(b) 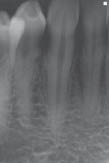
What caused the tooth to become discoloured?
In this case, the tooth discoloured as a result of the trauma, and subsequent pulp necrosis caused by her son accidentally hitting the tooth with his toy. Pulpal haemorrhage may have resulted in blood products (for example, haemoglobin and haematin) penetrating the dentinal tubules. In addition, pulp necrosis produces noxious by-products which may also have penetrated the dentinal tubules; this would result in the tooth becoming discoloured.
Diagnosis and treatment planning
What was the diagnosis and treatment plan?
The diagnosis was a discoloured tooth caused by a necrotic pulp.
The patient was advised that the tooth should be root treated, and ideally bleached internally to improve its appearance.
What are the possible consequences of not treating the tooth?
- Eventually, the tooth may become symptomatic, and the patient may develop pain and/or swelling (for example, acute periapical periodontitis).
- The tooth may become progressively darker, and this staining may ultimately be harder to remove.
The patient agreed to proceed with root canal treatment and subsequent bleaching.
Treatment
The endodontic treatment was carried out in a single visit under local anaesthetic and rubber dam. The access cavity encompassed the pulp horns which contained necrotic pulp tissue. Too small an access cavity design would, firstly, result in failure to completely ‘lighten’ the shade of the tooth as necrotic tissue would have been left behind in the pulp horns, and secondly, may result in the tooth discolouring again.
The root was prepared with a combination of stainless steel hand files and nickel–titanium rotary files, and irrigated with sodium hypochlorite. The root canal was then obturated with gutta-percha and sealer to just below the cemento–enamel junction. The exposed gutta-percha was sealed over with a 3 mm sub-seal of glass ionomer to prevent any of the bleaching agent from potentially diffusing apically through the root filling material. Sealing the cemento–enamel region of the tooth has been shown to reduce the occurrence of external cervical resorption. The use of sodium hypochlorite as an irrigant resulted in a slight improvement of the shade of the tooth; this was not surprising as sodium hypochlorite is a bleaching agent.
The access cavity was then conditioned with phosphoric acid to expose the dentinal tubules, thus improving the penetration of the bleaching gel into the dentinal tubules. Hydrogen peroxide (35%) bleaching gel was then applied into the access cavity and also onto the labial aspect of the tooth. The bleaching gel was replaced every 10–15 minutes with a fresh mixture of gel until the tooth lightened up to a satisfactory level (Figure 6.1.2a). With this ‘non-vital power bleaching’ technique, it is essential that the exposed gingivae are protected with a caulking agent to prevent these tissues being burnt with the bleaching gel. The access cavity was then restored with a permanent glass-ionomer restoration (Figure 6.1.2
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


