Chapter 16 Porcelain Veneers
Section A Porcelain Veneers
Relevance of Porcelain Veneers to Esthetic Dentistry and Brief History of Clinical Development and Evolution of the Procedure
Treatment Planning
Conventional dentistry focuses on treatment for dental disease and diminished oral function (traditional dentistry).
Esthetic dentistry also focuses on treatment for dental disease and function, but has the added proviso that the restoration strongly resembles the original tooth in shape and color.
Cosmetic dentistry focuses on elective treatment. The difference between esthetics and cosmetics is semantic: esthetic dentistry is needed dentistry with a naturally esthetic result whereas cosmetic dentistry is elective dentistry that alters the appearance beyond natural parameters.
Clinical Case Study
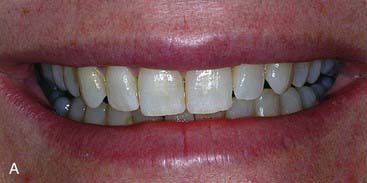
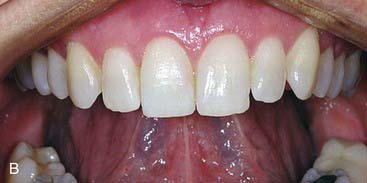
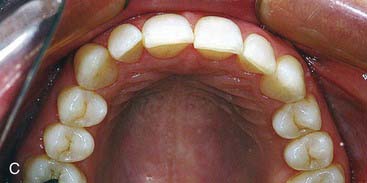
The elective case presented here was performed to enhance the patient’s smile by providing 10 porcelain veneers with minimal preparation. Layered porcelain was used to achieve the maximum esthetics in a veneer. Figure 16-1, A, shows the patient’s smile before treatment. Her teeth were slightly malaligned, but were in excellent condition. She was free from dental disease and was well aware that the cosmetic treatment she was seeking was not reversible and not permanent. She was comfortable with a 10- to 15-year life expectancy of her veneers and was prepared to replace them when needed to achieve the esthetic benefits they would provide. Figure 16-1, B, shows a retracted view of the maxillary 10 most anterior teeth before treatment, and Figure 16-1, C shows the incisal view of her teeth before treatment.
Preparation
The first step was to anesthetize the patient’s teeth and place depth cuts of 0.5 mm on the facial surfaces of the teeth to be veneered (Figure 16-2, A). The depth cuts were joined with a chamfer-ended diamond bur (Figure 16-2, B). Subtle chamfer margins were created at the height of the tissue (Figure 16-2, C). Incisal preparation involved 1.0 to 1.5 mm of reduction, leaving a “butt” margin and rounded corners (Figure 16-2, D). Interproximal preparation involved continuing the chamfer to the proximal contacts, forming an “elbow” preparation (Figure 16-2, E). A diamond strip was used to slightly open the contacts (Figure 16-2, F). Where no occlusal preparation was performed on the premolar teeth, a 0.25-mm horizontal groove for seating purposes was placed (Fi/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses