Chapter 14
Burning mouth syndrome: an update on diagnosis and treatment methods
14.1 Diagnosis of Burning Mouth Syndrome
Imagine the frustration of having a continuous painful disorder that cannot be definitively diagnosed with any known test or X-ray, interferes with eating, becomes progressively worse, has no known cause, and lacks any highly effective treatment. This is what patients with burning mouth syndrome (BMS) deal with every day of their lives.
Clinical Presentation
Burning mouth syndrome has various synonyms, such as stomatopyrosis, glossopyrosis, stomatodynia, glossodynia, sore mouth, sore tongue, and oral dysesthesia. These terms are used to emphasize the quality and or the location of pain in the oral cavity. The diagnostic criteria are as follows: (1) pain in the mouth is present daily and persists for most of the day; (2) oral mucosa is of normal appearance; and (3) local and systemic diseases have been excluded.1 The International Classification of Disease (version 9 [ICD-9]) has assigned the term glossodynia, which included the subterms glossopyrosis and painful tongue, a specific identity code number (ICD-9 #529.6).2
Onset and Pattern
Burning mouth syndrome typically has a spontaneous onset, although its intensity will increase gradually over time. The International Association for the Study of Pain has identified BMS as a distinctive named entity characterized by oral burning pain episodes lasting at least 4–6 months.3 There is no published data on the natural life history of burning mouth syndrome. While many speculate that, over time, this disorder fades in intensity, data is lacking.
Character
It is characterized by sensory symptoms, both positive (burning pain, dysgeusia, dysesthesia) and negative (loss of taste, paraesthesia).
Location
The primary locations for these symptoms are the lips and tongue (mainly the tip and anterior two-thirds). BMS patients also complain of sensory discomfort in the hard palate and alveolar ridges. Conversely, the buccal mucosa and floor of the mouth are almost never involved.4 At least for the tongue, the anatomic distribution of the burning pain in BMS patients corresponds, to a great degree, to where tastebud density is greatest in the mouth. With regard to the issue of location, one study examined tastebud density on the tongue and found that tastebud density was 4.6 times higher on the tip than the midtongue region.5 In the anterior hard palate or alveolar ridges this association between tastebuds and BMS is not absolutely tied to tastebud density because tastebuds are not commonly located on the inner lip mucosa. Nevertheless, most BMS patients report a persistently diminished taste or altered (metallic) taste sensations. Acidic foods such as tomatoes and orange juice cause considerable distress with an increase in burning sensations. These descriptions vary but often include a stinging or burning sensation as if the patient’s mucosa has been scalded.
Diagnostic Tests
Most of the common laboratory tests suggested for BMS patients, which we present in table form (see Sec. 14.6, Table 14.2), will turn out to be negative.6 In fact, the International Classification of Headache Disorders classifies burning mouth syndrome as an intraoral burning sensation for which no medical or dental cause can be found.
14.2 Are There Subpopulations of Burning Mouth Syndrome?
The population of patients that have burning mouth syndrome tend to be female patients over the age of 50 and there are more oral disease and dysfunction problems in this age population than in a younger group of patients (e.g., hyposalivation, lichen planus, autoimmune diseases). A recent paper suggested that a subpopulation of BMS cases presents with a common triad of symptoms including (1) idiopathic sensorial disturbance of burning mouth, (2) taste disturbance (dysgeusia), and (3) dry mouth.7 Another paper suggested three subgroups with BMS type 1 being characterized by burning pain increasing throughout the day and reaching its peak in the evening; BMS type 2 was characterized by complaints of continuous sensory disturbances; and BMS type 3 had intermittent symptoms with pain-free periods during the day. 8 The most pragmatic method of grouping BMS is by dividing patients into the primary BMS sufferers (no other evident disease) and secondary BMS sufferers (oral burning from other clinical abnormalities). In fact, using this last classification scheme, one paper examined 69 BMS patients (83% female) and asked them to fill out both the Multidimensional Pain Inventory and Symptom Checklist 90–Revised.9 The study found that the primary BMS patients and the secondary BMS patients showed no differences with respect to age, pain duration, pain intensity, or levels of psychologic distress. There was one substantial difference: If the associated clinical abnormality was treatable, then the burning sensations would improve in the secondary BMS group, but the primary BMS group did not demonstrate remarkable symptom cessation with treatment.
14.3 Epidemiology
Burning mouth symptoms are reported in up to 4% of adults; this percentage increases with age, becoming more prevalent in the fifth to seventh decades. One study surveyed 669 men and 758 women randomly selected from 48,500 individuals ages 20–69. Researchers reported that 53 individuals (3.7%) exhibited BMS (11 men, or 1.6%; 42 women, or 5.5%).10 The presence of BMS was found to be very uncommon before the age of 30 years (40 years for men) and the onset in women usually occurs within 3–12 years after menopause and is higher in women who have more systemic disease.11 Another epidemiologic study surveyed US adults and estimated the overall prevalence of burning mouth to be 0.7% of the adults up to age 65.12 This study was repeated on a subset of over 5800 individuals 65 and older in South Florida.13 Researchers report a prevalence of 1.7% for burning mouth pain in this elderly group. Clearly, the differences in these prevalence figures are related to sampling bias in surveyed populations and disease definition being used.
14.4 Quantitative Sensory Testing in Burning Mouth Syndrome
The frequent occurrence of numbness, pain, dysgeusia, and dysesthesia in BMS has prompted researchers to perform a quantitative assessment of the sensory and chemosensory functions in these patients.
14.4.A Neurosensory Threshold Testing
Until recently, researchers have not consistently found a statistically significant alteration in the sensory perception (touch and temperature) of BMS patients. For example, one study carefully examined 20 BMS patients versus 20 controls for different abilities to perceive different shapes of objects with their tongues.14 No systematic disparity was evident in the two groups regarding object size perception ability. Of course, detecting the shape of objects with your tongue is not the only test of sensory acuity; several years ago researchers used argon laser stimulation to examine 23 BMS subjects versus 23 age-matched controls for differences in their sensory and pain thresholds.15 This study used brief laser stimulation to six test sites (tongue tip, lower lip mucosa and skin, buccal mucosa, anterior hard palate, and dorsum of the hand). The study reported the sensory thresholds were significantly higher and the ratios between pain and sensory thresholds significantly lower in patients with BMS at all tested sites. The resulting widespread sensory threshold differences seen in this study argues for a centrally mediated sensory amplification abnormality.
14.4.B Blink Reflex Testing
Another study used an objective electrophysiological examination of the trigeminal–facial nerve system using the blink reflex response in 11 BMS subjects and 10 controls.16 Researchers reported BMS patients have clear-cut alterations in their blink response to applied stimulation. Finally, a study examined evoked brainwave potentials after lingual nerve stimulation in 22 BMS patients with pain, 10 BMS patients with reported numbness, and 6 controls. 17 The study found that pain thresholds were significantly lower and evoked potential response latencies were significantly different (shorter) in the BMS with pain group. The latencies in the BMS with numbness were significantly longer. Overall these sensory data suggest that peripheral and/or central nervous system changes are clearly present in BMS but the data do not pinpoint where within the somatosensory system the responsible underlying changes are to be found.
14.4.C Taste Threshold Changes and Burning Mouth Syndrome
Dysgeusia is a term used to describe a distorted gustatory perception or persistent gustatory sensation in the absence of gustatory stimulants.18 As mentioned earlier, BMS patients frequently report a positive taste sensation which they describe as a persistently altered (metallic) taste. They also have a diminished ability to detect bitter flavors, and spicy and acidic foods increase their burning sensations. One recent study examined 50 patients with BMS (study group) and 50 healthy subjects (control group) and analyzed their ability to taste three flavors (bitter, acidic, and spicy substances).19 This study found that taste sensations were normal in all controls but 30 of the BMS patients had a diminished response to bitter taste. The use of a spicy substance (pepper sauce) applied to the tongue produced a strong burning sensation on the tongue in 28 patients of the BMS group but the same response was seen in only 10 of the controls. Another study examined 180 subjects with complaints of BMS, xerostomia, and taste disturbances versus 90 age- and gender-matched healthy controls.20 This study also reported that the BMS patient group had clear-cut taste acuity differences compared with the controls, with more of the BMS patients reporting sweet abnormality than with the other three taste substances (salt, bitter, and sour). Another study examined taste acuity in 73 BMS patients (57 women and 16 men) and 52 control subjects (38 women and 14 men) who were age and gender matched to the BMS group.21 Researchers used various concentrations of sweet, salty, sour, and bitter solutions and asked subjects to rate the intensity and quality of each solution. The study found that the 57 women in the BMS group gave lower-intensity ratings for salty and sweet test solutions than the 38 women controls. For the women in this study, there were no group differences on sour or bitter test solutions, and for the men in this study, there were no group differences on any of the substances tested.
14.4.D Special Case of Metallic Dysgeusia
Because metallic dysgeusia is a common early symptom of a BMS disorder, it would be appropriate to review a 2004 article that describes medication-induced dysgeusia.22 This paper reports that the medications most commonly linked to metallic dysgeusia are those used to treat bacterial infections, psychosis, arthritis, and hypertension. The study found case reports for metallic dysgeusia linked with tetracycline,23 lithium carbonate,24,25 D-penicillamine,26 and captopril. A 1985 paper described a link between metallic dysgeusia and Crohn’s disease that is manifesting oral effects as well as the usual intestinal changes.27 In summary, metallic dysgeusia is not well understood, but in the absence of medications or brain disease causing it, the possibility remains that it may be related to damaged peripheral nerves, especially considering the information already presented about small sensory fiber neuropathic changes in the tongue. The hypothesis that pain and taste pathways are both affected and interact is reasonable and certainly worthy of further testing, especially if an animal model could be developed.
14.4.E Chorda Tympani, Taste, and Burning Mouth Syndrome
There are patients who complain of numbness of the tongue after an otologic procedure, probably related to surgical damage of the chorda tympani nerve during the procedure. Examining this issue, a 2006 study assessed tongue sensations in 15 patients before and twice after undergoing middle ear surgery and in 18 nonsurgical controls.28 The authors reported that 47% of the surgery patients complained of numbness or tingling of the tongue shortly after surgery, with a significant reduction in sensitivities to light touch and two-point discrimination on the operated side. This sensory deficit returned to baseline levels on subsequent evaluations and no patient in this study developed burning mouth syndrome. The main difference between subjects in this study and those in the burning mouth patient population was age: the study subjects were substantially younger. Another 2007 study found similar results. They reported on changes of trigeminal sensitivity of the tongue after middle ear surgery.29 The authors concluded that pain-related sensitivity of the ipsilateral tongue side decreases after the mentioned surgery, suggesting that the chorda tympani nerve function influences both gustatory sensibility and intraoral trigeminal sensitivity, but again no increased pain or burning sensation resulted in this population.
14.5 Other Local Oral Factors and Burning Mouth Syndrome
Many local and systemic precipitating factors have been suggested beyond the salivary changes and sensory dysfunction changes described previously. The local factors included other diseases that may be causing burning sensations such as oral candidal infections, autoimmune mucosal reactions such as lichen planus, geographic tongue, atrophic tongue (Fig. 14.1), and tissue trauma from ill-fitting dentures.
Figure 14.1 Bald or atrophic tongue (left) and geographic tongue (right).
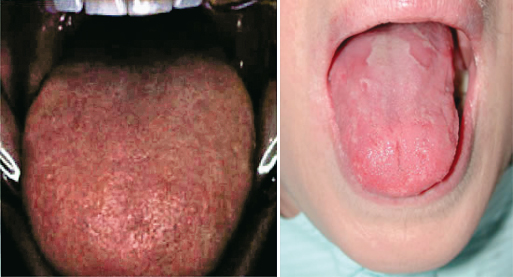
Of course there are always case reports of burning type pains occurring from oral carcinomas that invade the trigeminal nerve and from a variety of local oral mucosal tissue irritants.30 These local oral conditions have been seen often enough to suggest that some cases of BMS are secondary BMS cases.31 More than one-third of all BMS patients presenting for diagnosis are estimated to have multiple causes; the most common causes of secondary BMS are listed in Table 14.1.
Table 14.1 Primary and secondary burning mouth syndrome
| Presumed etiology | Clinical presentation |
| Primary BMS treatment | |
| Nerve atrophy | Focal neuropathic pain involving small-fiber atrophy of the oral tissues. |
| Secondary BMS treatment | |
| Dry mouth (xerostomia) | Several medications cause decreased salivary flow (tricyclic antidepressants, central nervous system depressants, lithium, diuretics, and medications used to treat high blood pressure). It can also occur with aging or Sjögren’s syndrome. |
| Oral infection | Yeast infections (thrush) have been seen in BMS patients and may be related to immune dysfunction (e.g., HIV infection), uncontrolled diabetes, poorly maintained or cleaned dentures, and certain immunosuppressive medications. |
| Autoimmune mucosal prescriptions | Lichen planus and geographic tongue are conditions that are usually painless, but sometimes cause a stomatitis and a sore, patchy tongue. |
| Nutritional deficiencies | Being deficient in nutrients, such as iron, zinc, folate (vitamin B9), thiamin (vitamin B1), riboflavin (vitamin B2), pyridoxine (vitamin B6), and cobalamin (vitamin B12), may affect oral tissues and cause a burning mouth. These deficiencies can also lead to vitamin-deficiency anemia and oral stomatitis. |
| Allergies | The mouth burning may be due to allergies or reactions to foods, food flavorings (especially cinnamon), other food additives, fragrances, dyes, or other substances. Similarly, direct chemical irritation and allergic reactions to dental materials may be a factor in BMS. |
| Reflux of stomach acid | The sour- or bitter-tasting fluid that enters the mouth from the upper gastrointestinal tract may cause irritation and pain. |
| Certain medications | ACE inhibitors, used to treat high blood pressure, may cause side effects that include a burning mouth. |
| Endocrine disorders | Endocrine disorders such as diabetes and underactive or overactive thyroid are known to produce peripheral neuropathic pain and generalized hyperalgesia. |
ACE, Angiotensin-converting enzyme; BMS, burning mouth syndrome; HIV, human immunodeficiency virus.
14.6 Other Common Co-Morbid Systemic Diseases
Various systemic conditions have been associated with BMS, including diabetes, hormonal changes, and nutritional or mineral deficiencies. The condition of BMS is more prominent in female patients over 40.32 The causal relationship between hormonal changes in women that occur with menopause and BMS is unclear. One study examined the effect of hormonal replacement therapy (HRT) on BMS. The researchers found that HRT helped in 15 of 27 of their postmenopausal women with BMS.33 Unfortunately, this study was an open-label study and not a randomized blinded placebo-controlled study and thus the data are not convincing proof of a causal link between hormone alterations and BMS. Patients with BMS often have high blood glucose levels, but this does not occur on a consistent basis so no causal relationship has been demonstrated.34 Next, nutritional deficiency (vitamins B1, B2, B6, and B12, iron, folic acid, zinc, etc.) is yet another reported systemic abnormality associated with BMS. Like hormonal status and diabetes, these suggested nutritional deficiencies are not consistently supported by the literature. Nevertheless, local and systemic factors must be ruled out before a final diagnosis of BMS is made. Femiano’s group (2008) proposed that the study of thyroid function tests and echography be inserted in the diagnostic process for BMS patients. The study reveals that individuals with thyroid alterations are often considered to be BMS patients and that hypothyroidism could be responsible for oral burning and/or dysgeusia in some supertaster subjects. Their protocol allows researchers to easily distinguish patients with true BMS from those who present burning mouth as a result of hypothyroidism.35 The common diagnostic tests used for BMS are listed in Table 14.2.
Table 14.2 Diagnostic tests used as part of the diagnostic process for burning mouth syndrome
| Complete blood cell count (CBC) | This common blood test provides a count of each type of blood cell in a given volume of blood. The CBC measures the amount of hemoglobin, the percentage of blood that is composed of red blood cells (hematocrit), the number and kinds of white blood cells, and the number of platelets. This blood test may reveal a wide variety of conditions, including infections and anemia, which can indicate nutritional deficiencies. |
| Other blood tests | Because nutritional deficiencies are one cause of a burning mouth, running a test on the blood levels of iron, zinc, folate (vitamin B9), thiamin (vitamin B1), riboflavin (vitamin B2), pyridoxine (vitamin B6), and cobalamin (vitamin B12) is important. Also, because diabetes causes neuropathic pain, a check may be done of the fasting blood sugar level. |
| Allergy tests | While it is not common, occasionally, testing to see if the patient may be allergic to certain foods, additives, or even substances in dentures can be ordered through an allergist. |
| Oral swab culture or cytologic smear | If a fungal infection is suspected, a small tissue sample (biopsy) or an oral swab of the mouth for culture and examination may be ordered. |
| Tongue tissue biopsy | With the recent suggestion that small nerve fibers are depleted in the affected area, some special tests may be ordered when a biopsy is taken. |
14.7 Psychological Factors
Anxiety is prominent feature of BMS patients and many speculate that the pain disorder itself causes increase anxiety over time. Various other psychological disorders, including depression and somatization, are also commonplace features in a BMS patient population, but the presence of co-morbid psychological disease is not evidence of causality.36 Because BMS patients are generally older, the question is, “Are psychological disorders in higher prevalence in BMS patients compared with an age-matched control group?” One study examined 25 patients with a diagnosis of primary BMS and 25 age- and gender-matched patients with organically based painful disorders of the mouth; the authors reported a positive psychiatric diagnosis in 44% (11/25) of the BMS patients but in only 16% (4/25) of the non-BMS patients. This study involved an interview by a psychiatrist and a questionnaire that screened for psychiatric disorders. While 44% seems a high number, when compared with other chronic pain patients this rate is not unusual or even high. For example, the same 28-item psychiatric screening questionnaire (general health questionnaire [GHQ-28]) used in the prior study was given to 31 primary BMS subjects. These authors found that although 51.9% of the patients showed evidence of psychiatric illness using the GHQ-28 questionnaire, this rate was similar to or lower than what has been reported for other chronic pain subjects, except those attending a psychiatric clinic.37 One study examined 74 BMS patients using a psychiatric interview plus the Hamilton’s Depression and Anxiety Scales (HADS).38 This study reported that a positive psychiatric diagnosis (mostly depression) was established in 38 of the 74 cases (51.4%). The HADS questionnaire data suggested that, when anxiety was present, it strongly influenced the psychiatric condition of these patients. An elevated rate of positive findings when a systematic psychometric analysis of BMS patients is performed was confirmed again in a more recent study that examined 32 BMS patients and 32 matched control subjects using a comprehensive, reliable, and validated inventory.39 Like the studies cited previously, their results showed highly significant differences between the BMS group and the non-BMS controls with regard to several personality factors. Unfortunately, high levels of anxiety, depression or even somatization tendencies are not unusual or unique to BMS patients. Chronic disease patients in general have elevated findings when compared with age- and gender-matched nonpain patients. The question remains whether the BMS pain is etiologically related to these personality characteristics or vice-versa. A report on 33 BMS patients suggested that psychological factors are not consistently elevated over control subjects in this population.40 These authors used the revised Symptom/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


