Functional Anatomy and Biomechanics of the Masticatory System
“NOTHING IS MORE FUNDAMENTAL TO TREATING PATIENTS THAN KNOWING THE ANATOMY.”
—JPO
THE MASTICATORY SYSTEM, a functional unit of the body, is primarily responsible for chewing, speaking, and swallowing. Its components also play a major role in tasting and breathing. The system is made up of bones, joints, ligaments, teeth, and muscles. In addition, an intricate neurologic controlling system regulates and coordinates all these structural components.
The masticatory system is a complex and highly refined unit. A sound understanding of its functional anatomy and biomechanics is essential to the study of occlusion. This chapter describes the anatomic features that are basic to an understanding of masticatory function. A more detailed description can be found in the numerous texts devoted entirely to the anatomy of the head and neck.
Functional Anatomy
The following anatomic components are discussed in this chapter: the dentition and its supportive structures, the skeletal components, the temporomandibular joints (TMJs), the ligaments, and the muscles. After the anatomic features are described, the biomechanics of the TMJs are presented. Chapter 2 presents the complex neurologic controlling system responsible for carrying out the intricate functions of the masticatory system.
Dentition and Supportive Structures
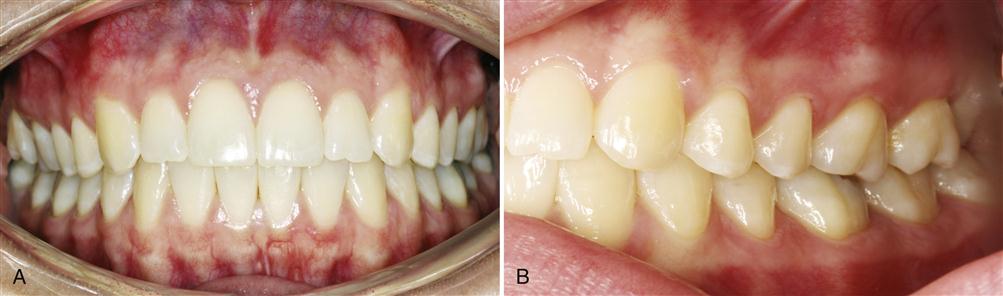
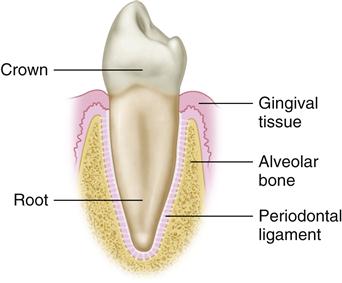
The human dentition is made up of 32 permanent teeth (Figure 1-1, A,B). Each tooth can be divided into two basic parts: the crown, which is visible above the gingival tissue, and the root, which is submerged in and surrounded by the alveolar bone. The root is attached to the alveolar bone by numerous fibers of connective tissue that span from the root’s cementum surface to the bone. Most of these fibers run obliquely from the cementum in a cervical direction to the bone (Figure 1-2). These fibers are known collectively as the periodontal ligament. It not only attaches the tooth firmly to its bony socket but also helps dissipate the forces applied to the bone during functional contact of the teeth. In this sense it can be thought of as a natural shock absorber. The periodontal ligament has specialized receptors that provide information on pressure and position. This sensory information is essential for function, as described in the next chapter.
The 32 permanent teeth are distributed equally in the alveolar bone of the maxillary and mandibular arches: 16 maxillary teeth are aligned in the alveolar process of the maxilla, which is fixed to the lower anterior portion of the skull; the remaining 16 teeth are aligned in the alveolar process of the mandible, which is the movable jaw. The maxillary arch is slightly larger than the mandibular arch, which usually causes the maxillary teeth to overlap the mandibular teeth both vertically and horizontally when in occlusion (Figure 1-3). This size discrepancy results primarily from the fact that (1) the maxillary anterior teeth are much wider than the mandibular teeth, which creates a greater arch width, and (2) the maxillary anterior teeth have a greater facial angulation than the mandibular anterior teeth, which causes some horizontal and vertical overlapping.
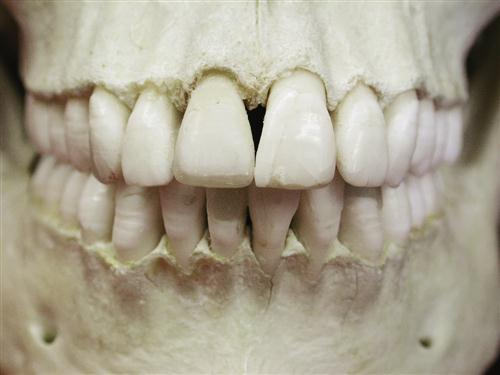
The permanent teeth can be grouped into four classifications, according to the morphology of the crowns, as follows.
The teeth located in the most anterior region of the arches are called incisors. They have a characteristic shovel shape, with an incisal edge. There are four maxillary incisors and four mandibular incisors. The maxillary incisors are generally much larger than the mandibular incisors and, as previously mentioned, commonly overlap them. The function of the incisors is to incise or cut off food during mastication.
Posterior (distal) to the incisors are the canines. The canines are located at the corners of the arches and are generally the longest of the permanent teeth, with a single cusp and root (Figure 1-4). These teeth are very prominent in other animals such as dogs; hence the name canine. There are two maxillary and two mandibular canines. In other animals, the primary function of the canines is to rip and tear food. In humans, however, the canines usually function as incisors and are used only occasionally for ripping and tearing.
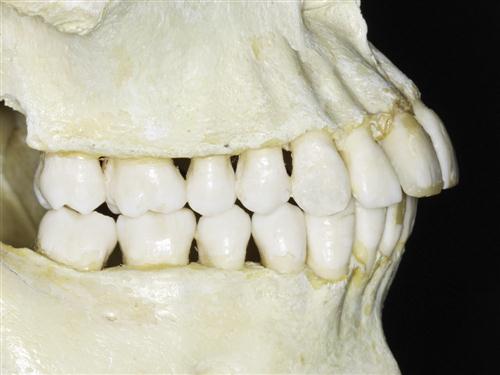
Still more posterior in the arch are the premolars (Figure 1-4). There are four maxillary and four mandibular premolars. The premolars are also called bicuspids, since they generally have two cusps. The presence of two cusps greatly increases the biting surfaces of these teeth. The maxillary and mandibular premolars occlude in such a manner that food can be caught and crushed between them. The main function of the premolars is to begin the effective breakdown of food substances into smaller particle sizes.
The last class of teeth, found posterior to the premolars, comprises the molars (Figure 1-4). There are six maxillary and six mandibular molars. The crown of each molar has either four or five cusps. This provides a large broad surface upon which the breaking and grinding of food can occur. Molars function primarily in the later stages of chewing, when food is broken down into particles small enough to be easily swallowed.
As discussed, each tooth is highly specialized according to its function. The exact interarch and intra-arch relationships of the teeth are extremely important and greatly influence the health and function of the masticatory system. A detailed discussion of these relationships is presented in Chapter 3.
Skeletal Components
The skeletal components of the human head are the skull and mandible (Figure 1-5). The skull is composed of several bones connected by fissures. The major components are the temporal bone, the frontal bone, the parietal bone, the sphenoid bone, the occipital bone, the zygomatic bone, the nasal bone, and the maxilla. The mandible is a separate bone suspended below the cranium in a muscle sling. The three major skeletal components that make up the masticatory system are the maxilla and mandible, which support the teeth (Figure 1-6), and the temporal bone, which supports the mandible at its articulation with the cranium.
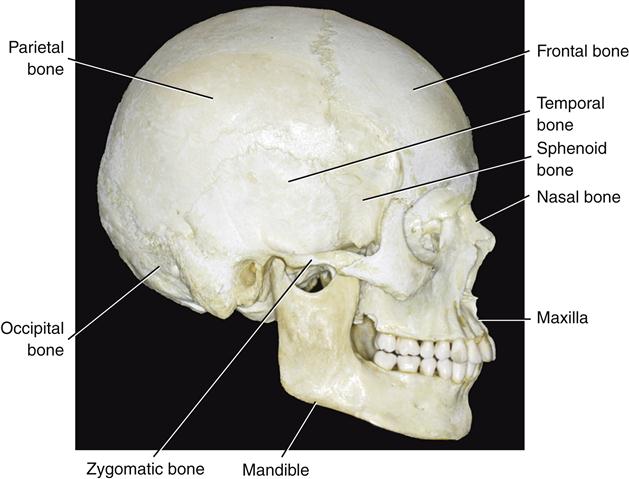
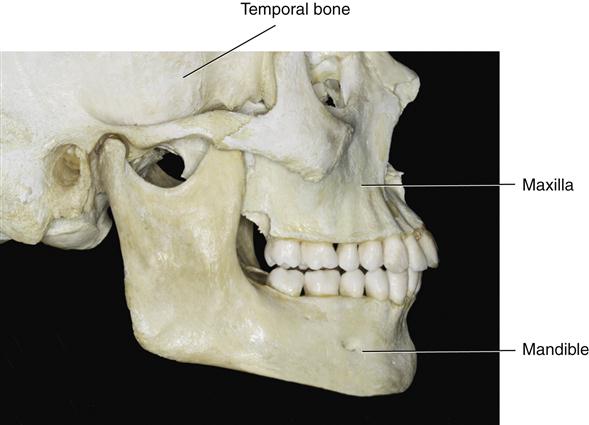
The maxilla
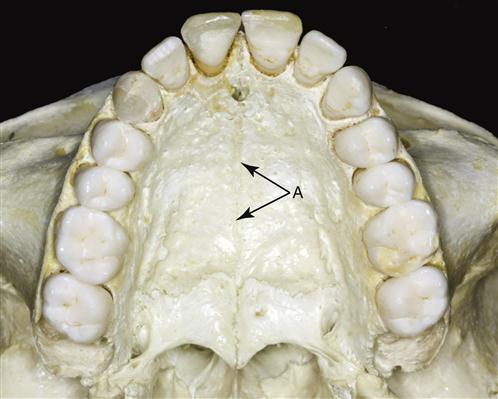
Developmentally there are two maxillary bones, which are fused at the midpalatal suture (Figure 1-7). These bones make up the greater part of the upper facial skeleton. The border of the maxilla extends superiorly to form the floor of the nasal cavity as well as the floor of each orbit. Inferiorly, the maxillary bones form the palate and the alveolar ridges, which support the teeth. Since the maxillary bones are intricately fused to the surrounding bony components of the skull, the maxillary teeth are considered to be a fixed part of the skull and therefore make up the stationary component of the masticatory system.
The mandible
The mandible, a U-shaped bone, supports the lower teeth and makes up the lower facial skeleton. It has no bony attachments to the skull. It is suspended below the maxilla by muscles, ligaments, and other soft tissues, which therefore provide the mobility necessary for the mandible to function with the maxilla.
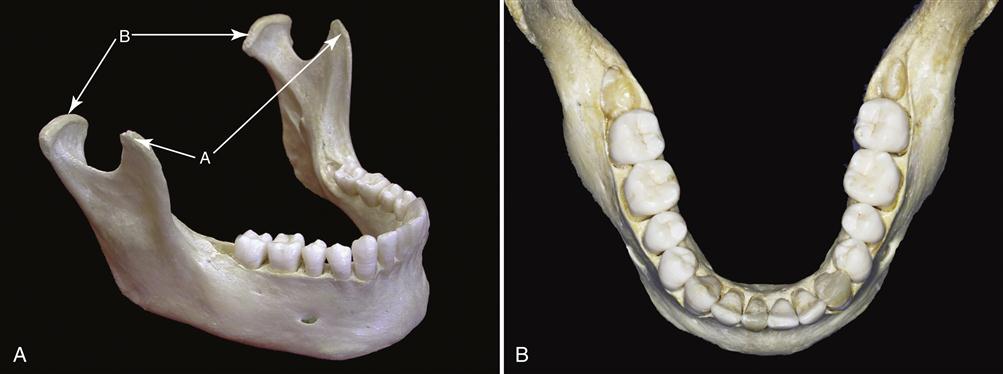
The superior aspect of the arch-shaped mandible consists of the alveolar process and the teeth (Figure 1-8). The body of the mandible extends posteroinferiorly to form the mandibular angle and posterosuperiorly to form the ascending ramus. The ascending ramus of the mandible is formed by a vertical plate of bone that extends upward as two processes. The anterior of these is the coronoid process. The posterior process is the condyle.
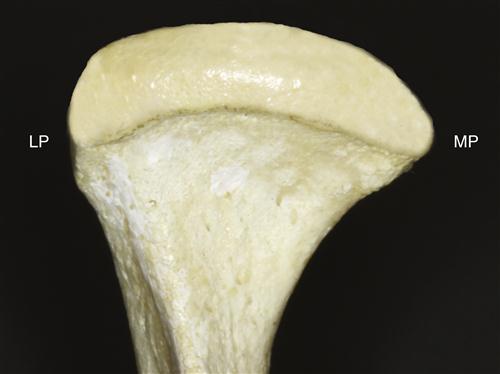
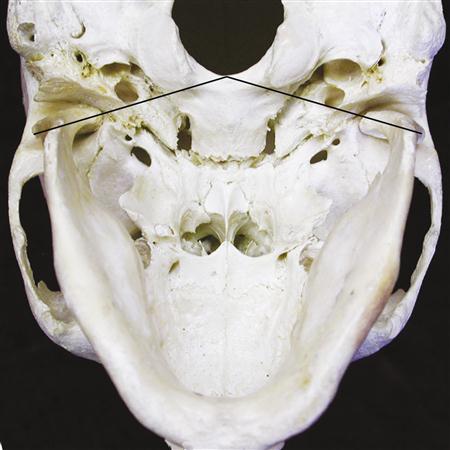
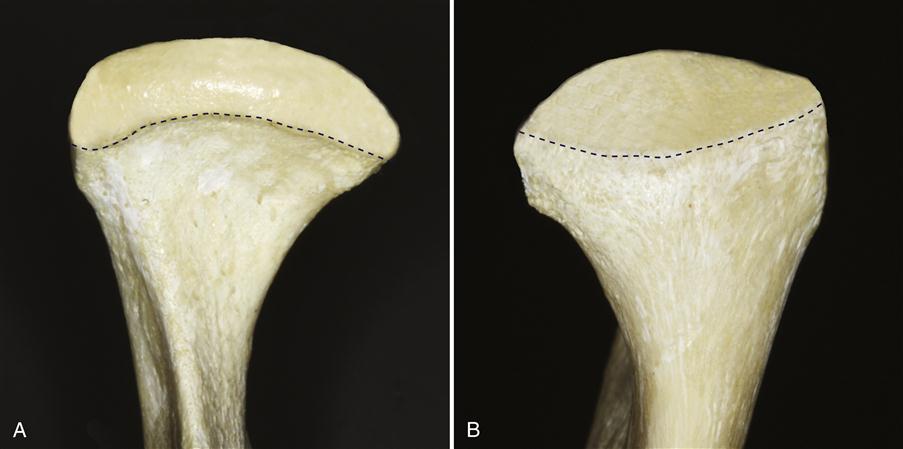
The condyle, the portion of the mandible that articulates with the cranium, is the structure around which movement occurs. From the anterior view it has medial and lateral projections, called poles (Figure 1-9). The medial pole is generally more prominent than the lateral one. From above, a line drawn through the centers of the poles of the condyle will usually extend medially and posteriorly toward the anterior border of the foramen magnum (Figure 1-10). The total mediolateral length of the condyle is between 18 and 23 mm; the anteroposterior width is between 8 and 10 mm. The actual articulating surface of the condyle extends both anteriorly and posteriorly to the most superior aspect of the condyle (Figure 1-11). The posterior articulating surface is greater than the anterior surface. The articulating surface of the condyle is quite convex anteroposteriorly and only slightly convex mediolaterally.
The temporal bone
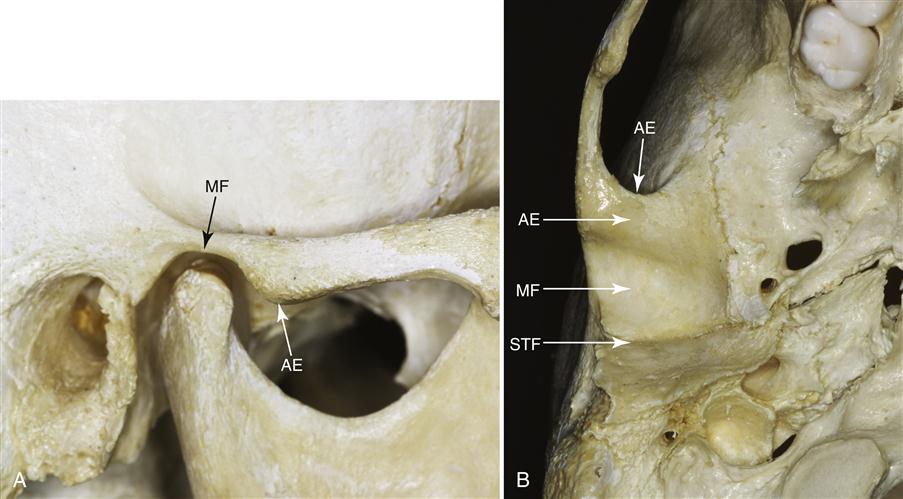
The mandibular condyle articulates at the base of the cranium with the squamous portion of the temporal bone. This portion of the temporal bone is made up of a concave mandibular fossa, in which the condyle is situated (Figure 1-12) and which has also been called the articular or glenoid fossa. Posterior to the mandibular fossa is the squamotympanic fissure, which extends mediolaterally. As this fissure extends medially, it divides into the petrosquamous fissure anteriorly and the petrotympanic fissure posteriorly. Immediately anterior to the fossa is a convex bony prominence called the articular eminence. The degree of convexity of the articular eminence is highly variable but important, since the steepness of this surface dictates the pathway of the condyle when the mandible is positioned anteriorly. The posterior roof of the mandibular fossa is quite thin, indicating that this area of the temporal bone is not designed to sustain heavy forces. The articular eminence, however, consists of thick dense bone and is more likely to tolerate such forces.
The Temporomandibular Joint
The area where the mandible articulates with the temporal bone of the cranium is called the temporomandibular joint (TMJ), certainly one of the most complex joints in the body. It provides for hinging movement in one plane and therefore can be considered a ginglymoid joint. However, at the same time it also provides for gliding movements, which classifies it as an arthrodial joint. Thus it has been technically considered a ginglymoarthrodial joint.
The TMJ is formed by the mandibular condyle and the mandibular fossa of the temporal bone, into which it fits. The articular disc separates these two bones from direct articulation. The TMJ is classified as a compound joint. By definition, a compound joint requires the presence of at least three bones, yet the TMJ is made up of only two. Functionally, the articular disc serves as a nonossified bone, which permits the complex movements of the joint. Since the articular disc functions as a third bone, the craniomandibular articulation is considered a compound joint. The function of the articular disc as a nonossified bone is described in detail later in this chapter under “Biomechanics of the Temporomandibular Joint.”
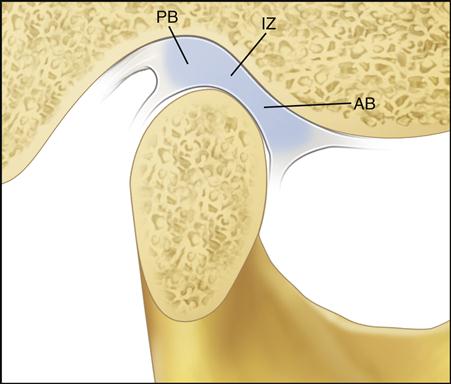
The articular disc is composed of dense fibrous connective tissue for the most part devoid of any blood vessels or nerve fibers. The extreme periphery of the disc, however, is slightly innervated.1,2 In the sagittal plane it can be divided into three regions, according to thickness (Figure 1-13). The central area is the thinnest and is called the intermediate zone. The disc becomes considerably thicker both anterior and posterior to the intermediate zone. The posterior border is generally slightly thicker than the anterior border. In the normal joint the articular surface of the condyle is located on the intermediate zone of the disc, bordered by the thicker anterior and posterior regions.
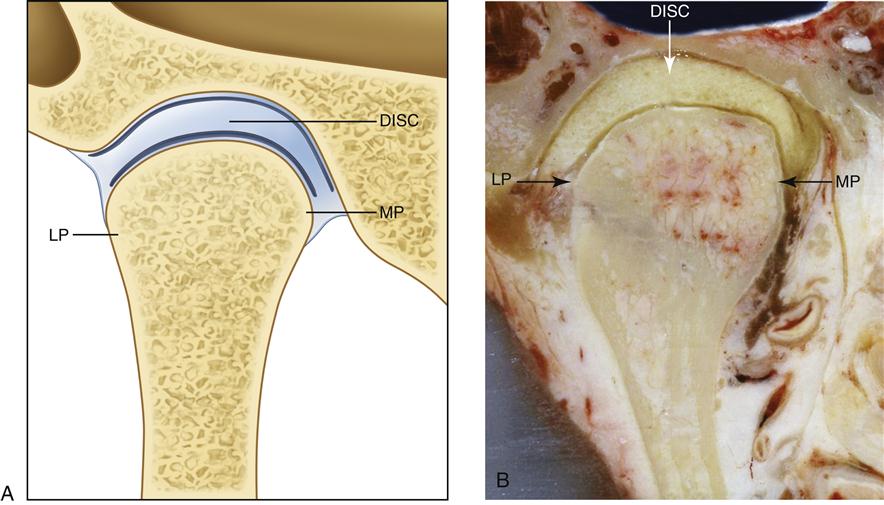
From an anterior view, the disc is usually a little thicker medially than laterally, which corresponds to the increased space between the condyle and the articular fossa toward the medial portion of the joint. The precise shape of the disc is determined by the morphology of the condyle and mandibular fossa (Figure 1-14). During movement, the disc is somewhat flexible and can adapt to the functional demands of the articular surfaces. However, flexibility and adaptability do not imply that the morphology of the disc is reversibly altered during function. The disc maintains its morphology unless destructive forces or structural changes occur in the joint. If these changes occur, the morphology of the disc can be irreversibly altered, producing biomechanical changes during function. These changes are discussed in later chapters.
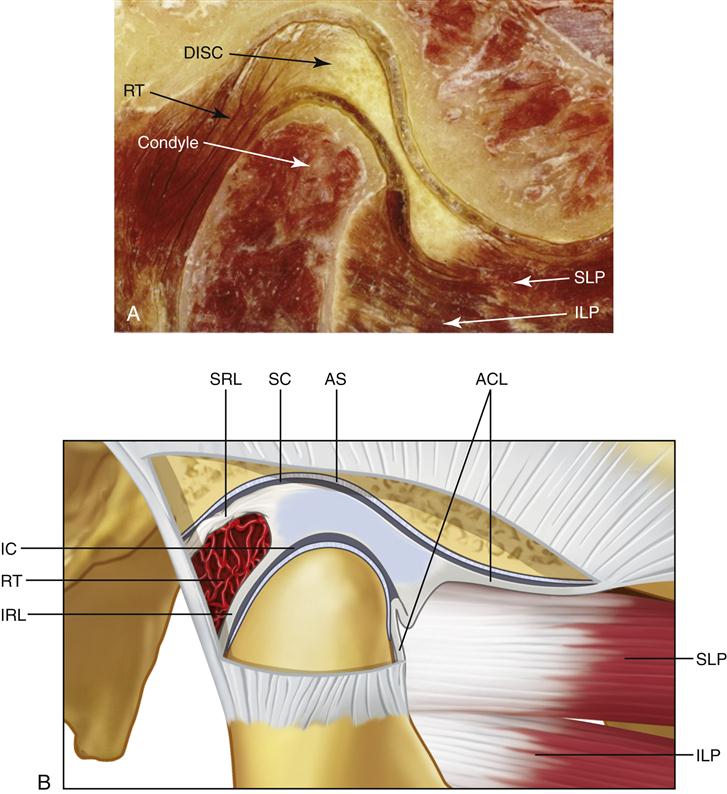
The articular disc is attached posteriorly to a region of loose connective tissue that is highly vascularized and innervated (Figure 1-15). This tissue is known as the retrodiscal tissue or posterior attachment. Superiorly, it is bordered by a lamina of connective tissue that contains many elastic fibers, the superior retrodiscal lamina. The superior retrodiscal lamina attaches the articular disc posteriorly to the tympanic plate. At the lower border of the retrodiscal tissues is the inferior retrodiscal lamina, which attaches the inferior border of the posterior edge of the disc to the posterior margin of the articular surface of the condyle. The inferior retrodiscal lamina is composed chiefly of collagenous fibers, not elastic fibers like the superior retrodiscal lamina. The remaining body of the retrodiscal tissue is attached posteriorly to a large venous plexus, which fills with blood as the condyle moves forward.3,4 The superior and inferior attachments of the anterior region of the disc are to the capsular ligament, which surrounds most of the joint. The superior attachment is to the anterior margin of the articular surface of the temporal bone. The inferior attachment is to the anterior margin of the articular surface of the condyle. Both these anterior attachments are composed of collagenous fibers. Anteriorly, between the attachments of the capsular ligament, the disc is also attached by tendinous fibers to the superior lateral pterygoid muscle.
The articular disc is attached to the capsular ligament not only anteriorly and posteriorly but also medially and laterally. This divides the joint into two distinct cavities. The upper or superior cavity is bordered by the mandibular fossa and the superior surface of the disc. The lower or inferior cavity is bordered by the mandibular condyle and the inferior surface of the disc. The internal surfaces of the cavities are surrounded by specialized endothelial cells, which form a synovial lining. This lining, along with a specialized synovial fringe located at the anterior border of the retrodiscal tissues, produces synovial fluid, which fills both joint cavities. Thus the TMJ is referred to as a synovial joint. This synovial fluid serves two purposes. Since the articular surfaces of the joint are nonvascular, the synovial fluid acts as a medium for providing metabolic requirements to these tissues. Free and rapid exchange exists between the vessels of the capsule, the synovial fluid, and the articular tissues. The synovial fluid also serves as a lubricant between articular surfaces during function. The articular surfaces of the disc, condyle, and fossa are very smooth, so that friction during movement is minimized. The synovial fluid helps to minimize this friction further.
Synovial fluid lubricates the articular surfaces by way of two mechanisms. The first is called boundary lubrication, which occurs when the joint is moved and the synovial fluid is forced from one area of the cavity into another. The synovial fluid located in the border or recess areas is forced on the articular surface, thus providing lubrication. Boundary lubrication prevents friction in the moving joint and is the primary mechanism of joint lubrication.
A second lubricating mechanism is called weeping lubrication. This refers to the ability of the articular surfaces to absorb a small amount of synovial fluid.5 During function of a joint, forces are created between the articular surfaces. These forces drive a small amount of synovial fluid in and out of the articular tissues. This is the mechanism by which metabolic exchange occurs. Under compressive forces, therefore, a small amount of synovial fluid is released. This synovial fluid acts as a lubricant between articular tissues to prevent sticking. Weeping lubrication helps eliminate friction in the compressed but not moving joint. Only a small amount of friction is eliminated as a result of weeping lubrication; therefore prolonged compressive forces to the articular surfaces will exhaust this supply. The consequence of prolonged static loading of the joint structures is discussed in later chapters.
Histology of the articular surfaces
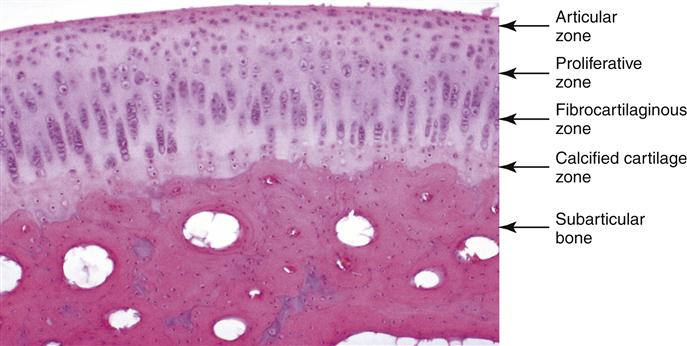
The articular surfaces of the mandibular condyle and fossa are composed of four distinct layers or zones (Figure 1-16). The most superficial layer is called the articular zone. It is found adjacent to the joint cavity and forms the outermost functional surface. Unlike the superficial layers of most other synovial joints, this layer is made of dense fibrous connective tissue rather than hyaline cartilage. Most of the collagen fibers are arranged in bundles and oriented nearly parallel to the articular surface.6,7 The fibers are tightly packed and able to withstand the forces of movement. It is thought that this fibrous connective tissue affords the joint several advantages over hyaline cartilage. It is generally less susceptible than hyaline cartilage to the effects of aging and therefore is less likely to break down over time. It also has a much better ability to repair itself than does hyaline cartilage.8 The importance of these two factors is significant in TMJ function and dysfunction and is discussed more completely in later chapters.
The second zone is called the proliferative zone and is mainly cellular. It is in this area that undifferentiated mesenchymal tissue is found. This tissue is responsible for the proliferation of articular cartilage in response to the functional demands placed on the articular surfaces during loading.
The third zone is the fibrocartilaginous zone. Here the collagen fibrils are arranged in bundles in a crossing pattern, although some of the collagen is seen in a radial orientation. The fibrocartilage appears in a random orientation, providing a three-dimensional network that offers resistance against compressive and lateral forces.
The fourth and deepest zone is the calcified cartilage zone. It is made up of chondrocytes and chondroblasts distributed throughout the articular cartilage. In this zone the chondrocytes become hypertrophic, die, and have their cytoplasm evacuated, forming bone cells from within the medullary cavity. The surface of the extracellular matrix scaffolding provides an active site for remodeling activity during endosteal bone growth, as it does elsewhere in the body.
The articular cartilage is composed of chondrocytes and an intercellular matrix.9 The cho/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses