entities.
The introduction by Amsterdam and Cohen (1) of the concept of periodontal prosthesis almost 50 years ago helped to define this interrelationship. While complex, state of the art therapies were presented and the results were documented over decades, such execution was not the greatest contribution the concepts of periodontal prosthesis have made to modern clinical practice. Rather, periodontal prosthesis afforded clinicians something even more important. A system was presented by which comprehensive record taking, diagnosis, and treatment planning could be carried out with specific treatment endpoints in mind, resulting in long-term therapeutic success. The advent of implant therapy has done nothing to change this concept. Comprehensive care mandates thorough examination and record taking, a multifactorial diagnosis, and interdisciplinary treatment planning to maximize therapeutic outcomes. Case types may be categorized as follows.
THE PERIODONTAL RESTORATIVE CASE
A patient presents with significant periodontal concerns, manifesting themselves as hard- and soft-tissue changes, deepening pocket depths, and inflammation. In these situations, restorative therapy may be required to help improve the outcomes of comprehensive periodontal treatment. Restorative therapy often includes splinting of mobile teeth, coverage of sensitive roots, and correction of occlusal abnormalities to improve periodontal prognoses.
It is important to realize that while less mobility is always desirable, increased mobility patterns should not be viewed as a contraindication to periodontal or restorative therapies of various complexities. Increased mobility, if it is not to such a degree as to result in either continued dysfunction or tooth extraction, will not negatively impact long-term prognosis to a significant degree. However, should fixed partial dentures be contemplated to replace a missing tooth or teeth, additional teeth may be required to serve as abutments in the presence of increased tooth mobility, to afford the necessary stability to the fixed partial denture under function. Increasing mobility should be viewed as a highly significant negative factor when determining expected prognoses for various therapies, and may be an absolute contraindication, to performing complex treatments on given teeth rather than removing these teeth and replacing them with implant-supported prosthetics. This type of case will not be discussed in detail, as it is not the purpose of this text.
THE RESTORATIVE PERIODONTAL CASE
Maximization of long-term restorative treatment outcomes is highly dependent upon the periodontal milieu into which restorative therapy is placed. A harmonious occlusion, probing depths of 3 mm or less, no horizontal furcation involvements, stable bands of attached keratinized tissue of at least 3 mm in the apico-occlusal dimension and 2 mm in the buccolingual dimension, and restorative margin positions that are accessible to the patient for predictable home-care efforts are all prerequisites for attainment of successful restorative treatment outcomes.
The methods available to attain these goals will be discussed in detail throughout the text. A restorative periodontal case is one that requires periodontal intervention not to eliminate active periodontal diseases, but rather to appropriately prepare the periodontium for reception of restorative dentistry. Such therapies may include, for example, hard- and/or soft-tissue crown lengthening, soft-tissue augmentation, ondontoplasty, and frenectomy.
INTRODUCTION OF ORTHODONTIC THERAPY INTO EITHER CASE TYPE
Although this is not the format in which to discuss complex full-mouth orthodontic therapy, appropriate utilization of orthodontic treatment approaches in isolated areas will significantly enhance the functional and aesthetic outcomes of therapy in both periodontal restorative cases and restorative periodontal cases. Such orthodontic utilization includes:
- alignment of malpositioned teeth to improve ease of patient home care
- alignment of malpositioned teeth to ameliorate off-angle functional and parafunctional forces
- establishment of more ideal occlusal planes
- establishment of flatter occlusal planes with shallower incisal guidance to help ameliorate forces being placed upon the anterior teeth
- tooth reangulation for ease of prosthetic therapy
- tooth reangulation to assist in patient home-care efforts
- tooth uprighting to help eliminate cementoenamel junction position induced osseous defects (Figs. 1.1–1.6)
- tooth supereruption in anticipation of crown-lengthening osseous surgery in the aesthetic zone, to allow appropriate restoration and maintenance of a compromised tooth without negatively affecting patient aesthetics and/or allow crown lengthening without compromising the support of the adjacent teeth (Figs. 1.7–1.15)
- supereruption prior to tooth extraction to extrude hard and soft tissues, improve aesthetics in the papillary and/or marginal areas, and afford site preparation in anticipation of either pontic or implant crown placement (Figs. 1.16–1.20)
Fig. 1.1 A mesially tilted second molar demonstrates an infrabony defect due to cementoenamel junction positions.
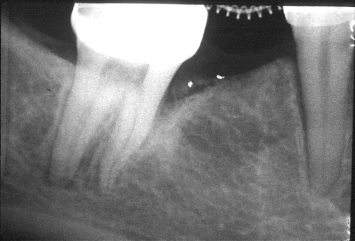
Fig. 1.2 Orthodontic uprighting of the tilted molar is beginning to eliminate the infrabony defect that was present.
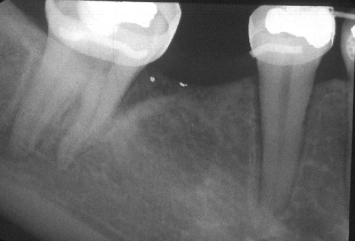
Fig. 1.3 The molar has been brought into an appropriate position. No infrabony defect remains. Note the “bone regeneration” on the mesial aspect of the molar.
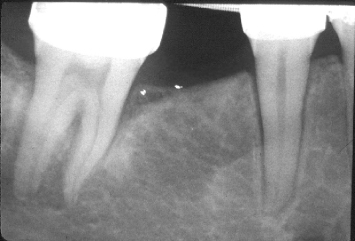
Fig. 1.4 A severely tilted second molar demonstrates an “infrabony defect” on its mesial aspect. Note the positions of the cementoenamel junctions.
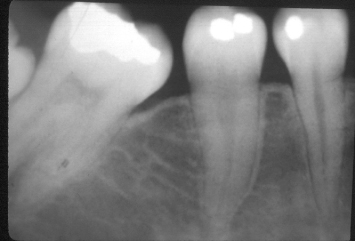
Fig. 1.5 Molar uprighting is proceeding. Note the elimination of the defect on the mesial aspect of the molar.
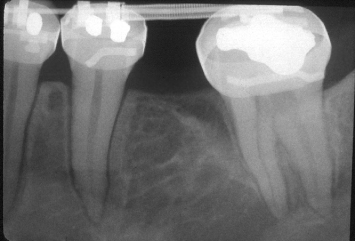
Fig. 1.6 Upon completion of orthodontic uprighting, no infrabony defect remains on the mesial aspect of the second molar.
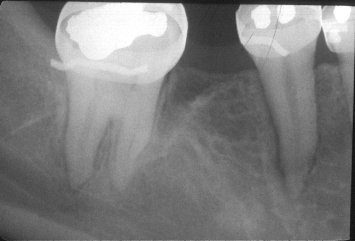
Fig. 1.7 A 51-year-old female presents with caries on her mandibular right first and second premolars. The caries on the first premolar extends approximately 3 mm apical to the alveolar crest. Attempts at crown-lengthening osseous surgery around the first premolar would require removal of extensive supporting bone from the adjacent teeth.
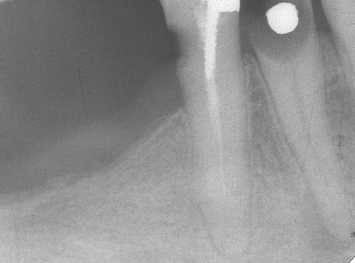
Fig. 1.8 A laboratory view of the fixed orthodontic appliance that will be cemented in place and will engage the root of the mandibular first premolar.
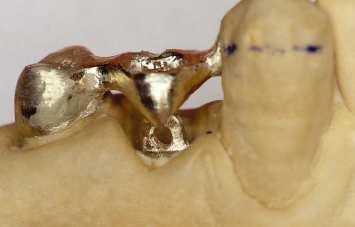
Fig. 1.9 A lingual view of the fabricated orthodontic appliance.
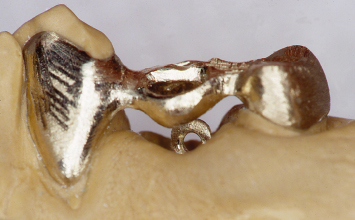
Fig. 1.10 A lingual view of the orthodontic appliance in place. The area is temporized around the appliance to help ameliorate the patient’s aesthetic concerns.
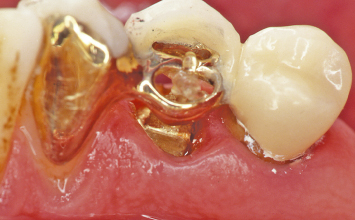
Fig. 1.11 A buccal view of the supereruptive appliance and temporary prosthesis in place.
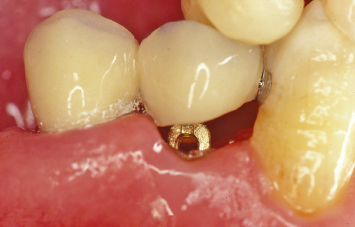
Fig. 1.12 Following supereruption of the root of the mandibular first premolar, crown-lengthening osseous surgery may now be performed without unduly compromising the alveolar support of the adjacent teeth.
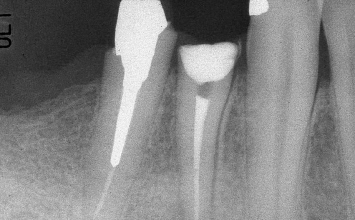
Fig. 1.13 Crown-lengthening osseous surgery has been performed around both mandibular premolars.
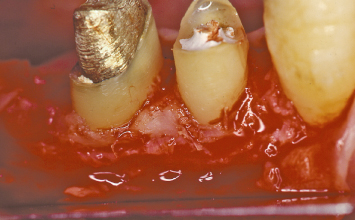
Fig. 1.14 Following suturing of the mucoperiosteal flaps at alveolar crest and replacement of the provisional restoration, the extent of crown lengthening that has been attained is evident.
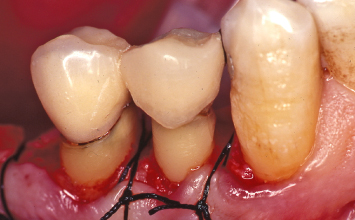
Fig. 1.15 A radiograph taken after post and core fabrication and insertion into the mandibular premolars demonstrates the relationship of the planned restorative margins to the alveolar crests.
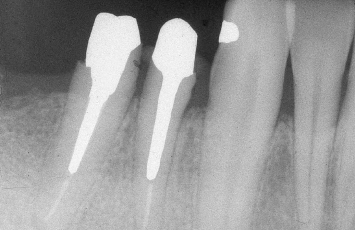
Fig. 1.16 A 62-year-old male presents with a hopeless prognosis for his maxillary left first premolar. Note the extensive bone loss around this tooth, which is affecting the support of the adjacent teeth.
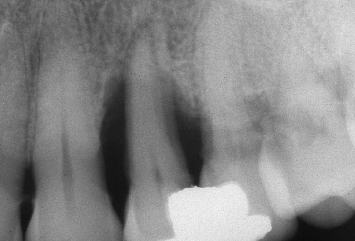
Fig. 1.17 Following orthodontic supereruption of the hopeless maxillary left first premolar, the osseous defects that were present have been resolved, with no loss of alveolar bone on the facing surfaces of the adjacent teeth. The patient now presents with an ideal alveolar crest for implant placement, and maximization of the periodontal health of the adjacent teeth.
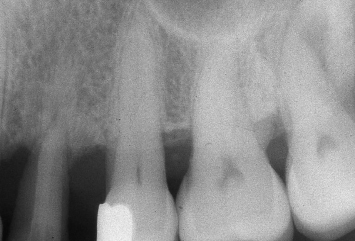
Fig. 1.18 The alveolar bone crest, which has been repositioned through orthodontic supereruption, is evident following implant placement in the maxillary left first premolar position.
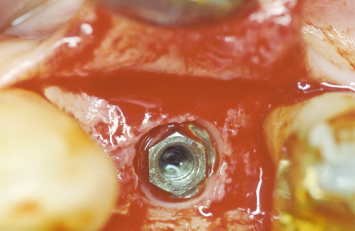
Fig. 1.19 The mucoperiosteal flaps are sutured in the desired positions with interrupted silk sutures.
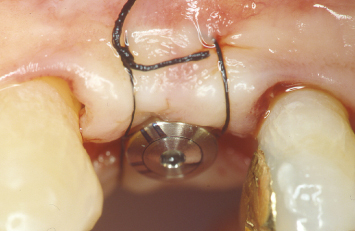
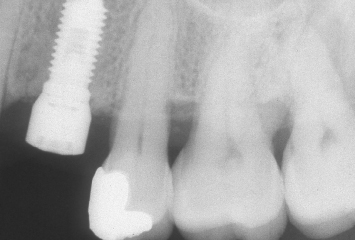
Fig. 1.20 A radiograph taken after implant placement demonstrates the ideal contour and position of the alveolar crest, which was rebuilt utilizing orthodontic supereruptive techniques.
CLINICAL EXAMPLE ONE
A 51-year-old female presents with extensive caries on her mandibular right first and second premolars. The caries on the first premolar extends approximately 3 mm apical to the osseous crest. Attempts at crown-lengthening osseous surgery would result in removal of extensive and significant supporting alveolar bone from the distal aspect of the cuspid and the mesial aspect of the second premolar (Fig. 1.7).
Following caries excavation on both mandibular premolars, an impression is taken and a fixed orthodontic appliance is fabricated, which will be utilized to supererupt the root of the first premolar. This orthodontic appliance will be fixed to the cuspid and second premolar, and will engage a specifically designed post in the root of the first premolar (Figs. 1.8, 1.9). Once the orthodontic appliance is inserted, a temporary provisional restoration is placed over both the first and second premolars to help satisfy the patient’s aesthetic concerns (Figs. 1.10, 1.11). Following supereruption of the root of the first premolar, the orthodontic appliance and the orthodontic post in the root of the first premolar are removed. A radiograph taken at this time demonstrates that the supererupted mandibular first premolar can now be safely crown lengthened without compromising the prognoses of the adjacent teeth (Fig. 1.12).
Crown-lengthening osseous surgery is carried out (Fig. 1.13). The technical aspects of this therapy will be described in detail in Chapter 2. Following suturing of the buccal and lingual mucoperiosteal flaps at osseous crest with interrupted silk sutures, the provisional restorations are replaced on the crown-lengthened first and second mandibular premolars (Fig. 1.14). The extent of crown lengthening that has been attained is evident. A radiograph taken following post and core buildup and preparation of the mandibular right first and second premolars demonstrates that adequate dimensions are present between the planned restorative margins and the osseous crest to allow development of a healthy periodontal attachment apparatus. Neither the cuspid nor second premolar have been compromised by the crown-lengthening therapy that has been carried out (Fig. 1.15).
CLINICAL EXAMPLE TWO
A 62-year-old patient presents with a periodontally hopeless maxillary left first premolar. Radiographically, extensive osseous loss is present around this tooth. In addition, the thin nature of the remaining supporting alveolar bone on the distal aspect of the maxillary cuspid and the mesial aspect of the maxillary second premolar is evident (Fig. 1.16). Extraction of the first premolar and performance of simultaneous regenerative therapy, with or without implant placement, would place this thin supporting alveolar bone at risk, and potentially compromise the long-term prognoses of the cuspid and second premolar.
Following orthodontic supereruption of the hopeless root of the first premolar, both resolution of the aforementioned periodontal defect and maintenance of all supporting bone on the adjacent teeth are evident (Fig. 1.17). This root may now be extracted and an implant safely placed, without compromising the prognoses of the adjacent teeth.
Following reflection of buccal and palatal mucoperiosteal flaps, an implant is placed in the position of the maxillary left first premolar (Fig. 1.18). The interproximal alveolar bone, which has been maintained and rebuilt through orthodontic supereruption, is evident. The mucoperiosteal flaps are sutured at the desired positions, utilizing interrupted 4-0 silk sutures (Fig. 1.19). A radiograph taken following implant placement demonstrates an ideal alveolar ridge form and the health of the periodontal attachment apparatus on the facing surfaces of the adjacent teeth (Fig. 1.20).
CLINICAL EXAMPLE THREE
A 47-year-old female presents with a fractured maxillary central incisor (Fig. 1.21). A radiograph demonstrates extensive bone loss between the fractured maxillary central incisor and the adjacent lateral incisor (Fig. 1.22). Extraction of this tooth, with or without concomitant regenerative therapy and/or implant placement, would result in significant shrinkage of the soft tissues and loss of the interdental papilla in the region.
Fig. 1.21 A 47-year-old female presents with a fractured maxillary central incisor.
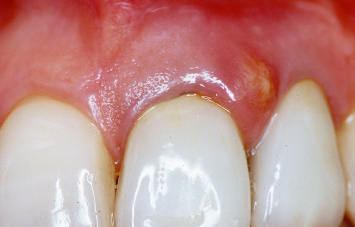
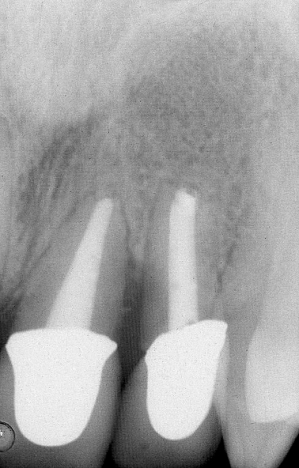
Fig. 1.22 Significant bone loss is evident radiographically between the fractured central incisor and the adjacent lateral incisor.
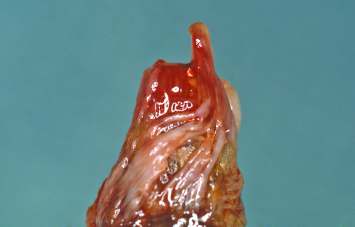
Following removal of the fractured portion of the central incisor, the root is supererupted with a fixed orthodontic appliance (Fig. 1.23). A radiograph taken during the supereruptive process demonstrates how the attachment apparatus and alveolar bone have been “brought coronally” along with the retained root of the maxillary central incisor (Fig. 1.24). The retained root is extracted without reflecting a flap, so as to minimize trauma to the hard and soft tissues in the area (Fig. 1.25). Examination of the extracted root demonstrates the orientation of the periodontal ligament fibers, which results during supereruption (Fig. 1.26). The attachment of these fibers to the surrounding alveolar bone is critical when this bone is to be repositioned coronally.
Fig. 1.23 Following removal of the fractured portion of the central incisor, the retained root is supererupted utilizing a fixed orthodontic appliance.
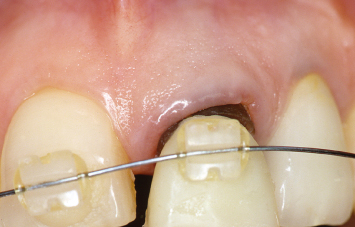
Fig. 1.24 A radiograph taken during the supereruptive process demonstrates coronal repositioning of the alveolar bone between the central and lateral incisors.
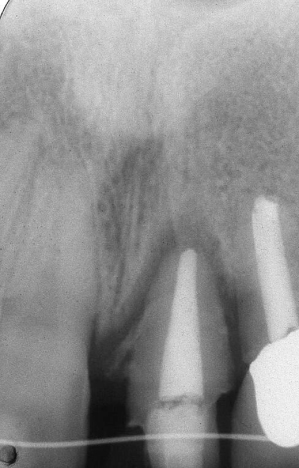
Fig. 1.25 The retained root of the central incisor is removed without reflecting a mucoperiosteal flap, so as to minimize trauma to the hard and soft tissues in the area.
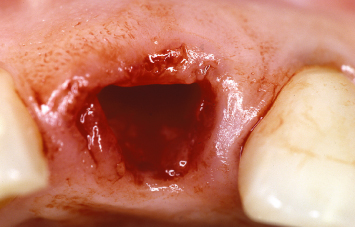
Fig. 1.26 Note the orientation of the periodontal ligament fibers on the root surface, as a result of the supereruptive process.
Following implant placement, retention of the interproximal soft-tissue papillae is evident (Fig. 1.27). The volume of bone that has been brought into position on the mesial aspect of the lateral incisor is highlighted in a radiograph taken following implant placement (Fig. 1.28). This alveolar bone will be crucial to the support and maintenance of the interproximal papilla, and thus the patient’s aesthetics following completion of therapy. Retention of the interproximal papillae and acceptable aesthetics are noted following temporization of the implant (Fig. 1.29).
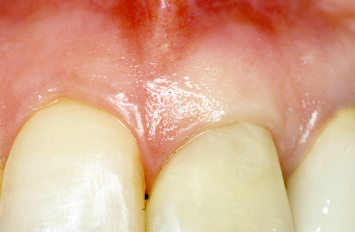
Fig. 1.27 Following implant placement, the soft-tissue papillae have been maintained.
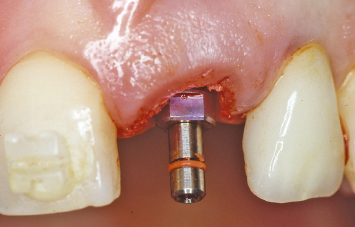
Fig. 1.28 A radiograph taken following implant placement demonstrates the extensive repositioning of the alveolar bone which has taken place on the mesial aspect of the lateral incisor. This bone will be crucial to the support and maintenance of the interproximal soft-tissue papilla.
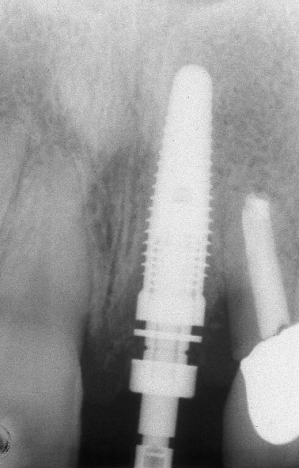
Fig. 1.29 Following implant temporization, retention of the interproximal papilla between the implant and the lateral incisor is evident.
While supereruption offers considerable potential clinical advantages, it is imperative that the possible disadvantages of such therapy be recognized and considered when formulating a comprehensive treatment plan. These disadvantages include the time and expense involved in supereruption. In addition, supererupting a maxillary lateral incisor to the point where it will demonstrate a poor crown-to-root ratio following restoration is not in a patient’s best interest. Orthodontic considerations will be discussed in Chapter 6.
INTRODUCTION OF REGENERATIVE AND/OR IMPLANT THERAPIES
Such treatments may impact the partially edentulous patient on a number of levels, including replacement of less-predictable therapies, replacement of more costly therapies, augmentation of existing therapies, introduction of newer therapies, and simplification of therapy. Use of implants is not the topic under consideration in this text. For a detailed discussion, see Fugazzotto (2009) (2).
Regardless of which therapeutic approaches are utilized, maximization of treatment outcomes is dependent upon identification of etiologic factors, a thorough and insightful diagnosis, and formulation of a multidisciplinary, comprehensive treatment plan. The importance of these considerations is highlighted in the two cases presented below.
CLINICAL EXAMPLE FOUR
A 57-year-old male, presented with severe wear of his maxillary and mandibular anterior teeth, caries on many older restorations, and general aesthetic dissatisfaction (Figs. 1.30, 1.31). Prior to formulating a treatment plan and initiating active therapy, a determination must be made as to whether or not this is an example of tooth wear and loss of vertical dimension, or if vertical dimension has been maintained as the anterior teeth have worn due to the presence of a parafunctional habit. Examination of the occlusal surfaces of the maxillary and mandibular posterior teeth (Figs. 1.32, 1.33) demonstrates retention of the anatomy initially developed in the restorations and a lack of occlusal wear. Loss of vertical dimension has not occurred.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


