Chapter 10
Overdentures: The Bottom Line for Older Adults?
Aim
This chapter aims to review the rationale for the use of complete overdentures in older adults.
Outcome
At the end of this chapter, the practitioner should be aware of the advantages and disadvantages of overdentures, the treatment of patients requiring overdentures and maintenance issues. The possibility of minimising bone loss and thus potentially overcoming some of the limitations of complete replacement dentures should also be recognised.
Rationale for Overdenture Therapy
This technique utilises roots of natural teeth to support a complete denture. Atrophy of alveolar bone occurs following the loss of natural teeth. This phenomenon is particularly noticeable in the mandible that resorbs at approximately four times the rate of resorption of alveolar bone in the maxilla. Transmission of masticatory forces to the underlying bone via the teeth is thought to provide a functional stimulus to the bone, thus leading to turnover of bone. Loss of teeth removes this stimulus and bone atrophy is the inevitable consequence. Despite extensive research, the reason for great individual variation in bone loss remains unclear. From the evidence currently available, it seems that post-extraction alveolar bone loss is influenced by a combination of both local and systemic factors. While the pathogenesis of alveolar bone loss remains unclear, there is no reliable way in which to predict the rate of alveolar bone loss on an individual basis.
During the 1970s, the technique of using roots of teeth to support removable complete dentures (overdentures) was described. Research at that time indicated that retention of roots beneath removable dentures maintained bone height and prevented alveolar bone resorption adjacent to the roots (see Fig 1-2). This greatly facilitated the stability and retention of complete dentures.
In some patients, the loss of most of the natural dentition may be inevitable. Given that complete replacement dentures have many limitations, a sensible “bottom line” in the management of older adults should be the retention of some roots to support complete overdentures.
Benefits of overdentures
Potential benefits of overdentures include:
-
preservation of alveolar bone
-
aiding the stability and retention of dentures
-
psychological well-being
-
maintaining proprioception.
In addition to preserving bone, the roots provide a means of increasing retention and stability of a complete denture. The contact between the roots themselves and the fitting surface of the denture provides a degree of friction grip. Furthermore, the roots can be used to retain precision attachments (Fig 10-1), which in turn can be used to enhance denture retention in certain situations.
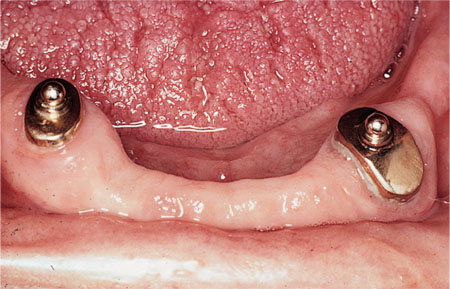
Fig 10-1 Ball attachments on cast post and diaphragm on mandibular overdenture abutments. Corresponding o-ring attachments are incorporated into the denture.
Retention of some part of the natural dentition can be important from a psychological point of view for some patients. As the oral health of older adults improves, it seems likely that older adults will be less likely to accept that tooth loss is an inevitable part of the ageing process. Consequently, retaining some portion of their natural dentition will be of benefit.
Proprioceptive receptors are found in the periodontal ligaments of teeth and form part of the reflex loop for mastication. Masticatory forces are detected by these receptors and this information is conducted to the masticatory centre in the brain. A reflex loop is completed by signals being transmitted to the masticatory muscle groups in the jaw to depress the mandible. This precise control mechanism facilitates fine chewing movements and detection of food texture. When all natural teeth have been lost, this mechanism is also lost and this impacts significantly on chewing performance.
Selection of abutment teeth for overdentures
The principle criteria for selection of teeth as suitable for overdenture abutments are:
-
At least two roots should be retained.
-
They should be symmetrically distributed.
-
It should be possible to create a dome shape with or without restorations.
-
At least 50% bone support remains.
-
Endodontic procedures should be possible.
For complete overdenture prostheses, at least two roots should be kept for support. These should be symmetrically distributed in the dental arch to ensure stability of the denture. Failure to follow these guidelines is likely to result in a denture that “rocks” as it pivots around a single root surface or roots not symmetrically distributed. The roots chosen for overdenture support should have a reasonable degree of bone support, and as a general rule of thumb there should be at least 50% bone support. A moderate degree of mobility is not a contraindication, as this is likely to diminish once the crown root ratio has been reduced with preparation of the crown of the tooth. It should be possible to create a dome shape either by preparing the roots or by inserting cast dome-shaped restorations into the root canals. Teeth that have decayed below the alveolar crest of bone are not suitable as overdenture abutments. A further relative contraindication would be if the tooth were not suitable for endodontic procedures. This sometimes occurs in older adults where deposition of secondary dentine occludes the root canals and makes access for instrumentation along the whole of the root canal difficult or impossible. In some cases, the clinician may choose to use such roots as long as there is no evidence of apical pathology. A further option is to choose an adjacent root that is more favourable for endodontic procedures.
Endodontic considerations
In most circumstances, root canal therapy is required and this should be undertaken using standard guidelines. A variety of materials can be used to fill access cavities, and the most commonly used are dental amalgam, composite resins and glass ionomer cements. Whichever material is chosen, it is vital that the material is well retained – the clinician should remove 2–3 mm of gutta percha from the root canal to ensure adequate bulk of material is placed in the access cavity. Should the access cavity restoration fall out or fail, there is a distinct possibility of coronal leakage with infection of />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


