Chapter 4
Bruxism and the Use of Splint Therapy
Aim
The aim of this chapter is to consider the roles played by bruxism in temporomandibular disorders (TMDs) and splint therapy.
Outcome
Having read this chapter, the practitioner should:
-
understand the differences between clenching and grinding
-
be able to identify the various factors responsible for chronic TMDs
-
be familiar with the indications and design of splints in the management of TMDs.
Case Presentation
-
Complaint. A 23-year-old male college student had attended his general medical practitioner complaining of right-sided otalgia. He was diagnosed with a middle ear infection and started on a course of antibiotics. There was no change in his pain and he returned to the doctor several times complaining of persistent earache. Following repeated courses of antibiotics and no appreciable change in his pain, he was referred to an ENT specialist. A comprehensive ENT evaluation, including endoscopic nasal and sinus examinations and computed tomography of the middle ears and sinuses, indicated no abnormalities. He was advised to attend his dentist. At this point, he was complaining of pain radiating from the right ear into the right temporal, mandibular and postauricular regions.
-
Clinical examination. His dental evaluation was unremarkable and a provisional diagnosis of right temporomandibular joint (TMJ) capsulitis was made following palpation of the right TMJ, which was particularly tender with pain radiating to the ears and jaw. A soft splint was provided to be worn at night. However, the pain continued, with increasing intensity in the morning. The patient then noticed that he had perforated the soft splint in a number of places. The patient commented that he felt increased tension in his jaw on waking and it would appear that he is grinding aggressively, causing the damage to the splint.
Introduction
The case presentation outlined above illustrates the diagnostic complexity of patients suffering from TMDs. Does this case sound familiar? As the debate surrounding the aetiology of TMJ dysfunction and masticatory muscle disorders continues, the focus is now shifting from the traditionalists, who suspect malocclusion to be the principal factor, to the concept of parafunctional behaviours overloading the stomatognathic system. Various parafunctional behaviours exist, ranging from gum chewing to clenching and grinding. Although the behaviours can differ greatly, they are similar in one respect: they overload the TMJ apparatus. When the load exceeds the adaptive capacity of the joint or related muscles, pain occurs. Common parafunctional behaviours are:
-
grinding
-
clenching
-
gum chewing
-
nail biting
-
playing musical instruments: violin and wind instruments
-
lip and cheek biting.
What is Bruxism?
Bruxism is defined as diurnal or nocturnal parafunctional activity involving clenching and grinding of teeth. Clenching usually occurs during the day and is often called “awake or daytime bruxism”. “Nocturnal or sleep” bruxism is characterised by clenching and grinding of teeth at night. Rarely will patients grind their teeth during the day, unless the activity is associated with brain damage. Sleep bruxism is characterised by rhythmic or sustained contractions of the masticatory muscles, in particular the masseter and temporalis. Rhythmic episodes tend to be short lasting, often occurring for two to three seconds in duration and associated with a side-to-side grinding motion. Sustained contractions relate closely to clenching and may last for 30 seconds. Generally the jaw is open during sleep, given motor suppression. The masseter and temporalis muscles are most commonly implicated in bruxism. A small percentage of patients may also tap their teeth with rapid shock-like intensity. Each episode may last for less than a second; contractions can often occur in quick fire succession. This form of bruxism is described as sleep myoclonus. It is reported to be associated with conditions such as epilepsy and insomnia. The forces generated during myoclonic masticatory muscle activity are sufficient to shear cusps from teeth.
Clenching is defined as “awake” or daytime bruxism. It is not associated with tooth sounds. It is a semivoluntary behaviour and patients tend not to be aware of the habit until attention is drawn to it. It is not uncommon for patients to strenuously deny clenching during the initial consultation appointment, only to return, somewhat amazed, at a later date now aware of their aggressive daytime clenching behaviour. The skilled clinician will often identify the signs of clenching during the consultation appointment. It is estimated that the teeth remain in contact less than 20 minutes during a 24 hour period. This occurs primarily during mastication and deglutition. Nocturnal bruxism is associated with loud grinding and tapping tooth sounds. The forces generated during sleep bruxism can be significantly greater than the forces generated with conscious effort.
Classification
Primary or idiopathic bruxism occurs in the absence of a medical cause. Secondary or iatrogenic bruxism is associated with a medical cause, as outlined in Table 4-1.
| Type | Description |
|
Chemical/medication induced |
|
|
Movement disorders |
|
|
Sleep-related disorders |
|
|
Neurologic/psychiatric disorders |
|
Clinical Presentation
The signs and symptoms of a bruxer are numerous and can vary extensively (Fig 4-1). Some patients with extensive tooth wear, as seen in Fig 4-2, will not complain of jaw pain or dysfunction, in contrast to other patients who may have extensive subjective complaints. The signs and symptoms are listed in Table 4-2. It is important to differentiate night-time bruxing activity from a daytime clenching habit. This can be achieved by evaluating the temporal pattern of the complaint.

Fig 4-1 The problems of tooth grinding.
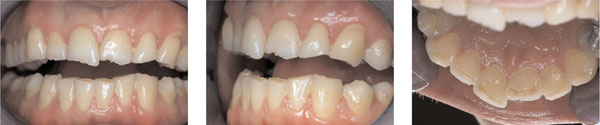
Fig 4-2 Extensive tooth wear as commonly seen in a bruxist.
| Features | |
|
Signs |
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


