Differential diagnosis of lesions of variable radiopacity in the jaws
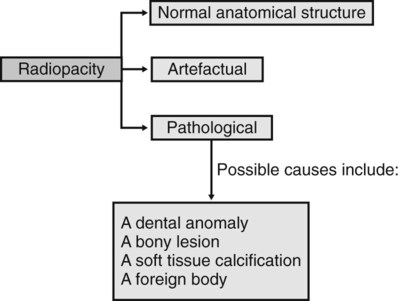
As explained in Chapter 25, a variety of conditions that can affect the jaws are radiopaque relative to the surrounding bone, although the degree of opacity can be very variable. A step-by-step guide, similar to that suggested for radiolucent lesions in Chapter 26, is outlined to emphasize the importance of a methodical approach when producing a differential diagnosis. The suggested approach is summarized in Fig. 27.1. Although most lesions are still detected using plain radiographs, this process can be greatly facilitated in many cases if advanced imaging modalities, described in Chapters 16 and 18, such as computed tomography (CT), cone beam CT or magnetic resonance (MR) are available.
Step I
Describe the variable radiopacity noting in particular:
• Site or anatomical position – is the opacity actually within bone or is it within the surrounding soft tissues and thus superimposed on the bone? To localize the opacity, two radiographs are usually required, ideally at right angles to one another.
• Outline or periphery – a particularly useful differentiating feature, since if the opacity is surrounded by a thin radiolucent line, it is invariably of dental tissue origin.
Step II
Decide whether the variable radiopacity is:
1. A normal anatomical feature
– An area of dense bone sometimes referred to as a dense bone island
– A bony prominence such as the external oblique ridge, mylohyoid line or genial tubercles
These depend largely on the type of radiograph, but examples include:
Step IV
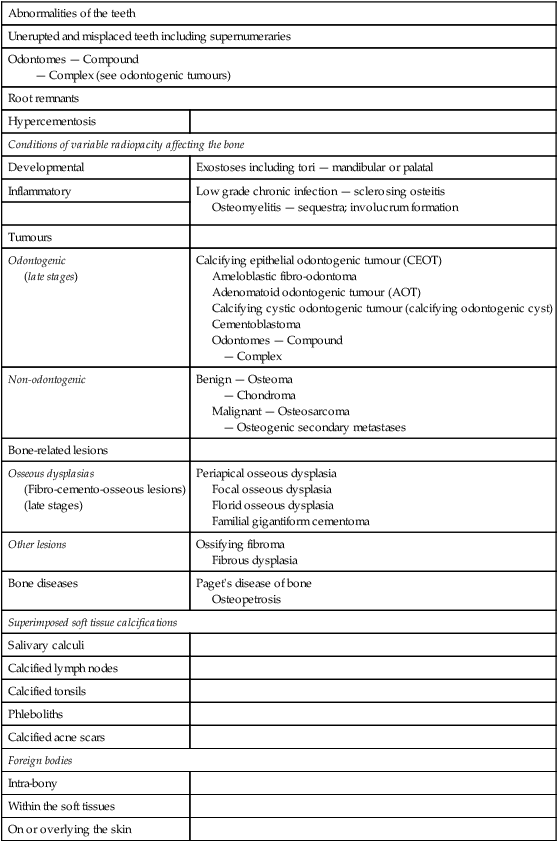
Consider the subdivisions of these pathological categories. A typical list is shown in Table 27.1.
Table 27.1
Classification of the more common lesions that can present as variable radiopacities in the jaws
| Abnormalities of the teeth | |
| Unerupted and misplaced teeth including supernumeraries | |
| Odontomes — Compound — Complex (see odontogenic tumours) |
|
| Root remnants | |
| Hypercementosis | |
| Conditions of variable radiopacity affecting the bone | |
| Developmental | Exostoses including tori — mandibular or palatal |
| Inflammatory | Low grade chronic infection — sclerosing osteitis Osteomyelitis — sequestra; involucrum formation |
| Tumours | |
| Odontogenic (late stages) |
Calcifying epithelial odontogenic tumour (CEOT) Ameloblastic fibro-odontoma Adenomatoid odontogenic tumour (AOT) Calcifying cystic odontogenic tumour (calcifying odontogenic cyst) Cementoblastoma Odontomes — Compound — Complex |
| Non-odontogenic | Benign — Osteoma — Chondroma Malignant — Osteosarcoma — Osteogenic secondary metastases |
| Bone-related lesions | |
| Osseous dysplasias (Fibro-cemento-osseous lesions) (late stages) |
Periapical osseous dysplasia Focal osseous dysplasia Florid osseous dysplasia Familial gigantiform cementoma |
| Other lesions | Ossifying fibroma Fibrous dysplasia |
| Bone diseases | Paget’s disease of bone Osteopetrosis |
| Superimposed soft tissue calcifications | |
| Salivary calculi | |
| Calcified lymph nodes | |
| Calcified tonsils | |
| Phleboliths | |
| Calcified acne scars | |
| Foreign bodies | |
| Intra-bony | |
| Within the soft tissues | |
| On or overlying the skin | |
Step V
Compare the radiological features of the unknown opacity with the typical radiological features of these possible conditions. Then construct a list showing, in order of likelihood, all the conditions that the lesion might be. As mentioned in Chapter 26, this list forms the radiological differential diagnosis.
The typical radiographic features of the important radiopacities are described below using a similar style to that adopted in Chapter 26. It must be emphasized that this is a simplified approach and that most lesions can produce a variety of appearances.
Typical radiographic features of abnormalities of the teeth
Unerupted or misplaced teeth including supernumeraries (Fig. 27.2)
Odontomes
Although both compound and complex odontomes are more accurately classified as epithelial odontogenic tumours with odontogenic ectomesenchyme showing dental hard tissue formation (WHO Classification 2005), they are often also described as dental developmental anomalies (see Ch. 24).
Typical radiographic features of conditions of variable opacity affecting bone
Developmental
Exostoses, including tori (mandibular or palatal)
Exostoses are small, irregular overgrowths of bone sometimes developing on the surface of the alveolar bone. They consist primarily of compact bone and produce an ill-defined radiopacity when superimposed over the bulk of the alveolar bone. Usually two views are required to establish the exact site (see Fig. 27.7).
Specific exostoses develop in particular sites and are often bilateral:
• Torus mandibularis – lingual aspects of the mandible, in the premolar/molar region
• Torus palatinus – either side of the midline towards the posterior part of the hard palate.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


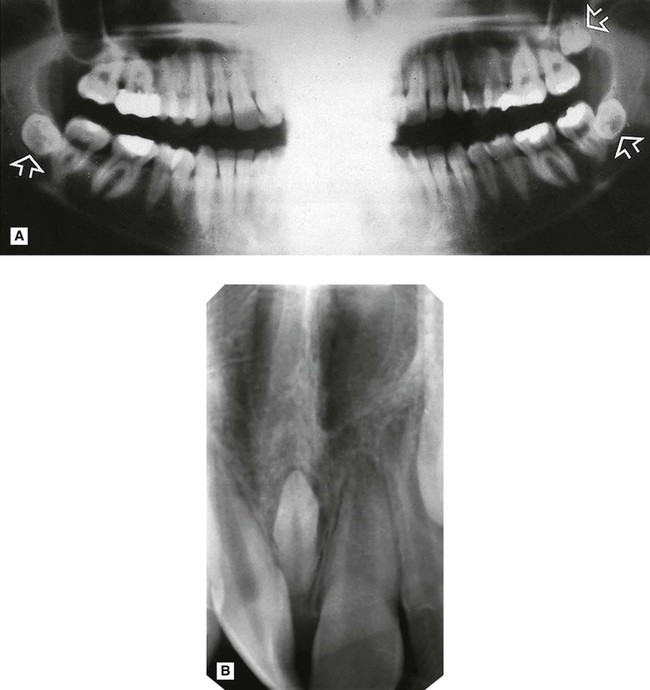
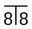 are positioned transversely. B Periapical showing a conically shaped mesiodens (arrowed) between
are positioned transversely. B Periapical showing a conically shaped mesiodens (arrowed) between 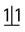 . Density, shape and outline confirm that the opacity is composed of dental tissue.
. Density, shape and outline confirm that the opacity is composed of dental tissue.
 region showing a radiopaque compound odontome (arrowed), consisting of small denticles. B Axial CBCT scan showing another compound odontome in the
region showing a radiopaque compound odontome (arrowed), consisting of small denticles. B Axial CBCT scan showing another compound odontome in the  region (arrowed).
region (arrowed).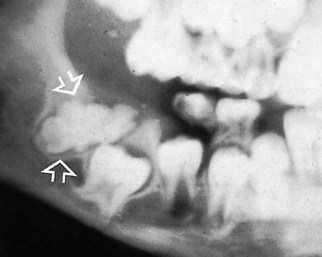
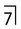 (arrowed). It is preventing the eruption of
(arrowed). It is preventing the eruption of 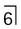 . The opacity shows the characteristic surrounding radiolucent line, confirming its dental tissue origin.
. The opacity shows the characteristic surrounding radiolucent line, confirming its dental tissue origin.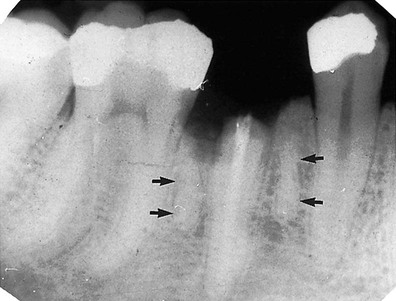
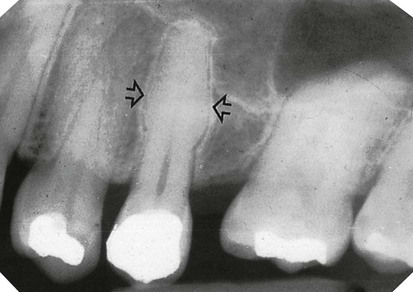
 root caused by the root remnants of the deciduous
root caused by the root remnants of the deciduous  .
.
 (arrowed).
(arrowed).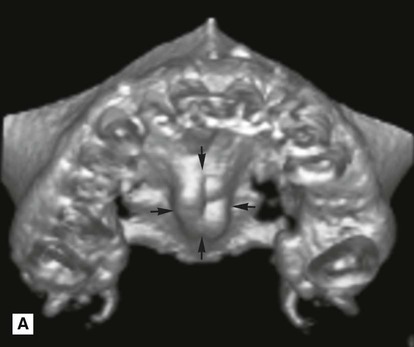 />
/> />
/>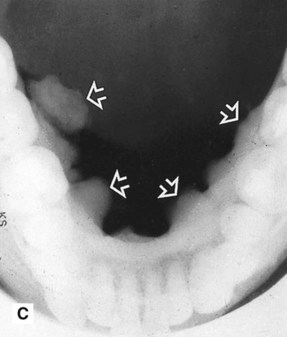
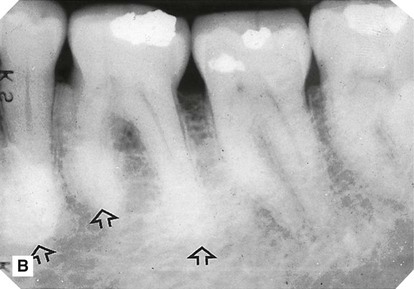
 showing ill-defined areas of radiopacity (arrowed) overlying the teeth. C Lower 90° occlusal of the same patient showing the large irregular exostoses (mandibular tori) on the lingual aspect of the mandible (arrowed).
showing ill-defined areas of radiopacity (arrowed) overlying the teeth. C Lower 90° occlusal of the same patient showing the large irregular exostoses (mandibular tori) on the lingual aspect of the mandible (arrowed).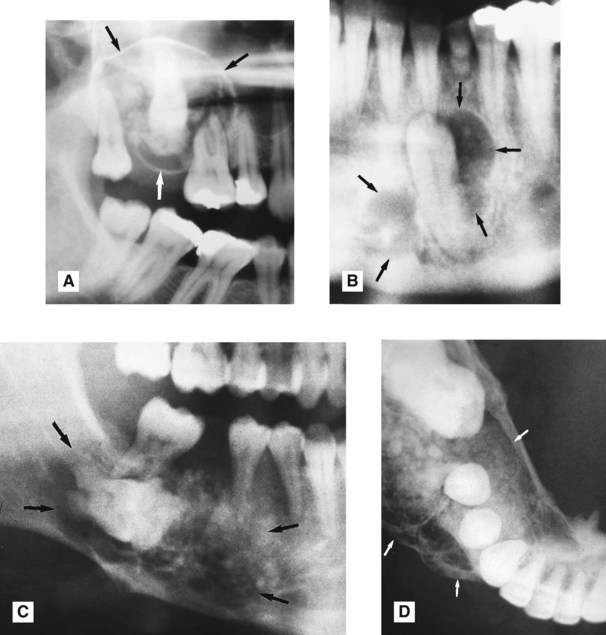
 . There are obvious areas of calcification within the lesion. B Part of a panoramic radiograph showing another CEOT (arrowed) associated with the unerupted lower left canine, with only faint internal calcification. C Right side of a panoramic radiograph showing a poorly defined calcifying epithelial odontogenic tumour (arrowed) associated with the unerupted molar. D Lower 90° occlusal of the same patient showing the expansive, multilocular nature of the lesion and the discrete internal calcifications.
. There are obvious areas of calcification within the lesion. B Part of a panoramic radiograph showing another CEOT (arrowed) associated with the unerupted lower left canine, with only faint internal calcification. C Right side of a panoramic radiograph showing a poorly defined calcifying epithelial odontogenic tumour (arrowed) associated with the unerupted molar. D Lower 90° occlusal of the same patient showing the expansive, multilocular nature of the lesion and the discrete internal calcifications.