1
General Principles of Radiology in Endodontics
“… And God said: Let there be light. And there was light. And God saw the light, which it was good; and God divided the light from the darkness …”
(Genesis 1:3–4, The Bible, King James version)
Endodontics is the branch of dentistry in which radiology plays a critical indispensable role. Radiology illuminates what otherwise would be dark and hidden zones and allows the dentists to visualize areas not accessible by other diagnostic means. It is the use of oral radiographs which enables visualization of the bone around the apices of the teeth, as well as the results of the root canal treatments, and as such it has allowed turning endodontics into a scientific professional entity (Grossman, 1982).
History of Dental Radiology
The many developments over the years in the field of dental radiology cannot be adequately appreciated without looking back to the discovery of X-radiation.
The Cathode Tube
The first step occurred in 1870. Wilhelm Hittorf found that a partially evacuated discharged tube could emit rays able to produce heat and cause a greenish-yellow glow when they strike glass. By placing a magnet within easy reach and changing the path of the rays Varley determined that these rays were negatively charged particles and they were later called electrons. It was Goldstein from Germany who called the streams of charged particles “cathode rays.” He was followed by William Crooks, an English chemist, who redesigned the vacuum tube which subsequently was known as Hittorf–Crookes tube. In 1894, Philip Lenard studied the cathode rays’ behavior with the aid of a tube with an aluminum window. He placed screens with fluorescent salts outside the aluminum window and found that most of the rays could penetrate the window and make the fluorescent screen glow. He noticed that when the tube and screens were separated, the light emitted decreased. When they were separated by 8 cm, the screens would not fluoresce.
Radiographs
Dr. Wilhelm Conrad Roentgen from Würzberg, Germany, studied rays emitted from a tube in a darkened room; he noticed that some crystals of barium platinocyanide from a table nearby became fluorescent The observation was made on the evening of Friday, November 8, 1895. Roentgen understood that the tube was emitting some hitherto unknown kind of ray which produced the fluorescence and called this rays “X-rays” because the nature of the rays was unknown and uncertain. He also noticed that if a metallic object was placed between the tube and screen, it cast a shadow, and he reported a number of “shadow-pictures” he had photographed. One was the shadow of a set of weights in a closed box; another was a piece of metal whose homogeneity was revealed by the X-rays. But the most interesting picture was of the bones of his wife’s hand which was exposed to the rays for 15 minutes. This was the first radiograph taken of the human body and represented the beginning of practicing radiology in medicine and dentistry.
Roentgen continued to study the X-rays and found that the beam could be diminished in relation to what was placed in its path. The only material that completely absorbed the beam was lead. He went on with his experiments and finally defined the following features of X-rays: (1) they are able to distinguish between various thicknesses of materials; (2) they cause certain elements to fluoresce; (3) they are made of pure energy with no mass; (4) they go in straight lines; and (5) they are not detectable by human senses. Roentgen’s great work revolutionized the diagnostic capabilities of the medical and dental professions, and he was awarded with the first Nobel Prize in Physics in 1901. In modern terms, X-ray radiation is a form of electromagnetic radiation with a wavelength from 0.01 to 10 nm. It is emitted from a metal anode (usually tungsten, molybdenum, or copper) when subjected to a stream of accelerated electrons coming from the cathode.
Dental Radiographs
It was Otto Walkhoff, a German dentist, who made the first dental radiograph 14 days after Roentgen’s discovery.
He placed a glass photographic plate wrapped in black paper and rubber in his mouth and submitted himself to 25 minutes of X-ray exposure. In that same year, W.J. Morton, a New York physician, made the first dental radiograph in the United States using a skull and also took the first whole body radiograph. A dentist from New Orleans, Dr. C. Edmund Kells, made the first intraoral radiograph on a patient in 1896. Kells exposed his hands to X-rays every day for years by holding the plates and trying to adjust the quality of the beam in order to achieve clear images. Unfortunately, this exposure led to the development of cancer in his hand which resulted in the amputation of his arm, demonstrating the potential risk and harmful effects of X-rays. Three years later (1899), Kells used the X-ray to determine tooth length during root canal therapy.
Radiograph Machines
William H. Rollins, a Boston dentist, developed the first dental X-ray unit in 1896, as well as intraoral film holders. He was the first one to publish a paper on the potential dangers of X-rays. Rollins proposed the use of filters to suspend the dangerous parts of the X-ray beam, the use of collimation, and the practice of covering the patient with lead to prevent X-ray penetration. Rollins also pointed out the importance of setting safe and harmful dose limits. In 1913, William D. Coolidge, an electrical engineer, developed a high vacuum tube that contained a tungsten filament, which became the first modern X-ray tube. Further in 1923, Coolidge and the General Electric Corporation immersed an X-ray tube, in oil, inside the head of an X-ray machine. This eliminated the accidental exposure to high voltage shock, cooled the tube, and served as a model for all modern dental X-ray machines. From that time on, the dental X-ray machine did not change much until 1957 when a variable kilovoltage dental X-ray machine was introduced, followed by the long-cone head in 1966.
Dental X-Ray Film
Dental X-ray films also changed through the years; from the original glass photographic plates, hand-wrapped dental X-ray packets in 1896, to the prewrapped intraoral films manufactured by the Eastman Kodak company which were first introduced in 1913. The current high-speed, double-emulsion films require a very short exposure time and were designed to further reduce X-ray exposure.
The bisecting oral radiographic technique was first introduced in 1904 by Weston Price, and the bite-wing technique was introduced by H. Raper in 1925. The paralleling technique was originally introduced in 1896 by C.E. Kells and reformed in 1947 by F.G. Fitzgerald with the introduction of the long-cone (see Table 1.1) (Cieszynski, 1925).
Table 1.1 Milestones in the history of dental radiography.
| 1895 | Discovery of X-rays | W.C. Roentgen |
| 1896 | First dental radiograph | 0. Walkhoff |
| 1901 | First paper on risks of X-radiation | W.H. Rollins |
| 1913 | First prewrapped dental films | Eastman Kodak Company |
| 1913 | First X-ray tube | W.D. Coolidge |
| 1923 | First dental X-ray machine | Victor X-ray Corporation |
| 1947 | Introduction of long-cone Paralleling technique |
F.G. Fitzgerald |
| 1957 | First variable kilovoltage dental X-ray machine |
General Electric |
Hazards of X-Ray Radiation
Ionizing radiation can have harmful effects. The largest man-made source of exposure of radiation to humans is from medical and dental radiographic examinations. Yet one should keep in mind that we are also exposed to other sources and types of radiation. These include radiation from building materials and luminous goods (i.e., television, computer), as well as natural sources (i.e., cosmic rays, soil).
The risk effects depend on the dose received, the frequency of exposure, and the type of tissue irradiated. In general, tissues whose cells divide frequently are more sensitive to the effects of radiation than those that are less active. Susceptible cells include hematopoietic cells, immature reproductive cells, young bone cells, and epithelial cells. The more radiation-resistant cells include the cells of bones, muscles, and nerves. Ionizing radiation has the effect of increasing the incidence and severity of DNA defects during mitotic division of cells and also interferes with the normal process of repair of these defects. As a consequence, the behavior of the cells may be altered and predispose them to malignant changes. To protect radiation exposure for patients and operators, the use of radiation is governed by state, national, and international agencies. Based on recommendations of the International Commission for Radiation Protection (ICRP), many countries have introduced the following regulation form on radiation protection: (1) doses should be kept as low as reasonably achievable (ALARA); (2) there should be a net benefit for the patient from the use of radiation; (3) radiation doses should not exceed limits laid down by the ICPR; (4) a shield or lead apron should always be used to protect the thyroid and the pelvis; (5) only dental X-ray equipment that is properly collimated, adequate filtrated, and well calibrated should be used; and (6) the X-ray operator shall stand outside the path of the useful X-ray beam or behind a suitable barrier, and should not hold the film in place for the patient during exposure (NCRP Report, 1970, 1989, 1990, 1988; Richard and Colquit, 1981).
Objectives of Dental Radiography
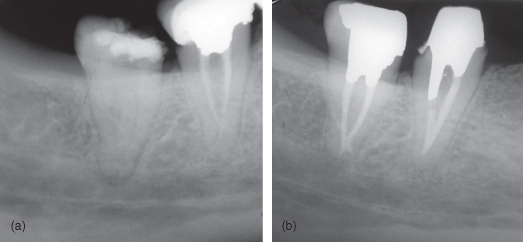
Dental radiographs are an essential part of the dental diagnostic process, as they enable the practitioner to see many conditions that are not apparent clinically and which could otherwise go undetected. An oral examination without dental radiographs limits the practitioner to what is seen clinically—the surfaces of teeth and soft tissues. Numerous conditions of the teeth and jaws can only be detected on dental radiographs. Missing teeth, extra teeth, and impacted ones, dental caries, periodontal disease as well as root canal fillings, periapical lesions, cysts, and tumors are among the most common conditions that cannot otherwise be diagnosed or properly detected. Suspected pathological conditions can often be confirmed only on using radiographs. Radiographs often contain a huge amount of information, far more than a written record will usually include. Therefore, initial radiographic examination may provide valuable baseline information about the patient. Follow-up radiographs can then be used to detect and evaluate subsequent changes resulting from treatment, trauma, or disease (Figure 1.1a,b). Patient communication may also greatly benefit from the use of dental radiographs (DeLyre and Johnson, 1995; Haring and Lind, 1996).
Figure 1.1 (a) Tooth #48 presenting apical lesion. (b) Tooth #48 after root canal treatment presenting healed periapex.
X-Rays and Endodontics
Endodontics is the branch of dentistry that has benefited the most from the introduction of X-rays into everyday dental practice. X-rays allow dentists to visualize areas not accessible by any other diagnostic means such as changes that occur in the bone surrounding the apices of nonvital teeth, intricate root canal anatomy, as well as the ability to follow up the results of endodontic treatment (Gröndahl and Huumonen, 2004). Due to introduction of X-rays, endodontics could turn from an empirical pursuit to a soundly based scientific discipline. Intraoral periapical, occlusal, and panoramic radiographs form the backbone of the endodontic diagnostic process, treatment procedures, and follow-up routine in most of endodontic cases.
Most osteolytic lesions in the jaws result from the pathological changes occurring in the periradicular tissue as a consequence of pulpal infection and necrosis.
The irritants exiting the infected root canal to the periradicular tissues activate both nonspecific inflammatory reactions and specific immune reactions. These not only prevent the spread of infection to the surrounding bone and to remote sites but also result in local bone resorption that can be visualized by radiographic techniques (Stashenko et al., 1998).
The use of radiographs in endodontics is intensive and not limited to the above. They are used to define anatomical features of the roots, such as numbers of roots, their locations, their shape and size, as well as the presence of root canal space. Technical aspects of root canal treatment are greatly assisted by radiographs. These include confirming the length of root canals before instrumentation, determining position of instruments during the procedure and of master cones at the obturation stage. Evaluation of the quality of the root canal filling is based mainly on its radiographic appearance and so is the evaluation of the result of treatment during the follow-up that takes place later. Traumatic injuries to the dentition also make use of radiography for the diagnosis of fractures in the roots and/or the alveolus or for examining the soft tissues for teeth fragment that may have been embedded in them during the traumatic incident. One can hardly imagine endodontic treatment without the assistance of radiography (Cotti and Campisi, 2004; Nair, 1998a; Torabinejad et al., 1985).
Limitations of X-Rays in Endodontics
With all its benefits, one has to keep in mind that conventional dental radiograph represents merely a two-dimensional (2D) shadow of a three-dimensional (3D) structure (Bender and Seltzer, 1961). As such, it has substantial limitations that should be recognized and taken into consideration when interpreting such records. The buccolingual dimension is not represented in conventional radiographs, thus limiting their interpretation as to the actual 3D size of the radiolucent lesions and their spatial relationship with anatomic landmarks (Cotti and Campisi, 2004; Gröndahl and Huumonen, 2004; Huumonen and Orstavik, 2002). It should also be kept in mind that radiographs do not provide information as to the true nature of the tissue that replaced the bone. Chronic inflammatory lesions cannot reliably be differentiated from cysts or from scar tissue that also mimic osteolytic lesions (Nair, 1998b; Simon, 1980).
For a radiolucent lesion to appear in the radiograph, a substantial amount of bone must have been resorbed; thus, the lack of radiolucency should not be interpreted as absence of bone resorbing process. Furthermore, bone resorption of the cancelous bone surrounding the apex may not be recognized in a periapical radiograph as long as a substantial part of the covering cortical bone has not been resorbed as well (Gröndahl and Huumonen, 2004; Marmary et al., 1999).
Observer Bias
Radiographic interpretation is prone to observer bias. Goldman has found that when recall radiographs of endodontic tre/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


