11
Radiographic Analysis of Periodontal and Endodontic Lesions
Introduction
The periodontium is a group of tissues that are involved with the support of the tooth. The tissues are the gingiva, alveolar mucosa, cementum, periodontal ligament, and alveolar and supporting bone (American Academy of Periodontology, 2001). The periodontal ligament space, alveolar bone, and supporting bone are visible radiographically. Radiographs provide important information and are an essential component of a comprehensive periodontal examination.
Normal Anatomy of Alveolar Process and Periodontal Ligament
Lamina Dura
The alveolar process is the bone that houses the tooth and is connected to the basal jaw bone. The alveolar process is composed of the outer cortical plate, the spongiosa which is trabecular or cancellous bone, and an inner cortical plate that faces the tooth which is known as the alveolar bone.
The alveolar bone is identified as the lamina dura radiographically. The lamina dura is a thin well-defined radiopaque line that is continuous around each tooth (Figure 11.1). The appearance of the lamina dura may vary where it may be diffuse or absent. This may be due to the X-ray beam being directed more obliquely or due to superimpositions of various structures. Teeth subjected to heavier occlusal forces may have a wider and denser lamina dura (White and Pharoah, 2009).
Figure 11.1 Normal radiographic bone level with intact lamina dura.
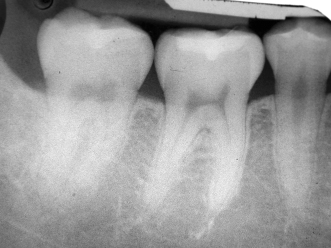
Alveolar Crest
The alveolar crest is formed where the outer cortical bone meets the alveolar bone. For the first three phases of passive eruption, a histologic study of clinically normal human jaws reported the distance from cementoenamel junction to the alveolar crest ranged (Gargiulo et al., 1961):
- Phase I: 0.04 mm to 3.36 mm (average = 1.08 mm)
- Phase II: 0.35 mm to 5.00 mm (average = 1.55 mm)
- Phase III: 0.88 mm to 3.20 mm (average = 1.71 mm)
Some studies have defined the presence of periodontitis if the distance was ≥1 mm while other studies had a threshold of ≥2 mm or ≥3 mm. Recognizing that there is a normal variation, the general consensus is the normal distance from the cementoenamel junction to the alveolar crest is 2.0 mm (Figure 11.1) (Armitage, 1996, Tetradis et al., 2006). The distance may be greater in older patients.
The shape and width of the alveolar crest or interdental septum is dictated by the convexity of the proximal tooth surface and the level of the cementoenamel junction of the adjacent teeth. In the anterior region, the alveolar crest comes to a point due to the close proximity of the teeth. In the posterior region where the interdental space is greater, the alveolar crest is broader and flatter. The angulation of the alveolar crest parallels a line connecting the cementoenamel junction of the adjacent teeth (Ritchey and Orban, 1953).
In a normal and healthy periodontium, the alveolar crest is a thin, continuous radiopaque line that is continuous with the lamina dura (Figure 11.1). Where the alveolar crest meets the lamina dura, the angle is a defined sharp angle (White and Pharoah, 2009).
Periodontal Ligament Space
The principal tissues involved with attachment of the tooth to the jaw can be divided into two parts. The soft tissue attachment are gingival fibers inserting into the cementum of the tooth and are not visible radiographically. The second part are periodontal ligament fibers that connect from the cementum to the alveolar bone. The periodontal ligament fibers are primarily collagen fibers, so they are not visible radiographically. The periodontal ligament space, which these fibers occupy, is a narrow radiolucent structure that is delineated by two radiopaque structures, the alveolar bone and tooth root.
The width of the periodontal ligament is 0.15 mm to 0.38 mm. The narrowest portion is around the middle third of the root while the ligament is the widest at the cervical aspect (Coolidge, 1937). Consequently, the periodontal ligament space is wider at the alveolar crest, narrows at the middle third, and then widens again at the apex.
The periodontal ligament reacts to occlusal forces and is able to accommodate physiological forces. There is a thickening of the fiber bundles and consequently, the periodontal ligament space widens. For example, the width of the periodontal ligament in the middle of the alveolus of a premolar in heavy function increases from 0.10 mm to 0.28 mm (Kronfeld, 1931).
Radiographic Appearance of Periodontitis
Periodontitis is defined as inflammation of the supporting tissues of the teeth (American Academy of Periodontology, 2001). The inflammation results in the destruction of the alveolar bone, periodontal ligament, and the gingival connective tissue attachment. Periodontal pathogens such as Porphyromonas gingivalis, Tannerella forsythia, and Aggregatibacter actinomycetemcomitans initiate this disease but most of the destruction is the result of the host inflammatory response. There are different clinical forms of periodontitis. The most common form is chronic and aggressive periodontitis.
Radiographs are an important adjunct to a clinical examination. They provide useful information about the extent and location of bone loss that have occurred, the width of the periodontal ligament space, local factors such as subgingival calculus, restorations with open margins or overhangs, morphology and length of the root, and crown-to-root ratio (Perschbacher, 2009).
However, there are limitations to the use of radiographs. They only provide a two-dimensional view. Dense bone or the root structure can mask bone loss that has occurred on the facial or lingual surface. Interproximally, the true extent and morphology of interdental craters can be obscured by dense buccal and lingual cortical plates. Typically, there needs to be about 50% bone mineral lost before radiographic changes are detected (Ortman et al., 1982). Clinical attachment loss precedes radiographic evidence of crestal alveolar bone loss by 6–8 months (Goodson et al., 1984). In other words, radiographs underestimate the true extent of destruction that has occurred clinically.
Earliest signs of bone loss include the absence, fuzziness or a break in the crestal lamina dura that may indicate early radiographic changes in periodontitis (Tetradis et al., 2006). However, many stable sites lack an intact lamina dura (Rams et al., 1994). In other words, the absence of the lamina dura is not indicative of disease.
On the other hand, the presence of an intact lamina dura at the alveolar crest indicates a high probability that the site is periodontally stable (Armitage, 1996). If the lamina dura is intact at the apex of the tooth, this strongly suggests a vital pulp (White and Pharoah, 2009).
Other signs of early bone loss are the blunting of the alveolar crest in the anterior region and the rounding or loss of the sharp angle between the lamina dura and alveolar crest in the posterior region (Perschbacher, 2009).
Bone loss is defined when the alveolar crest is more than 2 mm apical to the cementoenamel junction. Bone loss occurs in a horizontal and vertical manner.
Horizontal bone loss is defined when the pattern of the bone loss continues to parallel the line connecting the cementoenamel junction between the adjacent teeth (Figures 11.2 and 11.3). In other words, the alveolar crest remains perpendicular to the root surface. There has been proportionately equal loss of interdental septa, buccal, and lingual bone.
Figure 11.2 Moderate horizontal bone loss with radiolucency in the furcation of the mandibular first molar.
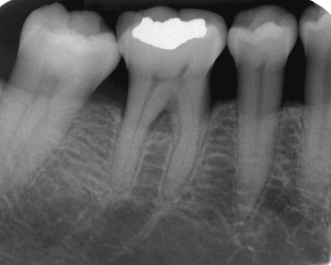
Figure 11.3 Advance horizontal bone loss.
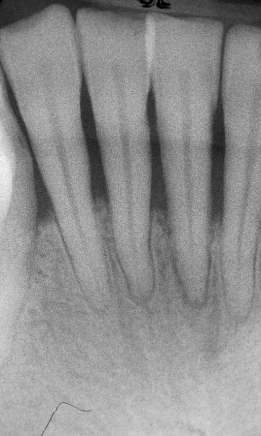
Vertical or angular bone loss is the result of vertical defects where bone loss has occurred in an oblique manner. As a result, the alveolar crest is not parallel to the line between the cementoenamel junctions of the adjacent teeth. Vertical bone loss indicates the presence of vertical or angular osseous defects where they may be classified as one-, two- and three-walled vertical defects (Figures 11.4 and 11.5).
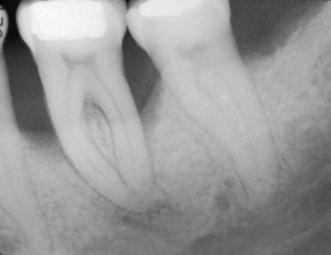
Figure 11.4 Moderate vertical bone loss on the mesial aspects of the mandibular second premolar.
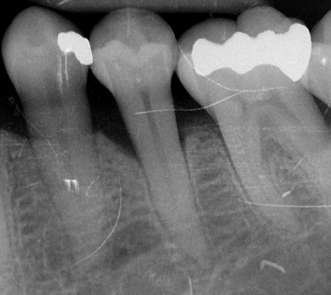
Figure 11.5 Advance vertical bone loss on the distal aspect of the mandibular first molar.
Severity of the bone loss is based on the extent of bone loss in relationship to the amount of root that remains in the bone. If less than 20% of the root is exposed due to the bone loss, then the severity is described as mild. The severity is moderate when there has been 20–50% bone loss (Figures 11.2 and 11.4). Advance bone loss is when more than 50% bone loss has occurred (Figures 11.3 and 11.5). The severity describes the extent of osseous destruction which is o/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


