Chapter 7
Endodontics and the Older Adult
Aim
To consider special issues affecting endodontic decision-making and treatment in the elderly.
Outcome
At the end of this chapter, the practitioner should have raised awareness of general and local factors that may support or undermine the case for root canal treatment in an elderly patient.
Endodontics and the Older Adult
Apical periodontitis has the same aetiology in all age groups – namely, microbial infection of the pulp space. Tissue responses to infection control are predictable, and there is no reason to expect that the elderly will respond any less well to adequate treatment than other age groups. The decision whether to extract a pulpally or periapically involved tooth in the elderly should not therefore be based on age considerations, but on an evaluation of general and local factors for and against tooth preservation. Some of these will be of special relevance in the elderly.
Key Issues
Can the tooth be saved?
Is root canal treatment technically possible, and will the tooth be restorable after treatment?
Should the tooth be saved?
Even if the tooth can be root canal treated and restored, is there any benefit to be gained by its preservation? Would retention or loss of the tooth create general or local complications in patient care?
Can the Tooth be Saved?
Is the tooth restorable?
Teeth judged after clinical and radiographic examination to be unrestorable should be extracted. There are no rewards for heroically conducting root canal treatment on teeth that have no functional capacity due to tissue loss, fracture or periodontal compromise.
Can infection be controlled?
Predictable treatment demands an access to the infected pulp space. If this is complicated by limited mouth opening; unfavourable tooth alignment or overeruption; intolerance of lengthy operative procedures or calcification of the pulp space, it may not be possible to save the tooth, and treatment should be planned accordingly.
Will the patient consent to treatment?
Treatment planning should not be self-indulgent and go beyond the realistic aspirations of the patient. There may be occasions when patients will not consent or subject themselves to complex treatment plans, ruling out the preservation of a tooth that could be saved by root canal treatment.
Is the proposed care affordable?
Ideal treatment plans are all well and good, but these are sometimes beyond the financial means of patients. Simpler treatment is often dictated, and, once again, a tooth that could be preserved should be sacrificed within a simpler plan of care.
Should the Tooth be Saved?
Medical considerations
There are few medical contraindications to endodontic therapy. Antibiotic prophylaxis is not usually required for endodontic treatment confined to the pulp space since this carries a very low risk of significant bacteraemia. In fact, root canal treatment may be positively indicated to avoid extraction in patients with cardiac problems or those taking anticoagulant medication.
Relative contraindications to endodontic treatment include:
-
Patients requiring radiotherapy to the head and neck region. All foci of infection should be removed prior to commencement of radiotherapy.
-
Poor compliance (e.g. patients with Parkinson’s disease, tremors, or dementia).
-
Patients unable to lie comfortably in a dental chair for prolonged periods (e.g. those with ankylosing spondylitis).
Is this a critical tooth?
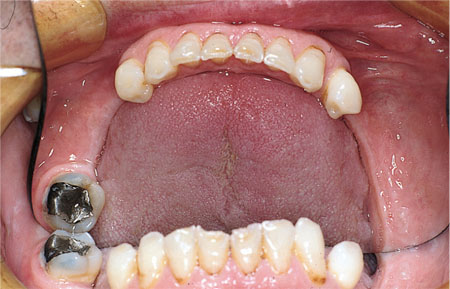
The functional and aesthetic value of the tooth should be reviewed. From a functional point of view, the tooth may not be critical and extraction may be a more attractive option. Conversely, the tooth may be useful as a retainer for an RPD (Fig 7-1) or as an overdenture abutment.
-
Teeth that are periodontally compromised may serve well as overdenture abutments after root canal treatment and decoronation.
-
Retention of a final standing molar may help to preserve occlusal stability, avoid the need for an RPD altogether, or at least avoid the need for it to have a free-end saddle.
-
Even short-term retention of a tooth may facilitate the progressive transition into edentulousness by providing natural occlusal stops and facilitating the development of motor skills in controlling partial dentures.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses