Chapter 14
Management of Maxillofacial Trauma
- Initial assessment
- Applied anatomy
- Diagnosis
- Treatment planning
- Principles of treatment
- Definitive treatment
- Complications of fractures
The commonest causes of fractured jaws are fights, road accidents, falls and sport. They occur chiefly in males between 15 and 35 years of age and twice as frequently in the mandible as in the maxilla. Fractures may be direct, following a blow at the point where the break occurs, or may be indirect as a result of a blow on the bone at some distance from where the lesion occurs. They may be single, linear or comminuted, that is fragmented into two or more small pieces, and are said to be compound when they communicate with a wound in the skin or mucous membrane of the mouth, nose or air sinuses. Where there is a tooth in the line of the fracture the latter is almost certainly compound into the mouth through the periodontal membrane. In the young, incomplete or greenstick fractures of the mandible can occur. Diseases of the bone predispose to spontaneous pathological fractures. All traumatised patients need to be fully assessed.
Initial Assessment
The American College of Surgeons has established a pattern of assessment of the traumatised patient that has been adopted as the gold standard in many countries around the world. This is disseminated through advanced trauma life support courses (ATLS). The initial assessment should not concentrate on the most obvious injury but involve a rapid survey of the vital functions to allow management priorities to be established. The primary survey involves:
- A – airway maintenance with cervical spine control
- B – breathing and ventilation
- C – circulation with haemorrhage control
- D – disability: neurological status
- E – exposure: complete examination of the patient.
During the primary survey, resuscitation is performed and afterwards shock management is initiated with fluid replacement while the vital signs are monitored for any deterioration in the status of the patient.
Once the patient is stabilised a secondary survey is carried out to ensure that all traumatic injuries are evaluated, after which definitive care can be prioritised.
Airway and Cervical Spine
In unconscious patients respiratory obstruction may be caused by blood clot, or a foreign body in the oropharynx or larynx. In bilateral fractures of the mandible through the canine region the tongue may fall back to occlude the airway. In maxillary injuries the palate can be displaced down and back to occlude the oropharynx. Cervical spine injury should be suspected in any blunt trauma above the clavicle and excluded by appropriate radiographs. Until then a hard cervical collar should be worn.
Control of the airway is an absolute priority. The tongue or palate is drawn forward and the mouth and pharynx sucked or wiped clear of debris to re-establish the airway. To keep the tongue forward, a suture may be passed through it, or the patient turned on their side, with control of the cervical spine, to allow saliva and blood to drain out of the mouth. Where these measures are ineffective, intubation may be necessary and consideration given to a tracheostomy. Before giving an anaesthetic to the unconscious patient soon after the accident, the stomach must be emptied of swallowed blood using an orogastric tube.
Haemorrhage
Acute bleeding can be life threatening if major vessels are involved and should be controlled as described in Chapter 7.
Surgical Shock
This condition is as a result of excessive blood loss, leading to circulatory collapse. In closed wounds, blood and plasma may bleed from the vessels into the tissue spaces. The abdomen is a common reservoir following major trauma. If the initial loss is over one litre this cannot be compensated for by general vasoconstriction. Where fluid is not replaced, the falling blood pressure and vasoconstriction cause oxygen lack in the tissues and an increased permeability of the capillaries with still further loss of fluid into the tissues.
Signs and Symptoms
The patient is typically cold, sweating and pale or cyanosed. In the limbs the degree of swelling in closed injuries gives some indication of the fluid loss into the tissues, but this is of little use in facial injuries. Increased respiratory rate, rapid pulse and falling blood pressure are strong indications of deterioration.
Treatment
Prompt and energetic measures are necessary. Immediate replacement of fluid is lifesaving whilst arrest of haemorrhage must be undertaken to prevent further loss. Blood pressure and pulse must be continually monitored to gauge the effectiveness of replacement therapy until the patient stabilises. A patient with a pulse rate persistently over 100, and systolic blood pressure of under 100 mmHg (13.3 kPa), requires transfusion of whole blood. Grouping and cross matching should be done early, and intravenous access to allow a saline or plasma substitute drip should be established immediately.
Haemoglobin estimations are of little use in the acute phase owing to the haemoconcentration which usually occurs, but should be checked after haemodilution has taken place.
The circulation to the head is improved by raising the foot of the bed, and oxygen should be administered. Warmth should be applied with blankets to keep the patient in an environmental temperature of 32°C.
Head Injury
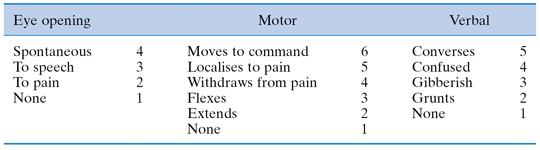
Many patients who sustain facial injuries may also have lost consciousness. All these patients, however short the time they were unconscious, must be fully assessed using the Glasgow Coma Scale (GCS) and referred to a neurosurgeon. The Glasgow Coma Scale consists of ranking of behavioural responses (Table 14.1). Motor responses, verbal responses and eye opening are independently assessed and scored numerically out of a total of 15. The patient’s condition must be carefully observed and recorded for change in GCS status. In addition pulse, blood pressure and pupil reaction to light are monitored, as these reflect changes in intracranial pressure. A rise in intracranial pressure is denoted by a slow reaction to light of the pupil on the affected side and as the pressure increases the pupil becomes fixed and dilated. As the condition of the patient worsens the opposite pupil also dilates. In the initial stages of assessment and resuscitation following acute trauma, monitoring may be virtually continuous but should be maintained even in the apparently stable patient at intervals up to one hourly for 24 hours after the initial trauma.
Table 14.1 Glasgow coma scale (GCS). Take the best score from each category to give a total coma score

Prevention of Infection
External wounds are kept covered with dressings and a prophylactic course of antibacterial drug is administered. The wounds should be closed as soon as possible, under local anaesthesia if necessary.
Pain
This can be severe, particularly with comminuted and grossly displaced fractures, but can sometimes be less than anticipated. Morphine or its derivatives must not be given because they may mask the signs of increasing intracranial pressure or depress the patient with a compromised airway. Non-steroidal anti-inflammatory drugs (NSAIDs) may be prescribed to reduce both peripheral and intracranial pressure.
Temporary Immobilisation or Fixation
This has mainly fallen into disuse as early reduction and fixation is to be preferred. However, the use of a barrel bandage to support the comminuted mandible may be advocated. Careful consideration must be given to the effect this may have on the fragments, as an ill-applied bandage may increase the displacement. A bridle wire between teeth either side of the fracture line can be useful to stabilise a mobile fracture.
Supportive Treatment
This has been discussed in Chapters 2 and 4.
The management of maxillofacial injuries will now be considered.
Applied Anatomy
For describing injuries the face is divided into three parts. The lower third is the mandible and the soft tissues covering it. The middle third is bounded below by the occlusal line of the maxillary teeth and above by a line drawn through the pupils. The upper third lies above this.
The Mandible
The commonest sites of fracture in the mandible are the condyle neck, the angle and the canine region. The condyle may fracture through its thin neck, either within the capsule or below it, and may be bilateral as a result of blows to the chin, particularly if the mouth is open, or unilateral following blows to the body of the mandible on the opposite side. Fractures of the coronoid process are uncommon.
The angle of the mandible is a weak point because there is a change in the direction of the grain of the bone, which occurs where the vertical ascending ramus and horizontal body meet. Further, the shape of the mandible in cross-section changes as the thick lower border of the body becomes thin at the angle, so that the lower third molar sits in bone with little basal support lingually. Finally, the third molar, particularly if it is unerupted, may occupy up to two-thirds of the depth of the bone.
The body is the strongest part of the lower jaw but is weakened by the presence of the tooth sockets. The canine has a long broad root and its socket is a common site of fracture. The symphysis may also be involved as a result of blows on the chin. Alveolar fractures occur chiefly in the incisor region.
Displacement
Displacement depends on three factors: the force of the blow, gravity and the pull of the muscles inserted into the bone. The muscles concerned are the suprahyoid group attached to the lingual aspect of the anterior part of the mandible, which depress the lower jaw, and the muscles of mastication (masseter, temporalis and medial pterygoid) inserted into the ascending ramus, which elevate the mandible and move it laterally. The lateral pterygoid muscle, inserted into the condyle and meniscus of the temporomandibular joint, draws the condyle forward and therefore assists in opening the mouth.
Condylar Fractures
In these cases the lateral pterygoid muscle draws the fractured head forward medially and, in certain cases, over the eminentia articularis and out of the glenoid fossa to produce a fracture dislocation. The other muscles of mastication raise the ramus of the affected side to produce an anterior open bite between the incisors and canines on the opposite side. On opening the mouth the body of the mandible is displaced towards the affected side with marked deviation of the midline. In bilateral condylar fractures both ascending rami are drawn up and back equally so that gagging occurs on the posterior teeth causing an anterior open bite on both sides.
Fractures of the Angle or Body
In these the suprahyoid group of muscles depresses the anterior part of the mandible. Posteriorly the pull of the muscles of mastication attached to the ascending ramus draws it upwards. The posterior fragment is also drawn inwards as the pull of the medial pterygoid muscle is stronger than that of the masseter (Figure 14.1). Displacement is resisted by the periosteum, if it is intact, by the occlusion of the teeth and by the impaction of the fractured bone ends against each other. This last depends on the angle of the line of fracture which is said to be unfavourable if it would allow the posterior fragment to displace or favourable if it prevents it doing so.
Figure 14.1 Effects of muscle pull on mandibular fractures. Arrows indicate the direction of muscle pull. (a) Horizontal view of mandible showing horizontally favourable fracture (dotted line) and horizontally unfavourable fracture (continuous line); (b) vertical view showing vertically favourable (dotted line) and unfavourable (continuous line) fractures.
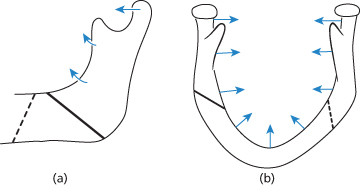
As displacement can take place in two planes, upwards and inwards, fractures are described as favourable or unfavourable when viewed from the side or horizontally, and from above or vertically. Thus a horizontally unfavourable fracture displaces upwards, a vertically unfavourable fracture inwards (Figure 14.1).
Where a bilateral fracture occurs in the anterior region through the canine sockets it is possible for the geniohyoid, genioglossus and mylohyoid muscles to displace the loose anterior portion downwards and backwards, with loss of control of the tongue, which may fall back into the pharynx and obstruct the airway.
Midline Fracture
In oblique fractures through the symphysis of the mandible, one half may be displaced lingually by the mylohyoid muscle to cause over-riding in the midline.
Age
In children, facial trauma more often involves the upper and mid third of the face as the relative size of the face is smaller (Figure 14.2a). With developing facial structure trauma is seen more evenly distributed and with an adult dentition the trauma seen fits the same pattern as adult patients regardless of chronological age. The mandible of a child is greatly weakened by the numerous crypts of the developing teeth, but the greater elasticity of the bone compensates for this (Figure 14.2b). In older patients the bones become more brittle and tend to break more easily and the mandible is weakened by resorption of the alveolar bone after the teeth are lost. The periosteum does, however, form a complete envelope round the edentulous mandible which, if not torn in the accident, holds the fractured ends in apposition. With advancing years the mandible becomes more dependent for its blood supply on the periosteum than on the inferior dental artery. For this reason methods of reduction or fixation that involve stripping of the periosteum must be avoided in the elderly. Classical plate fixation is compromised in these extremes of age.
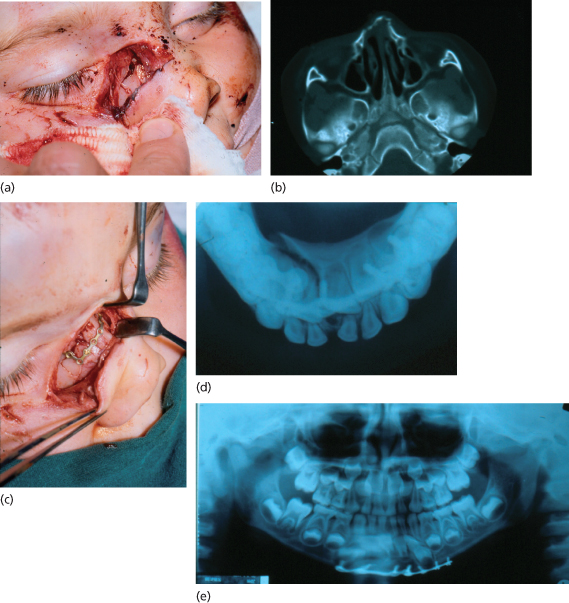
Figure 14.2 Trauma in children. (a) Nasal bone fracture in a 3-year-old child; (b) CT shows displacement; (c) ORIF via existing laceration to give good anatomical reduction of comminuted fragments; (d) displaced symphyseal fracture in a 6-year-old; lower occlusal radiograph giving clear view of fracture; (e) displaced symphyseal fracture in a 6-year-old; OPG shows ORIF applied at lower border via extraoral approach as very limited bone for classic sites of plate fixation due to developing dentition.
Middle Third of the Face
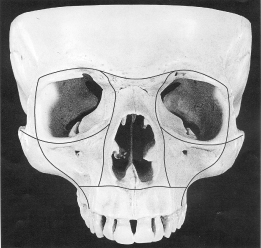
Fractures of the middle third of the face involve a complex of bones, which include the paired bones, the maxilla, palatine, zygomatic, nasal, lachrymal and inferior conchae, together with the single vomer and ethmoid bones. The structure of the maxillary complex consists of a grid system of buttresses (Figure 14.3). Strong vertical buttresses are formed by the frontal process of the maxilla, the zygomatic process of the maxilla and the zygomatic bone, and the pterygoid plates of the sphenoid with the tuberosity of the maxilla. Horizontal buttresses are formed by the supraorbital margin, the infraorbital margin and the palatine bones in continuity with the alveolar process. The spaces between are closed with thin bone plates, which enclose several large cavities, the maxillary air sinuses, the nasal cavity and the orbits. The vertical buttresses are more functionally challenged through the forces of mastication, particularly in the first permanent molar and canine regions, and the middle third is thus more resistant to upward forces but less to shearing stress from a horizontal blow.
Figure 14.3 Grid structure of face: these are the principal lines of reconstruction.
Fractures of the middle third of the face fall into six categories (Figure 14.4):
- alveolar
- Guérin’s/Le Fort I
- pyramidal/Le Fort II
- high transverse/Le Fort III
- naso-ethmoidal complex
- malar/zygomatic.
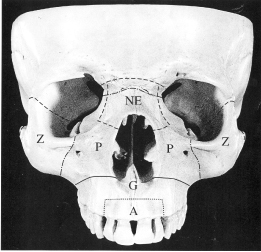
Figure 14.4 Fractures of the mid-third of the face: A – alveolar; G – Guérin’s (Le Fort I); P – pyramidal (Le Fort II); Z – zygomatic (malar); NE – naso-ethmoidal; Le Fort III is shown by the upper dotted line.
Alveolar fractures
Alveolar fractures occur in the tooth-bearing areas of the jaw.
Guérin’s/Le Fort I
These occur where the palate and alveolus are separated from the maxillary complex by a transverse fracture just above the floor of the nose and the antrum.
Pyramidal/Le Fort II
The fracture line passes through the lateral and anterior walls of the maxillary sinuses and continues up through the infraorbital margins to join across the bridge of the nose.
High Transverse/Le Fort III
The maxillary complex is virtually separated from the cranium by a fracture that traverses the lateral walls of both orbits and both orbital floors and crosses the midline at the root of the nose to involve the cribriform plate of the ethmoid.
The Nasal Bones and Naso-Ethmoidal Complex
This may be involved separately or in combination with other fractures.
The Malar Bone (Zygoma)
This can be fractured by a direct blow which may drive in the prominence of the cheek. The fracture line passes through the infraorbital margin, the anterior wall of the antrum, the malar buttress, the zygomatic arch and the frontal process of the zygoma.
It is important to understand that facial fractures rarely fall into such neat classifications. There is often a combination of injuries of the midface depending on the direction of the trauma. This can make exact classification difficult with fracture distribution being different on either side of the face. The clinical importance of this classification is that the Le Fort I involves only the alveolar process, the palate, nasal floor and maxillary antrum. The Le Fort II involves in addition the antrum, floor of the orbit and the nasal bones. The Le Fort III includes the structures affected by the Le Fort II and also the zygomas and anterior cranial fossa. It is emphasised that all Le Fort III fractures are head injuries and should be monitored as such. Further, as the anterior cranial fossa communicates with the nose through the fractured cribriform plate there is a grave danger of an ascending infection. The patient must be protected from a meningeal infection by the prescription of appropriate antibiotics. A cerebrospinal fluid (CSF) leak may require an intracranial dural repair by neurosurgeons, which may be effected at the same time as fracture fixation. Thus the management of such injuries calls for a team approach.
Displacement
In maxillary fractures the displacement is caused by the force of the blow and not by muscle pull as none of the muscles attached to the maxilla are strong enough to move the fragments. The most usual displacement is backwards and downwards, causing a typical concavity of the face (dish face) with anterior open bite due to gagging on the posterior teeth. This open bite is particularly marked in the Guérin’s type fracture.
Diagnosis
The oral surgeon should proceed to make a diagnosis in the usual way unless some urgent condition identified in the primary survey requires immediate attention.
History
In the unconscious patient the history may have to be taken from those who witnessed or attended the initial scene of trauma. The time of the accident is important in assessing the urgency of treatment, and the degree of infection in compound fractures. Soft tissue lacerations should be closed as soon as possible and certainly within 24 hours. The difficulty of reducing misplaced fractures increases as healing progresses. A history of any previous facial injury is important as old injuries can cause confusion in the diagnosis. The patient’s general condition and any tenderness or bruising of the head, chest or abdomen is noted. Shock is unusual in facial injuries and, unless the blood loss has been excessive, the cause should be sought elsewhere.
The patient should be asked if there was any loss of consciousness. In unconscious or confused patients, causes other than concussion, such as alcohol, recreational drugs, insulin or diabetic coma, or a cardiovascular catastrophe, should be considered. Any drug administered previously, especially sedatives, analgesics or antibacterials, should be recorded.
Examination
The surgeon must consider all the possible tissues that might be involved in the trauma – skin, connective tissue, blood vessels, nerves (both sensory and motor), muscles, underlying bones – together with special structures such as the eyes and salivary glands. The following signs of a fracture must be looked for. Swelling and bruising are usual at the point where the patient was struck, but may not coincide with the site of an indirect fracture. Deformity of the bone contour can be masked by swelling, but examination may reveal a break in the continuity of the bone or displacement. Intraorally, derangement of the occlusion may localise the fracture. Abnormal movement in the bone is diagnostic and when it occurs may be accompanied by pain and crepitus or grating as the rough bone ends rub against each other. Loss of function in the jaws is common as a result of trismus or pain.
The facial bones can be conveniently examined in the dental chair, but should the patient be too ill to get out of bed the headboard may be removed to allow the patient to be examined from above and behind.
Extraoral
The patient is first looked at full face for obvious signs of injury. Lacerations should not be probed or touched but are immediately covered with a dressing. Clots present in the nose and ears should not be disturbed but a discharge of CSF from these orifices is an important finding, indicating a fracture of the cranial base. To distinguish it from nasal secretion it should be tested for glucose, a constituent of CSF. CSF in contradistinction to blood does not clot and this can usefully differentiate them.
Facial Skeleton
The surgeon should then move behind the patient and, looking down from above, use the tips of their fingers to palpate and compare the right and left sides, and to determine points of tenderness or breaks in the continuity of the facial bones. This starts with the superior, lateral and inferior margins of the orbit and then proceeds to the bridge of the nose, where any deviation from the midline or depression is noted. The malar prominences are compared to detect loss of contour. Where there is marked oedema if may be very difficult to do this with certainty, but firm steady pressure on the swelling for a few moments will push it away and allow the bone to be felt.
The fingers then move over the zygomatic arch, to the temporomandibular joints. The patient is asked to open and close the mouth and perform lateral movements. The range of opening and of lateral movement is assessed. Fractures of the zygomatic arch may prevent opening as the coronoid process may jam against the displaced zygomatic process. In fractures of the condyle or ascending ramus there is little movement of the condyle head on the affected side or the mandible towards the opposite side. When the joint is difficult to palpate the little finger may be put into the external auditory meatus and the condyle felt through the anterior wall. Palpation is then continued to compare the ascending ramus, the angles and the lower border of the body of the mandible.
Eye
The surgeon then moves to face the patient and examines the eyes for damage, particularly depression, proptosis or a dif/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


