(b) 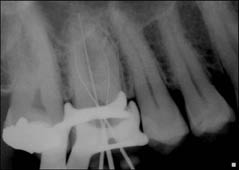
Diagnosis and treatment planning
A diagnosis of irreversible pulpitis was reached for the 16.
The following treatment options were discussed with the patient:
- Root canal treatment.
- Extraction, and brief discussion on replacement options (implant retained crown, fixed bridge).
- Leave alone (not advisable as the current symptoms may continue with the risk of the development of an acute apical abscess).
The patient was keen to retain his tooth and opted for root canal treatment. Before commencing treatment the patient was advised that the existing crown may have to be removed during or replaced after treatment was completed if caries or fracture lines were detected in the underlying tooth, or if the canal entrances could not be easily identified.
Treatment
The tooth was treated under local anaesthetic and rubber dam in a single visit. The working length was determined with an apex locator, after which a working length radiograph was taken to confirm the apex locator lengths (Figure 4.2.1b).
What should be taken into consideration when preparing an access cavity?
Access cavity design is crucial for the outcome of the root canal treatment. A poorly designed access cavity may result in failure to locate all the root canals, difficulty instrumenting the identified canals and increased likelihood of instrument separation. The objectives of access cavity preparation are to:
- Remove the roof and contents of the pulp chamber.
- Provide straight-line access into each root canal. This will allow unimpeded access into the coronal-third of each root canal and reduce the incidence of canal aberrations and instrument separation when using stainless steel or nickel–titanium instruments.
- Ensure that there is adequate resistance form to facilitate temporization of the access cavity between appointments.
- Prevent damaging the floor of the pulp chamber.
- Be as conservative as possible whilst trying to achieve the above objectives.
The classical ‘textbook’ access cavities of easily identifiable root canal entrances located at the base of a wide pulp chamber are infrequently found in the real life clinical setting. As teeth age, the pulp chamber (and root canals) become smaller as a result of secondary dentine deposition; this may be exacerbated by deposition of tertiary dentine in response to caries and microleakage.
Clinical examination may reveal the angulation and any rotation of the tooth/coronal restoration in relation to the root(s). The cement–enamel junction and furcation indicate the level of the canal entrances.
What information may be gained from the pre-treatment (diagnostic) radiograph which may aid access cavity preparation and canal preparation?
- Position and dimensions (width and height) of the pulp chamber.
- Pulp stones or other calcifications of the pulp tissue.
- Position of pulp horns.
- Carious lesions.
- Number and degree of curvature of the roots and root canals.
- Dimensions of coronal restorations.
In general, the number and position of root canals determines the dimensions of any access cavity. It is essential to use magnification in cases where the canals may be difficult to locate (for example, small pulp chambers, teeth restored with crowns). This improves visibility, thus reducing the likelihood of perforating the pulp chamber floor and removing unnecessary amounts of sound dentine whilst locating the root canal entrances.
In this case, four root canals were identified and prepared 0.5 mm short of the apex locator ‘0’ reading. Stainless steel files were used initially to ‘scout’ each root canal, and then to create a glide path to the working length. Nickel–titanium (NiTi) instruments were used to prepare the canals using a crown-down technique. The root canals were irrigated with copious amounts of sodium hypochlorite; patency was maintained throughout canal preparation with a size 10 stainless steel file. The root canals were then dried with paper points, and obturated with gutta-percha and root canal sealer using warm vertical compaction (Figures 4.2.2).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


