Fig. 4.1
Pain during early healing of donor sites of free gingival grafts caused by the exposure of the connective tissue layer of palatal gingival tissue (a). Swelling during early phase of healing of sites treated with subepithelial connective tissue grafts (b). Bleeding of a donor site of subepithelial connective tissue graft even after suture (c)
For instance, in a large practice-based study [8] considering the use of free gingival grafts (FGGs), subepithelial connective tissue grafts (SCTGs), and acellular dermal matrix grafts (ADMGs) for Class I and II root coverage, moderate to severe pain and swelling were the most significant adverse events, but less than 6 % of the sample experienced moderate or severe bleeding, and all of them were associated with the use of autogenous grafts [8]. The use of FGG was reported as the most painful procedure, followed by SCTG and ADMG. Additionally, longer chair-time procedures were straight associated to postoperative discomfort, such as pain and swelling, as well as the rate of pain and bleeding where superior for FGG than for SCTG [8]. On the other hand, it should be also noted that the incidence of infection (less than 1 %), bleeding (3.0 %), swelling (5.4 %), and pain (18.6 %) after the use of SCTG can be considered low to moderate [9].
It is also important to highlight that despite the possible occurrence of some adverse events related to the treatment with SCTG (i.e., development of cyst-like areas [10, 11], root resorption [12, 13], or bone exostosis [14]), these were restricted to a very limited number of cases and cannot per se undermine the safety/success of autogenous grafts. Regarding the development of bony exostosis (i.e., unknown etiology of peripheral localized benign bone overgrowth, with a base continuous to the original bone and which seems to have a nodular, flat, or pedunculate protuberance) [15], these were also reported at sites where free gingival grafts (FGG) have been used to increase the amount of keratinized tissue (Fig. 4.2a–c). The reduced base of literature suggests that periosteal trauma/fenestration is probably the primary main-causing agent linked with exostosis development in grafted sited by FGG [16]. Likewise, and as explained in Chap. 3, additional reductions in the recession depth may occur after healing of the treated sites due to creeping attachment (Fig. 4.3a–i).
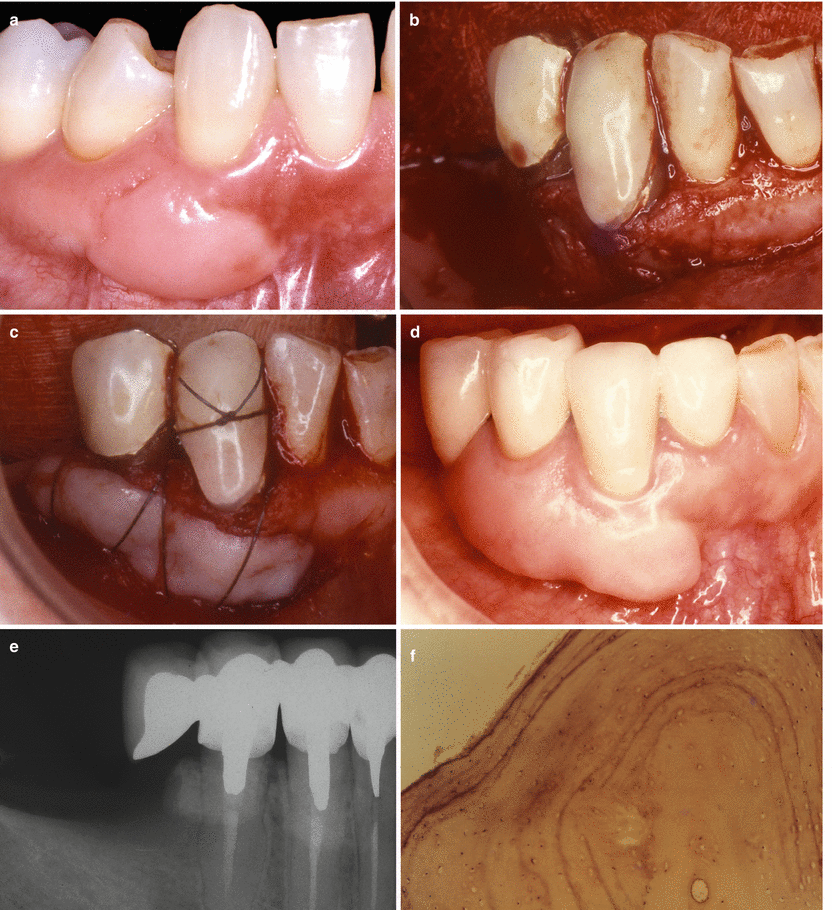
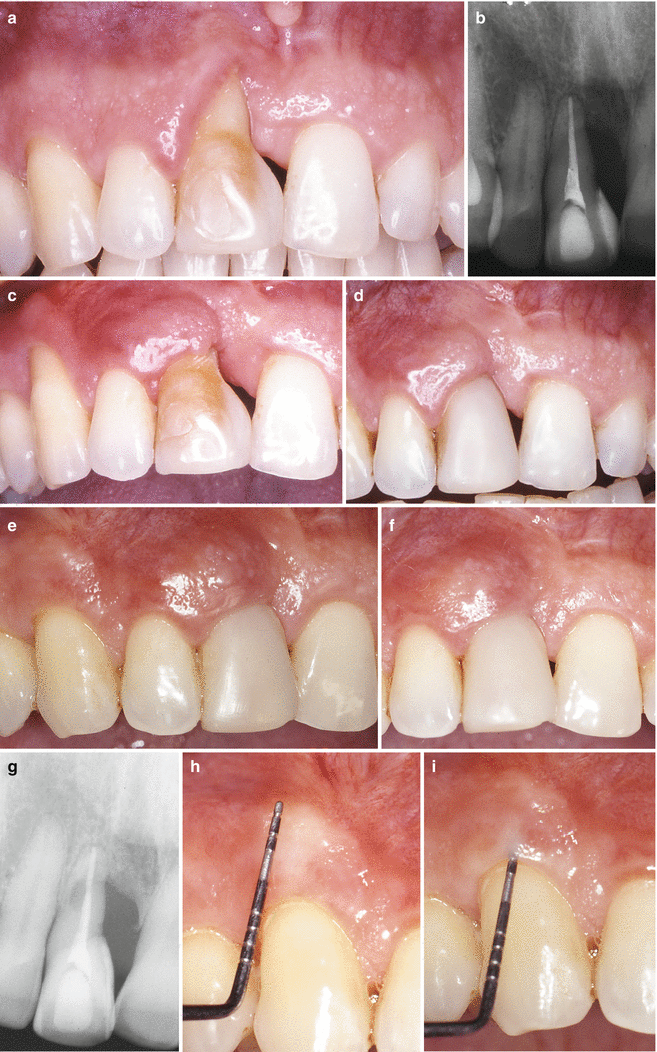

Fig. 4.2
Bone exostosis developed 5 years after frenectomy + periosteal fenestration + free gingival graft (a). Bone exostosis developed 15 years after a free gingival graft (b–f): accidental periosteal fenestration at teeth 44 & 43 (b), graft sutured (c), pronounced overgrowth at the graft site (d), increased radiopacity during radiographic exam (e), and very dense lamellar bone formation at graft site compatible to the exostosis diagnosis (f) (Figures originally published at Chambrone and Chambrone [16])

Fig. 4.3
(a–i) Class IV – Gingival recession in a heavy smoker patient >20 cigarettes a day (a),, baseline radiography (b), 4 months after a laterally positioned flap – presence of gingival recessions at tooth 13 (donor site) and 11 (recipient site) (c, d). 8 years follow-up – clinically relevant creeping attachment was evident on the donor and recipient sites (e, f) – 8 years follow-up radiography (g). Amount of creeping attachment achieved 8 years after surgery (h). Probing depth compatible to a health condition (i) (Figures originally published at Chambrone and Chambrone [28])
In addition, it has been clearly demonstrated that all periodontal plastic surgical procedures when properly performed are safe, as well as only a reduced number of patients can experience postsurgical complications (i.e., pain, swelling, or bleeding) or unusual healing outcomes [1–7].
4.1.2 Patient-Centered Outcomes: “The Role of a Patient as the Clinician Coworker”
As reported previously, it can be argued that patients might prefer procedures involving only one surgical site when those potential early postoperative complication/adverse effects are taken into account; however, data included in previous systematic reviews also showed that these outcomes were not associated with the final esthetic/functional outcomes [1–7].
With respect to the influence of root coverage on cervical dentin hypersensitivity and quality of life of patients, a recent study on the treatment of Class I GRs treated with SCTG + CAF demonstrated that thermal [cold] and evaporative [air blast] stimuli can be significantly reduced 3 months postsurgery [17]. Yet, the treatment of recession defects (independent of the amount of root coverage achieved and the treatment approach used) positively influenced patients’ oral health-related quality of life [17, 18].
Concerning patients’ perceptions and requests for treatment and postsurgical satisfaction, it has been recently considered that perception of buccal defects by patients should be taken into consideration during decision-making [19]. Most of the patients don’t mind the presence of GR, as well as considered such defects asymptomatic in nature and with no esthetical and/or functional relevance (73 %) [19]. In addition, 2/5 of the patients’ requests for surgical correction of the defects occurred because of esthetic concerns and only 1/5 as a result of cervical dentin hypersensitivity [20].
Taken into account the patient-reported outcomes on esthetical and functional demands, it has been suggested that most of the graft, flap, and soft tissue substitutes provide similar color/texture of the tissues, except for the use of free gingival grafts (Fig. 4.4a–h) [1–7]. On the other hand, less traumatic procedures, such as CAF without vertical incisions, seem to offer better postoperative course during early healing [7].
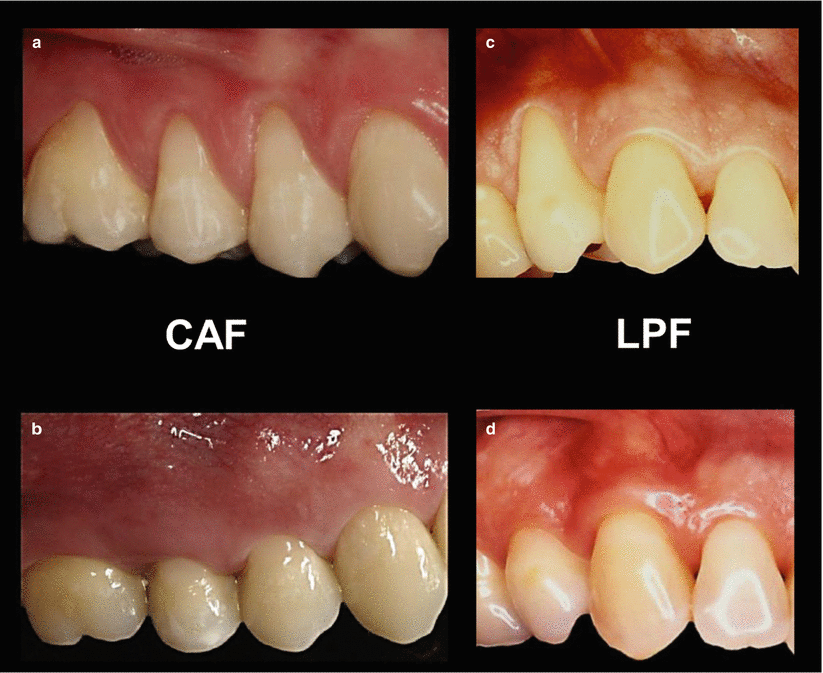
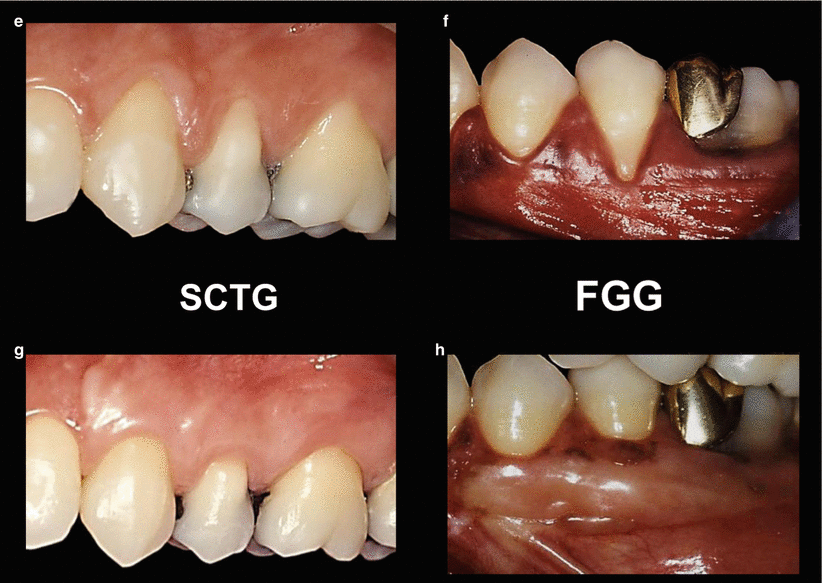


Fig. 4.4
Best color match and esthetics – flaps versus grafts. CAF coronally advanced flap (a, b), LPF laterally positioned flap (c, d), SCTG subepithelial connective tissue grafts (e, f), FGG free gingival grafts (g, h)
4.1.3 Clinical Concluding Remarks: “To Treat or Not to Treat Recession-Type Defects and Sites Lacking Keratinized Tissue”?
In clinical terms, it is clear that soft tissue augmentation procedures are safe and very well accepted by patients. The potential complications and adverse effects associated with such procedures are restricted to a limited number of cases and cannot per se undermine the safety/success of autogenous grafts. However, it is also clear that less traumatic procedures, with less chair time and involving only one surgical site, are preferred by most patients. These preferences are associated only with the surgical technique chosen and to some degree of pain, swelling, and/or bleeding some patients may experience at the early phases of healing of donor sites of autogenous grafts, but they do not have any impact on the final esthetical/functional outcomes or even amount to contraindications for treatment.
It is clear that less traumatic procedures, with less chair time and involving only one surgical site, are preferred by most patients. Independent of such preference, most of the treated patients considered esthetics as their main concern and, in their great majority, the final outcomes of the performed surgical procedure (irrespective of inclusion of one or more surgical sites) fulfilled their personal expectations. However, differences among patients’ and clinicians’ expectations and the manner they consider the success of treatment may be accounted as well. Apart of such preferences, most of the treated patients considered esthetics as their main concern and, in their great majority, the final outcomes of the performed surgical procedure may fulfill patients’ personal expectations [1–7].
Critical Summary of the Results of Systematic Reviews
Systematic reviews conclusions: All periodontal plastic surgery procedures are safe, as well as no relevant detrimental effects have been demonstrated associated with the main RC employed in daily practice [1–7]. On the other hand, there is not enough evidence to support or refute the assumption that RC may decrease hypersensitivity [17].
Summary of the reviews and critical remarks: Most of the research on the treatment of recession-type defects highlights the positive effect of treatment in terms of defect- and patient-centered outcomes. The incidence of adverse effects, such as discomfort with or without pain, is very low, and when present, these may occur at early phase of healing. Additionally, such events do not lead to changes in the final anticipated functional (root hypersensitivity) and/or esthetical outcomes [1–7].
Evidence quality rating/strength of recommendation (ADA 2013) [21]: Strong – Evidence strongly supports providing these interventions (i.e., treatment of recession-type defects and keratnized tissue augmentation)
4.2 The Use of Soft Tissue Substitutes
4.2.1 Historical Note and Types of Substitutes
The use of soft tissue substitutes for root coverage procedures, treatment of alveolar ridge deformities, and augmentation of the keratinized tissue band has been broadly proposed since the late 1990s. Specifically to the potential materials capable to be used in periodontal and peri-implant plastic surgery, allogenic and xenogeneic grafts have been developed [1, 3–7], and the main commercial brands are depicted below:
-
The Alloderm® Regenerative Tissue Matrix (BioHorizons IPH Inc., Birmingham, AL, USA) or ADMG is the most studied soft tissue substitute since its development in 1994. It is an allograft material obtained from a human donor skin tissue through a process that removes its cell components (in order to remove potential sources of disease transmission and immunologic reaction), while preserving the remaining bioactive components and the extracellular matrix, which is subsequently freeze dried [22–24]. According to its manufacturer, it “supports tissue regeneration by allowing rapid revascularization, white cell migration and cell population – ultimately being transformed into host tissue for a strong, natural repair.”
-
The Puros® Dermis Allograft Tissue Matrix (Zimmer Dental Inc., Carlsbad, CA, USA) is an allograft material (i.e., sterile dehydrated dermis from donated human) that “retains the natural three-dimensional collagen structure/matrix and mechanical properties of native dermis,” as well as it “provides a natural collagen scaffold to support replacement by new endogenous tissue.”
-
The PerioDerm™ Acellular Dermis Soft Tissue Matrix (DENTSPLY International, Inc., Tulsa, OK, USA) is a freeze-dried allograft material derived from donated human skin, and it “is minimally processed to remove epidermal and dermal cells (viable cells and antigens) to minimize the risk of rejection and inflammation of the surgical site while preserving the extracellular matrix (the framework for cellular infiltration and vascularization).” It is also described by “supporting the migration of host cells from wound margins and surrounding tissues.”
-
The Geistlich Mucograft® (Geistlich Pharma AG, Switzerland) is a purified, nonantigenic pure porcine collagen bilayer matrix. As described by its manufacturer, one of the layers is compact (“compact collagen fibers that protect against bacterial infiltration in open healing situations and allow tissue adherence as a prerequisite for favorable wound healing”), while the other is spongious (“a thick [2.5–5.0 mm], porous collagen spongious structure that should be placed in contact with the host tissue”).
In addition, the association of other biomaterials has been used to improve the outcomes of CAF-based procedures. Of them, the porcine enamel matrix derivative protein (EMD – Straumann® Emdogain, Straumann Holding AG, Basel, Switzerland) has been used for more than 10 years as an interesting and safe approach. Despite the additional costs related to the purchase of this biomaterial, it has been demonstrating superior outcomes in recession depth reduction, concomitant clinical attachment level, and keratinized tissue width gain when compared to CAF alone, as well as in regenerating part of the periodontal tissues at recession defects [1, 3–7].
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


