“Extent” of disease
Localized: <30 % teeth/sites affected
Generalized: >30 % teeth/sites affected
“Severity” of disease
Based on clinical attachment loss noted in the patient
Slight: 1–2 mm CAL
Moderate: 3–4 mm CAL
Severe: ≥5 mm CAL
“Condition”
Chronic periodontitis
13.2.2 Aggressive Periodontitis (Lang et al. 1999)
Classification of aggressive periodontitis is not based on the age of the patient. However, the profile of many affected patients is typically younger (usually <30 years).
The following are primary features of aggressive periodontitis:
-
Rapid rate of attachment loss and destruction of bone.
-
Familial aggregation.
-
Patients are otherwise clinically healthy – no systemic disease.
Secondary features (may/may not be present):
-
Severity of disease may be disproportionate to amounts of microbial deposits (especially for localized aggressive).
-
Increased Aggregatibacter actinomycetemcomitans (Aa) (and in some cases Porphyromonas gingivalis (Pg)) may be present.
-
Cellular: Hyper-responsive macrophage phenotype and abnormal phagocytes.
-
Disease (attachment loss and bone loss) may be self-limiting.
13.2.2.1 Localized Aggressive (LAP)
-
Diagnosis of “localized” not based on the 30 % rule
-
Diagnosis: LAP has a first molar/incisor presentation; interproximal attachment loss on at least two permanent teeth (one of which is a first molar) and not more than two teeth other than first molars/incisors are involved.
-
Typical onset around puberty.
-
Prevalence: Limited data available; generally estimated to be <1 % adolescents but more prevalent in African-American population.
13.2.2.2 Generalized Aggressive (GAP)
-
Diagnosis of “generalized” not based on the 30 % rule (although this is often met; indeed, disease often affects the entire dentition).
-
Diagnosis: Interproximal attachment loss on at least three permanent teeth other than first molars/incisors.
-
Affected patients usually young (<30 years) but may be older.
-
Episodic pattern of destruction.
-
Prevalence: Limited data available; estimated at 0.13 % of the US adolescents (Lӧe and Brown 1991).
13.3 Patient Assessment
- A.
Chief Complaint
-
Periodontal disease can affect different parts of a patient’s dentition to varying degrees. Some patients may not even be aware that they have a problem, while others will come to you complaining that their teeth are loose or that their gums bleed.
-
- B.
Medical and Dental History
-
It is very important to gather an accurate medical history from the patient to help determine possible barriers to treatment as well as possible systemic factors contributing to the presence of disease.
-
- C.
Periodontal Examination (AAP 2011)
The main objectives of a thorough clinical exam pertain to identifying the main problems and their sources in the patient’s mouth. Identify etiologic factors, whether past or present, that will affect the long-term prognosis of all the teeth involved (Table 13.2).
Table 13.2
Components of periodontal examination
|
Clinical parameters
|
Radiographic parameters
|
|---|---|
|
Probing depth
|
Bone height relative to CEJ
|
|
Clinical attachment level
|
Assessment for horizontal/vertical bone loss
|
|
Plaque
|
Presence of intact lamina dura
|
|
Bleeding on probing
|
|
|
Suppuration
|
|
|
Mobility
|
|
|
Furcation involvement
|
|
|
Mucogingival tissue assessment
|
- 1.
Probing Depth (PD)
-
Record at six sites per tooth with a calibrated periodontal probe (e.g., UNC-15): distobuccal, buccal, mesiobuccal, mesiolingual, lingual, and distolingual surfaces
-
- 2.
Clinical Attachment Level (CAL)
-
Calculated by adding the probing depth and gingival margin together (PD + GM = CAL).
-
CAL measurements are used in developing a periodontal diagnosis for the patient. Situations of CAL loss are classified as slight (CAL 1–2 mm), moderate (CAL 3–4 m), or severe (5–6 mm).
-
- 3.
Bleeding on Probing (BOP)
-
BOP should be assessed while probing and recorded as “present” or “absent” at each site.
-
The percentage of bleeding sites can be calculated and used during re-evaluations to determine changes in periodontal health.
-
- 4.
Suppuration (S)
-
Similar to BOP, the presence of suppuration indicates a disease process in the periodontium such as infection.
-
If suppuration is suspected, the periodontal probe can be used as a supplemental tool to express the pus by placing the probe flat against the tissue and dragging the probe towards the gingival margin with slight pressure.
-
- 5.
Plaque Score
-
At each periodontal visit for cleaning, nonsurgical therapy, or recall, a plaque score should be calculated, utilizing a plaque disclosing agent.
-
Of all the measurements taken during the periodontal charting process, a plaque score is the most visual way to show patients the effects of their home care and oral hygiene.
-
Plaque presence is recorded at six surfaces per tooth as a binary “yes” or “no” measurement for the presence of plaque on that particular surface from which a percentage may then be calculated.
-
After disclosing the patient and calculating the plaque score percentage, it is important to show the patient with a mirror the sites on their teeth that are not being brushed properly. Effective plaque removal is modelled for the patient. The patient should subsequently be given an opportunity to practice plaque removal at the affected sites.
-
The goal is to achieve and maintain a plaque score of 25 % or less.
-
- 6.
Furcations (F)Furcation probe accessPractical assessmentClass I Furcation (F1)Does not exceed 1/3 of the width of the tooth (<3 mm)Probe engages furcation slightly but no “catch” present when withdrawnClass II Furcation Lesion (F2)Exceeds 1/3 of the tooth width but does encompass the total width of the tooth (>3 mm)Probe hooks into roof of furcation, “catch” present on attempt to withdrawClass III Furcation Lesion (F3)“Through and through” access – probe penetrates through entire width of furcation areaProbe enters furcation (e.g. buccal) and emerges via another furcation site (e.g. lingual) on tooth
-
Furcation involvement is assessed using a Nabers (furcation) probe.
-
The degree of furcation involvement has implications for individual prognosis of the tooth and for the ability of the patient to successfully maintain this surface devoid of plaque and biofilm.
-
- 7.
Mobility (M)
-
To assess mobility, the blunt end of the explorer and the blunt end of the mirror can be placed on the B and L surfaces of the tooth, respectively, and pressure applied to assess if any pathologic movement is observed. If a gloved finger is used in place of one of these hard objects, a depression in the soft tissue of the finger may incorrectly mimic tooth movement (Fig. 13.1).
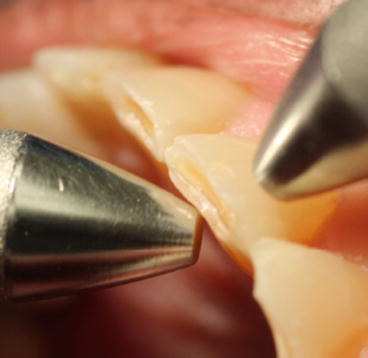 Fig. 13.1Check for mobility with instruments on either side of the tooth (Photo Courtesy of Dr. Daniel Buono)
Fig. 13.1Check for mobility with instruments on either side of the tooth (Photo Courtesy of Dr. Daniel Buono) -
The extent of the mobility is categorized in classesClass IMovement of the crown is between 0.2 and 1 mm horizontally in any directionClass IIMovement of the crown is >1 mm horizontally in any directionClass IIIMovement of the crown in the vertical direction is present in addition to horizontal movement
-
- 8.
Mucogingival Assessment
-
Evaluation gives a descriptive picture of the relative amount of attached, keratinized gingiva.
-
Note the presence of any abnormal attachment of a labial, lingual, or buccal frenum, i.e., close to gingival margin and whose movement impacts on gingival tissue. Friel’s test involves stretching the lip in the area of a labial/buccal frenum – blanching of the marginal gingival tissue indicates a frenal pull that may be associated with the risk of further gingival recession.
-
Stretch the lips gently and note the position of the mucogingival junction (MGJ-where attached gingiva and the alveolar mucosa meet). Note and document the amount of keratinized gingiva present.
-
Gingival Recession is categorized using the Miller classification (Miller 1985) (Table 13.3).Table 13.3Classification of gingival recessionClassMarginal tissue recessionInterdental areaRoot coverage anticipatedIDoes not extend to MGJNo periodontal loss100 %IITo or beyond MGJNo periodontal loss100 %IIITo or beyond MGJLoss of tissue or malpositionPartialIVTo or beyond MGJSevere loss of tissueNot anticipated
-
- 9.
Radiographic Analysis
-
Bitewing radiographs are helpful in determining bone levels both at a single moment in time as well as looking at progression of periodontal disease over time.
-
Subgingival calculus can sometimes be visualized as faint radiopaque wisps attached to the tooth usually at the CEJ (Fig. 13.2).
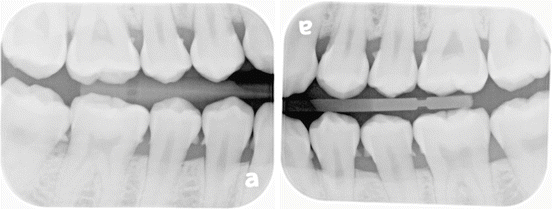 Fig. 13.2Calculus deposits can be visualized at interproximal surfaces
Fig. 13.2Calculus deposits can be visualized at interproximal surfaces -
It is important to remember that radiographs alone are not diagnostic for periodontal issues, and a thorough clinical examination must be conducted.
-
13.4 Risk Factors
Risk factors, when present, increase the probability that an individual will develop disease. The terminology used to discuss these concepts can be confusing. While many systemic, local, and environmental factors may be associated with disease aetiology, only a few meet the definition of a “true” risk factor (Table 13.4).
Table 13.4
Factors associated with periodontal disease risk
|
Description
|
Examples
|
|
|---|---|---|
|
Risk factor
|
Exposure to the factor must precede the onset of disease
Association confirmed in a prospective longitudinal study
|
Tobacco smoking
Diabetes
Plaque deposits/specific pathogenic bacteria
|
|
Risk indicator
|
Potential risk factor – has been identified in a cross-sectional study
However, not yet confirmed in a longitudinal study
|
Osteoporosis
HIV/AIDs
Stress
|
|
Risk marker
|
Factors that are associated with/predictive of disease but do not cause it
|
Previous history of periodontal disease
|
|
Background characteristica
|
May sometimes be described as non-modifiable risk factors
Evident in epidemiologic studies but causal role difficult to assign
|
Genetics
Age (older)
Gender (male)
Socio-economic status (lower SES)
|
13.4.1 Plaque Deposits/Specific Pathogenic Bacteria
-
A modifiable risk factor.
-
Role as risk factor for gingivitis is clear. Experimental accumulation of plaque deposits results in gingival inflammation; removal of deposits is associated with clinical improvement (Löe et al. 1965).
-
Association with periodontitis is not as strong – not all patients with bacterial deposits develop disease and increased plaque does not imply increased disease. However, specific bacterial species have been identified as aetiologic agents for periodontal diseases: Aggregatibacter actinomycetemcomitans (Aa), Porphyromonas gingivalis (Pg), and Tannerella forsythia (Tf) (World Workshop Consensus Report 1996).
-
The presence of calculus and local anatomic (e.g., furcations, root concavities, cervical enamel projections) or clinical features (e.g., restoration overhangs, crowding) may contribute to disease risk due to their potential to accumulate/harbour plaque, as well as making plaque removal (patient/professional) more difficult to achieve.
13.4.2 Tobacco Smoking
-
A modifiable risk factor strongly associated with periodontal disease and impaired response to therapy.
-
Smoking cessation is associated with improved clinical response to therapy (Grossi et al. 1997).
-
Cigarette smokers may still be candidates for periodontal surgery, but the magnitude of beneficial effect is compromised in these patients relative to nonsmokers (Kotsakis et al. 2015).
13.4.2.1 Potential Mechanisms to Mediate Effect on Periodontium
-
Effect on microflora
-
Evidence is conflicting – many studies fail to show differences in the amount or composition of plaque. However, increased prevalence of pathogenic species/higher proportion of subjects positive for pathogenic species has been demonstrated in smokers (Zambon et al. 1996).
-
-
Effects on host response:
-
Impaired neutrophil function (reduced chemotaxis/phagocytosis)
-
Altered lymphocyte function
-
-
Effects of nicotine:
-
Altered fibroblast attachment
-
Impact on vascularity of tissues and production of inflammatory mediators
-
13.4.3 Diabetes
-
Strongly associated with periodontal disease.
-
Cross-sectional studies indicate that diabetics have approximately a threefold risk of developing periodontal destruction, as measured by bone loss (Emrich et al. 1991).
-
Poor glycaemic control has been associated with increased risk of progressive disease, whereas well-controlled diabetics may not have increased risk (Taylor et al. 1998).
-
Bidirectional relationship – evidence exists for an association between severe periodontitis and complications of type 2 diabetes (Chapple et al. 2013).
-
Advise diabetic patients (i) that risk of periodontal disease is increased by diabetes and (ii) that glycaemic control may be impaired if they have periodontal disease.
-
Preventive care and periodontal maintenance strategy should be particularly emphasized.
13.4.3.1 Potential Mechanisms to Mediate Effect on Periodontium (Mealey and Oates 2006)
-
Effect on host response
-
Impaired neutrophil function (reduced adherence, chemotaxis/phagocytosis)
-
Hyper-responsiveness of macrophages/monocytes – triggers increase in pro-inflammatory cytokines
-
-
Delayed wound healing (via altered metabolism of connective tissues)
-
Hyperglycaemia affects osteoblasts and fibroblasts – bone formation and collagen turnover affected.
-
Formation of AGEs promotes inflammation and further affects collagen turnover.
-
Interaction of AGEs with specific receptors (AGE-RAGe interactions) on various cells contributes to hyper-inflammatory response.
-
-
Effect on microflora
-
Based on current knowledge, there is insufficient evidence that diabetes significantly modifies the oral microflora (Chapple et al. 2013).
-
-
Hyperglycaemia contributes to an imbalance of free radicals resulting in oxidative stress mediated tissue damage.
13.5 Nonsurgical Periodontal Therapy
13.5.1 Goals
-
Remove microbial deposits from tooth surfaces
-
Eliminate plaque-retentive irregularities
-
Create intra-oral environment that helps in maintenance of gingival tissue health
-
Increase effectiveness of patient’s self-administered plaque control
13.5.2 Components
-
Nonsurgical instrumentation – hand instruments + powered instruments
-
Preventive advice – oral hygiene instruction (OHI), tobacco cessation, dietary advice (See Appendix for oral hygiene aids and smoking cessation)
-
Address local aetiologic factors – removal of overhangs, replace defective restorations, etc.
-
Address other aetiologic factors – systemic disease, habits, etc.
13.5.3 Basic Principles
OH alone is not enough: Some, but limited improvement of gingival conditions may occur in periodontal pockets following improved supragingival plaque control alone (Cercek et al. 1983).
Instrumentation alone is not enough: Instrumentation alone, without improved OH, may result in microbial repopulation of instrumented sites within a short period after therapy (Magnusson et al. 1984).
13.5.4 Expectation Setting for Your Patient
-
Explain that periodontal disease is common among the US population and represents a chronic disease. As periodontal disease is frequently asymptomatic, so the dentist has a key role in monitoring progress of disease.
-
Address the aetiology of periodontal disease and highlight that only some factors are modifiable – hence, the emphasis on the importance of plaque control and tobacco cessation.
-
Advise your patient from the outset if further treatment is likely to be necessary.
-
Outline the importance of periodontal maintenance and compliance to longer-term periodontal health.
13.5.4.1 Calculus Detection
-
Periodontal explorer
-
Primary instrument for calculus detection.
-
Properties include fine tip and curvature of shank and tip to allow universal use.
-
Used with light grasp, light touch.
-
Example: ODU 11/12.
-
-
Periodontal probe
-
The markings on some manual periodontal probes are inset/grooved, increasing tactile sensation and allowing their use in calculus detection. Example: UNC-12 probe.
-
-
Radiographs
-
Calculus may be detected on radiographic films as a relative opacity on the crown/root surface of a tooth. This may be more easily distinguishable on intra-oral radiographic images and may be noted particularly in the root area approximating the CEJ.
-
Not all calculus deposits will be radiographically visible.
-
-
Visual detection
-
Supragingival calculus and some superficial subgingival deposits may be detected by direct vision. This facilitated by drying the teeth, using good lighting and with gentle air deflection of inflamed gingival tissues. In non-pigmented tissues, heavy focal calculus deposits may sometimes be associated with “shadowing” through the gingival tissues and/or localized sites of focal inflammation.
-
13.5.5 How Do I Know If What I’m Feeling Is Calculus?
-
Calculus detection is difficult. Microscopic deposits of calculus may remain undetected in many instances following nonsurgical/surgical therapy, particularly in posterior teeth, interproximal and furcation regions.
-
Calculus is most frequently (but not exclusively) detected in the areas at/immediately apical to the CEJ and slightly coronal to the base of the periodontal pocket.
Use light grasp to improve tactile sensation.
-
Establish where your explorer position is apico-coronally – can you exclude certain anatomic/tooth-related factors (e.g., CEJ, restoration margins)?
-
Explore in several planes (vertical, horizontal, oblique) to distinguish the size and nature of a questionable roughness/deposit (Fig. 13.3).
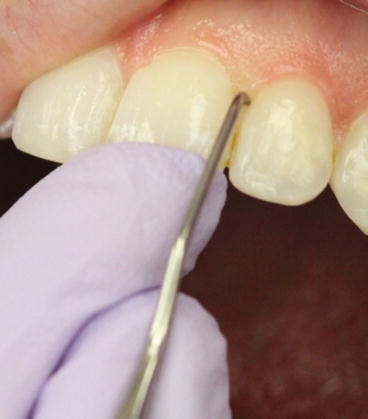 Fig. 13.3A light grasp of your instrument and a finger rest on the same arch help detection and removal of calculus (Photo courtesy of Mrs. Lorie Primosch)
Fig. 13.3A light grasp of your instrument and a finger rest on the same arch help detection and removal of calculus (Photo courtesy of Mrs. Lorie Primosch)-
Calculus deposit may take the tactile form of a lump, bump, ledge, ring, or spine; these may be detected as a relative prominence on the root which may be detected in multiple planes. This may assist differentiation from the CEJ.
-
-
Do your radiographs indicate the presence of calculus in the region?
13.5.6 What Else Could It Be?
-
CEJ
-
Tight contact catching instrument
-
Restoration margin
-
Tooth anatomy – e.g., root concavity/enamel pearl
-
Root roughness
13.5.6.1 Effectiveness of Calculus Removal (Table 13.5)
Table 13.5




Factors influencing effectiveness of calculus removal
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


