Legal Issues, Quality Assurance, and Infection Prevention
Learning Outcomes
On completion of this chapter, the student will be able to achieve the following objectives:
• Pronounce, define, and spell the Key Terms.
• Describe the components of informed consent with regard to dental imaging.
• Describe the types of laws that affect the practice of dental radiography.
• Describe the Consumer-Patient Radiation Health and Safety Act.
• Identify the individual who legally “owns” the dental images.
• Name the eight annual tests recommended for x-ray equipment.
• Describe the components of a quality assurance program.
• Describe quality control tests for processing solutions.
• Explain the use of a stepwedge.
• Discuss the purpose of a reference radiograph.
• Explain the infection control requirements for preparing a radiography operatory.
• Describe the infection control protocol when making exposures using phosphate storage plates.
• Describe the infection control protocol when making exposures using digital sensors.
• Describe the infection control protocol when making exposures using conventional dental x-ray film.
Performance Outcomes
On completion of this chapter, the student will be able to meet competency standards in the following skills:
• Perform infection control practices required for all dental imaging techniques.
• Practice infection control measures when in the darkroom.
• Practice infection control measures when using the daylight loader in processing dental films.
Electronic Resources
![]() Additional information related to content in Chapter 40 can be found on the companion Evolve Web site.
Additional information related to content in Chapter 40 can be found on the companion Evolve Web site.
Key Terms
Artifact A blemish or unintended radiographic image that is not present in the actual structure.
Disclosure Process of informing the patient about a procedure, for example, the procedure for taking x-rays.
Image receptor Recording medium for an image—a digital sensor, a phosphor storage plate (PSP), or conventional dental x-ray film.
Informed consent Permission granted by a patient after being informed about the risks, benefits, and alternatives of a procedure.
Liable Accountable or legally responsible.
Phosphor storage plate (PSP) Reusable film-sized flexible plate coated with phosphor as the image receptor.
Positioning device Instrument used to hold the film, phosphor storage plate (PSP), or digital sensor in the proper position during exposure. Also commonly known as a “film-holder.”
Quality assurance (QA) A plan to ensure that the dental office produces consistent, high-quality images with a minimum of exposure to patients and personnel.
Quality control tests Specific tests used to ensure quality in dental x-ray equipment, supplies, and film processing.
Stepwedge Device constructed of layered aluminum steps to demonstrate film densities and contrasts.
View box An illuminated boxlike device used to view radiographs.
As a dental assistant, it is your responsibility to understand the laws that apply to you when you are exposing dental images.
Federal and state regulations control the use of dental x-ray equipment. Individual state requirements also determine the educational qualifications of dental personnel who expose dental images.
To ensure the highest quality dental images and the least risk for exposure to patients and personnel, a quality assurance program is necessary. Quality assurance (QA) means regular testing to detect equipment malfunctions, planned monitoring, and scheduled maintenance. Regular testing of equipment also helps to ensure compliance with state and federal regulations.
Regardless of the imaging technique used, the potential is always present for cross-contamination of equipment and environmental surfaces, if good infection control procedures are not practiced.
In this chapter, you will learn the details and the step-by-step infection control procedures that are required in the various techniques of dental imaging. Refer to Part 4 of this text for a detailed discussion of disinfection, sterilization, and other general infection control measures.
Legal Considerations
Three major categories of legal considerations regarding the use of images in dentistry have been identified: (1) federal and state regulations regarding x-ray equipment and its use, (2) licensure for individuals who expose dental images, and (3) risk management for avoiding potential lawsuits.
Federal and State Regulations
The use of dental x-ray equipment is regulated by federal and state regulations. All dental x-ray machines manufactured or sold in the United States after 1974 must meet federal regulations. These include safety specifications for minimum filtration and accuracy of the milliamperage, time, and kilovoltage settings.
All x-ray equipment is also subject to state, county, or city radiation health codes. These codes may include regulations pertaining to barriers, film speeds, position of the operator, and image processing. Many states require that x-ray machines must be registered and charge a fee for this registration. In addition, most states have laws that require inspection of dental x-ray equipment on a regular basis, such as every 5 years. Be certain that you understand the requirements in your area.
Licensure Requirements
The Consumer-Patient Radiation Health and Safety Act is a federal law that requires that all persons who use x-rays to take dental images must be properly trained and certified. It is then up to the individual state to establish its own policies.
Thus, requirements for certification in radiography for dental assistants vary from state to state. Some states require Dental Assisting National Board (DANB) certification, and other states may require an additional examination. Because each state deals with dental radiography differently, it is your responsibility to become informed about the specific requirements in your particular state.
Risk Management
Risk management involves following policies and procedures that will reduce the chance that a malpractice lawsuit will be brought against the dentist. Key areas of risk management include patient consent, patient records, liability issues, and patient education, as discussed in the following sections.
In today’s society, people tend to file more malpractice lawsuits than in the past. Thus, the dental assistant should always practice risk management. For example, the assistant must be careful not to make casual negative comments about the radiograph equipment or its operation. Statements made without thinking, such as “The timer must be off,” “This thing never works right,” or “The solutions are weak,” are unnecessary and can make the patient feel uncomfortable. Remember, statements made by anyone at the time of an alleged negligent act are admissible as evidence in court (refer to Chapter 5).
Informed Consent
It is the dentist’s responsibility to discuss with the patient the need for dental images and treatment procedures, but the dental assistant may participate in the process of obtaining informed consent. Patients must give their informed consent for dental images, in addition to other procedures. Before patients can give informed consent, they must be provided with the following information in lay terms:
• Risks and benefits of imaging procedures
• Person who will be exposing the images
• Number and type of images that will be taken
• Consequences of not having the images
• Alternative diagnostic aids that may provide the same information as dental images
The process of informing the patient about the nature and purpose of dental imaging is termed disclosure. After disclosure, the patient may give informed consent or may refuse the images. If the dentist has not obtained informed consent from a patient before exposure of dental images, a patient may legally claim malpractice or negligence.
Liability
Under state laws, the supervising dentist is legally responsible, or liable, for the actions of dental auxiliary personnel. Known as the respondeat superior doctrine, this means that the employer is responsible for the actions of the employee.
Even though dental assistants work under the supervision of a licensed dentist, they still can be held legally liable for their own actions. Most often, the dentist is the only person sued for negligence or malpractice, but in some cases, the dentist and the dental assistant have been sued for the actions of the dental assistant. You must be aware of the laws in your state and practice accordingly.
Patient Records
Whether conventional film or digital images are obtained, they are a part of the patient’s dental record and are regarded as a legal document. The dental record must accurately reflect all aspects of patient care. Documentation of all imaging must include the following information:
It is important to document the exposure of dental images. The number of exposures and the quality of the images may be important issues in a malpractice suit. If poor-quality images are used in court, this reflects poorly on the dentist.
Ownership of Dental Images
Legally, dental images are the property of the dentist, even though the patient or the patient’s insurance company paid for them, because dental images are a part of the patient’s dental records.
However, patients have a right to reasonable access to their records. When patients transfer to another dentist, it is reasonable for them to have a copy of their records, including dental images, forwarded to the new dentist. Patients may request a copy of their images; this request should be written and signed by the patient. The dentist should be informed of the patient’s request, and an entry should be made in the chart stating when and to whom duplicate or digital images were sent. A reasonable fee may be charged. Never give or send the original images to a patient. If a lawsuit should occur, no defense is possible without the dental images.
Dental images and other dental records should be retained indefinitely. Statutes of limitation may vary, and the question of when to destroy or discard a patient record may not always have a simple answer. Patient records and computer data must be stored carefully so they do not become damaged or lost. Computer files should always be backed up both within the dental office and at an off-site storage facility. It is critical that a protocol and labeling system is used to ensure that computer records are not accidentally overwritten.
Digital Files Security
An advantage of digital files is that they can be sent over computer networks. Before doing so, you must check with local, state, and federal regulations about patient confidentiality. It may be necessary to encrypt the files or use virtual private networks (VPNs) rather than sending files over the public Internet.
Patient Refusal
On occasion, patients may refuse to undergo dental imaging. This refusal presents a difficult situation because the dentist must decide whether an accurate diagnosis can be made without images, and whether treatment should be provided. In most cases, a lack of images compromises the patient’s diagnosis and treatment. The use of dental images is now the accepted standard of care.
Every effort should be made to educate the patient about the importance of dental imaging. No document can be signed that totally releases the dentist from liability for treating a patient without taking dental images. Even if the patient suggests signing a release or waiver that would release the dentist from liability, such a document would be considered invalid if an injury were to result. Legally, a patient cannot consent to negligent care. It should be stated in the patient’s record if a patient refuses recommended images. The dentist then must make the decision as to whether to proceed without dental images.
Patient Education
As a dental assistant, you should understand and be sensitive to the patient’s concern and fears about exposure to radiation during dental imaging. The patient often feels more comfortable confiding these fears to the dental assistant rather than to the dentist.
The dental assistant can explain to the patient the importance of dental imaging in detecting disease and planning treatment (Fig. 40-1). The dental assistant can inform patients of the federal and state laws enacted for their protection. In addition, you can give patients educational materials on the subject (e.g., American Dental Association pamphlets, such as Dental Radiograph Examinations, Your Dentist’s Advice, and The Benefits of Radiograph Examinations, or the U.S. Food and Drug Administration’s Radiographs: Get the Picture on Protection). These educational materials also can be placed in the reception room. Furthermore, the dental assistant can remind patients that the dose from four bitewing images is about the same as a single day’s worth of natural background radiation.
Quality Assurance in the Dental Office
QA is a way of ensuring that everything possible is being done to produce high-quality diagnostic images. QA includes quality control tests that monitor dental x-ray equipment, supplies, and image processing. It also involves quality administration procedures that include keeping schedules of maintenance and record-keeping logs.
The benefits of a QA program far outweigh the associated time, effort, and costs. Fewer retakes mean time and cost savings for both patients and operators.
Quality Control Tests
Quality control tests are specific tests that are used to monitor dental x-ray equipment, supplies, and film processing. The American Academy of Dental Radiology recommends a number of annual tests for dental x-ray machines. These tests are designed to identify minor malfunctions, including (1) variations in radiation output, (2) inadequate collimation, (3) tubehead drifting, (4) errors in timing, and (5) inaccurate kilovoltage and milliamperage readings. Note: When not in use, always leave the tubehead and extension arm in a closed position (see Fig. 38-15, A). The weight of the tubehead on an open extension arm can weaken the unit and cause the tubehead to drift during exposures (see Fig. 38-15, B).
Dental X-Ray Machines
Regulations require that dental x-ray machines must be inspected periodically. Some state and local regulatory agencies provide inspections of dental x-ray equipment without charge as part of their registration and licensing procedures. Dental x-ray machines also must be calibrated, or adjusted for accuracy, at regular intervals. A qualified technician must check the x-ray machine performance and calibrate the dental x-ray equipment.
The dentist, the dental assistant, or the manufacturer’s service representative can perform annual tests for dental x-ray machines. These tests are easy to perform and require only basic test materials and test logs to record the results. You can obtain a free pamphlet called Quality Control Tests for Dentistry from Eastman Kodak (Rochester, New York). This easy-to-follow pamphlet describes step-by-step procedures for performing each of these tests.
Dental X-Ray Film
You should check each box of film while opening it. Even though the film may not be expired, the box may have been improperly stored before it reached your office. Follow these easy steps to test the film for freshness:
Phosphor Storage Plates
Reusable phosphor storage plates (PSPs) require less radiation exposure than film (see Fig. 39-6).
Screens and Cassettes
Intensifying screens inside the extraoral cassette should be periodically checked for dirt and scratches. Screens should be cleaned monthly with a commercially available cleaner. After cleaning, an antistatic solution should be applied to the screen to prevent static electricity that may affect film quality. Screens that appear visibly scratched should be replaced.
Cassettes should be checked for worn closures, light leaks, and warping, which may result in fogged and blurred radiographs; damaged cassettes must be repaired or replaced. Follow these easy steps to test the cassette for adequate film-screen contact:
1 In the darkroom, insert one film between the screens in the cassette.
2 Place a wire mesh test object on top of the loaded cassette.
3 Using a 40-inch target-film distance, direct the central ray perpendicular to the cassette.
4 Expose the film with the use of 10 mA, 70 kVp, and 15 impulses.
6 View the film on a view box in a dimly lit room at a distance of 6 feet.
View Boxes
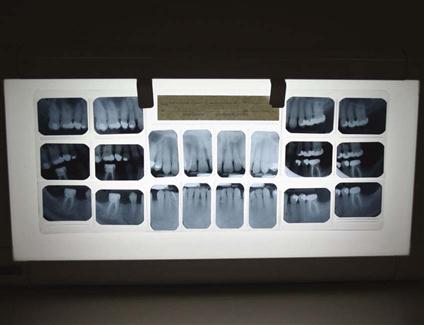
A properly functioning view box is necessary for the interpretation of conventional radiographs (Fig. 40-2). The view box contains fluorescent bulbs that emit light through an opaque plastic or Plexiglas front. The view box should emit a uniform and subdued light when functioning properly.
The view box should be periodically checked for dirt and discoloration of the Plexiglas surface. The surface of the view box should be wiped clean daily. Permanently discolored Plexiglas or blackened fluorescent bulbs must be replaced.
Darkroom Lighting
Check the darkroom for light leaks every 6 months. Follow these easy steps to test the darkroom for light leaks:
1 While standing in the darkroom, turn off all the lights, including the safelight.
4 If the darkroom has no visible light leaks, the room is safe for processing films.
Safelight Test
The “light-tightness” of the darkroom must be confirmed before you can test the effectiveness of the safelight. Follow these easy steps to use the coin test to check the safelight:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses