The aging United States population living in the new millennium has dental needs that are very different and more complex than those experienced by previous older adult cohorts during the twentieth century. The type of dental care to be provided for older Americans goes way beyond emergency care, extractions and denture care. Dental caries is still clearly a public health problem for subgroups of older Americans, such as those of lower socioeconomic status, with dementia, who are homebound and who are institutionalized. These are also the subgroups experiencing greater barriers to accessing dental care. Stakeholders, including dental professionals and the dental benefits industry, need to work together to develop innovative dental financing programs that will increase older Americans access to dental care.
Demographics of the aging population and epidemiology of their oral health
In the twentieth century, dramatic changes occurred with regard to health and disease, longevity, and mortality in the United States population. We have become an aging society. In 1900, 4% (3.1 million persons) of the United States population was aged 65 years or older and by 2005 it had increased to 34.3 million persons or 12.4% of the population, a more than tenfold increase . The fastest growing sector of older adults is of those 80 years or older. Heterogeneity among persons 65 years of age or older is probably greater than at any other time period in the life span . The challenges of life make older adults different from each other; yet all too often people aged 65 and older are considered as one homogeneous group when programs are planned.
Older adults are a complex combination and expression of their individual genetic predispositions, lifestyles, socialization, and environments; these factors affect health beliefs and impact health behavior. To treat an older adult, dentists must understand the cultural, psychologic, educational, social, economic, dietary, and chronologically related experiences that may have influenced that older person’s life. Oral health is influenced by similar factors and is the accumulation of an individual’s life experiences with dental care, as well as with caries, periodontal disease, and iatrogenic disease. Oral status reflects a history of the older person’s behavioral attitudes and expectations for their own oral health. The skills, attitudes, and philosophies of the various dentists that persons may have encountered in their life spans will also affect oral status . The oral health care of any of these older adults is termed “geriatric dentistry” and includes—but is not limited to—the diagnosis, treatment, and prevention of caries and periodontal disease, as well as oral mucosal diseases, head and neck pain, salivary dysfunction, and impaired chewing, tasting, and swallowing .
Older adults in the past comprised a relatively small proportion of the population; the majority of these people were edentulous and used dental care infrequently, and then only when previous unmet needs could no longer be ignored . However, there is now adequate evidence to show that a new, older dental consumer has emerged, who is better educated, more politically aware and, more importantly, has some remaining natural teeth. Thus, the aging United States population living in the new millennium has dental needs that are very different and more complex than those experienced by previous older adult cohorts during the twentieth century. It is no longer appropriate to equate geriatric dental care with denture care, because care now must include complex restorative procedures as well as esthetic dentistry and implants .
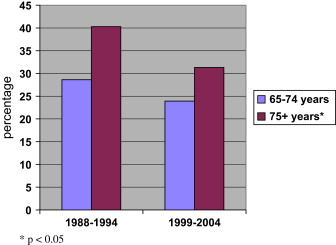
For those older adults who are edentulous, oral health impacts are reported to be more frequent and affect chewing and food choice: they require ongoing dental care even when wearing complete dentures . In the past 35 years the overall prevalence of edentulism in the United States has declined from 20.3% in 1972 to 13.9% in 2001 . The most recent national data reported that 31.3% of people aged more than or equal to 75 years were edentulous, whereas the younger elderly (aged 65–74 years) have a prevalence of edentulism of 23.9% ( Fig. 1 ) . Edentulism also varies by state in the United States, with the highest prevalence of edentulism in 65 years or older adults in Kentucky (42.3%), West Virginia (41.9%), Tennessee (36%), and Mississippi (35.1%) . The lowest prevalence of edentulism was reported in Hawaii (13.1%), California (13.3%), Utah (14.7%), and Minnesota (14.8%) . Retention of teeth is significantly higher in older adults with higher income and education levels, Hispanics and Whites, nonsmokers, and those reporting excellent general health status . A 2000 report indicated that tooth loss was highest in the United States among older American Indians and Alaskan Natives .
Older adults have been defined as a cohort of people aged 65 years or older. However, a chronologic definition of the aging population is not particularly useful in dentistry. A functional definition, based upon an older individual’s ability to travel to seek services, is more appropriate; such a definition is also dynamic, with older adults often moving among the various categories as their health declines or improves . The aging population can be functionally categorized into three broad groups: the functionally independent older adult, the frail older adult, and the functionally dependent older adult .
The majority of older adults (95%) live in the community; of these it can be estimated that around 5% are homebound and another approximately 17% have a major limitation in mobility because of some chronic condition. This still leaves about 73% of the population over the age of 65 years who are living in the community and are able to come to the dental office independently . Approximately 5% are institutionalized; over 1.65 million older Americans reside in nursing homes . Nearly half of nursing home residents are aged 85 or more years . These residents have high levels of functional dependence combined with high levels of cognitive impairment. Assistance with three or more activities of daily living is needed by more than 75% of residents, such as showering or bathing (including oral hygiene care), dressing, and eating. Cognitive impairment is evident in more than 70% of residents .
Coronal and root caries
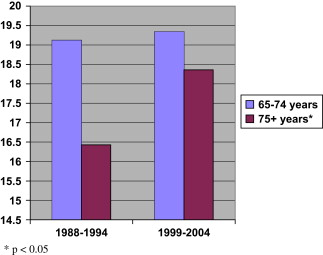
National data detailing the oral health status of older Americans reveal some interesting trends over time. Mean number of permanent teeth among dentate older adults aged 65 or more years have increased between the National Health and Nutrition Examination Survey (NHANES) round III (1988–1994) and that conducted in 1999 to 2004, especially in the aged 75 or more cohort, and those with higher incomes, better education, and nonsmokers ( Fig. 2 ). Mean number of decayed, missing, and filled teeth in older Americans aged 65 or more years have decreased slightly across these surveys, including the contribution of decayed coronal surfaces . NHANES comparison data from rounds I (1971–1974) and III (1988–1994) reported that the percentage of teeth with caries (treated or untreated) decreased for participants aged 18 to 54 years but increased for participants aged 55 to 74 years . The overall prevalence of coronal caries in older adults aged 65 or more years did not significantly change between NHANES rounds in 1988 to 1994 and 1999 to 2004, but the prevalence of untreated dental caries overall in older Americans significantly decreased, with higher untreated caries prevalence evident in older African Americans and Hispanics, those with lower incomes, less education, and current or former smokers. This was also the case for untreated root caries . Greater retention of teeth predisposes many older adults to a continual risk of both new and recurrent coronal and root caries, and extends the risk for developing gingivitis and periodontal diseases . Dental caries is still clearly a public health problem for subgroups of older Americans, such as those of lower socioeconomic status, with dementia, who are homebound and who are institutionalized .
Periodontal and oral mucosal diseases
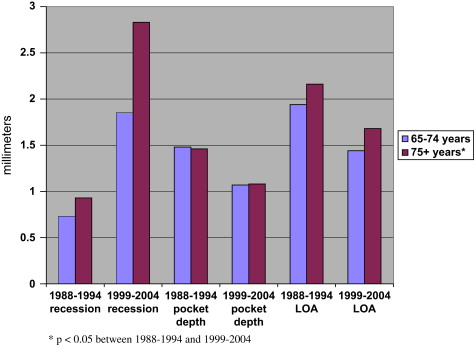
Removal of dental plaque becomes a more difficult challenge because of age-related toothbrush abrasion, gingival recession, salivary dysfunction, dexterity disabilities, and cognitive impairment . The prevalence and incidence of periodontal conditions in older adults has clearly been related to poor oral hygiene and high levels of dental plaque . Data from the NHANES surveys has reported a significant increase in mean recession in older adults, but a significant decrease in mean pocket depth and mean loss of attachment, and in severe periodontal disease ( Fig. 3 ). Mean loss of attachment was significantly higher in older males, older African and Hispanic Americans, in poorer older Americans, those older adults with less than high school education, and older current or former smokers . A variety of oral mucosal conditions may be present in older adults, and may be exacerbated by salivary dysfunction. Oral and pharyngeal cancer in particular are relevant to older Americans, with the median age at diagnosis at 64 years; the primary determinants of this cancer are smoking and alcohol use .
Geriatric access, barriers, and use of dental care in the United States: models of care provision
The aging United States population is a “looming and major challenge that will exacerbate the issue of access to care” in dentistry . Older adults are seeking dental care at a growing rate. Locker and others have evidenced that “improvements in the oral health of older adults depend upon access to comprehensive dental treatments.” Indeed, the type of dental care needing to be provided for older adults goes way beyond emergency care and denture care, as was discussed by Barmes : “…public policies to support community awareness and acceptance of broad-based preventive behaviors to preserve oral health in old age are essential. Policies also must provide guidance on how to… ensure access to cost-effective and high-quality services for all.”
The percentage of community-living older Americans who visited the dentist within the past year is steadily increasing and is expected to continue to do so for several decades. However, a lower percentage of older adults (56.3% in 2004) visited the dentist within the past year, in comparison to adults (64.0% in 2004) and children (76.4%). The lowest use was reported for the poorest older adults and for older African Americans. Data also indicated that rural older Americans were less likely to report being regular dental care users than urban older Americans. Data from the 2006 United States National Health Interview Survey indicated that 71.69% of dentate persons 75 years and older had been to the dentist within the last year. However, only 17.8% of edentulous adults over age 65 had such a visit . The majority (59.2%) of these edentulous older adults had not used the services of a dentist for at least 5 years. Older adults with some natural teeth were using dental services in a manner similar to younger adults. The value older adults place on dental care seems to influence use more than any other factor, including their ability to pay for care . Data from the 1996 Medical Expenditure Survey confirmed that persons over age 65 used more restorative, prosthetic, and oral surgery services than any other age group . Another study examined dental service use by independent living adults in private practice, and showed that older adults sought dental services at rates greater than those expected by their representative percentage . It was also reported that “patient visits by older adults generated, on average, as much or more income than did visits by individuals from any other age grouping” .
Several other barriers to dental care for older Americans include lack of perceived need, poor health literacy, and inadequate federal policies and regulations. There is a clearly reduced perceived need for dental care and dental use by edentulous older adults versus dentate older adults. Perceived need is also reduced as functional dependency increases, and dental care use concurrently decreases, especially in those older adults who are institutionalized . Some reviews have highlighted reduced perceived need as the greatest barrier to dental care use in older adult cohorts . Another less studied barrier is that of poor health literacy; this is reflected in challenges for older adults with accessing dental services, performing oral hygiene tasks, completing fully informed consent procedures, participating actively in decision-making in dental treatment planning, and undertaking follow-up oral health care activities . Despite the enactment of federal legislation in 1987 mandating that nursing homes provide access to dental care for residents, the poor oral health status and use data reported in recent years evidenced that adequate access to dental care does not exist for many United States nursing home residents . Thus, the treatment older adults seek will depend directly upon their self-perceived need, their financial ability to pay for that care, and issues such as transportation and documentation, rather than the normative need detected during an oral examination by a dentist .
The Agency for Health care Research and Quality reported in 2000 that older adults aged 65 or more years paid 75% or more of their dental expenses out-of-pocket, compared with the general population out-of-pocket expenses of around 50% . The main reason for this large out-of-pocket expense in older Americans is the lack of reimbursement for dental care; after retirement, dental insurance is often only available for older adults with retiree plans, which is a minority of the older population . Routine dental care is generally not covered by Medicare, and Medicaid coverage varies greatly between states .
In an analysis of the Asset of Health Dynamics Among the Oldest Old dataset from 1993 to 1995, it was clear that economic access factors had a strong indirect effect on dental use disparities among African Americans and Hispanics, because of the fact that dental services were not covered by Medicare . This analysis indicated that Medicare played a very important role in providing older minority Americans with access to medical care, and the lack of Medicare dental coverage was a barrier to them accessing dental care . One of the greatest barriers to care for Medicaid recipients is that the reimbursement rate is so low that many dentists are discouraged from treating Medicaid patients, especially those in nursing homes . Rubinstein portrays the current situation succinctly: “Americans are concerned about access to health care and the cost of prescription drugs, (but) Americans’ interest in increased access to dental care for seniors never registers.” A suggested solution is the increased use of tax-deferred dental or medical savings accounts, where balances accrue over time and then can be accessed later in life. Others have suggested a Medicare dental supplemental insurance program, with an emphasis on preventive dental services, or a dental insurance plan that is prepaid during employment similar to long-term care insurance .
Stakeholder partnerships to improve access to dental care
There will be many challenges in reducing barriers and improving access to and use of dental care for older Americans in the coming years. Stakeholders, including dental professionals and the dental benefits industry, need to develop innovative dental financing programs that will increase older Americans access to dental care. Most dental services for older adults are provided in community-based offices by private dental practitioners. For functionally independent and frail older adults, a few modifications in office design to allow for normal aging changes will allow private practitioners to treat this population . For nonambulatory dependent older adults, including nursing home residents, a variety of dental service delivery system models are needed, which involve several stakeholder partnerships.
The most common model used to provide dental care for dependent older adults is transporting them to a dental office, which is the most convenient for dental professionals as they can treat patients in their own offices with auxiliary personnel and appropriate equipment . It is also the most cost-effective service for a dentist, as no traveling or set-up time is required, but it is expensive and time-consuming for a nursing home, as a staff member needs to accompany their resident to the dental office. Thus, not surprisingly, many nursing homes are reluctant to contract such an arrangement, and thus little care under these circumstances is voluntarily offered to nursing home residents. Transporting dependent older adults requires a suitable vehicle and use of volunteer drivers, subsidized transport, or ambulances, which creates many coordination, organization, and financing problems for both the patient and nursing home. Many modifying factors need to be considered when transporting a dependent older adult to a dentist’s office: the person’s activity level, continence, transferability appointment times, accompanying person, communication, legal consent issues, and ethical considerations.
There are some excellent partnerships that have been formed on regional levels across the United States, between private dental practitioners and local nursing homes, in which the nursing home provides a “dental office” with a dental chair and other required dental equipment. The equipment may be owned by the nursing home or the dentist, or may have been donated. The main advantage of this partnership model is that residents can be treated within their own environment, for it has been shown that frail and cognitively impaired older adults do not withstand well the disruption of being transported, and disruptive behaviors often result when they are taken out of their nursing home setting. Some disadvantages are that the “fixed” dental equipment may not be able to be used bedside, and that the nursing home needs to be large (150 or more residents) to ensure financial success of the dental program. A modification of this model is when the dental professional brings portable dental equipment with them each visit, but the nursing home has a fixed dental chair that is also used for other purposes, such as for aromatherapy or podiatry. Several comprehensive reviews of portable and mobile dental equipment have been published .
A very successful partnership model in the United States has been that of larger groups of dental practitioners working together as a not-for-profit entity, using a combination of portable and mobile dental equipment. Long-standing examples of this model are Apple Tree Dental in Minnesota ( http://www.appletreedental.org ), and Access Dental and Carolina’s Mobile Dentistry in North Carolina ( http://www.accessdentalcare.org/ http://www.carolinas.org/services/seniorcare/mobileDentistry.cfm ). Another variation of this model is when the dental professionals include dental students from dental schools (some examples include the University of Iowa, Ohio State University, University of British Columbia, Marquette University, University of Southern California, and University of Minnesota).
Additional stakeholders in these programs have included state dental associations, state government public health and aging entities, and dental insurance companies. In these programs, dentists, dental hygienists, and dental assistants work together to provide dental treatment on-site at nursing homes and other sites for older adults. A variety of light and heavier portable equipment is transported in a truck or recreational vehicle from site to site. The program stays at a nursing home site for several weeks or months to provide comprehensive dental treatment for residents. A room is provided by the nursing home for the setting-up of the portable dental clinic, which includes dental chairs, portable high-speed dental units, portable headrests for wheelchairs, and portable x-ray equipment. These larger partnership models have gradually replaced mobile dental vans, which were often used in the 1970s and 1980s to provide dental treatment at nursing homes. The many disadvantages of the mobile vans included initial capital costs, weather conditions, and the electrical capacity of the motor home. Many residents are stressed when they are moved from the controlled environment of a facility through inclement weather into the mobile van.
One of the largest and nationally focused stakeholder partnerships in geriatric dentistry is that between GlaxoSmithKline Consumer Health care, the American Dental Association (ADA), and the ADA Foundation, which have entered into a 3-year $1 million national partnership to help address the oral health needs of aging Americans. These partners, together with the Special Care Dentistry Association, will present the upcoming OralLongevity series at the ADA national meeting in 2007, with an accompanying brochure and DVD education program for dental professionals to use with older adults and caregivers.
Interactions among state dental associations, state dental public health officials, academicians, and private practitioners have resulted in some productive partnerships to improve access to dental care for frail and dependent older adults. In these partnerships, links and communication have been established and maintained among dental professionals and nursing homes. Some also involving the sharing of portable dental equipment, as well as handbooks containing policies and procedures such as contracts, oral hygiene care manuals, and other reference materials (some examples are the Iowa Dental Association, British Columbia Dental Association, Louisville Dental Society, and North Carolina Dental Society with Carolina’s Mobile Dentistry). Another example of such a stakeholder partnership is Iowa’s Seniors Smiles project, coordinated by the Iowa Department of Public Health, Oral Health Bureau, and the University of Iowa, which links Medicaid waiver program homebound older adults and local dental professionals with the support of the home nursing program. In the Iowa program, oral health screenings by nurses identify homebound older adults with dental needs, and nurses are trained in preventive oral hygiene care activities to use with their older clients.
Geriatric access, barriers, and use of dental care in the United States: models of care provision
The aging United States population is a “looming and major challenge that will exacerbate the issue of access to care” in dentistry . Older adults are seeking dental care at a growing rate. Locker and others have evidenced that “improvements in the oral health of older adults depend upon access to comprehensive dental treatments.” Indeed, the type of dental care needing to be provided for older adults goes way beyond emergency care and denture care, as was discussed by Barmes : “…public policies to support community awareness and acceptance of broad-based preventive behaviors to preserve oral health in old age are essential. Policies also must provide guidance on how to… ensure access to cost-effective and high-quality services for all.”
The percentage of community-living older Americans who visited the dentist within the past year is steadily increasing and is expected to continue to do so for several decades. However, a lower percentage of older adults (56.3% in 2004) visited the dentist within the past year, in comparison to adults (64.0% in 2004) and children (76.4%). The lowest use was reported for the poorest older adults and for older African Americans. Data also indicated that rural older Americans were less likely to report being regular dental care users than urban older Americans. Data from the 2006 United States National Health Interview Survey indicated that 71.69% of dentate persons 75 years and older had been to the dentist within the last year. However, only 17.8% of edentulous adults over age 65 had such a visit . The majority (59.2%) of these edentulous older adults had not used the services of a dentist for at least 5 years. Older adults with some natural teeth were using dental services in a manner similar to younger adults. The value older adults place on dental care seems to influence use more than any other factor, including their ability to pay for care . Data from the 1996 Medical Expenditure Survey confirmed that persons over age 65 used more restorative, prosthetic, and oral surgery services than any other age group . Another study examined dental service use by independent living adults in private practice, and showed that older adults sought dental services at rates greater than those expected by their representative percentage . It was also reported that “patient visits by older adults generated, on average, as much or more income than did visits by individuals from any other age grouping” .
Several other barriers to dental care for older Americans include lack of perceived need, poor health literacy, and inadequate federal policies and regulations. There is a clearly reduced perceived need for dental care and dental use by edentulous older adults versus dentate older adults. Perceived need is also reduced as functional dependency increases, and dental care use concurrently decreases, especially in those older adults who are institutionalized . Some reviews have highlighted reduced perceived need as the greatest barrier to dental care use in older adult cohorts . Another less studied barrier is that of poor health literacy; this is reflected in challenges for older adults with accessing dental services, performing oral hygiene tasks, completing fully informed consent procedures, participating actively in decision-making in dental treatment planning, and undertaking follow-up oral health care activities . Despite the enactment of federal legislation in 1987 mandating that nursing homes provide access to dental care for residents, the poor oral health status and use data reported in recent years evidenced that adequate access to dental care does not exist for many United States nursing home residents . Thus, the treatment older adults seek will depend directly upon their self-perceived need, their financial ability to pay for that care, and issues such as transportation and documentation, rather than the normative need detected during an oral examination by a dentist .
The Agency for Health care Research and Quality reported in 2000 that older adults aged 65 or more years paid 75% or more of their dental expenses out-of-pocket, compared with the general population out-of-pocket expenses of around 50% . The main reason for this large out-of-pocket expense in older Americans is the lack of reimbursement for dental care; after retirement, dental insurance is often only available for older adults with retiree plans, which is a minority of the older population . Routine dental care is generally not covered by Medicare, and Medicaid coverage varies greatly between states .
In an analysis of the Asset of Health Dynamics Among the Oldest Old dataset from 1993 to 1995, it was clear that economic access factors had a strong indirect effect on dental use disparities among African Americans and Hispanics, because of the fact that dental services were not covered by Medicare . This analysis indicated that Medicare played a very important role in providing older minority Americans with access to medical care, and the lack of Medicare dental coverage was a barrier to them accessing dental care . One of the greatest barriers to care for Medicaid recipients is that the reimbursement rate is so low that many dentists are discouraged from treating Medicaid patients, especially those in nursing homes . Rubinstein portrays the current situation succinctly: “Americans are concerned about access to health care and the cost of prescription drugs, (but) Americans’ interest in increased access to dental care for seniors never registers.” A suggested solution is the increased use of tax-deferred dental or medical savings accounts, where balances accrue over time and then can be accessed later in life. Others have suggested a Medicare dental supplemental insurance program, with an emphasis on preventive dental services, or a dental insurance plan that is prepaid during employment similar to long-term care insurance .
Stakeholder partnerships to improve access to dental care
There will be many challenges in reducing barriers and improving access to and use of dental care for older Americans in the coming years. Stakeholders, including dental professionals and the dental benefits industry, need to develop innovative dental financing programs that will increase older Americans access to dental care. Most dental services for older adults are provided in community-based offices by private dental practitioners. For functionally independent and frail older adults, a few modifications in office design to allow for normal aging changes will allow private practitioners to treat this population . For nonambulatory dependent older adults, including nursing home residents, a variety of dental service delivery system models are needed, which involve several stakeholder partnerships.
The most common model used to provide dental care for dependent older adults is transporting them to a dental office, which is the most convenient for dental professionals as they can treat patients in their own offices with auxiliary personnel and appropriate equipment . It is also the most cost-effective service for a dentist, as no traveling or set-up time is required, but it is expensive and time-consuming for a nursing home, as a staff member needs to accompany their resident to the dental office. Thus, not surprisingly, many nursing homes are reluctant to contract such an arrangement, and thus little care under these circumstances is voluntarily offered to nursing home residents. Transporting dependent older adults requires a suitable vehicle and use of volunteer drivers, subsidized transport, or ambulances, which creates many coordination, organization, and financing problems for both the patient and nursing home. Many modifying factors need to be considered when transporting a dependent older adult to a dentist’s office: the person’s activity level, continence, transferability appointment times, accompanying person, communication, legal consent issues, and ethical considerations.
There are some excellent partnerships that have been formed on regional levels across the United States, between private dental practitioners and local nursing homes, in which the nursing home provides a “dental office” with a dental chair and other required dental equipment. The equipment may be owned by the nursing home or the dentist, or may have been donated. The main advantage of this partnership model is that residents can be treated within their own environment, for it has been shown that frail and cognitively impaired older adults do not withstand well the disruption of being transported, and disruptive behaviors often result when they are taken out of their nursing home setting. Some disadvantages are that the “fixed” dental equipment may not be able to be used bedside, and that the nursing home needs to be large (150 or more residents) to ensure financial success of the dental program. A modification of this model is when the dental professional brings portable dental equipment with them each visit, but the nursing home has a fixed dental chair that is also used for other purposes, such as for aromatherapy or podiatry. Several comprehensive reviews of portable and mobile dental equipment have been published .
A very successful partnership model in the United States has been that of larger groups of dental practitioners working together as a not-for-profit entity, using a combination of portable and mobile dental equipment. Long-standing examples of this model are Apple Tree Dental in Minnesota ( http://www.appletreedental.org ), and Access Dental and Carolina’s Mobile Dentistry in North Carolina ( http://www.accessdentalcare.org/ http://www.carolinas.org/services/seniorcare/mobileDentistry.cfm ). Another variation of this model is when the dental professionals include dental students from dental schools (some examples include the University of Iowa, Ohio State University, University of British Columbia, Marquette University, University of Southern California, and University of Minnesota).
Additional stakeholders in these programs have included state dental associations, state government public health and aging entities, and dental insurance companies. In these programs, dentists, dental hygienists, and dental assistants work together to provide dental treatment on-site at nursing homes and other sites for older adults. A variety of light and heavier portable equipment is transported in a truck or recreational vehicle from site to site. The program stays at a nursing home site for several weeks or months to provide comprehensive dental treatment for residents. A room is provided by the nursing home for the setting-up of the portable dental clinic, which includes dental chairs, portable high-speed dental units, portable headrests for wheelchairs, and portable x-ray equipment. These larger partnership models have gradually replaced mobile dental vans, which were often used in the 1970s and 1980s to provide dental treatment at nursing homes. The many disadvantages of the mobile vans included initial capital costs, weather conditions, and the electrical capacity of the motor home. Many residents are stressed when they are moved from the controlled environment of a facility through inclement weather into the mobile van.
One of the largest and nationally focused stakeholder partnerships in geriatric dentistry is that between GlaxoSmithKline Consumer Health care, the American Dental Association (ADA), and the ADA Foundation, which have entered into a 3-year $1 million national partnership to help address the oral health needs of aging Americans. These partners, together with the Special Care Dentistry Association, will present the upcoming OralLongevity series at the ADA national meeting in 2007, with an accompanying brochure and DVD education program for dental professionals to use with older adults and caregivers.
Interactions among state dental associations, state dental public health officials, academicians, and private practitioners have resulted in some productive partnerships to improve access to dental care for frail and dependent older adults. In these partnerships, links and communication have been established and maintained among dental professionals and nursing homes. Some also involving the sharing of portable dental equipment, as well as handbooks containing policies and procedures such as contracts, oral hygiene care manuals, and other reference materials (some examples are the Iowa Dental Association, British Columbia Dental Association, Louisville Dental Society, and North Carolina Dental Society with Carolina’s Mobile Dentistry). Another example of such a stakeholder partnership is Iowa’s Seniors Smiles project, coordinated by the Iowa Department of Public Health, Oral Health Bureau, and the University of Iowa, which links Medicaid waiver program homebound older adults and local dental professionals with the support of the home nursing program. In the Iowa program, oral health screenings by nurses identify homebound older adults with dental needs, and nurses are trained in preventive oral hygiene care activities to use with their older clients.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


