Causal Therapy
Causal therapy is the first stage in the treatment of periodontal disease, a complex multifactorial condition whose manifestations are caused by pathogenic bacteria in association with other local and systemic factors (oral hygiene, environment, host susceptibility). Therefore the treatment of periodontal diseases needs a multilevel therapeutic approach (Figure 2-1).
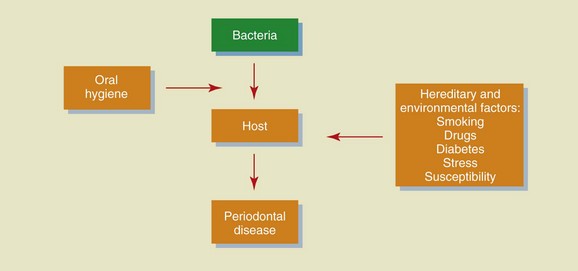
Figure 2-1 Causes of periodontal disease.
Diagnosis
Clinical Records
Clinical documentation consists of collecting data through the following:
Examination
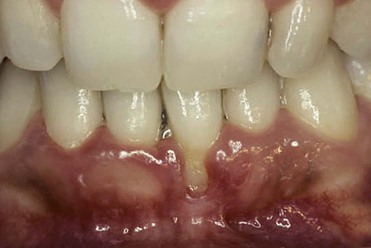
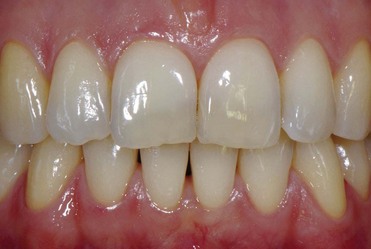
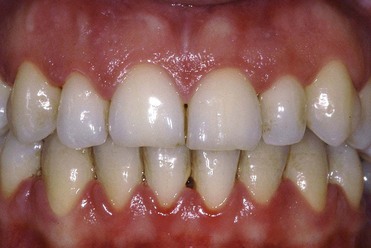
The tissues are examined to assess the shape, color, surface appearance, size, and architecture of soft tissues. The periodontal tissues can be classified into two main types: thin scalloped architecture and thick flat architecture (Figures 2-2 and 2-3).
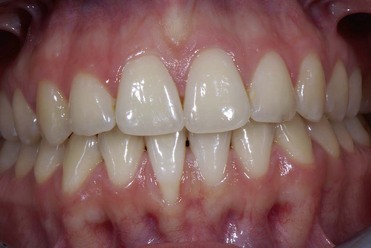
Figure 2-2 Thin and scalloped architecture.
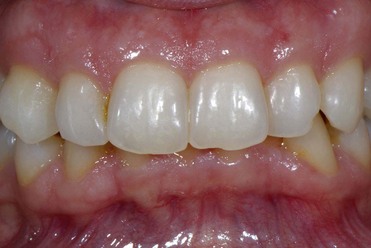
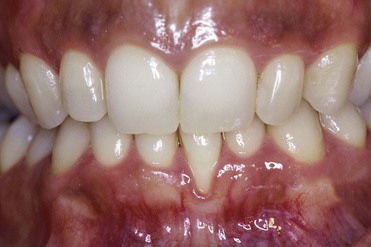
Figure 2-3 Thick and flat architecture.
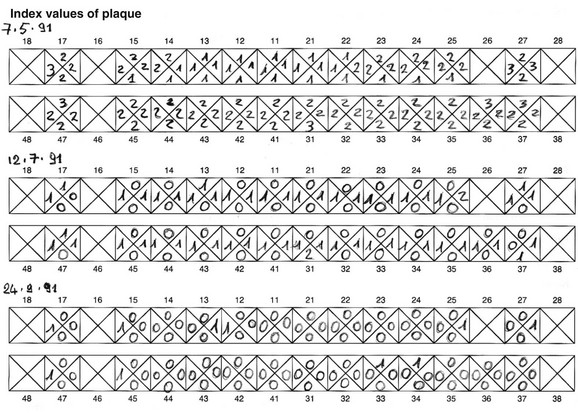
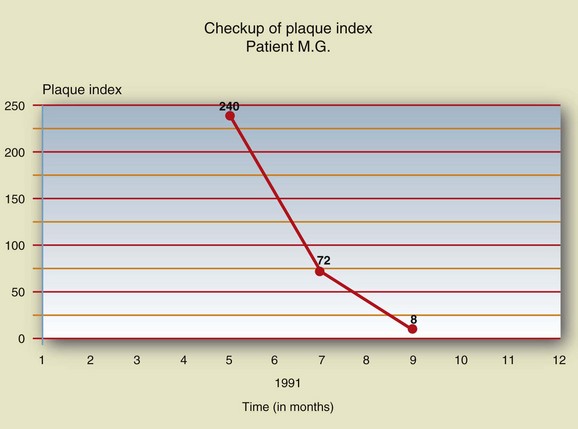
The collected data should carefully be recorded on a special chart to be consulted and updated at every periodontal maintenance appointment in order to observe changes over time (Figures 2-4 to 2-7).
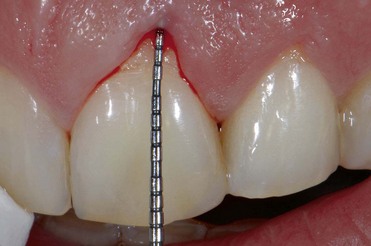
During examination, the extent of tissue inflammation is determined by means of the gingival index (Löe, 1967), whose values range from 0 to 3 (Figures 2-8 to 2-11).
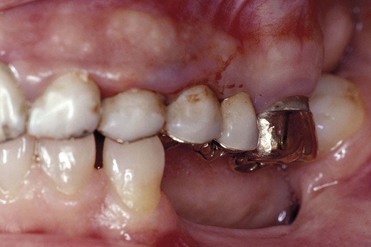
Figure 2-11 Gingival index 3: spontaneous bleeding.
Periodontal Probing
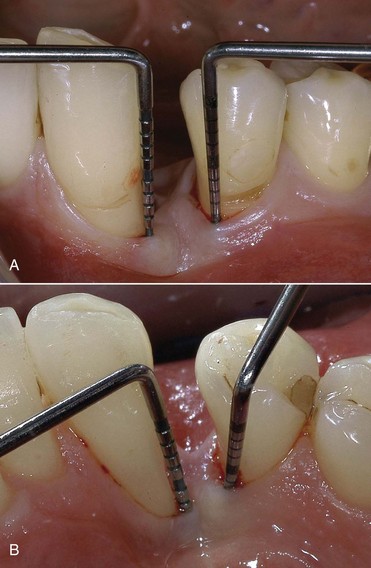
Probing makes it possible to evaluate the loss of attachment (clinical attachment level [CAL]), which is a pathognomonic sign of periodontitis. Probing is performed with straight and curved probes that have 1-mm scale markings (Figure 2-12). Using a probe, the specialist can determine the probing access to the sulcus and bifurcations, respectively, and can assess the presence of calculus on the root surface, the topography of the periodontal pockets, BOP, and any retraction of the tissues after treatment. Probing is affected by several factors:
• Shape of the probe: A probe with a pointed tip penetrates the tissues more easily than a blunt instrument.
• Pressure applied on the probe: Strong pressure causes deeper penetration of the probe.
• Probing angle: Faulty prosthetic restoration can prevent proper insertion of the probe, leading to incorrect values.
• Local anatomic conditions: The presence of an enamel pearl, or calculus deposits on the root surfaces, can hamper probing of the site.
• Tissue inflammation: Edema and inflammation make the tissue more difficult to penetrate.
Probing Depth
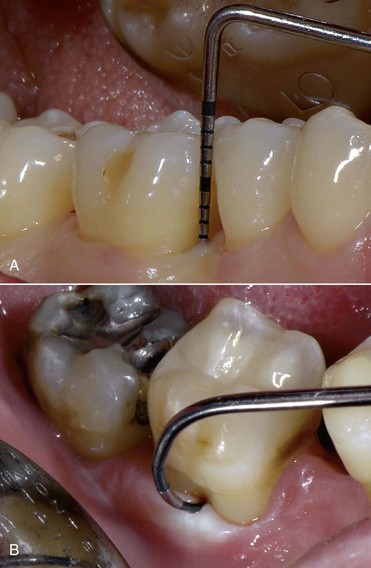
Probing depth (PD) corresponds to the depth of the periodontal pocket and is represented by the distance between the gingival margin and the bottom of the pocket, which is the ideal habitat for periodontal pathogenic bacteria (Figure 2-13; see also Figure 2-12).
Bleeding on Probing
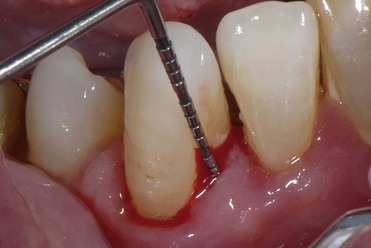
BOP is the parameter used to assess the presence of inflammation. The probe is inserted to the bottom of the periodontal pocket, gently slid against the surface of the tooth or root. If this maneuver induces bleeding from the apical region of the pocket, the area is considered to be inflamed (Figure 2-14).
Radiographic Records
Indications and Characteristics
Radiographs are stored and organized on special supports (full mouth series) (Figures 2-15 and 2-16).
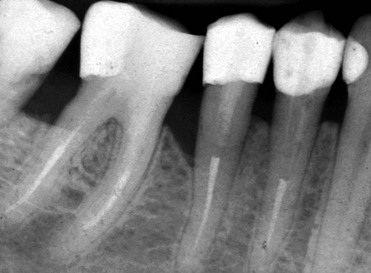
Figure 2-15 Intraoral radiograph.
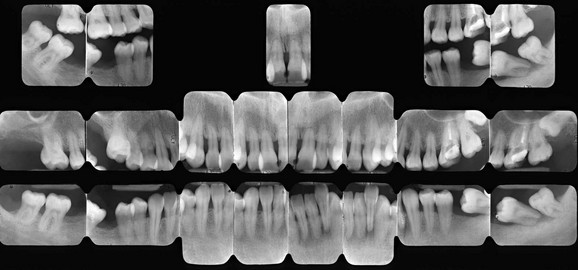
Figure 2-16 Full mouth series.
• Radiographs do not show the true buccal and lingual conditions, as the presence of mineralized tissues can disguise them.
• It provides a two-dimensional image of three-dimensional structures. For an in-depth examination of the anatomic conditions, one should use computerized axial tomography (CAT) scans.
• The radiographic image is subject to deformations caused by x-ray beam inclination and the shape and thickness of the examined structures.
• During the initial phase of the disease, when the clinical symptoms may already be apparent, the radiographic image does not show signs of pathologic alterations.
• Errors of execution or centering, poor film quality, and the wrong exposure time or development can affect the interpretation of radiographic images.
• Radiographs show changes in the mineralized portion of the periodontium but not in the soft tissues.
• The radiographic image of the destruction of the mineralized periodontal components is always less severe compared with the real status.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses