CHAPTER 33. Intellectual and physical disability and psychiatric disorders
The terminology for disability is confusing, evolving and subject to the forces of political correctness. Healthcare professionals often demand clear-cut definitions of degrees of disability that can be used to plan dental services. Unfortunately, this approach over-simplifies the problems. People with disability see their needs in social terms rather than just the sum of their medical problems and, rightly, demand individualised care. The dentist must consider what each patient is prevented from doing, rather than concentrating on the physical or mental impairments themselves. This way of thinking illustrates the social and environmental aspects of disability, and highlights ways in which the individual’s environment can be adapted to limit, or even abolish, handicap. Current terminology for disability is shown in Table 33.1.
| Term | Definition |
|---|---|
| Impairment | Any loss or abnormality of physiological function or anatomical structure |
| Disability or limitation of activity | Restriction or lack of ability to perform a function considered normal |
| Handicap | The disadvantage for the individual, resulting from their disability, which prevents them from performing a normal role in society |
Nowhere is terminology more difficult than in the case of intellectual impairment. The terms mental retardation, subnormality, deficiency or handicap are considered stigmatising and no longer acceptable. In practice, intellectual impairments cause a wide range of disability. Some patients are intelligent but cannot cooperate (e.g. cerebral palsy), others are intelligent but uncooperative (e.g. hyperactivity), yet others are intellectually impaired but may sometimes be easily treated (e.g. mild Down’s syndrome). The specific diagnosis and its severity are much more helpful in planning treatment than non-specific labels such as learning difficulty or intellectual impairment.
The prevalence of inherited disability is estimated at 1.5 to 2 per 1000 live births. Intellectual impairments account for approximately 0.9 per 1000 and major physical impairments for the remainder. The prevalence is rising as a result of better medical care for adults and improved survival for babies with congenital disorders. Approximately 12 000 children with disabilities are registered with dental practitioners. The management of their dental care is affected by both the disability and parents’ motivation and attitudes. However, mental or physical disability does not necessarily mean that dental care has to be compromised, though this may sometimes be inevitable.
Children and adults with disability present a wide variety of problems of dental management, but up to 90% of them can probably be managed by conventional means without sedation or general anaesthesia. Nevertheless, people with disability are a dentally neglected group, even though valiant attempts have been made to overcome this deficiency in recent years.
Preconceptions that ‘the disabled’ are necessarily grimacing, drooling and uncooperative are seriously misplaced. In fact, those who manage children with disability find the work more rewarding than dentistry in normal children. Dental treatment, which involves both relatively prolonged personal attention and a change from routine, can be a pleasure for them. One Down’s syndrome child, for instance, though well looked after by affectionate parents, was in a state of mysteriously eager expectation for days at the prospect (it was later found) of having an X-ray. Dental treatment may, therefore, be a real source of pleasure for those so deprived.
There is a welcome concern about the dental care of children with disability, but it should be remembered that disability persists for life. The transition from special school to community care can worsen dental disease because dental care must be provided in a less controlled setting and intensive prevention is more difficult to maintain. The elderly probably suffer more disabilities than children, because of the additional problems of declining health but, unfortunately, are less likely to get sympathetic help.
Difficulties in the provision of dental care for people with disability are summarised in Box 33.1. Unless the disability is severe, most of these difficulties can be overcome with patience, training and experience. It should be remembered that when disability is viewed in its social context, many difficulties become the responsibility of the dentist rather than being a problem associated with the patient.
Box 33.1
Typical difficulties with dental care of patients with disability
• Poor cooperation with routine dental treatment
• Difficulties in performing routine home oral hygiene
• Associated systemic disease
• Difficulties with transport and access to the surgery
• Need for sedation or general anaesthesia
• Medications or diets promoting caries
• Dysphagia, drooling, bruxism
• Oral effects of medication
• Competence to give consent
• Financial problems for patients
• Discrimination or prejudice in health care
Epilepsy is often associated with other disabilities but, with modern treatment, should present no special difficulties. There may be problems with phenytoin-induced fibrous gingival hyperplasia (Ch. 5). It is also important to be able to recognise and manage a major fit should it happen in the dental surgery (Ch. 36).
The importance of good prevention cannot be overemphasised. Many of the problems arising from treatment of people with disability would be solved by good preventive regimens.
Disabilities relevant to dentistry are summarised in Box 33.2.
Box 33.2
Common medical disabilities affecting dental management
Intellectual impairment
• Learning difficulty
• Down’s syndrome
• Microcephaly and hydrocephalus
• Metabolic disorders
• Hypoxia at birth
• Some syndromes
Behavioural disorders
• Autism
• Attention deficit hyperactivity disorder
Physical impairment
• Cerebral palsy
• Severe defects of the hands or arms
• Muscular dystrophies
• Spina bifida
• Epilepsy
• Some syndromes
• Communication problems: visual and hearing impairment
• Cleft palate (Ch. 2)
Physical and intellectual impairment are frequently combined, as in Down’s syndrome and some cases of cerebral palsy. Intellectual impairment (often associated with physical impairment) affects by far the largest group of children with disability needing dental care. All patients with Down’s syndrome, many with cerebral palsy and some with epilepsy are also intellectually impaired. These four groups account for approximately 70–75% of children with disability. Conversely, many patients with cerebral palsy have normal intelligence but may be mislabelled as mentally impaired because of communication difficulties.
Heart disease, haemorrhagic disease (particularly haemophilia), diabetes mellitus and other systemic diseases are discussed in Chapter 26, Chapter 27, Chapter 28, Chapter 29, Chapter 30, Chapter 31 and Chapter 32.
DISCRIMINATION LEGISLATION
The UK Disability Discrimination Act 2005 is intended to abolish discrimination and applies to all employers and service providers including dentists.
The Act defines disability as a physical or mental impairment which has a substantial and long-term adverse effect on an individual’s ability to carry out normal day-to-day activities. The definition is broad and applies equally to conditions such as colour blindness, visual or hearing impairment and severe learning difficulty.
Under the Act, service providers must not use any reason related to patients’ disability as an excuse to treat disabled people less favourably than other people. Dentists must make ‘reasonable adjustments’ so that disabled people can access and use their services. This means more than providing wheelchair ramps. All aspects of the clinical practice and business of dentistry must comply. Some examples of the measures expected under the Act are shown in Box 33.3. Which are reasonable in any particular setting depends on guidance from the Disability Rights Commission and will change over time and with legal precedents.
Box 33.3
Some factors to ameliorate disability in dental practice
| Access | Level access, ramps, easy-grip door handles, doors hold open easily, wide corridors and aisles, obstructions clearly marked, if necessary provide off-site or domiciliary visits. Provide for guide dogs |
| Design and structure of buildings | Colour schemes contrast floors and walls, well lit, alarms in toilets (visible and audible) |
| Signs and practice leaflets and paperwork | Large type, succinct, good colour contrast, easy to read, use symbols as well as words, use sans serif fonts, no justification of right hand margins, simple page layouts. Consider Braille and audio versions |
| Websites | Should meet British Standard Specification for accessible websites |
| Staff and policies | Provide disability awareness training for staff, record and survey needs of disabled users and consult local disability groups. Each practice should have a disability policy |
Practices that are ‘disability-friendly’ will also be more suitable for the elderly and many other groups of normal patients.
LEARNING DIFFICULTY
Learning difficulty is an all-inclusive term to describe those with intellectual impairment whether caused by a specific disorder or of unknown cause. Down’s syndrome, fragile X syndrome and hypoxia at birth are the more common causes and the specific features of these conditions are dealt with below. Learning difficulties may be unrelated to any physical disorder, or physical defects may be severe, as in some cases of cerebral palsy. A minority of patients with genetic syndromes have craniofacial anomalies associated with intellectual impairment.
Intellectual impairment is classified according to the level of learning difficulty and children are taught either in mainstream schools or special schools, according to the degree of impairment. Institutional care is avoided if possible. Unfortunately, the learning difficulty classification gives no more than a broad indication of probable problems with dental care because patients vary so widely.
Children with mild learning difficulty can usually be coaxed into accepting regular treatment and (if the parents are supportive) to maintain acceptable standards of oral hygiene. However, oral hygiene is usually suboptimal or poor when it depends on parents or carers. At the other extreme, all that may be possible, particularly for children with uncontrollable muscular activity such as jaw clenching, is first-aid dentistry under general anaesthesia. All intermediate grades exist, but the level of dental health that can be achieved depends greatly upon the level of the dentist’s skill and devotion to the task (Fig. 33.1) and prevention by carers.
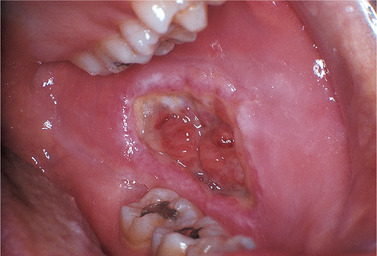 |
| Fig. 33.1
Traumatic ulceration. This child with learning difficulties produced this deep and extensive ulcer after a local anaesthetic for dental treatment.
|
Down’s syndrome
Down’s syndrome is the most common clinically recognisable syndrome with severe learning difficulty. It is caused by trisomy of chromosome 21 giving a total complement of 47 chromosomes instead of 46. This is usually caused by failure of the chromosomes to separate during meiosis in the ovum, a defect closely linked to maternal age. The overall incidence is 1 in 700 live births, but the risk rises to 1 in 25 in mothers aged 45 years or over. Because the defect arises in the ovum, both parents are normal and the condition is not inherited.
In contrast, about 4% of Down’s patients have the additional chromosome 21 genetic material translocated to another chromosome. The translocation is transmitted in a familial pattern, but the parents are normal and the risk of an affected child is relatively low.
The rarest form is mosaic Down’s syndrome in which the trisomy arises during early development and the patients have a mosaic of cells with and without trisomy 21. In this type of Down’s syndrome, the features are very variable and intelligence may be normal despite the typical appearance.
General features
Down’s children have a characteristic facial appearance (Fig. 33.2), abnormalities of the skull and frequently of the dentition, abnormal susceptibility to infection (particularly viral) due to multiple immune defects and congenital cardiovascular disease in up to 50%.
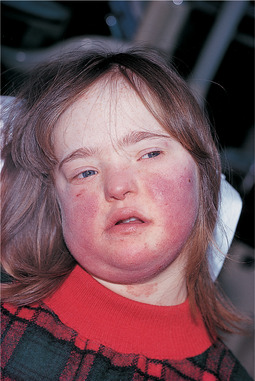 |
| Fig. 33.2
Down’s syndrome. This shows both the characteristic facial appearance and a cyanotic flush caused by associated congenital heart disease.
|
The prominent medial epicanthic skin fold gives the eyes their readily recognisable appearance. There is hypoplasia of the mid-face, poorly developed paranasal sinuses and a malformed upper respiratory tract. Upper respiratory tract infections are common and breathing is often partially obstructed. Underdevelopment of the maxillae is usually associated with a protrusive mandible and class III malocclusion, with anterior open bite (Fig. 33.3, Box 33.4). The ears are often malformed and there is excess skin on the neck.
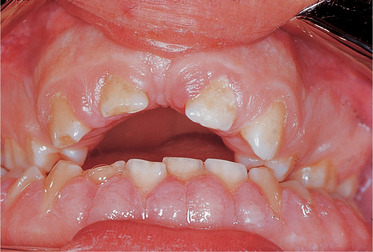 |
| Fig. 33.3
Down’s syndrome. This shows the characteristic anterior open bite together with gross gingival hyperplasia caused by phenytoin treatment for concomitant epilepsy.
|
Box 33.4
Down’s syndrome: features relevant to dentistry
• Class III malocclusion with hypoplastic maxilla
• Protrusive, fissured and apparently enlarged hypotonic tongue (Fig. 33.4)
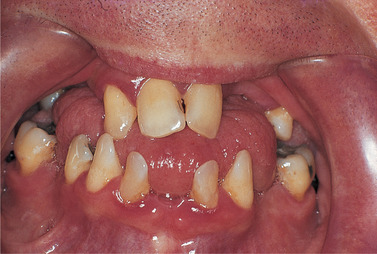 |
| Fig. 33.4
Down’s syndrome. As is frequently the case there are many missing teeth and, in the gaps between them, the hypotonic tongue is protruding.
|
• Lip hypotonia, mouth breathing and drooling
• Everted, thick, dry and crusted lips
• Oligodontia
• Delayed eruption of permanent teeth
• Hypoplastic dental defects and short roots
• Low caries activity
• Gross plaque accumulation
• Rapidly progressive periodontal disease
• Bruxism
• Short stature with short limbs
• Poor muscle tone
• Generalised susceptibility to infection
• Visual or hearing impairment in 50%
• Cardiac anomalies in 40%
• Weakness of atlantoaxial joint
• Susceptibility to leukaemia
• Alzheimer-like dementia in later life
Plaque accumulation and poor oral hygiene, due to the patient’s disabilities and made worse by mouth breathing, together with the systemic predisposition to infection, contribute to the early onset of periodontal disease and early tooth loss (Fig. 33.5). Acute ulcerative gingivitis is also common and often recurs.
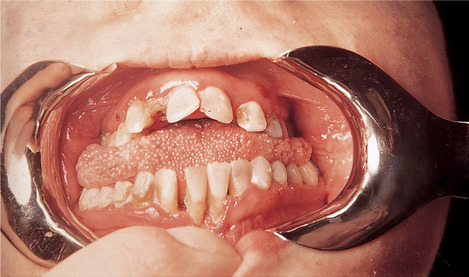 |
| Fig. 33.5
Down’s syndrome. Poor oral hygiene, periodontal destruction and malocclusion.
(By kind permission of Professor C Scully.)
|
Management
All Down’s children have learning difficulties, some severe, but they continue to learn throughout life and may develop many skills if supported by good educational programmes and occupational therapy. Some can maintain an independent life. Patients with Down’s syndrome are often, but not invariably, good-natured, cooperative within their ability and affectionate and receptive to dental care. However, this stereotype fails to recognise many who are frightened or more severely affected and completely uncooperative. The success of dental treatment depends mainly on the level of care provided. Those with milder learning disability can be treated normally in the dental chair, while the more severely affected may require general anaesthesia.
Control of periodontal disease is usually difficult and success depends almost entirely on prevention by good oral hygiene. Teeth may be lost relatively early because of their short roots. Retention of teeth is important because dentures are usually poorly tolerated and retained because of the large protrusive tongue, poor muscle tone and poor comprehension. The apparently large tongue results from muscle hypotonia and forward posture, which also cause problems with mastication and swallowing.
Other features of the syndrome may affect dental treatment. The unstable atlanto-occipital joint is at risk of dislocation with severe consequences if the head is manipulated, particularly during general anaesthesia or sedation. All Down’s syndrome patients should have been screened for this anomaly during early childhood. Deafness and visual problems are common. With improved medical care, life expectancy in Down’s syndrome has lengthened and patients often live into their sixth decade. Unfortunately, almost half of older Down’s patients suffer an Alzheimer-like dementia, which further compromises their independence.
Cardiac defects are present in 40% and half of these are severe enough to warrant surgical intervention. Atrial and ventricular septal defects, mitral and tricuspid valve defects, Fallot’s tetralogy and patent ductus are common. These are repaired in childhood but, in later life, valvular regurgitation and prolapse may develop. Despite many contributory factors, the incidence of infective endocarditis does not appear to be particularly high, but prophylactic antibiotic cover must be given as for normal patients (Ch. 27).
Fragile X syndrome
Fragile X syndrome is the next most common chromosomal defect with learning disability after Down’s syndrome; it affects at least 1 in 1000 of the population.
In this syndrome, the tip of the X chromosome appears as a thin thread of chromatin that is weakly attached and may break off.
Clinical features include learning disability, hyperactivity and behaviour similar to that of autism. Open bite and crossbite are frequent.
Hydrocephalus
Hydrocephalus is caused by failure of drainage of cerebrospinal fluid and may be seen in isolation or associated with spina bifida. Compression of the cerebral tissue can cause severe intellectual impairment. Treatment is to relieve the intracranial pressure by insertion of a catheter and, in the past, this released the cerebrospinal fluid directly into the right atrium (Spitz–Holzer valve). This shunt is susceptible to infection, causing blockage rather than endocarditis. Although antibiotic prophylaxis is not of proven effectiveness, antibiotics are usually given as a precaution, using the same regimen for infective endocarditis. Younger patients are more likely to have a shunt into the peritoneal cavity and this type does not require antibiotic prophylaxis. Severe hydrocephalus can also cause the skull to be so distended and heavy that the head has to be supported during treatment.
BEHAVIOURAL DISORDERS
Autism
Autism is a specific defect of mental development in which there is lack of emotional development, disordered use of language, defective communication and extreme ‘aloneness’. The cause is unknown and both environmental and genetic causes are suspected. The condition is much more common in males. At one extreme, there is severe learning disorder and repetitive behaviour so that it may be impossible to communicate with, or manage, autistic children without general anaesthesia. At the other, sympathy and patience may achieve all that is needed. Asperger’s syndrome is the mildest form of autism. Typical features are summarised in Box 33.5.
Box 33.5
Autism: typical features
• ‘Aloneness’
• Lack of social interaction
• Lack of eye contact with others
• Communication problems
• Apparent unawareness of others
• Fixation on a single object or toy
• Persistent hand-slapping or other repetitive activity
• Rarely, extreme mathematical or artistic talents
• Learning difficulties in 70%
Vey rarely, autistic persons possess bizarre, incomprehensible skills, often mathematical. If, for example, one of these ‘autistic savant’ is asked what day of the week March 7th 2025 will be, an immediate accurate answer is provided.
Hyperactivity/attention deficit disorder
These conditions are often grouped together despite their different presentations. Attention deficit is characterised by daydreaming, limited ability to concentrate and perform complex tasks. Hyperactivity is characterised by excessive movement, inability to concentrate on one task and, sometimes, repetitive movements. The number of children diagnosed with these conditions has risen dramatically since the advent of the drug methylphenidate (Ritalin), but there is no agreed dividing line between this disorder and normal child behaviour. Some cases seem to respond to dietary modification. It has been suggested that some children labelled as suffering hyperactivity/attention deficit are no more than mildly disruptive underachieving children. Such cases might be difficult dental patients but can be expected to respond to good behaviour management. Conversely, severe hyperactivity is profoundly disturbing and may be associated with self-mutilation. Extreme cases may require sedation or anaesthesia.
PHYSICAL IMPAIRMENT
Cerebral palsy
Cerebral palsy is common, with an incidence of 1:1000 and can be one of the most severe disabilities. These children, in the past loosely referred to as spastics, suffer various types of neuromuscular dysfunction (Box 33.6).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


