Fig. 3.1
Some potential aetiologic agents associated to the development of gingival recessions. Teeth crowding (a), reduced thickness of the alveolar bone plate (b), muscular inserts close the gingival margin + dental biofilm accumulation (c), periodontitis (d), improper extraction of a supernumerary tooth (e), trauma (oral piercing) (f), ortodontic tooth movement beyond the buccal alveolar bone plate (g), traumatic toothbrushing (h), lack of keratinised gingiva (i)
During anamnesis and clinical examination, any of these “differential” conditions should be analysed and shared with the patient. Apart from the primary aetiology of the defect, it should be clear in mind that its “elimination” (i.e. the removal of the factors associated with the onset and progression of the lesion and the provision of adequate information on that to the patient) is more important than any simple or highly sophisticated root coverage procedure [2–10].
3.1.3 Anatomy of Gingival Recessions: “How Should I Classify Them?”
Together with the identification of the agents causing the recession, the characterisation of the anatomical structures surrounding an exposed root surface demands special attention as well. This is because the diagnosis of the defects, as similar to all other fields of medicine and dentistry, can provide a “snapshot” and guide the treatment plan options.
Of an assorted group of classification systems described in the literature created to characterise and “quantify” the amount of tissue loss over the exposed root surface [28–33], the “classification of marginal tissue recession” proposed by Miller in 1985 [30] is certainly the most used and accepted one by regular clinicians and the scientific community. This classification system is based on the amount of soft tissue lost over the root surface and the condition of interproximal periodontal tissues, and it can separate defects into four classic morphological groups (Fig. 3.2):
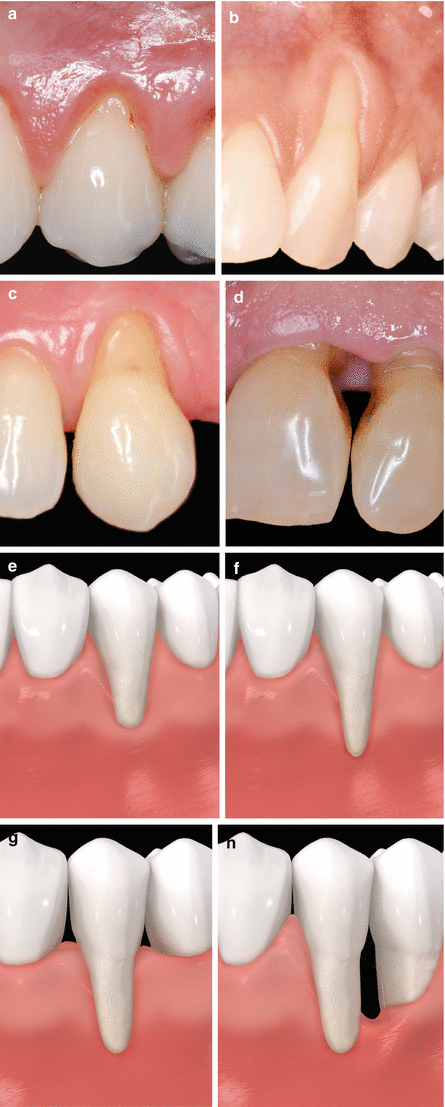

Fig. 3.2
Class I (a, e), Class II (b, f), Class III (c, g), Class IV (d, h)
-
Class I: “Marginal tissue recession which does not extend to the mucogingival junction. There is no periodontal loss (bone or soft tissue) in the interdental area, and 100 % root coverage can be anticipated” [30].
-
Class II: “Marginal tissue recession which extends to or beyond the mucogingival junction. There is no periodontal loss (bone or soft tissue) in the interdental area, and 100 % root coverage can be anticipated” [30].
-
Class III: “Marginal tissue recession which extends to or beyond the mucogingival junction. Bone or soft tissue loss in the interdental area is present or there is malpositioning of the teeth which prevents the attempting of 100 % root coverage. Partial root coverage can be anticipated” [30].
-
Class IV: “Marginal tissue recession which extends to or beyond the mucogingival junction. The bone or soft tissue loss in the interdental area and/or malpositioning of teeth is so severe that root coverage cannot be anticipated” [30].
3.1.4 Additional Conditions to Be Considered During Preparing the Treatment Plan: Smoking and Recipient Site’s Characteristics
The detrimental impact of smoking on nonsurgical and surgical periodontal therapy has long been studied [3, 7, 9, 10]. There is clear evidence that smokers may benefit from soft tissue root coverage; however, the use of SCTG does not provide the same effect of treatment as that achieved in nonsmokers [3, 7, 9, 10]. At 6 months post-therapy, smoking may affect the outcomes of therapy. It may be expected that there are 17.5 % less root coverage and around 36 % fewer sites with complete root coverage in smokers treated with SCTG [10]. By taking these numbers into account, it can be seen that at least three defects in smokers need to be treated to result in one more defect reaching CRC than in the nonsmokers [10]. At 1 year after treatment, recessions treated with SCTG + CAF present significant less root coverage for smokers (89.0 %) than nonsmokers (92.6 %). At 3 years, these values drop to 68.0 % versus 81.5 %, respectively [10]. Likewise, the number of sites exhibiting complete root coverage decreased between these time periods in both groups (i.e. for nonsmokers, it moved from 72.5 to 42.5 %), but within smokers, it was very drastic (62.1–12.5 %) [10].
These results may be associated to interleukin 1 gene polymorphism (i.e. smokers testing positive to it seem to be at an increased risk of periodontal breakdown after treating the recessions) [34], the anatomy of the palatal vault of smokers (less vascularised/inferior number of blood vessels) [35] and the flap thickness (it has been suggested that defects ≥0.95 mm were 100 % covered in nonsmokers, while for some smokers, it did not happen) [36]. These conditions seem to influence revascularisation and incorporation of the SCTG and overall wound healing [3, 10]. On the other hand, the effect of treatment to smoking and nonsmoking patients with CAF seems the same at 6-month follow-up; however, there is limited information available for a definitive analysis [3, 10]. In addition, heavy smokers (≥10 cigarettes/day) may be benefited by the treatment of their recessions as well, but the use of graft or flap procedures alone may not be enough [3, 10]. The use of enamel matrix derivative associated to ADMG + CAF suggests better clinical outcomes than defects treated without such a protein [37].
For recessions presenting also non-carious cervical lesions (i.e. root abrasion due to traumatic toothbrushing), the use of resin-modified glass ionomer or microfilled resin composite prior to surgery (and the subsequent coverage of part of these restorations) does not cause detrimental negative effects on bleeding on probing [38–43] or subgingival microflora [44]. The depth and the vertical extension of the cervical lesion should be assessed prior to any treatment. Deeper cervical lesions may lead to greater coverage, but CRC of the defect might not be achieved [45].
Moreover, the option of restoring or not these defects before treatment may be critically accounted (Fig. 3.3), since there has not been a significant difference in the amount of root coverage between restored and non-restored lesions, and virtually half of the cervical restorations presented colour change after 2 years of treatment (e.g. an aditional question may arise, how these restoration can be removed/changed?). Also, SCTG + CAF seems to perform better than CAF [42]. Thus, it seems more advantageous to treat the recession first (i.e. to perform the chosen root coverage procedures), wait for early healing (at least 6 months) and then perform the definitive restoration of the remaining cervical lesion. Zucchelli et al. [46] suggested that the selection of procedures should be based on the following types of combined defect: (a) Types I and II (radicular cervical lesions plus Class I or II GR), RC alone; (b) Type III (crown-radicular cervical lesion plus Class I, II or III GR), coronal and radicular odontoplasty + restoration + RC; (c) Type IV (radicular cervical lesion plus Class III or crown-radicular cervical lesion plus Class I or II with the deepest point of the cervical lesion localised at the level of the anatomic crown), coronal and radicular odontoplasty + restoration + RC; and (d) Type V (radicular cervical lesion plus Class III or IV GR with the cervical lesion located “on that portion of the root surface that was not coverable with soft tissues”), restoration alone [46]. Additionally, the contralateral tooth may be used to identify and reconstruct the cemento-enamel junction level of the teeth with non-carious cervical lesions [47].
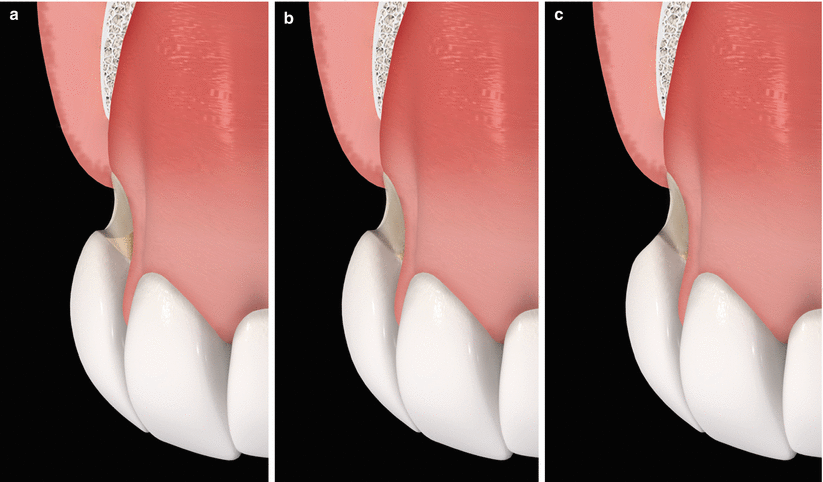

Fig. 3.3
Types of non-carious cervical lesion [46] – gingival recession associated to root abrasion (a), gingival recession associated to root abrasion and loss of dentinary support of the enamel (b), gingival recession associated to root abrasion and enamel loss (c)
With respect to teeth with caries or previously restored, these may be successfully treated, but the carious dentin/root restorations need to be removed and the root surfaces be meticulously planned prior to surgery (Fig. 3.4). Independently of treating exposed roots with or without caries/lesions, it is of paramount importance to perform thoroughly “cleaning” of the anticipated surface to be covered. Scaling and root planning with hand or ultrasound instruments and root polishing may be used [10]. Chemical agents like 1 % citric acid, EDTA and tetracycline hydrochlorides may be used as well, but these will not promote additional benefits to the surgical therapy applied (Fig. 3.5) [2–10].
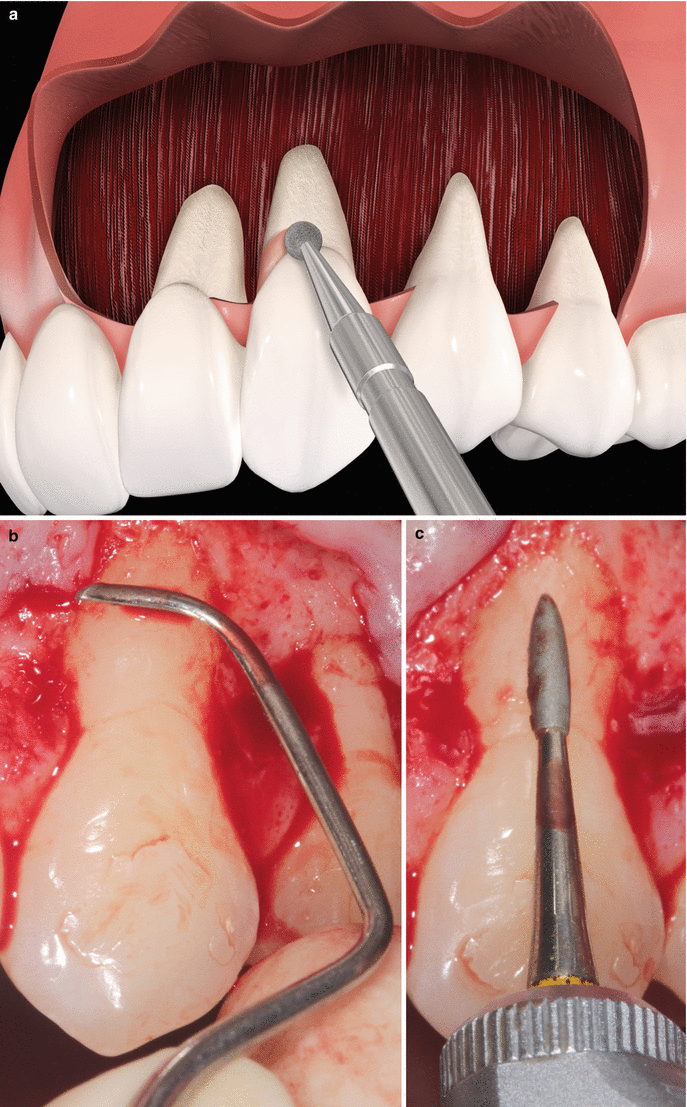
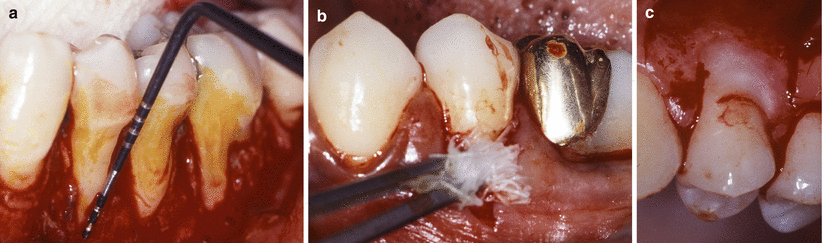

Fig. 3.4
Removal of old restorations (a), scaling and root planning (b), finishing with rotary instruments/handpiece (c)

Fig. 3.5
Use of root modification agents. Tetracycline hydrochloride (a), citric acid (b), EDTA (c)
In addition, both maxillary/mandibular and anterior/posterior teeth may be equally benefited by treatment of their associated recessions, but gains in the amount of keratinised tissue can be superior in sites located in the upper arch (without importance from a clinical point of view) [48, 49]. Furthermore, evidence indicates that palatal/lingual defects may be safely treated by SCTG.
3.1.5 Diversity of Clinical Scenarios and Clinician’s Reflection of Treatment Options to Be Considered
Many times, the treatment plan of recession-type defects may not only account for the best treatment option available but to the inherent characteristics of the defect/area to be treated as well. For instance, not only localised and narrow Class I recessions will be forwarded to treatment (in fact, many patients presenting such defects do not mind in treating them). The occurrence of dissimilar “clinical scenarios” may increase the degree of difficulty during decision-making once their treatment will not only lead with the best evidence available but with clinician’s experience and patients’ expectations as well. Thus, questions related to the potential treatment options available and the importance of treating that specific types of defect require attention.
With respect to the diversity of potential clinical scenarios faced day by day by clinicians attending at private clinical practice, the American Academy of Periodontology [10] in its recent workshop has pointed out some common conditions and questions that may be accounted to help them during the preparation of a treatment plan:
-
Clinical scenario #1: A complex case involving multiple recession–type defects in aesthetic areas [10]:
Is there sufficient donor tissue to be removed from the palatal vault? Is it safe to use a flap procedure alone? or Should other biomaterial be used? What factors will lead me to the best choice? [10]
How can I improve my odds of achieving a satisfactory result? Is it possible to use a flap procedure alone or should I associate a graft/biomaterial to it? Will a restorative/prosthetic approach be required? [10]
What is the best technique/material to graft over these previously restored root surfaces? Should the restoration be removed or changed? Is it safe and predictable to surgically treat these areas? [10]
Should that alter the treatment approach? Do these areas need to be restored? If yes, before, during or after the surgical procedure? [10]
Is it possible to cover carious root surfaces? After removing the caries it is obvious a restoration will be necessary. How does that change the treatment plan? Similarly to abraded surfaces, do these areas need to be restored before, during or after the surgical procedure? [10]
What are the risks and benefits associated to the use of allogenous or xenogenous graft substitutes? Do they provide an evidence of long term stability? [10]
-
Clinical scenario #7: Most patients are interested not only in root coverage but in achieving the best colour and texture match [10]:
What technique should be used to achieve these goals? [10]
Are the results of therapy stable? What is known about the attachment of the graft/flap to the root and should I care? Is it possible to estimate the outcomes and propose treatment options (i.e. establish a decision tree)? Is it possible to obtain satisfactory results when treating smoking patients? [10]
Are the geometry and the degree of recession important (e.g. narrow and deep versus wide and shallow)? Is the amount of available keratinized attached gingiva important in the decision making process? Does the degree of keratinized gingiva in the final outcome affect the long-term stability of cases? [10]
3.1.6 Healing of the Recessions After Treatment: “Why Is It Important and Why Should I Care?”
Information on human histology is not easy to be accessed due to inherent ethical conditions related to it. Within the available cases published in the literature, on acellular dermal matrix graft, coronally advanced flap, enamel matrix derivative, free gingival graft, guided tissue regeneration, laterally positioned flap, subepithelial connective tissue grafts and xenogenic collagen matrix, wound healing may be anticipated consisting of long junctional epithelium and connective tissue attachment (with fibres parallel to the root surface) (Fig. 3.6) [10]. Additionally, some degree of tissue regeneration may happen in the most apical portion of the defects mostly for EMD- and GTR-based procedures (i.e. new connective tissue attachment with newly formed cementum and crestal bone) [10].
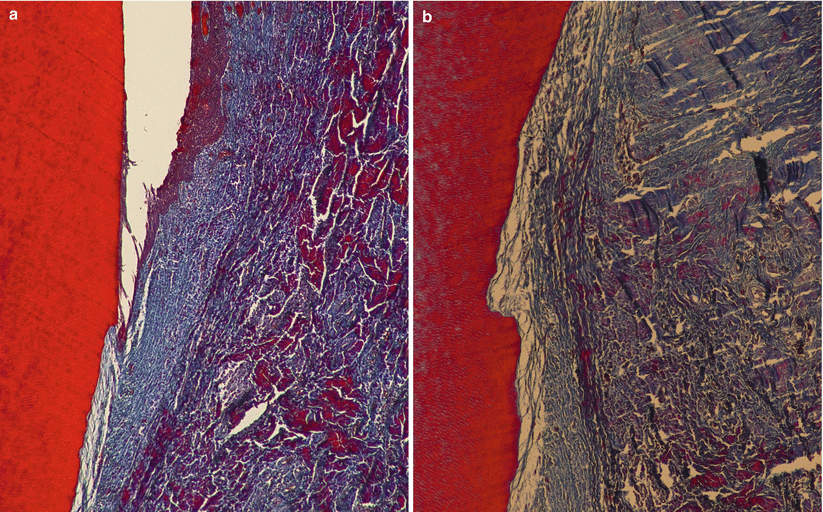

Fig. 3.6
Histologic healing – formation of a long junctional epithelium and connective tissue attachment (100× (a), 200× (b))
Consequently, after treatment, it is expected a shallow gingival sulcus that may be maintained over the long term when the causal agent was treated/removed. On the other hand, when the causal agent of the recession is not removed, apical migration of the gingival margin may quickly occur. In clinical terms, it should be noted that the majority of patients seeking root coverage procedures are not periodontitis patients and their defects are of traumatic origin (e.g. traumatic toothbrushing). For such patients, clinicians should pay attention to correct/adequate detrimental hygiene measures (Fig. 3.7) and remove other potential traumatic agents (e.g. oral piercings) in order to maintain the stability of the result achieved with the treatment [10].
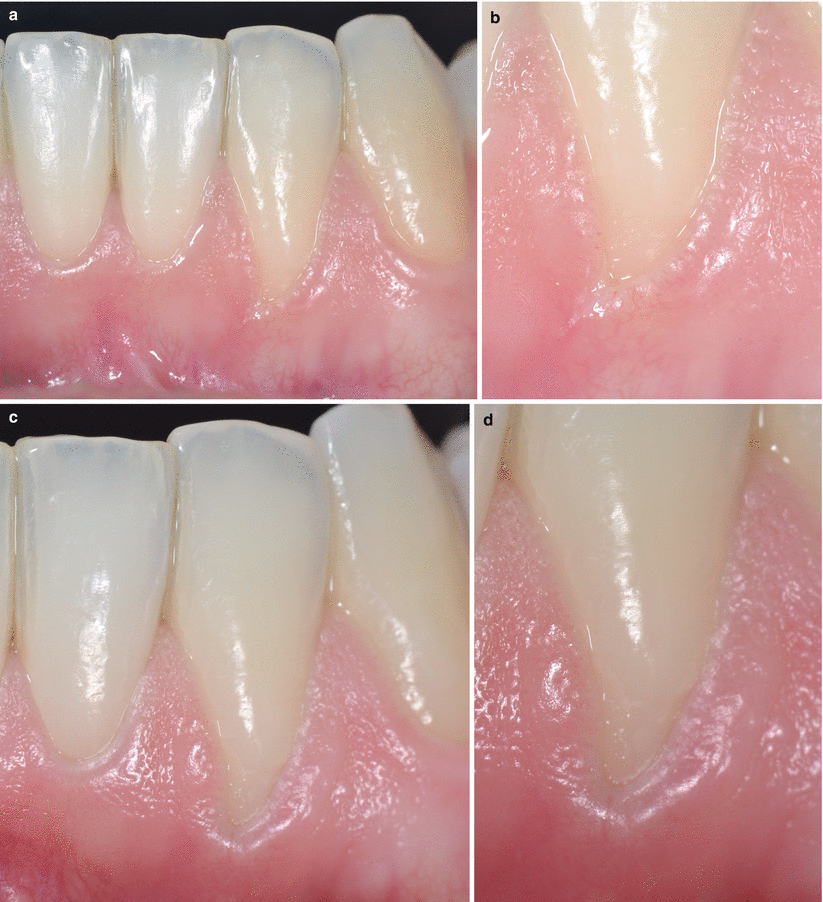

Fig. 3.7
Recession caused by traumatic toothbrushing (a), presence of a gingival fissure at the base of the defect (b); 60 days after proper toothbrushing (c), clinical improvements could be noted as well as the gingival fissure is no longer visible (d)
In general clinical terms, which results should I expect at private practice in terms of unusual healing response and long–term stability?
Unusual healing responses associated to the use of SCTG, such as root resorption [50], formations of cyst-like areas [51, 52] or bone exostosis [53], were described in the literature but involve a very restricted number of defects. In general terms, these unexpected outcomes do not weaken the safety and success of the connective graft. Additionally, some degree of creeping attachment (i.e. the coronal displacement of the gingival margin covering exposed root surfaces) may occur when subepithelial connective tissue grafts, and mainly free gingival grafts, are the choice of treatment [54]. For all of these unusual conditions, their occurrence cannot be anticipated.
The recent AAP paper [10] observed that at least 70 % of recession reduction can be anticipated 2 or more years after treating the recessions, but the number of defects showing 100 % defect coverage can drastically vary (up to 67.5 % of variation) depending on the type of surgical procedure and the follow-up period. For instance, Pini Prato and co-workers [55] described that “a coronal displacement of the gingival margin was observed in the SCTG + CAF treated sites, while an apical relapse of the gingival margin was found in the CAF-treated sites between the 6-month and 5-year follow-ups”.
It seems that the improvement on the keratinised tissue band, in terms of width and thickness gain (i.e. the concomitant root coverage and biotype change), is also responsible for keeping the stability of the results obtained with therapy. Overall, the use of subepithelial connective tissue grafts or enamel matrix derivatives in association to the coronal advancement of the gingival margin over the exposed root surface can provide the most stable outcomes. In contrast, coronally advanced flap alone and guided tissue regeneration were described as those procedures losing significantly more soft tissue [2, 4, 5, 8–10].
In addition, the elimination of the causative agent of the recession (e.g. traumatic toothbrushing, periodontal disease, etc.) and compliance with regular periodontal maintenance seem directly associated to long-term stability of results achieved with surgical therapy [56].
3.1.7 Role of Flap Preparation and Suture on Soft Tissue Root Coverage
Flap preparation and suture may not be underestimated during the surgical sequence. Recently, Burkhardt and Lang [57] highlighted some important issues on these surgical steps that demand special attention, and these are reproduced below:
1.
Flap preparation (design, advancement, adaptation and stabilisation) deserves special attention when split- or full-thickness flaps are placed on avascular surfaces (root surface, dental implants, restorations), mainly in sites presenting aesthetic demands [57].
2.
Tissue vascularisation guides flap design and favours graft incorporation (“the anatomical structures and their vascular supply are key issues”) [57].
3.
Flap lengthening regularly involves one or two vertical releasing incisions and a periosteal incision at the base of the buccal flap, given that the periosteum is primarily formed by dense collagen fibres (i.e. the use of a periosteal cut can release the flap tension and allow easy stretch of the elastic fibres of the adjacent mucosa) [57].
4.
Flap advancement may be limited by the length of the gingival recession to be covered, as well as greater extent of buccal flap advancement requires releasing incisions [57]. The use of verticals can lead to the formation of scars, alter mucosal texture and modify the anticipated aesthetic results. The use of flaps without vertical incisions (when applicable) leads to similar outcomes than the traditional approaches with vertical ones [57].
5.
Ideal flap preparation and releasing incisions should be based on the following: (1) incision of the sulcular area around the teeth and avoidance of marginal and para-marginal incisions, (2) the use of releasing incision as short and as medially as possible and (3) not performing releasing incisions on the buccal root prominences as the mucosal tissues covering the roots are usually thin and delicate [57].
6.
Since suture can interrupt the microcirculation of flaps and modify wound healing, these can remain as little as absolutely needed for primary stability (each individual case should be considered, and not a “standard” regime of a seven- to 10-day period, for instance) [57].
3.1.8 American Academy of Periodontology Recommendations on Soft Tissue Root Coverage [10]
Information on the inclusive evaluation performed by the American Academy of Periodontology at its recent workshop on Enhancing Periodontal Health Through Regenerative Approaches were used to answer specific important questions commonly made by clinicians in their daily practice, regarding the best possible choice of treatment modality to satisfy their patients’ needs [10].
Regarding the specific questions on soft tissue root coverage addressed by the AAP, the following can be considered during the decision-making process (as reported in the publication by Chambrone and Tatakis [10]):
-
“1. “What is the efficacy/effectiveness of root coverage procedures by the degree of recession?”[10] – The vast majority of the studies in the literature evaluated Miller Class I and II single recession defects” [10]. The following are all types of recession defects:
-
“(a) Miller’s [17] class I and II GR: [10] All RC procedures can reduce recession depth and improve clinical attachment without changing of probing depth of single or multiple recession-type defects, SCTG-based procedures provided the best outcomes for clinical practice due to their superior percentages of coverage and improved possibility of completely covering the defects, as well as significant increase of KT when compared to most of the other procedures. The combination of CAF with ADMG, EMD and CM also provided gains, many of them similar to SCTG-based procedures, and thus these may be considered as adequate substitute treatment approaches. Defects treated at mandible as well as at posterior sites (i.e. molars) can be safely and satisfactory treated as well. The final outcomes achieved seem to benefit by the use of magnification during the surgical procedures, but little evidence was available for analysis. Conversely, smoking may decrease the expected results of SCTG” [10].
-
“(b) Miller’s class III and IV: [10] For Class III defects, these may benefit by the use of RC procedures (at short-term) when SCTG-based procedures were used. Alternatively, EMD + CAF, ADMG + CAF and GTR + CAF can be used as graft substitutes. Overall, the marginal level of the gingival tissue of teeth adjacent to the GR seems to be the clinical reference point when planning and foreseen the expected results of Class III defects. Concerning Class IV recessions, the data from the limited number of case reports suggests that these defects may be improved after treatment, but the amount of root coverage cannot be anticipated, as well as restorative procedures may be necessary in order to reach the final expected esthetical outcomes” [10].
-
-
“2. “Which factors may influence the outcomes (i.e. smoking status and root surface conditions)?” For instance, “Is it possible to accomplish root coverage for teeth with non–carious cervical lesions, root caries or cervical root resorption?” [10] – It was clearly demonstrated that smoking may significantly decrease the effect of therapy, especially when SCTG-based procedures had been used. With respect to the surface conditions and from the limited number of studies available, it could be seen that non-carious cervical lesions, whether restored with composites/ionomer materials or not, may be safely treated by SCTG + CAF and CAF. Moreover, there is no evidence on the optimal timing for non-carious cervical lesions restoration (before/during RC procedure or after wound healing). For teeth previously restored or presenting caries, there is some evidence indicating the positive effects of treatment of these areas by RC procedures, but for both conditions there is a need of removal of old restorations/caries prior to the surgical therapy (i.e. the need for a “clean/disease-free root surface”) [10]”.
-
“3. “What is the anticipated success and attachment apparatus of root coverage enhancements with autogenous grafts compared to alternative methods and materials?” [10] – As already mentioned, SCTG-based procedures seem to be the best option in terms of clinical outcomes and cost-benefit ratio. On the other hand, the use of matrix grafts (ADMG and CM) and EMD may be used as safe substitutes for autogenous grafts in patients with great demands of donor tissue (e.g. patients with multiple recession type defects) or patients who do not want to be submitted to a secondary surgical procedure at the palatal vault. Histologically, most of the techniques may result in the formation of a long junctional epithelium (over the previously exposed root surface) and connective tissue attachment with fibers parallel to the root surface. Diversely, GTR and EMD procedures can lead to partial periodontal regeneration (i.e. formation of new cementum, alveolar bone and periodontal ligament inserted in the new formed cementum) [10]”.
-
“4. “What are the long term and short term advantages of root surface biomodification? [10]” – The long-term outcomes (≥24 months) presented in the literature indicate that SCTG-based procedures and EMD + CAF may provide superior outcomes than CAF, as well more stable results. Overall, great part of the root coverage achieved at short-term may be maintained long-term. The use of root modification agents or other surface biomodification procedures did not provide superior gains on clinical outcomes, either short- or long-term, than those expected for procedures performed without such agents [10]”.
-
“5. “What are the relative risks from a patient’s viewpoint with the different approaches to root coverage procedures? [10]” – Regarding patient-centered outcomes, all RC procedures were considered safe and effective for attaining root coverage and satisfactory esthetics. Data on root hypersensitivity is still scant, but recent data suggests the positive impact of RC treatment on such an outcome. Moreover, a small percentage of patients may experience post-operative bleeding, swelling and pain. It could be considered that patients seem to prefer procedures that involve only one surgical site when considering these early post-operative adverse effects, but these were not associated with the final esthetic/functional outcomes [10]”.
-
“7. “Do we have evidence for innovation when treating thin and thick biotypes with existing treatment modalities? [10]” – SCTG, ADMG and CM can positively change thin periodontal biotypes of recession sites to thick periodontal biotypes. As reported within long-term studies, patients treated with graft procedures (and their consequent biotype improvement) benefited by more stable outcomes and less recession recurrence. Overall, it seems reasonable to suggest that biotype modification (i.e. thin to thick biotypes) should be considered when planning and treating recession-type defects due to the positive more stable long-term outcomes reported [10]”.
3.1.9 Clinical Concluding Remarks: “What Should I Expect of the Treatment of Gingival Recession Defects?”
The treatment of a gingival recession is safe and leads to significant clinical reductions in recession depth and attachment level within Miller Class I and II defects. Class III recession may be benefited as well, but the amount of coverage will be based on the amount of interproximal tissue lost (usually the amount of root coverage expected is based on the position of the gingival margin of the adjacent teeth).
Altogether with the improvements on the aesthetic condition, a decrease of dentin hypersensitivity and prevention of caries/cervical lesion over the exposed root surface may be expected. Both single and multiple recessions may be benefited by periodontal plastic surgery, but apart from the type of procedure or recession, the rationale for treatment should be focused on the clinician’s knowledge and patient-centred outcomes (e.g. aesthetic assessment, functional limitations, discomfort, root sensitivity and preferences). Overall, a small percentage of patients may experience early post-operative bleeding, swelling and pain, but these do not modify the final aesthetic/functional outcomes. Moreover, it should be noted that the amount of vascularisation adjacent to a root surface is crucial when a flap is moved over avascular sites (root surface); consequently, it is adequate to extend the base of the pedicle (flap) to improve the local blood supply during early healing [56].
Likewise, flap stabilisation and suture coronal to the CEJ are important and desirable too [56], but other local conditions should be considered during the decision-making process (choice of best procedures), such as periodontal conditions (lack of biofilm inflammation), recession anatomy (classification, depth and width), anatomy of adjacent soft tissue (thickness and presence of keratinised tissue) and tooth/root conditions (tooth position and root prominence) [56].
Critical Summary of the Results of Systematic Reviews
Systematic reviews conclusions: All periodontal plastic surgery procedures are safe and can lead to clinical significant gains in gingival recession depth and in clinical attachment level [2–10].
Summary of the reviews and critical remarks: Most of the research on the treatment of recession-type defects highlights the positive effect of treatment in terms of defect- and patient-centred outcomes, such as the amount of root coverage and aesthetical improvement. The incidence of adverse effects, such as discomfort with or without pain, is very low, and when present, these may occur at the early phase of healing. Additionally, such events do not lead to changes in the final anticipated functional (root hypersensitivity) and/or aesthetic outcomes [2–10].
Evidence quality rating/strength of recommendation (ADA 2013) [58]: Strong – evidence strongly supports this intervention (i.e. treatment of recession-type defects).
3.2 Laterally Positioned Flap-Based Procedures
3.2.1 Historical Note
Described in 1956 by Grupe and Warren [59], this technique was based on the preparation of a full-thickness pedicle flap using the soft tissue (gingiva and mucosa) of a tooth adjacent to the gingival recession and its positioning/rotation over the exposed root surface in order to cover it. Despite its promising results on the restitution of the lost soft tissue and aesthetic improvement, loss of gingiva at the donor site was frequent as well.
Almost a decade later, modifications to the original technique (including papillary tissue-based procedures) were proposed to reduce the adverse effects related to the donor sites, as well as to improve the coverage of the recipient site. Between 1964 and 1968, several groups of clinicians/researchers proposed the following changes:
-
Staffileno [62] suggested the use of a partial-thickness flap created by sharp dissection to maintain the donor bed covered by periosteum.
-
Friedman and Levine [63] improved the area of the flap by increasing its width to include two adjacent teeth and thus to reduce the exposure of the facial alveolar ridge surface.
-
Goldman et al. [64] recommended the use of mixed flap capable to cover both the donor and recipient beds. In this technique, the recipient site should be covered with the full-thickness portion of the flap, whereas the donor area should be covered by the split-thickness flap to prevent for any bone exposure.
-
Pennel et al. [65] introduced the use of an oblique incision to improve the area of coverage and to facilitate the accommodation of the flap, by permitting the concomitant lateral and coronal positioning/moving of the flap.
-
Grupe [66] modified his former technique, by leaving a narrow band (1 mm) of marginal gingival tissue at the donor tooth to prevent for tissue loss at this area.
-
Ariaudo [67] extended the flap to four or more adjacent teeth.
Furthermore, other subsequent modifications and standardisations of technique by Bjorn [69], Smukler [70], Patur [71], Guinard and Caffesse [72], Leis and Leis [73], Bahat et al. [74], Milano [75] and more recently Zucchelli et al. [76] were proposed either to improve the characteristics of the flap or to provide better protection to the donor areas. In addition, with the development and results of other techniques after the mid-1980s, especially those involving the use of subepithelial connective tissue grafts, soft tissue substitutes and guided tissue regeneration combined with coronally advanced flap procedures, the scientific community seems has lost interest in the evaluation of LPF.
3.2.2 Type of Defect to Be Indicated
Treatment of localised Class I or II GR [30] (Class III may be benefited by this procedure) adjacent to the donor teeth presenting a width of attached keratinised tissue (KT) of at least 2 mm and thick periodontal biotype
3.2.3 Type of Defect not to Be Indicated
Treatment of localised or multiple GR adjacent to the donor teeth presenting a width of attached keratinised tissue (KT) <2 mm and thin periodontal biotype
3.2.4 Basics of the Surgical Sequence
Following local anaesthesia, the recipient site should be prepared to accommodate the LPF. An incision is made around the recession defect creating a 1-mm-wide gingival collar. After this, the collar is excised, and two vertical incisions are made at the ends of the gingival recession and extended to the alveolar mucosa. These incisions are then connected by a horizontal incision and the recipient site is de-epithelialised. In the donor site (i.e. adjacent tooth), a horizontal submarginal incision is made at the mesial end of the gingival recession and extended in the mesial-distal direction.
A vertical releasing incision should be made at the end of the horizontal incision and extended to the alveolar mucosa. It is important to highlight that the interdental papilla distal to the defect should be preserved as much as possible. After that, a full- or partial-thickness flap (depending on the type of LPF-based technique used) is raised with blade dissection, and a 3-mm-wide collar of intact gingiva should be left undisturbed around the donor tooth. After flap incision and dissection, the exposed root surface should be thoroughly, but carefully, planned with hand curettes and/or finishing burs. At this stage, root modification agents may be used, but no additional clinical benefits should be expected. The planned root surface is rinsed with saline; the flap is laterally positioned at the level or beyond (coronal) of the cemento-enamel junction and sutured by 5-0 or 6-0 nylon/Teflon sutures (Fig. 3.8). It is also essential to note that the flap should be passively adapted over the recipient site (i.e. it must remain stable at that position even without sutures), so all muscle inserts located on the internal side of the flap should be removed leaving the flap with no tension. Subsequently, a non-eugenol periodontal dressing may be placed over the donor sites. The dressing and sutures are removed 14 days after surgery.
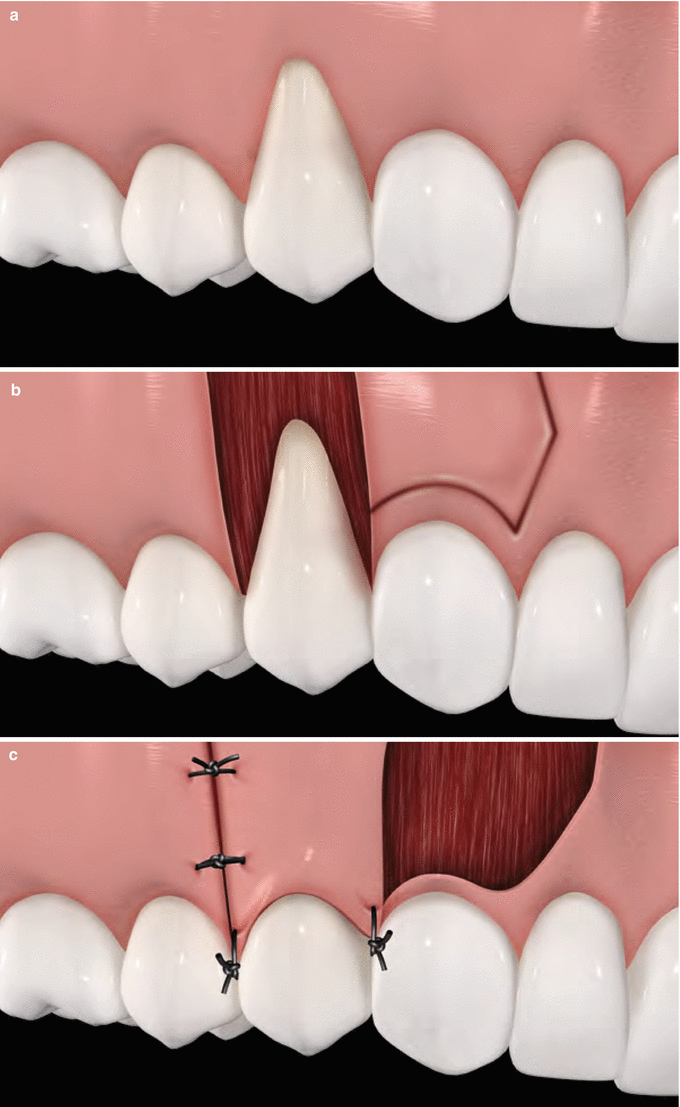

Fig. 3.8
Laterally positioned flap. Baseline (a), recipient bed preparation and delimitation of the flap over the donor bed (b), partial-thickness flap positioned and sutured over the recipient bed (c)
In addition, patients should be instructed not to brush the tooth in the treated area, as well as they are prescribed 0.12 % chlorhexidine gluconate and instructed to rinse gently twice a day for 2–3 weeks or until safe and comfortable toothbrushing can be performed. Overall, analgesics, anti-inflammatory drugs and/or systemic antibiotics are prescribed if needed, as well as no adverse effects are expected in the donor or recipient sites.
3.2.5 Clinical Remarks: Implications for Practice and Clinical Decision-Making on Soft Tissue Coverage
The use of LPF may lead to significant reduction in recession depth and clinical attachment level gain for Miller Class I and II localised defects, as well as a great part of the root coverage achieved at short term may be maintained long term. Creeping attachment may occur in donor and recipient sites, but the amount of coronal displacement of the gingival tissue cannot be defined. By requiring only one surgical site, its use is easier and less painful, and the chair time is smaller than SCTG, which, in practical terms, may be better indicated for less experienced clinicians. On the other hand, in terms of achieving complete root coverage, this technique is less effective than SCTG-based procedures, as well as its use is limited to localised areas, with an adjacent thick periodontal biotype. Consequently and despite their clinical advantages, the use of LPF is better suitable when SCTG could not be used (Figs. 3.9, 3.10, 3.11, 3.12, 3.13, 3.14 and 3.15).
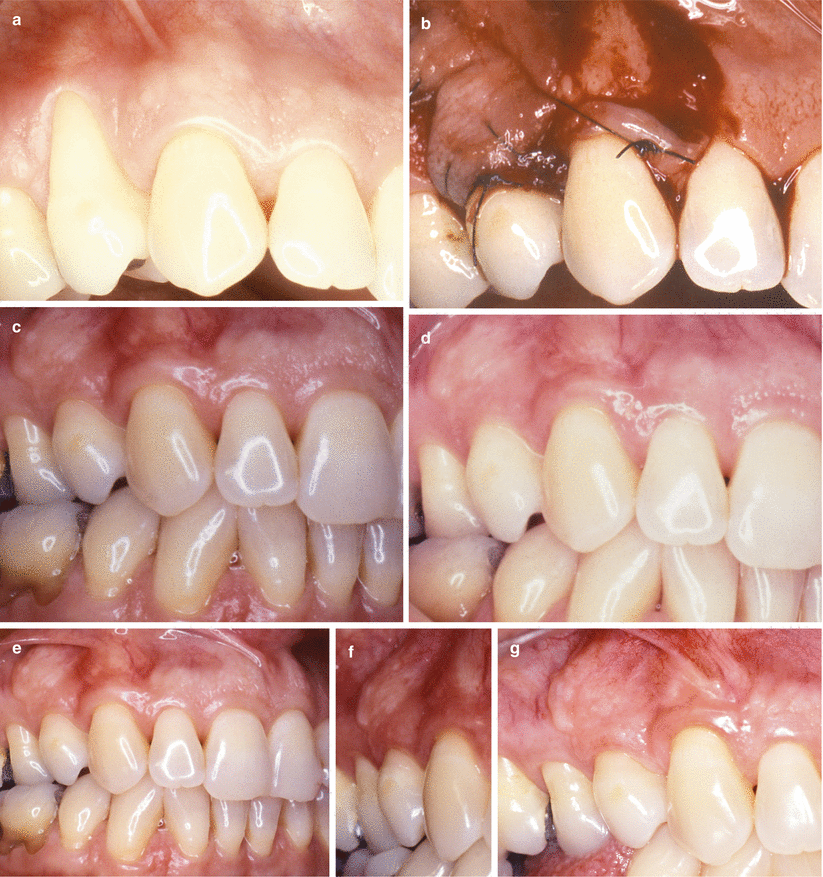
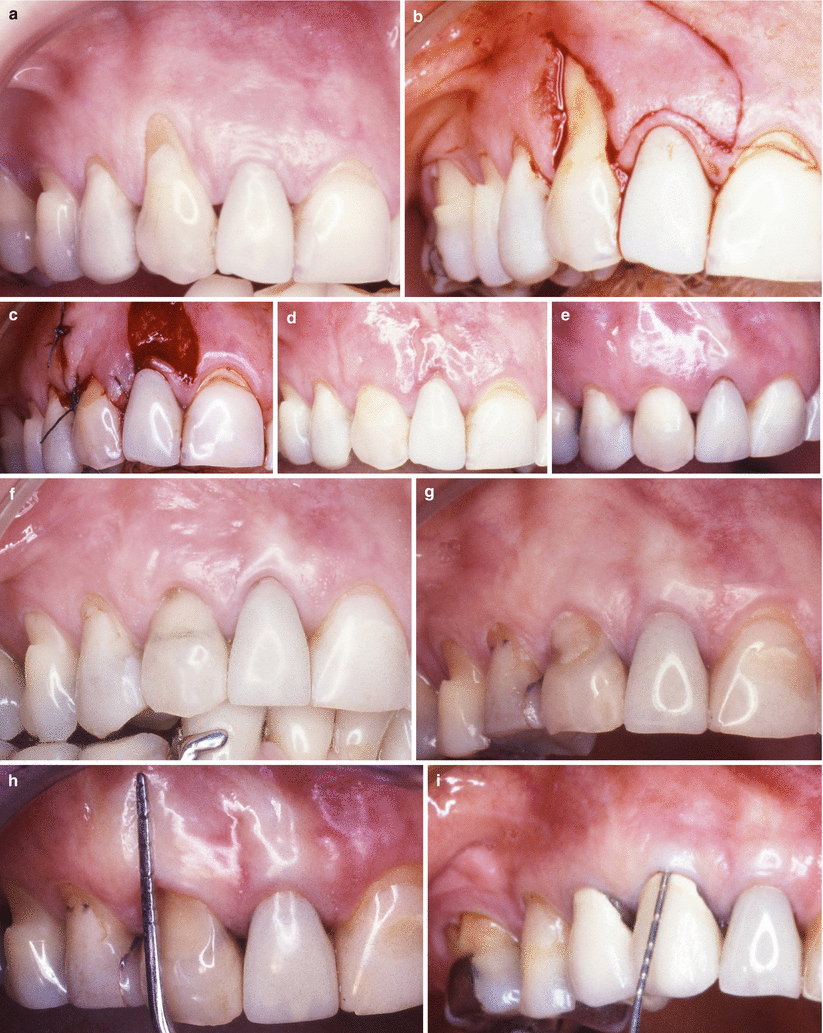
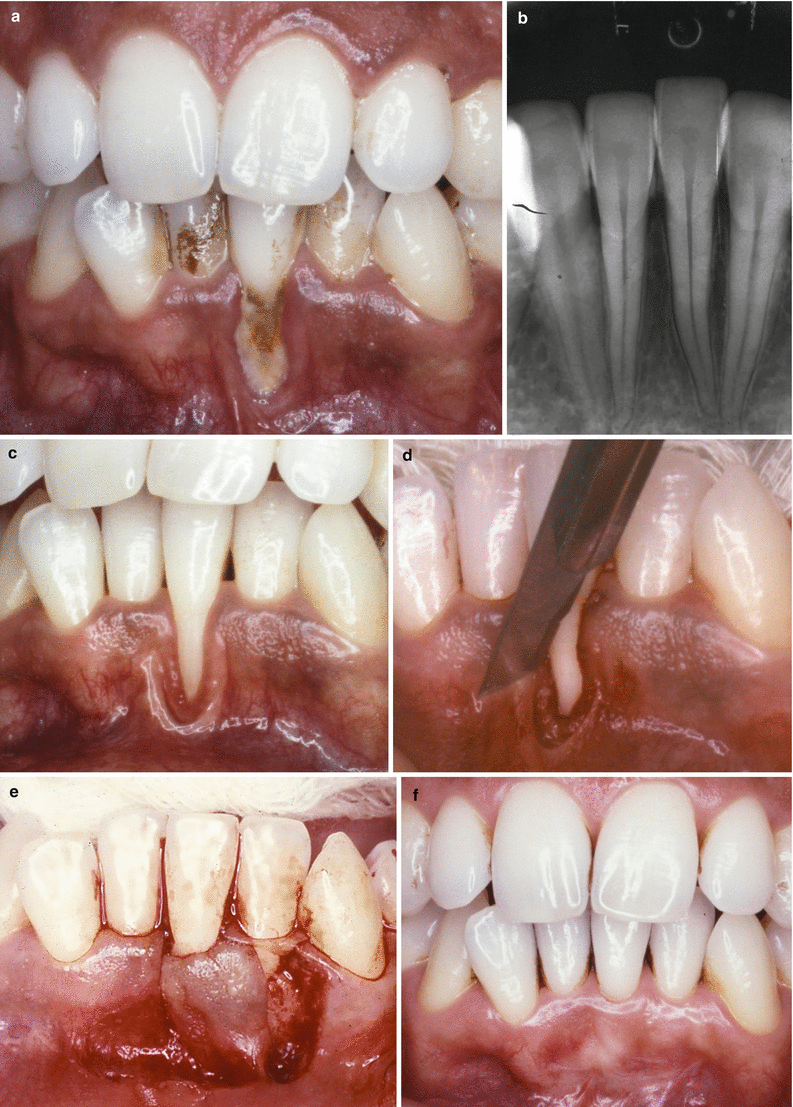
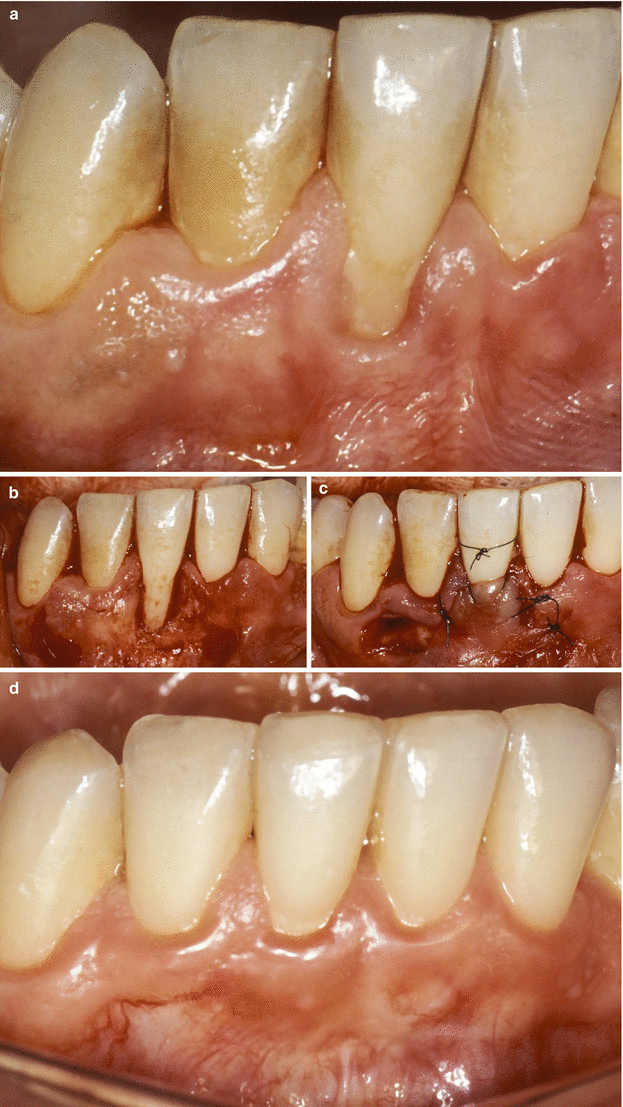
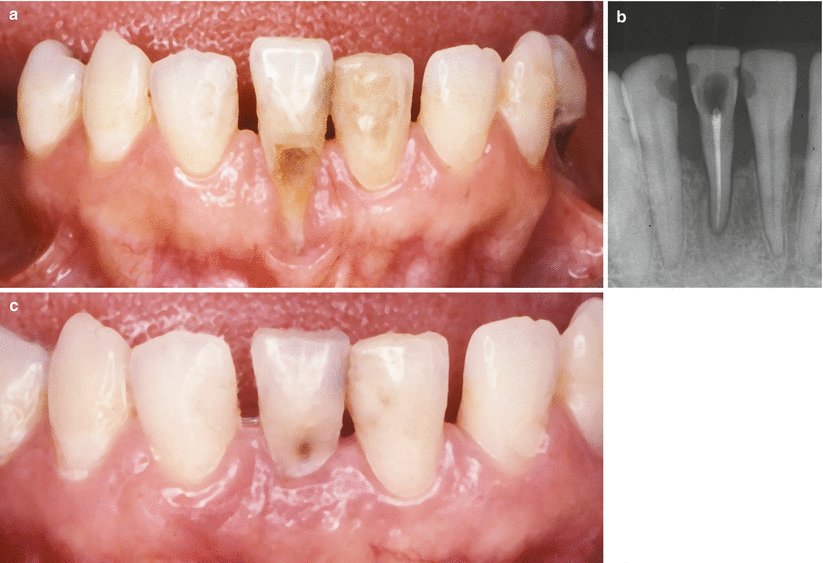
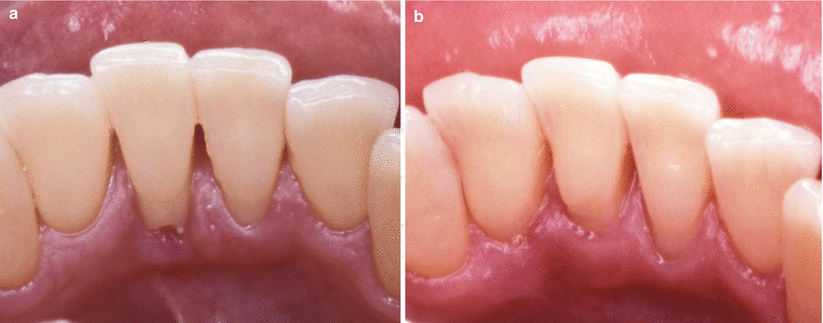
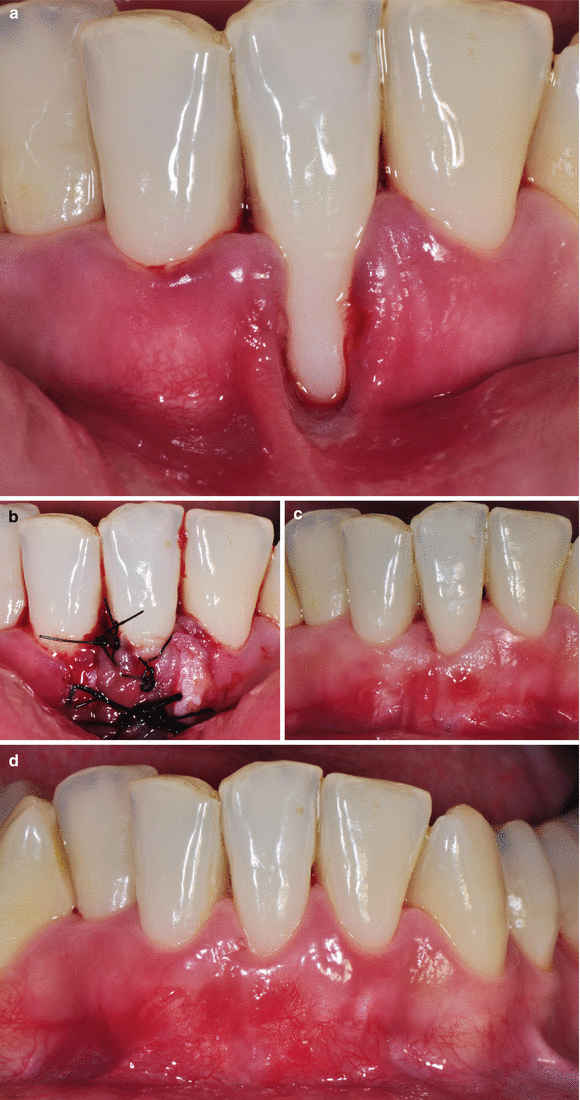

Fig. 3.9
Case I. (a–g) Class I gingival recession on tooth 14. Baseline (a) flap (13) positioned and sutured over the recession (b), 4-year follow-up (c, d), 9-year follow-up (e), 16-year follow-up (f, g)

Fig. 3.10
Case II. (a–i) Class I recession on tooth 13. Baseline (a). Removal of restoration, incisions for flap and gingival collar delimitation – tooth 12 (b), flap laterally positioned and sutured (c), 1-month follow-up (d), 12-month follow-up (e), 8-year follow-up (f), 15-year follow-up (g), long-term stability 15 years the procedure after (h), 24-year follow-up (new metal ceramic crowns were installed at the donor and recipient teeth 7 years prior this evaluation)

Fig. 3.11
Case III. (a–f) Gingival recession in smoking patient (>20 cigarettes per day) on tooth 31. Baseline – recession developed due to the association of muscle insert close to the gingival margin, dentinary hypersensitivity and biofilm accumulation (a, b), clinical condition after the basic procedures (c). Horizontal incision around the recession (d), flap positioned over the exposed root (e), 8-year follow-up (f)

Fig. 3.12
Case IV. (a–d) Class II gingival recession on tooth 41 – smoking patient (20 cigarettes per day). Baseline (a), flap delimited (b), flap laterally positioned and sutured (c), 7-month follow-up (d)

Fig. 3.13
Case V. (a–c) Class III gingival recession at tooth 41. Baseline (a), baseline radiograph (b), 2-year follow-up (c)

Fig. 3.14
Case VI. (a, b) Lingual Class II recession associated to external root resorption – tooth 41. Baseline (a). 4-month follow-up (b)

Fig. 3.15
(a–d) Class III gingival recession adjacent to a lip frenum (prior to orthodontic treatment) – tooth 31. Baseline (a), double papilla flap positioned and sutured over the exposed root surface (d), 1-month follow-up (c), 4-month follow-up (d)
Critical Summary of the Results of Systematic Reviews
Summary of the reviews and critical remarks: Most of the research available for this procedure relies on studies performed at the 1970s and early 1980s (the use of RCTs to test root coverage relates to the early 1990s). Of the most recent literature, four studies (one of them a RCT) show that:
-
Santana et al. [77] – MRC of 95.5 % and CRC of 83.3 % (15/18) at 6 months
-
Ricci et al. [78] – MRC of 61.9 %; sites with CRC of 15 % (3/20) at 12 months
-
Zucchelli et al. [76] – MRC of 96.0 % and CRC of 80 % (96/120) at 12 months
-
Chambrone and Chambrone [49] – MRC of 93.8 % and CRC of 62.5 % (20/32) at 24 months
Evidence quality rating/strength of recommendation (ADA 2013) [58]: Weak – evidence suggests implementing this intervention after alternatives have been considered.
3.3 Coronally Advanced Flap-Based Procedures
3.3.1 Historical Note
Historical reports proposing the advancement of the gingival marginal tissue over an exposed root surface were published initially in 1907 (by Harlan) and 1912 (by Rosenthal) in the USA [79]. However, Norberg [80] may be considered as the first author to describe a clinically viable technique involving the use of the coronally advanced flap (CAF).
At the end of the 1940s, different modifications and improvements of the CAF were also proposed [81–89]. Of them, the following surgical variations deserve reasonable attention:
-
Tarnow [87] described a new flap design, the semilunar coronally advanced flap, to be used in areas presenting a band of keratinised tissue. According to the publication, areas lacking keratinised tissue should be treated with an FGG 2 months before the coronal advancement of the flap.
-
Zucchelli and de Sanctis [88] presented changes to the CAF procedure to improve the predictability of multiple recession-type defects. The authors proposed the use of a horizontal incision and a split-full-split approach to create an “envelope flap” with no releasing incisions in order to preserve the maximum soft tissue thickness above the root exposure. This incision should be extended laterally to include at least one adjacent tooth of each side of the GR.
3.3.2 Type of Defect to Be Indicated
3.3.3 Type of Defect Not to Be Indicated
Treatment of localised or multiple GR presenting a width of attached keratinised tissue (KT) <2 mm and thin periodontal biotype.
3.3.4 Basics of the Surgical Sequence
Following local anaesthesia, an intrasulcular incision is made at the tooth presenting the gingival recession, and two vertical incisions are made at the ends of the gingival recession and extended to the alveolar mucosa. For procedures not involving releasing incisions [88], the intrasulcular incision should be extended to one to two teeth adjacent of the recession to allow advancement of the flap over the exposed root surface without tension. Subsequently, a partial-thickness flap is elevated by sharp dissection, the interdental papilla are de-epithelialised and the exposed root surface should be thoroughly, but carefully, planned with hand curettes and/or finishing burs. Likewise to all root coverage procedures, at this stage, root modification agents may be used, but no additional clinical benefits should be expected. The planned root surface is rinsed with saline; the flap is coronally advanced at the level or beyond of the cemento-enamel junction and sutured by 5-0 or 6-0 nylon/Teflon sutures (Figs. 3.16 and 3.17
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


