(b) orthodontic band in place around molar 36. A sinus tract is visible buccally.
(a) 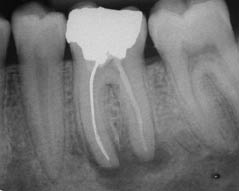 (b)
(b) 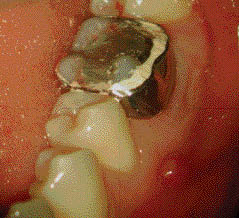
Diagnosis and treatment planning
The diagnosis was a chronic periapical periodontitis with suppuration associated with an existing root canal treatment.
What were the treatment options for this patient?
- Leave alone.
- Extraction.
- Non-surgical root canal re-treatment followed by core build-up and cuspal coverage restoration.
Is there a logical way to plan the treatment of endodontic cases?
Initially it is important to assess the prognosis of the tooth to be treated; this may be done by categorizing the tooth as follows:
- Good prognosis.
- Questionale (guarded) prognosis.
- Hopeless prognosis.
Teeth with a good prognosis are likely to respond well to treatment, while teeth with a hopeless prognosis should be extracted. Teeth with a questionable prognosis may require investigation, with the consent of the patient, prior to a definitive decision regarding any proposed treatment. After the prognosis has been ascertained, stabilization and definitive treatment can be planned.
Prognosis and treatment chosen
In this case, the 36 was restorable as there appeared to be sufficient coronal tooth structure; the periodontal condition was satisfactory and the tooth was functional, i.e. it was in occlusion with the maxillary second premolar and first molar. The patient was young and wished to retain his tooth. The proposed root canal re-treatment had an anticipated good outcome and the tooth was deemed to have a good prognosis. Extraction may have resulted in mesial drifting of the 37 and over-eruption of the opposing the 26, unless the 36 was replaced (with an implant retained crown or bridge) soon after extraction. The option of leaving the tooth alone was discussed with the patient; this included advising the patient of the drawbacks (for example, discharge, swelling and discomfort).
What are the stabilization and definitive phases of treatment?
- Stabilization treatment includes supportive tissue management (periodontal scaling, oral hygiene instruction) and any other preliminary treatment such as splinting, extraction, initial root canal treatment (i.e. pulp extirpation), removal of fractured cusps or placement of a temporary bridge or denture.
- Definitive treatment includes root canal treatment, crown placement, construction of a permanent denture, bridge or implant placement and restoration. At the end of the definitive treatment, the patient’s treatment should be complete and suitable follow-up should be all that is required.
The treatment plan for this case was:
Stabilization phase
- Supportive tissue management ’ supragingival scaling and oral hygiene instruction.
- Placement of orthodontic band to reduce the risk of longitudinal fracture during treatment.
Definitive phase
- Root canal re-treatment of the 36.
- Placement of a suitable core material to prevent microleakage and retain cuspal coverage restoration.
- Provision of a cuspal coverage restoration.
Maintenance
- Periodic reviews to assess signs and symptoms of apical healing.
Treatment
Orthodontic band placement
Due to the size of the amalgam restoration in the tooth, there was concern regarding possible fracture during the treatment procedure. Therefore, a suitably sized orthodontic band was selected, trimmed to avoid damage to the soft tissues and modified to suit the occlusion, and cemented (Figure 4.1.1b). The importance of oral hygiene was reinforced to the patient.
Access cavity
An access cavity was prepared and straight line access to the canal orifices was made through the existing amalgam restoration. Ultrasonic instruments were used when nearing the previous root canal treatment so as not to remove any silver point, which may be protruding into the pulp chamber. This aids the predictable removal of the silver point.
Retrieved silver point
The silver point was removed from the mesio-buccal canal by a combination of initial gentle filing laterally to loosen it and SteiglitzTM forceps (Figure 4.1.2a). The mesio-lingual canal had been previously obturated with paste; this was removed by a combination of ultrasonics and Hedström files.
Figure 4.1.2 (a) Retrieved silver (left) and gutta-percha (right) points, (b) working length radiograph.
(a) 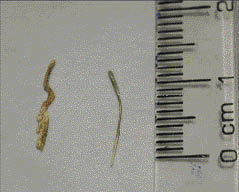 (b)
(b) 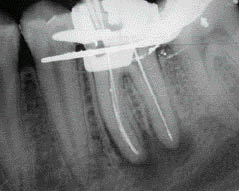
Cleaning and shaping
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


