CHAPTER 11 Occlusion
Your Bite, Temporomandibular Joints, Temporomandibular Dysfunction
Until recent years the area of occlusion in dentistry has not been emphasized. Therefore, many dentists have not been involved with treatment of people with occlusion problems. As a rule, the specialty most involved with movement of teeth to provide acceptable occlusion is orthodontics. Other areas of dentistry, including prosthodontics, periodontics, oral surgery, and general dentistry, are more involved with the condition commonly called temporomandibular dysfunction (TMD) or temporomandibular joints (TMJ) in the lay literature.
Currently, TMD is used most often to describe the syndrome (or disease), while TMJ is used to describe the anatomy of the specific location. This chapter is primarily concerned with TMD, whereas moving of teeth into proper function and appearance is included in the chapter on orthodontics (p. 99).
WHAT YOU SEE OR FEEL
Conditions, Signs or Symptoms Related to Occlusion, or Temporomandibular Dysfunction
1. Pain in the Head (Headaches), Neck, Shoulders
Often, unstimulated pain in the head, neck, and shoulders may be muscle dysfunction related to malaligned occlusion. This syndrome is described as temporomandibular dysfunction (TMD). Innumerable causes are related to head and neck pain, and patients are advised to contact their dentist as soon as possible before making any conclusions, to confirm that the pain they are experiencing may or may not be related to occlusion (bite).
3. Grinding or Grating Sound in Jaw Joints (Crepitus)
4. Can’t Open Jaw Or Can’t Close Jaw
Occasionally the bones, ligaments, and muscles that make up the mechanism of the jaw joints become malaligned, and, as a result, the jaw locks open or closed. This can be painful as well as frustrating. Frequently, your dentist can assist the jaw to open with simple manipulations in the dental office, but more often other treatment is required. One or more of the following treatment methods will probably be used:
5. Teeth Visibly Worn From Bruxism or Clenching
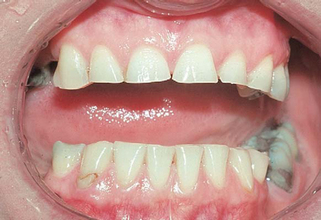
At least one fourth to one third of the world population grinds their teeth excessively, thereby wearing tooth structure beyond normal expectations (Fig. 11.1). This activity is called bruxism or clenching. During the first years of life this wear usually goes undetected, but soon it is evident, and concern is expressed. In the later stages of this problem, pain or even tooth death is caused by the wear. If you brux or clench your teeth excessively, you have the following potential treatment options, directly related to the severity of the condition as observed by your dentist:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses