Chapter 11
Nitrous Oxide/Oxygen Inhalation Sedation in Children
Nitrous oxide (N2O) is an invaluable tool in managing the mild to moderately anxious child. Its ease of administration, wide margin of safety, analgesic and anxiolytic effects, and, most of all, its rapid reversibility make it an ideal drug for use in children (Paterson-Tahmassebi 2003; Houpt 2004). The American Academy of Pediatric Dentistry (AAPD), among other organizations, recognizes nitrous oxide/oxygen inhalation sedation as a safe and effective technique to reduce anxiety, produce analgesia, and enhance effective communication between a patient and health care provider (AAPD 2012). However, clinicians should not make the mistake of thinking that N2O sedation by itself controls behavior. Nitrous oxide serves as an adjunct to behavior management.
Nitrous oxide is now widely accepted as a behavior management technique in pediatric dentistry. Wilson and Alcaino’s (2011) recent international survey, based on 311 replies, revealed that at least 56% of the respondents used nitrous oxide in their practices. Similar numbers were found in a survey of AAPD members by Wilson in 1996 (66.3%) and Houpt in 2002 (61%). Thus, in contrast to earlier studies, N2O is used by more practitioners, and more frequently than before. Its utilization is likely to continue, and it will probably increase. The results from a survey conducted by the Academy of General Dentistry demonstrate that about 74% of American dentists used nitrous oxide/oxygen sedation (Lynch 2007). Adair et al. (2004), who surveyed behavior management teaching techniques in pediatric dentistry advanced education programs, reported that all US dental schools taught N2O sedation.
N20 Historic Milestones
Over the past 200 years, nitrous oxide has been regarded as an asphyxiant, a useless agent, and an anesthetic panacea (Hogue et al. 1971). This has created a colorful history for the drug. Since its applicability to dental practice is still a topic for debate, especially in non-western nations, background knowledge of this agent can be considered relevant for the clinician.
Not long after Joseph Priestley synthesized nitrous oxide in 1772, Sir Humphrey Davy reported on the pleasurable and unusual sensations following the inhalation of nitrous oxide and coined the term “laughing gas.” Davy further suggested that the euphoria associated with nitrous oxide inhalation would be of great benefit in the practice of dentistry (Raper 1945). Some dentists took this advice, and in the early 1840s Wells made practical use of nitrous oxide. He had his own tooth extracted while inhaling N2O that was used for clinical anesthesia (Archer 1944).
Although the analgesic properties of N2O were recognized for some time, the risk of asphyxia when using it as the sole anesthetic agent prevented its use for lengthy operations. However, in 1868, Chicago surgeon Edmund W. Andrews published the results of a large survey which suggested that the anesthetic use of ether and chloroform would be safer by combining these agents with 70% N2O and 30% oxygen. This extended the anesthetic time for longer operations, and the notion of balanced anesthesia was born. At about the same time, gas machines were introduced, making anesthesia more convenient. Dentistry took advantage of this progress. Before the turn of the century, a limited number of dentists were beginning to use nitrous oxide and oxygen for cavity preparations.
Throughout the first half of the twentieth century, the primary interest in nitrous oxide was in its analgesic properties (Langa 1968). Most discussions concerning nitrous oxide stressed the analgesic and anesthetic properties for extractions. Dental offices remained dependent upon nitrous oxide for pain control until the introduction of local anesthesia. The feeling of euphoria caused by nitrous oxide, which was so sought-after during the “laughing gas parties” 100 years earlier, were either ignored or considered a minor benefit during dental procedures.
Since the prevalent attitude among dentists in the early twentieth century was that young children were not suitable patients, few references have suggested using nitrous oxide for the child patient. However, in 1925, physician John S. Lundy specifically described the use of nitrous oxide as an induction agent to prepare children for extractions. Shortly thereafter, Leonard N. Ray, a dentist, acknowledged that many children dreaded the thought of the dentist and dental extractions (1929). Hence, he advocated the use of nitrous oxide and recommended initiating induction with 90% nitrous oxide and 10% oxygen for 30 seconds. He felt that this enabled children to move quickly toward surgical anesthesia. After induction, the oxygen was lowered to 7% and nitrous oxide was increased to 93% for the duration of the procedure. With this approach, he contended that the necessary dentistry for children could “go on unhampered in a way that would be impossible with a local anesthetic.” Concomitant with the nitrous oxide, Ray used behavior management. Suggestion, demonstration, and encouragement were necessary so that children would accept the nasal mask.
Sporadic reports concerning nitrous oxide use in dentistry for children continued to appear, but these remained focused on the anesthetic benefits. As late as 1972, Amian reported on his fifteen years of experience with nitrous oxide and indicated that nitrous oxide analgesia was used routinely for cavity preparations in children. He found that in more than 50,000 applications, usually using 60% nitrous oxide and 40% oxygen, adequate analgesia was provided for cavity preparation. He also noted that the euphoric state was a major benefit to patients. The following year, Sorenson and Roth (1973) emphasized the value of inhalation sedation to reduce children’s fears, particularly the fear of injections. They de-emphasized the analgesic effect of nitrous oxide-oxygen, which is associated with concentrations of nitrous oxide exceeding 40%, and emphasized the sedative/tranquilizing/euphoric benefits of dilute concentrations; that is, less than 40% of nitrous oxide (Allen 1984; McCarthy 1969).
It may be because of the history, but for many years there has been some confusion regarding the terms nitrous oxide inhalation sedation and anesthetic nitrous oxide. As a consequence, anesthesiologists were opposed to the use of N2O by dentists. This is unfortunate because it delayed the widespread use of the agent by dentists. Although N2O now is routinely used in dentistry and considered a safe drug, in medicine it is frequently combined with other general anesthetic agents to produce a balanced anesthesia.
Physiology and Pharmacology
Nitrous oxide is a non-irritating, colorless gas with a faint sweet taste and odor. It is a true general anesthetic, but the least potent of all anesthetic gases in use today. It is an effective analgesic/anxiolytic agent which causes central nervous system (CNS) depression and euphoria with little effect on the respiratory system. Nitrous oxide has rapid uptake, as it is absorbed quickly from the alveoli and held in a simple solution in the serum. It is dissolved and transported in blood; it does not combine with hemoglobin, and it does not undergo biotransformation.
It is relatively insoluble, passing down a gradient into other tissues and cells in the body, such as the CNS. It is excreted quickly from the lungs. Elimination of nitrous oxide occurs by means of expiration in a manner that is precisely the reverse of uptake and distribution, and nitrous oxide’s low solubility allows it to be removed rapidly (Emmanouil and Quock, 2007).
Cardiovascular Effects
N2O causes minor depression in cardiac output while peripheral resistance is slightly increased, thereby maintaining normal blood pressure. This is of particular advantage in treating patients with cerebrovascular system disorders. There are no changes in the heart rate (pulse) or blood pressure. N2O is transported through the blood stream in a free gaseous state. Total saturation in the blood occurs within 3–5 minutes. Total circulation time for one breath of nitrous oxide/oxygen is 3–5 minutes. Any noted changes in respiratory rate are related more to the relaxation of the patient than to the nitrous oxide itself.
CNS Effects
Nitrous oxide has multiple mechanisms of action that underlie its varied pharmacological properties. Subanesthetic concentrations of N2O produce only analgesic and anxiolytic effects without unconsciousness (Dundee et al. 1960). The anesthetic effect of N2O appears to be caused by inhibition of NMDA glutamate receptors, removing its excitatory influence on the nervous system.
Analgesia and Anxiolysis
Analgesic N2O has a long history of use in obstetrics for labor-pain relief (Rosen 2002). Nitrous oxide is also used for self-administered analgesia in cancer patients (Parlow et al. 2005) to alleviate pain and discomfort associated with a number of medical procedures, and in emergency medicine departments for procedures such as treatment of lacerations and orthopedic procedures (Baskett 1970). It is essential to make a clear distinction between the high anaesthetic concentrations of nitrous oxide which produce unconsciousness and the much lower doses that are associated with consciousness and its psychotropic actions; i.e., analgesia, anxiolysis, and euphoria. There is evidence that the relaxation and relief from anxiety during inhalation of N2O is a specific anxiolytic effect that is independent of the analgesic action of N2O. The mechanisms involved are not yet completely understood. However, there is sufficient evidence to suggest that nitrous oxide’s analgesic and anxiolytic actions are parallel to those of opioids and benzodiazepines, respectively (Emmanouil and Quock 2007).
Anesthesia
Nitrous oxide has a well-known role in medical history because it was the first drug used for surgical anesthesia. Despite its limited anesthetic potency, N2O is the most widely used general anesthetic agent. With a minimum alveolar concentration of 104% at 1 atm in humans, N2O by itself would require high-volume percentage and hyperbaric conditions to achieve anesthesia (Hornbein et al. 1982). Therefore, due to its low potency, in clinical practice N2O is generally used to reduce the minimum alveolar concentration of a second inhalation agent for anesthesia and increase the rate of induction (i.e., the second gas effect), and to provide or augment the analgesic component of general anesthesia. General anesthetics like N2O have long been hypothesized to act in a nonspecific manner on neuronal membranes, alter membrane fluidity, and/or influence ion channels. However, a great deal of work is required before the molecular and neural pathways involved in mediating nitrous oxide anesthesia are fully determined (Emmanouil and Quock 2007; Sanders et al. 2008). It is suggested that a common property of NMDA receptor antagonism may underlie the similar pharmacological profiles of N2O and ketamine, an intravenous dissociative anesthetic. The two drugs, in fact, produce synergistic neurotoxicity when used together (Jevtovic-Todorovic et al. 2000).
Nitrous Oxide in Pediatric Dentistry: Rationale and Objectives
Dentistry generates more stress than most other professions, primarily because of the working conditions of the dental practice (Bodner 2008). In particular, the specialty of pediatric dentistry can feature crying children, clashes with parents, and children’s small mouths and teeth, which contribute to a stressful environment. The use of N2O sedation can reduce some of these stresses in the dental office—it helps produce a relaxed atmosphere and it can benefit everyone in the pediatric dental treatment triangle.
The administration of nitrous oxide has major advantages not common to other sedation agents used in dentistry for children. These include: rapid onset, rapid withdrawal, and convenient dosage adjustment to maintain a tranquil and sedated state.
In modern dentistry, children do not often experience real physical pain. Although many procedures are less than pleasurable, children usually fail to recognize shades of gray—only the polarity of black or white, pain or no pain. However, pain, with its physiological and psychological components, can be somewhat difficult to define in the clinical setting. As a result, minor discomforts can be magnified and interpreted as pain. Nitrous oxide can modify these discomforts by the diminution or elimination of pain and anxiety in a conscious patient. It is well recognized for these analgesia/anxiolysis properties.
Like children, adults have fears and anxieties, but they are contained by previous experiences. A child lacking the experiences of an adult has an emotional overflow when placed in an anxious or stressful situation. Due to a lack of experience, the child acts out primary feelings. This reaction or emotional outburst to stress or anxiety is usually in the form of fight-or-flight behavior. Children reacting this way may need assistance in controlling their emotions. Nitrous oxide, as an adjunct to behavior management, can help many children learn to cope with the stressful environment.
Emotions and pain thresholds are interwoven. When a child patient is fearful, anxious, or apprehensive, there is a lower pain threshold. Minor things may irritate and upset the patient. If minimizing pain during treatment is one of the objectives, then reducing the child patient’s level of anxiety is critical. There is a positive association between anticipatory anxiety and procedural pain. Interventions designed to reduce task-specific anticipatory anxiety may help reduce pain responses in children and adolescents (Tsao et al. 2004). When N2O sedation eliminates or reduces fear or anxiety, it raises the pain reaction threshold and reduces fatigue (Weinstein et al. 1986). Both pain sensitivity and pain reaction are altered. Additionally, the pain threshold can be raised with attention and distraction tasks. When the placebo effect of distraction is combined with the sedative properties of nitrous oxide, the injection experience is much more easily accomplished.
Table 11-1. Objectives of nitrous oxide/oxygen inhalation sedation.
| 1. Reduce or eliminate anxiety. 2. Reduce untoward movement and negative reaction to dental treatment. 3. Enhance communication and patient cooperation. 4. Raise the pain reaction threshold. 5. Increase tolerance for longer appointments. 6. Reduce gagging. |
Studies have reported on the effects of N2O from the child’s perspective. Children described dreaming or being on a “space-ride” (Hogue et al. 1971). Berger et al. (1972) reported that some children described a “floating, warm, and tingling sensation” with nitrous oxide. In yet another study, children indicated a preference for music in conjunction with nitrous oxide during dental treatment (Anderson 1980). Langa (1968) described the child under N2O sedation as being in “suspended animation”; i.e., the child’s body does not move, head and extremities remain relaxed, and sudden movements commonly associated with children are eliminated. With the child in a relaxed state, a dentist can provide optimum treatment for a child with minimum trauma for both dentist and patient. Following the foregoing rationale for the use of nitrous oxide/oxygen sedation, many pediatric dentists adopted the technique for managing their child patients. The objectives for nitrous oxide usage are shown in Table 11-1.
Stages of Anesthesia
Four stages of general anesthesia were recognized in Guedel’s classification: (1) induction (also referred to as analgesia), (2) excitement, (3) surgical anesthesia, and (4) overdose (Guedel 1937). The first stage begins with the induction of anesthesia and ends with a patient’s loss of consciousness. Patients still feel pain in this stage. In 1968, Langa introduced a term to represent N2O inhalation sedation: relative analgesia (RA). Langa (1968) proposed that there were three planes of analgesia in the first stage. The planes vary from moderate to total analgesia and are dependent on the concentration of nitrous oxide in the mixture and the signs and symptoms shown by patients (Table 11-2). During N2O inhalation sedation, the patient always remains at the first stage of anesthesia.
In Plane One (5-25% N2O) the patient appears normal, relaxed, and awake, and may feel slight tingling in toes, fingers, tongue, or lips, and may giggle. Vital signs remain normal. There are no definite clinical manifestations.
Table 11-2. Effects of N2O in relation to its concentration.
| 100% will produce anoxia. 80% will produce hypoxia with hallucinations and bizarre dreams; may cause respiratory, cardiovascular, kidney or liver damage. 65% can cause patients to enter the excitement stage. 35% usually provides maximum analgesia with maintenance and cooperation of the patient. 25% is an analgesic equipotent to 10 mg morphine sulphate. |
In Plane Two, or relative analgesia (20-55% N2O), the patient may have a dreamy look, eyes appearing “glassy” (occasionally with tears), reactions are slowed and the voice may sound “throaty.” The patient will feel warm and drowsy, may drift in and out of the surrounding environment, and may hear pleasant ringing in the ears. Partial amnesia may occur. Vital signs remain normal. Pain is reduced or eliminated, but touch and pressure are still perceived. The patient is less aware of surroundings; sounds and smells are dulled. The term psychotropic analgesic nitrous oxide (PAN) was introduced by Gillman and Lichtigfeld (1994) to describe Plane Two of analgesia. This term clearly distinguishes the concentrations of nitrous oxide used for anxiolysis/analgesia from the much higher doses used for anesthesia, wherein the patient is totally unconscious.
In Plane Three (55-70% N2O), the patient becomes angry, with a hard stare; the pupils usually are centrally fixed and dilated, the mouth tends to close frequently, and the patient is unaware of his surroundings and may hallucinate. When patients are in Plane Three, Roberts (1990) reported that they may experience sensations of flying, falling, or uncontrolled spinning, or the chest may feel heavy, and the patient will no longer cooperate.
Plane Two provides adequate N2O sedation and allows dentist-child communication, although some clinicians prefer the dream period, usually characterized by closed eyes and difficulty with speech. Figure 11-1 portrays a patient’s appearance in Plane Two. Plane One is usually of short duration, while Plane Two can be maintained for several hours. Children in Plane Two usually respond to questions by moving the head rather than speaking. Facial features are relaxed and the jaw usually sags, remaining open without mouth props. The eyes are usually closed but will open in response to questions. The arms are heavy and will stay where placed, and the hands are open. The legs often slide off the side of the chair. All vital signs are stable. There is no significant risk of losing protective reflexes, and the child is able to return to pre-procedure mobility. The objective of the sedation should be to reach, but not pass, this plane. This is the desirable sedation level when performing N2O sedation.
Figure 11-1. A patient’s appearance in Plane Two. Facial features are relaxed and the jaw usually sags, remaining open without mouth props. The eyes are usually closed but will open in response to questions. Courtesy of Dr. Ari Kupietzky.
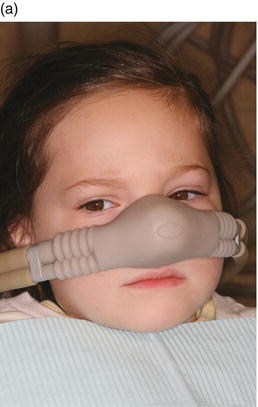
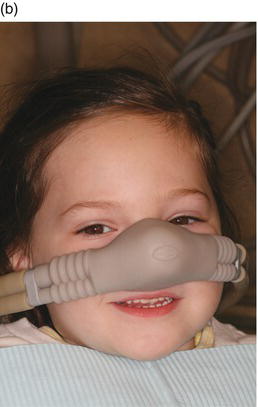
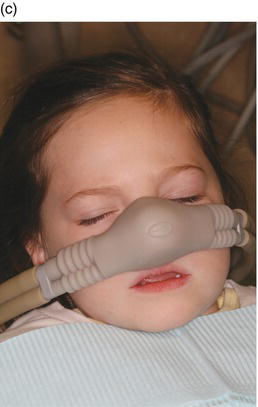
Table 11-3. Clinical tips to evaluate level of N2O inhalation sedation.
| Eyes are very indicative of the sedation level. Reduced activity of the eyes indicative of desirable level of sedation. Increased activity of the eyes may indicate that sedation is too light. Fixed, hard stare of the eyes: sedation is too deep, N2O % needs to be decreased. Arms and legs crossed: the patient is not relaxed yet, increase N2O %. Patient talks too much: sedation is too light due to mouth breathing. Do not increase; just try to get patient to stop talking. Use of a rubber dam will prevent this situation. Patient answers rapidly: sedation is too light. Patient answers slowly and deliberately: good sedation. Patient does not answer: may be tired and asleep. If used in combination with another sedative agent, stimulate patient and check verbally. Perspiration appears on the face: reassure patient that this is expected and will pass. Paraesthesia of extremities: reassure patient that this is normal and will dissipate after treatment. Paraesthesia of lips, tongue, or oral tissues: profound depth; time for injection of local anesthetic. |
For some patients, the feeling of “losing control” may be troubling. Others may be claustrophobic and unable to tolerate the nasal hood, finding it confining and unpleasant (Stach 1995). A patient’s experience after nitrous oxide is believed to be similar to a posthypnotic state. During N2O there is an enhancement of suggestibility and imaginative ability that may be utilized while managing the child’s behavior and dental experience. This can be advantageous. Suggestions, such as “fixing teeth is fun,” made while a patient is experiencing N2O sedation might make subsequent visits easier and more readily accepted (Whalley and Brooks 2009). Another beneficial suggestion is to instruct ways to improve oral hygiene.
Individual biovariability accounts for different reactions to various concentrations of N2O. Some individuals experience several symptoms, while others experience only a few. Symptoms are intense for some and insignificant for others. Sometimes signs are obvious; at other times, they are subtle. Titration allows for the biovariablility of any patient that may be associated with the administration of the substance. Titrating nitrous oxide/oxygen and careful observation of patient responses are keys to successful administration.
Clinicians must know what signs and symptoms to look for when administering and monitoring N2O sedation(Table 11-3).. Keeping a constant vigil is imperative because pleasant sensations may quickly change and become unpleasant. Knowledge of the appropriate technique and associated physical, physiologic, and psychological changes minimizes negative patient experiences.
Case 11.1, Discussion: While the ultimate goal is to increase patient comfort through relaxation (Clark and Brunick 2007), another important goal is for nitrous oxide/oxygen to serve as an adjunct to behavior management. It is not for all patients, and before selecting a management method for a/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


