A. Dental plaque-induced gingival diseases
Whether they are associated with hormonal imbalances, mediations, systemic disorders, or malnutrition, these gingival diseases have the following characteristics in common (Mariotti, 1999):
— The signs and symptoms are confined to the gingiva.
— Plaque is the main etiological factor which will initiate or exacerbate the gingival lesions.
— Inflammation of the gingival tissues will produce changes in color (transition to a red/bluish-red hue), shape (enlarged gingival contours due to edema or fibrosis), texture, bleeding upon stimulation, and elevated sulcular temperature (
Figure 2.1).
— There is no alveolar bone loss and pocket depth; clinical attachment levels around teeth are stable.
— This is a reversible condition which resolves upon removal of the etiological factors.
— Possible role as a precursor to attachment loss around teeth.
Gingivitis primarily induced by dental plaque includes the following disease subdivisions:
1. Gingivitis associated with dental plaque only: Signs and symptoms typical of gingivitis can be observed at all ages of dentate populations and this disease has been considered to be the most common form of periodontal disease (Page, 1985). The disease can be observed in a child as young as five years of age, progress with a peak during puberty, and remain present throughout life at various extents. Plaque is present at the gingival margin and a positive correlation exists between gingivitis and plaque accumulation.
There is no pathognomonic flora associated with gingivitis, although the dental plaque in gingivitis differs from that present in gingival health (Ranney, 1993). Note that gingivitis may also occur on a reduced periodontium (decreased amount of alveolar bone height and connective tissue support around teeth) which was previously surgically treated for a periodontitis. This situation is encountered when there is a recurrence of inflammation of the marginal gingiva on a periodontium with previous attachment loss but without any evidence of progressive attachment loss (no indication of active disease) (Mariotti, 1999).
a. Without local contributing factors
b. With local contributing factors (see VIII A, below):
— Artefacta gingivitis (automutilation)
2. Gingival diseases modified by systemic factors:
a. Associated with the endocrine system
This type of gingivitis is caused by a combination of plaque and steroid hormones. The composition of dental plaque remains non-specific (non-related to the microbiological analysis).
1) Puberty-associated gingivitis: A rise in gingival inflammation and gingival volume is noted during puberty in both sexes without necessarily seeing a rise in the quantity of plaque (Sutcliffe, 1972). The incidence of the severity of gingivitis in adolescence is not only related to the rise in steroid hormones but is also influenced by a variety of factors such as dental caries, mouth breathing, teeth crowding, and tooth eruption (Stamm, 1986). These changes are reversible after puberty. More specifically, hyperplastic gingivitis often seen during the adolescence period can be associated with:
— Orthodontic treatment: Note that fibrotic tissue tends to recur if surgical removal is attempted during orthodontic treatment. It is recommended to wait until orthodontic appliances are removed before surgically removing excess tissue (
Figure 2.2).
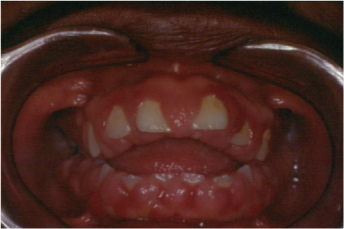
— Mouth breathing: Mouth breathing, which often accompanies Angle’s classification 2 division 1 malocclusion, is considered to be an exacerbating factor to gingivitis (Lindhe, 2003). Gingival hyperplasia tends to affect mostly the anterior superior region and is also prone to recurrence if surgical removal is performed without any correction of the actual mouth breathing through orthodontic treatment or cessation of habit.
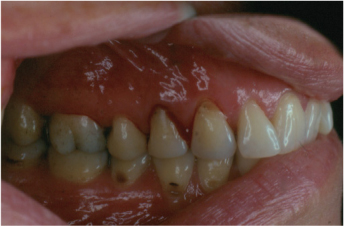
Figure 2.1. Localized gingivitis, characterized by bleeding upon probing. There is no attachment loss.
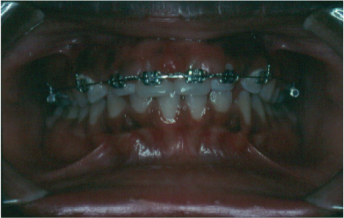
Figure 2.2. Maxillary generalized moderate gingivitis following the placement of braces. Notice the difference with the mandibular arch, which does not have braces.
2) Menstrual-cycle-associated gingivitis: The most common sign is a minor gingival inflammation during ovulation; gingival exudate has been shown to increase at least 20% in 75% of women (Hugoson, 1971). This situation is reversible after ovulation.
Note: Hormonal gingivitis or post-menopausal gingivitis can be seen in women taking hormone replacement therapy. Signs and symptoms may involve atrophic, thin, erythematous gingival tissues and patient complaints of gingival sensitivity to spicy foods and acidic beverages. Palliative treatment is suggested.
3) Pregnancy-associated:
a) Gingivitis: A combination of pregnancy hormones and dental plaque may increase the severity of gingivitis in women sensitive to local irritants. In addition to the typical gingivitis signs, severe inflammation can develop in the presence of relatively low amounts of dental plaque (Hugoson, 1971). It will usually affect pregnant women in their second or third trimester, and is reversible after child delivery.
b) Pyogenic granuloma: This refers to a mass of hyperplastic gingival tissue principally found in the interdental maxillary regions (
Figure 2.3). It is not a tumor but an exaggerated inflammatory response to irritation resulting in a solitary poliploid capillary hemangioma which can easily bleed upon mild provocation (Sills et al. 1996). Pregnancy-associated pyogenic granuloma presents clinically as a painless protuberant exophytic mass attached by a sessile or pedunculated base from the gingival margin. It has been reported to occur in 0.5% to 5% of pregnancies and can develop as early as the first trimester (Mariotti, 1999). It usually regresses or completely disappears following parturition. If needed, surgical excision can be performed post-partum. The treatment for pregnancy-associated gingivitis and pyogenic granuloma during pregnancy is an impeccable control of the etiological factors (scaling, prophylaxis, and chlorhexidine rinses).
Figure 2.3. Pyogenic granuloma between teeth number 4 and 5. Reprinted with permission from Chapple and Hamburger, 2006.
4) Diabetes-mellitus-associated gingivitis: Diabetes mellitus is a complex disease with varying degrees of systemic and oral complications involving abnormalities in insulin production, fat, proteins, and sugar metabolism, and resulting in an impaired vascular and immune system as well as an inadequate inflammatory response. Diabetes mellitus is categorized as Type 1 and Type 2. Type 1 develops due to impaired production of insulin and Type 2 is caused by deficient utilization of insulin. There is evidence to suggest that uncontrolled Type 1 diabetes in children is associated with exaggerated response of the gingival tissues to dental plaque (Lindhe, 2003). It is a reversible condition once the diabetes is under control and the dental plaque is removed.
b. Associated with blood dyscrasias
1) Leukemia-associated gingivitis: Leukemia is a progressive malignant hematological disease characterized by the development of abnormal leukocytes and leukocytes precursors in the blood and bone marrow. Leukemia is classified according to disease progression (acute or chronic), cell types involved (myeloid or lymphoid), and cell numbers in blood (leukemic or aleukemic). The oral manifestations are acute, consisting of cervical adenopathies, petechia, gingival enlargements, and mucous ulcers. Dental plaque can exacerbate the gingival inflammatory changes which include swelling, redness/blueness, sponginess, and glazed appearance of the gingiva which is infiltrated with leukemic cells (Lindhe, 2003). Persistent and unexplained gingival bleeding may indicate an underlying thrombocytopenia associated with the leukemic condition. Lesions are often found in the acute monocytic type, and consist of a modified gingival volume and bleeding of gingiva upon touch. Symptoms lessen when antiseptic mouthwashes are used and plaque volume is reduced.
2) Other
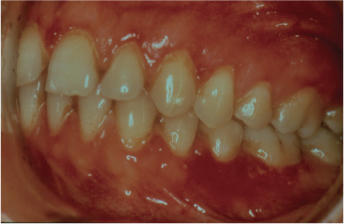
Figure 2.4. Gingival diseases modified by medications. cyclosporine-A-induced gingival enlargement in a 16-year-old after heart transplant.
3. Gingival diseases modified by medications:
a. Drug-influenced gingival diseases
1) Drug induced gingival enlargement: Three commonly used classes of medications create these lesions:
— Anti-convulsant drug used for treatment of epilepsy: Dilantin (Phenytoin sodium), 50% incidence
— Immunosuppressant drug used to avoid host rejection of grafted tissues: Cyclosporin A, 25% to 30% incidence (Over time, this drug is tapered and the gingival enlargements become easier to control.) (Figure 2.4)
— Calcium channels blocking agents used as hypertensive drugs: Nifedipine, Verapamil, Diltiazem, 15% to 20% incidence
Individuals taking these medications may develop gingival enlargements leading to pseudopockets. Characteristics of drug-influenced gingival enlargement include (Mariotti, 1999):
— Predilection of anterior gingiva; starts interproximally and expands
— Higher prevalence in children
— Onset within the first three months of taking the drug
— Enlargement of the gingival contours appears
— Stippling is present in the gingiva
— Pronounced inflammatory response in relation to the plaque volume
— Not associated with attachment loss but can be found in periodonitums with and without bone loss
Treatment consists of control of etiological factors followed by full mouth gingivectomy. Gingivectomy (full mouth or local) may need to be performed annually. If possible, the drugs can also be changed or dosages adjusted to improve the oral condition.
2) Drug influenced gingivitis:
a) Oral contraceptives: Studies have shown that women taking oral contraceptive drugs have a higher incidence of gingival enlargement in comparison to women who do not take the medications (Kaufman, 1969). Pronounced inflammation (change in gingival contour, color, exudate) is seen and is reversible upon removal of medications (
Figure 2.5).
b) Other
4. Gingival diseases modified by malnutrition:
a. Ascorbic acid deficiency gingivitis: Nutritional deficiencies such as ascorbic acid (vitamin C deficiency) can significantly exacerbate the response of the gingiva to plaque bacteria (Mariotti, 1999). The clinical description of severe vitamin C deficiency or scurvy consists of bulbous, spongy, hemorrhagic, swollen, and erythematous gingival lesions (Charbeneau et al., 1983). This condition is unusually seen in areas of adequate food supply but can potentially affect infants of low socioeconomic families, institutionalized elderly individuals, and alcoholics.
b. Other
B. Non-dental-plaque-induced gingival lesions
Although these gingival lesions are not produced by plaque and do not disappear when plaque is removed, it should be noted that the severity of the clinical manifestation can often be related to the presence of bacterial plaque.
1. Gingival lesions of specific bacterial origin:
These types of gingivitis and stomatitis can be found in immunocompromised and immunocompetent individuals. They occur when the microorganisms surpass innate host resistance. Clinical signs may range from painful, edematous ulcerations to asymptomatic cancres, mucosal patches, or atypical non-ulcerated inflamed gingiva. Lesions elsewhere on the body may also be present. Gingival lesions may occur due to infections with Neisseria gonorrhea, Treponema pallidum, streptococci, or other organisms.
a. Neisseria-gonorrhea-associated lesions: Gonorrhea is a sexually transmitted disease which can affect the oropharyngeal region in approximately 20% of infected individuals (Neville, 2002). Diffuse erythema, small erosive pustules, and edema can be seen in this region as well as on tonsils and uvula. Gingivitis and stomatitis, as well as a sore throat and a cervical or submandibular lymphadenopathy may also be present.
b. Treponema-pallidum-associated lesions: Syphilis is a chronic infection produced by Treponema pallidum. The primary modes of transmission are sexual contact or mother to fetus. The infection undergoes a characteristic evolution that classically proceeds through three stages: In primary syphilis, an asymptomatic contagious chancre appears three to four weeks post contact at the site of inoculation. When affecting the oral cavity, it can affect the lips, gingiva, tonsils, tongue, and palate. It leaves a scar and heals spontaneously. In secondary syphilis, whitish mucous patches as well as maculopalular cutaneous rashes are often present and are still contagious at this point. In tertiary syphilis, a non-contagious granulomatous inflammation (gumma) reaction appears which can often cause necrosis and perforation of the tongue or palate. Serious systemic conditions are involved (Neville, 2002).
c. Streptococcal-species-associated lesions: An upper respiratory tract infection usually causes fever and accompanies a diffuse gingivitis, tonsillitis, pharyngitis and ulceration of the oral mucosa. One of the most common species involved is the group A, β-hemolytic streptococci (Neville, 2002).
d. Other
2. Gingival diseases of viral origin: Several viral infections are known to cause gingivitis. Most of them enter the body during childhood and may give rise to the disease followed by periods of latency.
a. herpesvirus infection
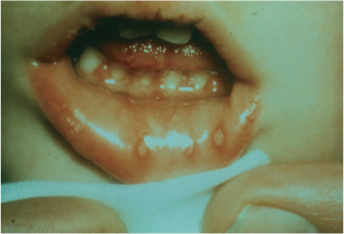
1) Primary herpetic gingigostomatitis: Herpes simplex virus type 1 (and occasionally type 2) is responsible for causing the primary infection which involves painful severe gingivitis with ulcerations (on keratinized and non-keratinized tissues) and edema followed by stomatitis. High fever and malaise is generally present. Vesicles on lips can produce a crusty lips appearance after rupturing (Miller, 1992) (
Figure 2.6).
Palliative treatment only is required. The infection lasts approximately 10 days. During this period, the patient must be well hydrated with liquids and topical application of anesthetic agents is also indicated. Chlorhexidine and an antibiotic may be needed to prevent a super-infection. In the adult infection, antiviral drugs such as Zovirax, #70, 200 mg, 1 tab qid, for 2 weeks can be prescribed.
2) Recurrent oral herpes: Reactivation of the virus resulting in recurrent infections occurs in 20% to 40% of individuals with the primary infection (Greenberg, 1996). These lesions (vesicles which become ulcers) usually only affect the keratinized tissues and are usually present unilaterally or locally. The treatment, if any, can consist of topical antiviral ointment or tablets.
3) Varicella-zoster infection: Varicella-zoster virus causes varicella (chickenpox) as the primary self-limiting infection. The virus then remains latent and can be reactivated resulting in the herpes zoster infection. This painful unilateral infection is often seen in older individuals and is accompanied by cutaneous lesions of the affected nervous territory (Miller, 1996).
Figure 2.6. Primary herpetic gingivostomatitis in a child. Notice the characteristic lesions on the lower lip. Photo courtesy of Iain Chapple.
b. Other: Such as herpangina, caused by the Coxsackie virus species.
3. Gingival diseases of fungal origin: The most frequent oral fungal infections consist of candidosis and histoplasmosis.
a. Candida-species infections: C.
albicans is one of the most frequent candida species affecting the oral cavity. It is considered an opportunistic infection occurring when the host resistance is diminished. Most subtypes of candidosis can be treated with anti-fungal medications (Ketoconazole 200 mg, 1 tab/day, 10 days, or Fluconazole 100 mg, 1 tab/day, 14 days).
1) Generalized gingival candidosis include:
— Acute types:
* Pseudomembranous candidosis: This type of infection produces soft white patches disseminated throughout the oral mucosa. These patches can be removed with an instrument leaving behind an erythematous mucosal surface.
* Atrophic or erythematous candidosis: This type of infection produces red lesions spreading all over the oral mucosa. They are associated with severe pain and discomfort.
— Chronic types:
* Hyperplasic candidosis: Typically, the lesion is longstanding and presents itself as a thick white patch which cannot be rubbed off (leukoplakia correlation).
* Mucocutaneous: This type of candidosis mostly affects the skin, scalp, and nails; much more rarely it affects the gingiva.
— Prosthetic stomatitis (types 1,2,3)
b. Linear gingival erythema: This disease was initially termed “HIV-related gingivitis.” It mostly affects immunocompromised individuals or HIV patients. The unusual pattern of inflammation appears as a distinctive linear band of erythema which involves 2 to 3 mm of marginal gingival (Neville, 2002). Redness can be circumscribed or diffused and can spread until it passes the mucogingival junction. It is often generalized in the oral cavity, but can be localized to just a few teeth. The main characteristic is that it does not respond to conventional treatment (SRP and plaque control).
Note: the HIV patient is also more prone to:
— Hyperplasic candidosis
— Pseudomembranous candidosis
— Cheilitis
— Ulcerative necrotizing gingivitis, ulcerative necrotizing periodontitis
— Hairy leukoplakia
— Kaposi’s sarcoma
c. Histoplasmosis: Histoplasmosis is a granulomatous disease caused by Histoplasma capsulatum and represents one of the most frequent systemic mycoses in the United States. The frequently seen subclinical development of infection usually includes either a pulmonary chronic histoplasmosis (30% have oral manifestations) or a disseminated form found primarily in HIV patients (60% have oral manifestations). Oral findings can consist of painful granulomatous ulcerations (Holmstrup, 1999).
d. Other
4. Gingival lesions of genetic origin:
a. Hereditary gingival fibromatosis: This gingival hyperplasia (ginvival overgrowth) is an uncommon condition of genetic origin. Of idiopathic etiology, this condition develops irrespective of effective plaque removal. Hereditary gingival fibromatosis can be an isolated condition or part of a syndrome or systemic condition (Gorlin et al., 1990) (
Figure 2.7).
b. Other
5. Gingival manifestations of systemic conditions:
a. Mucocutaneous disorders: Many dermatologic diseases present with gingival manifestations in the form of desquamative, ulcerative, or erythematous gingival lesions. The most relevant ones are presented in the following below:
1) Lichen planus: Lichen planus is one of the most common dermatological diseases affecting the oral cavity. Of autoimmune etiology, it can be classified according to the following subtypes: reticular, atrophic, plaque, erosive, and bullous. The characteristic clinical appearance resembles desquamative chronic gingivitis with the presence of white pa/>
Only gold members can continue reading.
Log In or
Register to continue