Orofacial Pigmentation Disorders
Pigmented Lesions of Oral Mucosa
Molecular and Pathologic Correlation of Pigmentation
In heavy metal poisoning also we can observe oral mucosal pigmentation because of formation of metal sulfides which get precipitated in inflamed areas of gingiva causing bluish black discoloration. Table 1 summarizes the type of exogenous substances that can cause oral mucosal pigmentation.
Table 1
Type of exogenous foreign materials causing pigmentation of oral mucosa
| Source | Color | Etiology |
| Silver, amalgam | Gray, black | Iatrogenic implantation, trauma |
| Graphite | Gray, black | Tattoo, trauma |
| Lead, mercury, bismuth | Gray | Ingestion of paints, medicines, poisoning |
| Chromogenic bacteria | Black, brown, green | Superficial colonization |
Oral mucosal pigmentation can also occur due to variety of endogenous pigments. Each of these endogenous pigments can result in a distinct oral discoloration suggestive of various disease processes which are described in Table 2. Blue, bluish red and purple type of oral pigmentation generally occur as a consequence of blood or vascular disorders. Black, brown or gray discoloration of the oral mucosa is because of melanin or hemosiderin pigments. Yellow discoloration of oral mucosa is because of bilirubin deposition or ingestion of large amount of beta-carotene. The pigmented lesions can either be localized or diffuse depending upon their etiology or disease process which they manifest.
Table 2
Type of endogenous pigments, the discoloration caused by them and disease process they indicate
| Pigment | Color | Disease process |
| Hemoglobin | Blue, red, purple | Varix, hemangioma, Kaposi sarcoma, angiosarcoma, hereditary hemorrhagic telangiectasia |
| Hemosiderin | Brown | Ecchymosis, petechiae, thrombosed vein, hemorrhagic mucocele, hemochromatosis |
| Melanin | Brown/black/gray | Melanotic macule, nevus, melanoma, hormonal imbalance, drugs |
| Bilirubin | Yellow | Jaundice/liver disorder |
| Carotene | Yellow | Precursor of vitamin A |
Blood pigments can cause red, bluish red or brown pigmentation of oral mucosa. These pigments are deposited into the connective tissues after lysis of erythrocytes causing extravasation of hemoglobin. The extravasation of blood into soft tissues is attributed to trauma, capillary fragility, platelet defects, or clotting disorders. This extravasated hemoglobin is acted upon by the enzymes to form hemosiderin, which is further broken down into bilirubin and biliverdin, all of which cause oral pigmentation. Therefore, the same endogenous pigments may result in different types of oral pigmentations over a period of time. An early hematoma is bluish red in color while a late hematoma becomes dark brown in color. Blood pigments are usually cleared from the skin or mucosa within 2 weeks.
In albinism the gene for tyrosinase is mutated. In vitiligo, depigmented patches are caused by diminished number of melanocytes. However, these entities are rarely seen in the oral cavity.
Metal Pigmentation
Amalgam tattoo
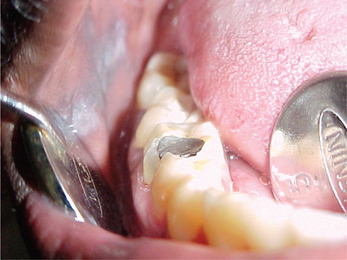
Amalgam tattoo is the most common solitary focal pigmentation lesion of the oral mucosa. These lesions are generally less than 1 cm (rarely amalgam tattoos can be large) and appear as flat, gray-black to blue-black color macules. They are usually found in close approximation to a restoration. Majority of the lesions are located on the buccal mucosa, gingiva and alveolar mucosa with mandibular region being more affected as compared to the maxillary region (Figure 1). All these lesions are asymptomatic and are discovered during routine dental examination. If particles are large enough they can be viewed with help of a radiograph (taken with reduced exposure parameters for soft tissues). The amalgam granules and fragments are found mainly in the lamina propria but were sometimes also seen in the submucosa. Histopathologically, we may observe a giant cell reaction surrounding these amalgam particles.
Bismuth
Orally, we usually see bismuth line which is a bluish black line in marginal gingiva confined to gingival papilla. Bismuth may react with hydrogen sulfide produced by the bacteria to form bismuth sulfide that gets precipitated around periphery of an ulcer or erupting molar. Patient may also complain of burning sensation and metallic taste in the mouth.
Diffuse and Multiple Pigmented Lesions
Racial/physiologic pigmentation
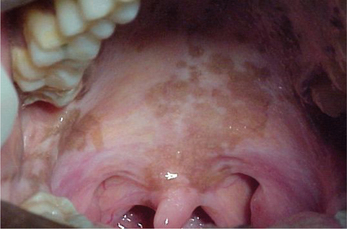
Physiologic pigmentation is seen as diffuse macular pigmentations that may be brown, gray or black in color and can appear anywhere in the mouth with buccal surface and gingiva being most commonly involved. On the gingiva it appears as well-demarcated, ribbon-like, dark brown continuous band that does not extend to involve the marginal gingiva. Occasionally pigmentation may also be seen on the tongue, lips and lingual gingiva as diffuse brown patches with ill-defined or diffuse borders (Figure 2).
Drug-induced pigmentation
Many medications when taken over a long period of time can cause oral mucosal pigmentation. Drug-induced pigmentation can be due to increased synthesis and accumulation of melanin pigments, deposition of the drug or its metabolites into the oral tissues or deposition of iron after damage to the dermal vessels (Table 3).
Table 3
List of drugs that can induce oral pigmentation
Bleomycin
Busulphan
Clofazimine
Chloroquine
Chlorpromazine
Cyclophosphamide
Doxorubicin
Estrogen
5-Fluorouracil
Gold
Hydroxychloroquine
Ketoconazole
Minocycline
Tetracycline
Quinacrine hydrochloride
Zidovudine
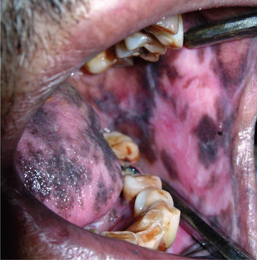
Chloroquine and other quinine derivatives which are usually used in the treatment of malaria and cardiac arrhythmia can cause pigmentation of oral tissues due to a direct stimulating effect on the melanocytes (Figure 3). According to some of the studies these drugs usually cause pigmentation of the palatal tissues.
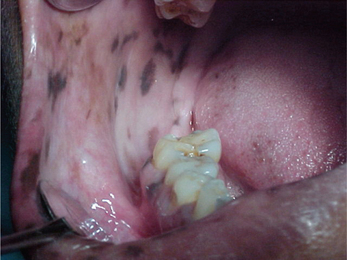
Figure 3 Brownish-black pigmentation of the lips and buccal mucosa caused by chloroquine. Courtesy: Dr Ajit Auluck
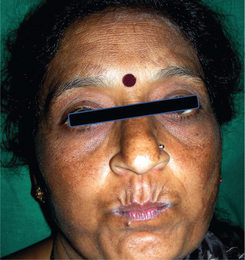
Oral pigmentation can also be due to intake of birth control pills. Chloasma is the term which is used to describe perioral and periorbital pigmentation in such patients (Figure 4). The pigmentation usually occurs as a diffuse brown macular pigmentation which is asymptomatic and lesions resolve upon cessation of drug intake. These lesions usually occur due to the hormonal changes which influence melanocyte stimulation.
Smoker’s melanosis
Tobacco smokers have more intense pigmentation of oral mucosa as compared to non-smokers. Smoker’s melanosis is more common in females. Women are more commonly affected than men because of synergistic effect between the female sex hormones and smoking. Smoking may cause oral pigmentation in light-skinned individuals and accentuate the pigmentation in dark-skinned patients. Clinically, there may be multiple diffuse brown pigmented macules of less than 1 cm in diameter. These lesions can occur anywhere in the mouth but may be usually localized on the attached labial anterior gingiva and the interdental papillae of the mandible. These lesions are completely asymptomatic and benign in nature (Figure 5).
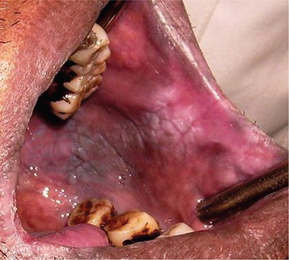
Figure 5 Smoker’s melanosis of the buccal mucosa associated with leukoplakia. Courtesy: Dr Ajit Auluck
Microscopically there is evidence of basilar melanosis but there is no melanocyte proliferation. The increased melanin production may be a biologic defense mechanism against the noxious agents present in the tobacco smoke. The intensity of the oral pigmentation is directly related to the duration and amount of smoking. Smoker’s melanosis usually disappears within 3 years of smoking cessation. Biopsy must be advised whenever there is a surface elevation or increase in the pigment intensity or rapid increase in the size of the lesion.
Endocrine disorders
In the oral cavity pigmentation may appear as diffuse brown patches on the gingiva, buccal mucosa, palate and tongue (Figure 6). This may resemble physiologic pigmentation. Physiologic pigmentation can be differentiated from pigmentation caused by Addison’s disease as the later develops and progresses during adult life and not present since birth. It is also accompanied by systemic manifestations like weakness, nausea and vomiting, abdominal pain, constipation or diarrhea, weight loss and hypotension. Oral pigmentation may be the first sign of Addison’s disease. Therefore complete examination must be done for patients with diffuse pigmentation of oral cavity and associated with systemic signs and symptoms. Patients presenting with such features should be sent for medical evaluation and laboratory tests to assess levels of ACTH, plasma cor-tisol and serum electrolytes.
Café au lait pigmentation
In Peutz-Jeghers syndrome patients have intestinal polyposis along with oral macular pigmentations that appear around the mouth (Figure 7) and on the fingers. When such lesions are observed, a detailed history of the patient should be taken about gastrointestinal complaints as well as the family history for intestinal polyps. These pigmented melanotic spots do not require any treatment and are not associated with any risk for malignant transformation. However, the patient should be monitored for the development of internal m/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses