CHAPTER 21 Provisional Prostheses
TOTALLY EDENTULOUS INTERIM PROSTHESES
First Stage
The patient usually has a complete denture that has been used for the jaw requiring treatment. Chapter 20 describes the preparation of a new denture and a replicated clear template, which subsequently serve as radiographic indicators for computed tomography (CT) scans, a surgical template, and an interim prosthesis. These prostheses must be made with unfailing attentiveness to classic prosthetic principles. Vertical dimension, centric occlusion, incisal length, free-way space, tooth position and angulation, and patient-approved cosmetics must be satisfied. Except for retention, the final implant-borne prosthesis can never be better than the initial one, the characteristics of which govern implant locations and emergence angles.
Occlusal relationships must be precisely the same as they were before these alterations were made.
Second Stage
Its progenitor, the surgical template (which should have been retained), is brought to the host area. With the assistance of the radiopaque markers and carefully made mapping notes, each implant, although not visible through the mucosa, can be located (see Chapter 9).
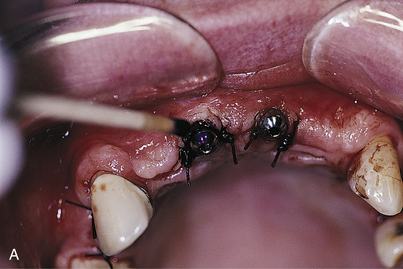
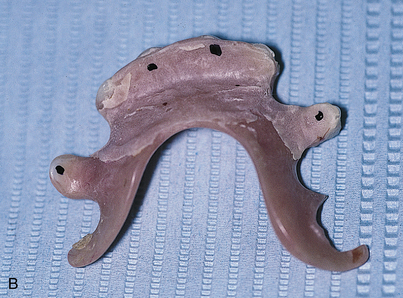
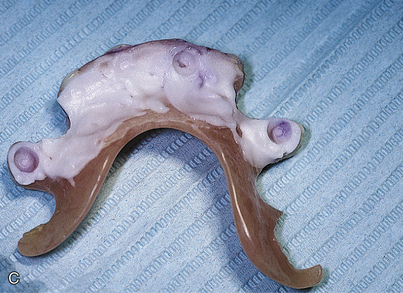
The exact locations in contact can be revealed by touching the dried occlusal surfaces of the abutments or collars with pressure indicator paste (PIP) and placing the denture, now relieved of its soft lining, against them (Fig. 21-1). Concentration on eliminating these areas leads to a prosthesis that is totally relieved of directing pressure to the implants. Again, a soft lining of choice is placed. Definitive prosthetic measures are completed while this removable interim denture serves in its classically versatile manner.
At second-stage surgery, the dentist and patient may want to substitute a fixed interim prosthesis for the removable one. This decision is based on the same principles that govern the design of fixed prostheses (see Chapter 24). The following section presents advice on preparing such devices and may be followed with essentially no modifications.
PARTIALLY EDENTULOUS INTERIM PROSTHESES
Implant-borne restorations range from single tooth (see Chapter 23) to more sophisticated, complex implant/tooth designs. The provisional prostheses may be removable or fixed, but they always must respect the recently submerged implants.
If a fixed provisional prosthesis is urgently needed, even when few or no potential abutments are available, the surgeon may plan to add some strategically placed implants at the time of first-stage surgery, in addition to those inserted for therapeutic use. Regions such as the tuberosities, pterygoid plates, or interimplant spaces may be suitable for placement of regular implants or mini-implants (see chapters 9 and 19). Although no significant expectations should be held for their long-range prognosis, some mini-implants succeed at osseointegration and may be kept for incorporation into the final prosthesis. Those that do not, because of mobility or bone loss or because they are not required for final superstructure stabilization because of location or angulation, can be shaved level to the gingivae or must be removed. Periodic radiographic and clinical observation of these interim implants is important, because peri-implant disease, if present, can affect adjacent teeth and implants. In such cases, immediate removal and repair are indicated (see Chapter 24).
Single-Tooth Implant Restorations
First Stage
In any event, the patient should be provided with a prosthesis that is not tissue borne.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses