12
12
Rhinoplasty Surgery
Introduction
Rhinoplasty surgery forms a vital part of the functional and aesthetic management of congenital or traumatic deformities of the facial skeleton. This chapter will cover important aspects of
- nasal anatomy,
- assessment of the deformity,
- surgical planning, and
- operative procedures.
It is essential that the reader refers to a comprehensive or specialist texts for detailed aspects of the surgery.
The nose is a complex structure cantilevered on the mid face. Its complex role embraces the senses of smell and taste, respiration, aesthetics and sex and so rhinoplasty surgery requires careful consideration. All mid face orthognathic surgery will affect the nose to a degree. LeFort I operation impactions broaden the alar width, and with inadequate trimming of the nasal septum they will lead to septal buckling and obstruction or deviation of the nasal tip. Advancements will raise the nasal tip and straighten out profile curvatures. For these reasons it is undesirable to do a rhinoplasty before, during or within 6 months of a mid face osteotomy.
Anatomy
It is important to understand the complex nasal anatomy which is made difficult by the nomenclature. The upper border of many structures is designated cephalic (headwise) and the lower border caudal (tailwise). The anterior surface of the nose is dorsal and posterior structures are posterior. Unfotunately some terms have been introduced in relation to the supine anaesthetised patient, so that what might be considered as anterior and posterior nasal sites are described as “high” and “low”.
Figures 12.1 and 12.2 show the anatomical subunits of the nose, which is conveniently divided in thirds. The upper third consists of the bony pyramid, made up of the nasal bones with their articulation to the ascending processes of the maxilla and the bony septum. The paired upper lateral cartilages insert just under the caudal (lower) end of the nasal bones and their fusion with the midline cartilaginous septum in a “T” type configuration forms the middle third (“vault”) (Figure 12.2). The attachment of the caudal aspect of the upper lateral Cephalic cartilage to the cephalic (upper) aspect of lower lateral cartilages forms the boundary to the lower third of the nose and is referred to as the scroll attachment. The paired lower laterals, sometimes called the alar cartilages, form the a prominent part of the lateral surface of many noses and the nasal tip, They are divided into the lateral, intermediate and medial crurae — or processes (Figures 12.3a and 12.3b). The intermediate crurae form the “domes” and are the tip defining points of the nose.
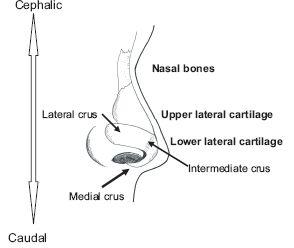
Figure 12.1 External anatomy of nose (lateral view).
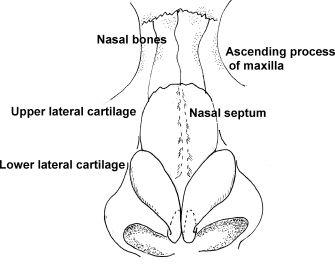
Figure 12.2 External anatomy of nose (frontal view).
The medial crura curve medially and backwards and their terminal processes, the so-called footplates abut against the border of the caudal aspect of the nasal septum and form the cartilaginous columella.
The columella with its cartilage and skin provide the external (caudal) border of the septum from the tip to the nasolabial angle. The outer margin of the nares are the soft tissue alar lobules that are devoid of cartilage.
The overlying superficial musculoaponeurotic system (SMAS) of the nose is a complex layer which provides a rich vascular supply covering to the underlying skeleton and is derived from the superior labial and facial arteries and corresponding venous and lymphatic vessels accompanying these. Its intrinsic aponeurotic muscles have elevator, depressor, compressor and dilator functions which contribute to olfaction and facial expression.
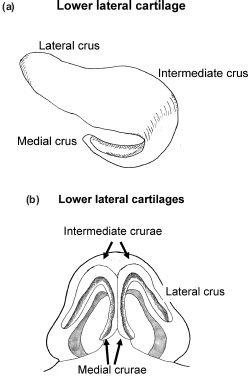
Figure 12.3 (a) and (b) Lower lateral cartilage anatomy.
The external anatomy of the nose is readily studied in any crowded place.
Assessment
History
A detailed history covering the functional and aesthetic aspects of the nose is mandatory.
To assess function, the patient is asked specifically regarding the presence and duration of nasal obstruction, sinus disease and allergic type symptoms. It is important to document prior medical and surgical treatments and their efficacy in treating any functional or aesthetic complaints.
A detailed history of traumatic injuries to the nose and surrounding facial skeleton is essential especially if operated on, and an indication of the pretraumatic appearance of the nose is helpful. It is particularly important to gauge the patient’s specific concerns about the appearance of each subsection of the nose with direct questioning. A generalised vague reference to a dislike of the overall look of the nose or any suggestion that the surgeon should decide where the problems lie is to be discouraged and may be suggestive of a dysmorphic disorder (see Chapter 6). The patient’s thoughts about the overall improvement desired are sought and realistic expectations estimated. A general medical history should screen the patient for bleeding disorders, cardiovascular and respiratory disease and importantly a psychiatric history.
Examination
A detailed examination of the internal and external aspects of the nose is performed. Anterior rhinoscopy to detail mucosal, caudal septal and turbinate deformities is supplemented with an endoscopic evaluation of the posterior nasal cavity and middle meatal areas to exclude infective or obstructive sinonasal disease. The internal nasal valve area which is bounded by the upper lateral cartilage, inferior turbinate, nasal septum and nasal floor is specifically examined and any high septal deformity noted. This is the narrowest part of the nasal airway and significant internal nasal valve collapse can be demonstrated by Cottle’s test (Figure 12.4) in which the airway improves when the cheek adjacent to the mid third of the nose, i.e. the upper lateral cartilage is pulled laterally.
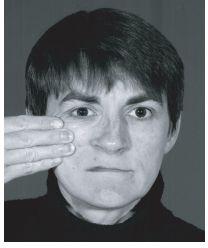
Figure 12.4 Demonstration of Cottle’s test.
The importance of the balance of the nose to other aspects of the face is important. Assessment of this relationship should form the initial part of the external examination process. The patient’s ethnic characteristics must also be considered. Facial and nasal asymmetries are documented and detailed to the patient.
The skin-soft tissue envelope is important and is critical in predicting postoperative changes. Thinner skin may show minor postoperative irregularities whilst very thick skin can hide any corrections made.
An initial evaluation of the underlying skeletal aspects of the nose considers three fundamental parameters: length (nasion to tip), projection of the dorsum and rotation of the nasal tip. Detailed examination should then document deformities in relation to these factors.
External deformity is most easily assessed and documented in nasal thirds. The frontal, lateral, oblique and basal views (Figures 12.5a–12.5g) are all separately visualised.
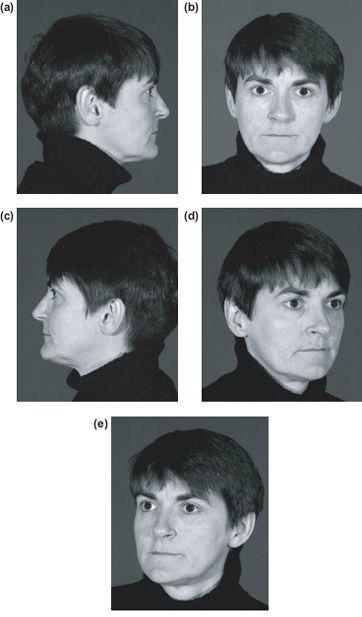
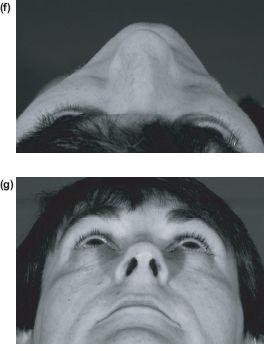
Figure 12.5 (a)–(g) Standard photography views.
- The upper bony pyramid is examined for deviation, irregularity and the extent of any dorsal hump. The width of the base of the dorsal pyramid is determined and the dorsum palpated to ensure there is no “open roof” type deformity.
- Similar deformities are sought in the mid third of the nose which is cartilaginous. In this area, an assessment of any externally visible collapse in the nasal valve area is made by inspection and Cottle’s test.
- The lower third nasal tip region, which is made up of the lower lateral cartilages is assessed for asymmetry, bulbosity, projection and rotation. A judgement regarding the width of the alar base in relation to the facial proportions is made. The alar width should match the normal intercanthal distance.
Documentation
Documentation of all aspects of the examination is critical for clinical and medicolegal purposes. A rhinoplasty assessment form can be very useful in this regard. It ensures all the areas of the evaluation are considered methodically and can be used for standardising the assessment for all patients.
The patient’s expectations and all discussion points are clearly noted. A surgical plan is formulated to correct the specific deformities. It is essential to ensure the patient is given realistic expectations for the outcome of intended surgery, and limitations together with potential complications are discussed. It is very important to ensure that improvement is indeed likely and a risk benefit profile needs to be detailed to the patient prior to obtaining consent and carefully noted.
The surgical approach, be it endonasal or external, should be discussed with the patient and incisions outlined and documented.
Photography and Computer Imaging
Preoperative photography is an absolute requirement for analysis and medicolegal purposes. Standard view photographs form a useful way of communicating deformities and potential changes to the patient. They assist in operative planning and are invaluable for reference during surgery. In combination with postoperative images, they allow self- and peer-reviewed assessment of results.
Standardisation is critical both from the views taken and lighting and background conditions. Digital SLR photography has now largely taken over from 35 mm film and the new technology lends itself well to computer archiving and digital imaging. A standard neutral background such a pale grey, or green or blue is used and ideally a soft exposure is achieved using a flash unit and umbrellas placed equidistant from the patient and camera. The camera should be two metres from the subject and an appropriate zoom used to compose the image using the portrait outline. An overhead lamp, a “kicker” above the patients head can help eliminate unwanted shadows (Figure 12.6).
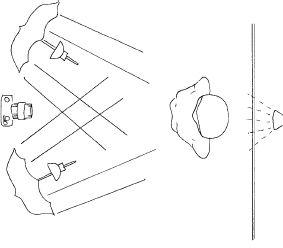
Figure 12.6 Photography setup.
The standard views are as follows (Figures 12.5a–12.5g):
- Straight frontal view. The patient looks directly into the camera with the eyeline in a horizontal plane.
- Lateral view. The patients Frankfort plane should be horizontal. This view assesses dorsal profile and is critical in assessing the three basic parameters of length, projection and rotation of the nose. The nose-chin relationship is also clearly demonstrated. A separate lateral view with the patient smiling may outline dynamic movement in the nasal tip.
- Oblique views. These views are at taken at 45 degrees to the frontal views and can outline asymmetries and contours.
- Basal view. This view is taken looking up the nose and focuses on the nasal tip detailing asymmetry and deformity.
- “Birds eye” view. This view is taken from the top of the patient looking down the nose. It can be useful in showing the subtleties of deviation of the nose.
Digital imaging has evolved greatly over the past few years and simple morphing is possible with inexpensive photo-imaging software. More complex programmes are, readily available with or without archiving capability and have purpose made user interfaces and more advanced digital manipulation of the images. With rhinoplasty surgery, they can be very useful in showing patients potential changes and postoperative outcomes. This is most useful in detailing profile changes in the lateral view but with some experience frontal views can be morphed to show potential width reduction and refinement in the nasal tip. Dedicated programmes have measurement abilities and so can be extremely helpful in operative planning. It is important not to convey unrealistic changes to the patient — this will be a source of dissatisfaction afterwards. As a rule a slight underestimation of the postoperative result is generally favourable. Most surgeons choose not to give printed images to the patient of the predicted changes but if you do so, a printed waiver should make clear that the image is only an indication of the likely result.
Surgical Approaches
As a general rule, it is best to limit surgical tissue dissection to a minimum to reduce the risk of vascular compromise of the skin-soft tissue envelope. In this way, additional scarring is prevented and healing is more predictable. Limited dissection also makes it easier to judge the underlying structural components and position of placed underlying grafts.
There are two basic approaches to the nasal skeleton:
i) the endonasal or closed approach and
ii) the external or open approach.
The advantages and disadvantages of each are much debated and many authors advocate one method to the exclusion of the other. Each offers benefits in specific situations and should be within the repertoire of a rhinoplasty surgeon.
The least traumatic method of dissection to achieve the specific goal should be used and as such the endonasal approach is favoured for all simple cases unless a better result using the open technique.
Endonasal Approach
The endonasal approach only requires incisions within the nose with no visible external scars (Figures 12.8–12.10). Minimal soft tissue dissection is needed, making this method favourable for less marked deformities and is ideal for correcting bony dorsal irregularities. Its benefits lie in the limited soft tissue disruption allowing early and predictable healing due to the comparatively reduced scar tissue formation. Its main limitations are the restricted exposure of the underlying nasal skeletal elements. The endonasal approach can further be divided into delivery and non-delivery approaches dependent on whether the lower lateral cartilages are fully delivered. With delivery the cartilage is exposed and withdrawn from its overlying subcutaneous layer. The incisions required for these are detailed later.
External Approach
The external approach requires a mid-columellar skin incision which is joined to bilateral marginal incisions (Figure 12.11). More soft tissue dissection is required but provides an unparalleled view of the nasal structures, facilitating diagnosis and correction by bimanual tissue handling. Other benefits include binocular vision for the surgeon, control of bleeding with diathermy, precise placement and suturing of struts, battens, shield and spreader grafts. This approach also offers a definite teaching advantage although this should not be thought of as an indication for its use. The external approach is favoured for most major reconstructive rhinoplasty and revision surgery, particularly where the nasal tip needs addressing. Recent incision refinements and surgical technique have overcome some of the earlier criticisms of a columellar scar, delay in resolution of the supratip skin oedema, loss of tip projection and extra operating time. However with this approach, it may be difficult to assess the supra-tip area and the desired tip projection due to the lack of traction of the soft tissue prior to closure of the columella incision. Specific indications for the external approach in rhinoplasty include:
- congenital deformities such as the “cleft lip nose”,
- extensive revision surgery,
- severe nasal trauma,
- the markedly deviated nose,
- marked tip deformities, and
- situations where assessment of the exact pathology is difficult.
Extended applications of the external approach enable greater exploitation of the nasal skeleton and the advantages this affords. It has been advocated for nasoseptal perforation repair, access to the nasal dorsum for treatment of nasal dermoids and even as an approach to hypophysectomy.
Operative Techniques
Anaesthesia
Rhinoplasty surgery is usually performed under general anaesthesia although local anaesthetic and sedation are also possible. The face is prepared with an aqueous detergent and draped to reveal the eyes, the corneas are simply protected with lacrilube ointment. The intranasal mucosal cavity is prepared preoperatively with a (10%) cocaine vasoconstrictor solution. Local anaesthesia with a vasoconstrictor is then injected to further minimise intraoperative bleeding. A dental syringe and needle are used with a 2% lidocaine and 1:80,000 adrenaline cartridge. The injection sites are as follows (Figures 12.7a–12.7d):
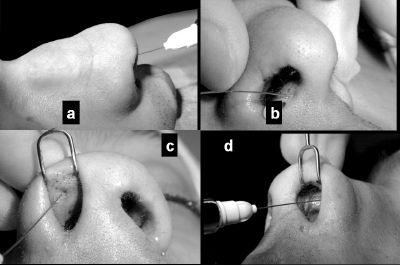
Figure 12.7 (a)-(d) Local infiltration technique for rhinoplasty.
a) along lateral wall of nose through intercartilaginous area,
b) base of the columella and collumellar region if the external approach is used,
c) vestibular and non-vestibular aspects of the lower lateral cartilages (the alar cartilages),
d) caudal septal cartilage area, and
e) alar bases if reduction planned (not shown).
Injection over the immediate dorsum is best avoided as the resultant swelling can make assessment of this area difficult. Lateral nose depot injections can be massaged upwards into the dorsal area to reduce bleeding when the skin-soft tissue envelope is being elevated. Leaving adequate time for the anaesthesia to take effect is critical in exploiting its haemostatic advantage.
Incisions
Elevation of the skin and soft tissue envelope is facilitated by various incisions.
1. Intercartilaginous
The intercartilaginous incision (Figures 12.8a–12.8c) is the most commonly used in endonasal rhinoplasty. It allows direct access to the mid and upper thirds of the nose but affords no exposure of the tip cartilages. It is often used in combination with other incisions if tip surgery needs to be performed.
The incision is made in the area separating the upper and lower lateral cartilages. A small linear hollow is seen intranasally demarcating the area between the caudal border of the upper lateral and the cephalic border of the lower lateral cartilages. It is usually seen and easily palpable when the alar margin is retracted upwards and everted using a two-pronged skin hook (Figure 12.8a).
- An incision is made into this hollow laterally (Figure 12.8b) and the blade is then turned forwards and medially along the intercartilaginous junction and onto the caudal septum to make a transfixion incision below the caudal cartilaginous septum, i.e. the incision passes through the membranous septum between the medial crura and the caudal septum.
- It is important to ensure this transfixion incision does not extend more than half way along the columella as further extension risks dividing the medial crural attachment to the caudal septum. This is one of the major tip support mechanisms, and division may result in postoperative tip ptosis. Conversely, an extended full transfixion incision can be utilised as a manoeuvre for deprojection of the tip if required.
- With retraction of the lower lateral cartilage, the overlying skin-soft tissue envelope can be gently elevated off the cartilaginous dorsum of the upper lateral cartilages by sharp dissection upwards using a sawing motion with a No. 15 blade in a supraperichondral plane (Figure 12.8c).
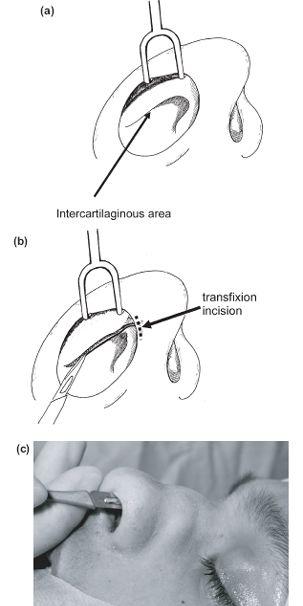
Figure 12.8 (a)-(c) Intercartilaginous incision technique.
- After the cartilaginous vault is freed of overlying tissue, an incision is made into the caudal end of the periosteum of the nasal bony pyramid.
- The periosteum and its overlying procerus muscle can then be elevated using the side of a Joseph elevator. Such elevation needs extend only far enough laterally to gain access to a dorsal hump.
- The intercartilaginous incision approach does not expose the lower later/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


