Chapter 5
Establishing a Dental Home
The recognition of and treatment for Early Childhood Caries (ECC) has been a major concern for the dental profession. Indeed, concerns about the dental treatment directed toward infants were reported at the beginning of the twentieth century (Cunha et al. 2000), and surveys have shown that caries in primary teeth have increased for two- to five-year-olds (Dye 2007). To combat this form of early dental caries, pediatric dentists in the 1980s began recommending that dental examinations for children should commence at one year of age or earlier.
Education, a less costly alternative, also has been a focus in solving the ECC problem. One of the earliest centers for delivering an educational program was the Baby Clinic, established in 1986 at the Londrina State University in Brazil. The aim of the Baby Clinic was to provide education to parents and to maintain or re-establish a good oral health status, creating a positive attitude in parents and children toward dentistry (Cunha et al. 2000). Education for improving oral health starts very early, and lectures on prevention of oral diseases are included in prenatal delivery preparation courses for parents (Soderling et al. 2000; Casamassimo 2001). A similar model was introduced in the United States and termed the Dental Home. This relatively new concept, with its prevention potential, has been included in the Guidelines of the American Academy of Pediatric Dentistry (2010). Reports describing new programs indicate the profession’s acceptance of this approach, and indeed, an entire book has been published recently on infant dentistry (Berg and Slayton 2009).
This chapter approaches the dental home from a different viewpoint—the patient management perspective. How can the dental home have an impact on future child dental behavior and the relationship between the pediatric dentist and parent? The chapter also presents the technical aspects of examining and managing a one-year-old child, the recommended age to establish a dental home. The management of a one-year-old presents the clinician with entirely different circumstances as compared to older children. Although there is only a year separating a one-year-old from a two-year-old child, there are great cognitive, physical, and dental differences (see Chapter Two).
All of the patient management techniques discussed in the preceding and following chapters have in common the need for effective communicative management. This leads to the conclusion that there is a need for a congenial relationship. Proper patient management and treatment can be achieved in a friendly, familiar environment. This concept has been labeled the “medical home” by our pediatric medical colleagues. The medical home concept was introduced by the American Academy of Pediatrics in 1967. At the time it was envisioned as a central source for all the medical information about a child. It focused primarily on those with special needs and in low socioeconomic groups, as underprivileged children were seeking basic medical treatment in hospital emergency rooms. In 1992 the concept was expanded and the medical home was defined as a strategy for delivering the family-centered, comprehensive, continuous, and coordinated care for all infants and children. In 2002, the organization further extended and operationalized the definition, including the requirement that each patient have an ongoing relationship with a personal physician trained to provide first contact and continuous, comprehensive care. The medical home is now applied to all children and suggests that a strategy be developed that ensures a familiar health care provider for each family. This concept argues for a place that does not change each year with the vagaries of the third-party payment system, governmental support, or practitioner market. The strategy worked: studies show that the medical home public health model allows appropriate care to be initiated more often in the primary care center than in the emergency room. Furthermore, it is associated with better preventive health, higher levels of disease management, and lower resource utilization and costs (Devries et al. 2012, Hearld and Alexander 2012).
The guideline on infant oral care was adopted by the American Academy of Pediatric Dentistry (AAPD) in 2001. In 2010, the AAPD reaffirmed its “Policy on the Dental Home,” describing it as inclusive of all aspects of oral health that result from the interaction of the patient, parents, non-dental, and dental professionals. Also in 2010, the AAPD reaffirmed its definition of the term, calling it “the ongoing relationship between the dentist and the patient, inclusive of all aspects of oral health care delivered in a comprehensive, continuously accessible, coordinated, and family-centered way. Establishment of a dental home begins by twelve months of age and includes referral to dental specialists when appropriate” (AAPD reference manual 2012). This concept supports a place where all families feel they will be welcomed for regular, comprehensive care and where they are understood and valued. Empirical evidence suggests great value to a long relationship with child patients as it allows additional learning and reframing of experiences after difficult procedures. This can only occur if the family has a comfortable relationship with the dental home. The present alternative is a system that leads to episodic and emergency care (Feigal 2001).
Figure 5-1. The pediatric dental triangle founded under ideal circumstances: during the establishment of a dental home at age one. Courtesy of Dr. Ari Kupietzky.
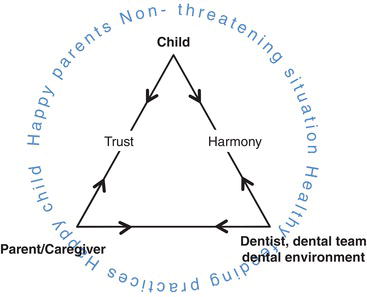
Figure 5-2. The pediatric dental triangle established under less-than-ideal circumstances: an emergencyfirst-time dental visit. Courtesy of Dr. Ari Kupietzky.
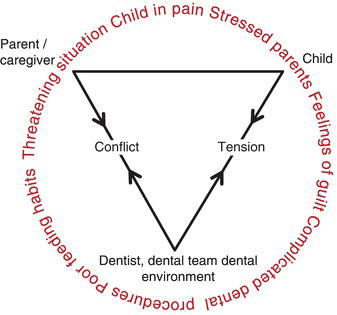
In a familiar and welcoming environment, relationships can be made that ease the stress of health care for children. A dental home enhances the likelihood of establishing parental compliance with early and regular care. It is a cornerstone of prevention in dentistry, and it is much more likely to lead to better child acceptance of dental procedures.
A major goal of the dental home concept is the prevention of ECC. Although not yet substantiated by research, researchers and clinicians state that the benefits of the dental home are substantial and intuitive with an increasing emphasis on disease prevention and management, advancements in tailoring care to meet individual needs, and better health outcomes (Nowak and Casamassimo 2008). The benefits of the dental home include early dental attendance and preventive services, resulting in lower future treatment costs, and a decrease in more invasive, complex dental treatments (Doykos 1997, Savage et al. 2004). Untreated dental problems may lead to hospitalization and expose children to additional health risks associated with conscious sedation and general anesthesia (Newacheck et al. 2000). However, among the non-tangible advantages of this approach to dental care is the fact that a dental home established early in life may also reduce children’s anxiety or fear of dental care. This is the reason for including this chapter in a book devoted to patient management. Again, the emphasis is on the prevention of disease.
With introspect one may conclude that establishing a dental home is simply the early foundation of a healthy, balanced, stable, and harmonious pediatric dental triangle (see Figure 5-1). The first year visit provides ideal conditions for development of the dentist-parent-child relationship. The child is free of pain and the accompanying parent is free of stress and anxiety. The healthy triangle has at its base the dentist and parent acting as a foundation for the apex of the triangle: the child. The dental team and parent are team members, on the same side of the triangle supporting the child through the dental experience. Conversely, when a two-year-old child appears at the dentist for the first time with ECC and possibly pain, the pediatric dental triangle is far from ideal (see Figure 5-2). Many parents are filled with feelings of guilt when their child is diagnosed with ECC, often with anxiety and stress. As the dentist explains the cause of the disease and discusses the treatment options many parents take on the role of child protector. The dental team is then situated on one side of the triangle opposite the child and parent. The dental team, bearing the weight and balancing force of the unstable and fragile triangle is at a disadvantage. The early establishment of the dental home allows the avoidance of such an unfavorable start.
The receptionist reassured her that Dr. Ann and the entire staff have much experience dealing with young children, even younger than Kayla. She told Mrs. G. that a pediatric dentist is similar to a pediatrician and will be able to help Mrs. G and Kayla through the visit. Mrs. G made the appointment.
Case 5.1, Discussion: The receptionist is the first contact with the dental office, and in this case needed to reassure the mother that bringing in her child for the one-year visit was the right thing to do. It is clear how important it is for Kayla to establish a dental home. Her mother mentioned on the phone that Kayla is not getting proper preventive dental care at home. She will need to be instructed on proper feeding habits, fluoride usage, and how to brush a young child’s teeth. Her predicament and uncertainty about this visit is typical, especially if Kayla is her first child. Contradicting information regarding the proper timing for the first dental visit is widespread in the dental profession. Referral from a pediatrician or family doctor lends more credibility to the concept. Many general dentists give parents misinformation either out of ignorance or perhaps because they themselves cannot manage a very young child and therefore do not comprehend the validity of such an early dental visit. Having a website explaining much of the above helps alleviate parents’ initial anxieties.
Although the dental home concept was introduced more than ten years ago, a 2011 survey of parent leaders confirmed that the majority of parents are not aware of it (Kagihara et al. 2011). The majority of respondents (84.8%) said parents do not know about the recommendation to establish a dental home for their child by twelve months of age. They elaborated on their answers with comments including the following:
- “I just learned this (age-1 dental visit concept) myself within the last week—and I’m supposedly in the loop.”
- “Some families need to be informed. Other families tell us that they have attempted to get that oral health screening from their dentist at age one and have been turned away because the dentist did not follow this as the standard of care.”
- “Many believe they can wait until either the child starts school or they lose their baby teeth.”
- “No way! Age three is what we always heard!”
- “Yes, but if the child is chronically ill, other health issues often come first and many children who do not feed by mouth are often taken to the dentist later because of other health complications.”
- “Not at all, as oral health care is not considered a priority in light of other medical diagnoses a child might have, and be/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


