Questions to ask
Reversible pulpitis
Irreversible pulpitis or necrotic
Is the pain there all the time?
No
Yes, possibly for hours or days
Is the pain induced by anything? Sweet? Cold? Hot?
Possibly
Pain may start on its own, not induced by anything. This is a clue that the pain is spontaneous
Does the pain go away when the stimulus is removed?
Yes, pain goes away quickly (no more than 10 s or so). Pain should go away when the stimulus is removed
No, the pain lingers for a while, a minute to all day
Is the pain relieved by anything?
Pain goes away on its own upon removal of stimulus
As the infection progresses, pain relief will not always be achieved by over the counter analgesics. Patients will often report taking many tablets of acetaminophen or ibuprofen without getting relief from pain
Can you tell where the pain is coming from?
Often the patient can tell the tooth or quadrant the source of pain is coming from
The patient is not always able to point out the source of pain as referred pain is a distinct possibility
Is the pain sharp or dull?
A sharp ache from biting or chewing can be a sign of a fractured tooth or a loose restoration
Dull throbbing ache on the affected side. A dull ache that keeps a patient from chewing on that side must be differentiated from temporomandibular joint problems by performing endodontic testing on the teeth
-
Nature of pain: dull vs. sharp
-
Duration of pain: short vs. prolonged
-
Frequency of pain
-
Spontaneity
-
Stimulus: causes/relieves pain
Clinical exam: intraoral and extraoral exam to evaluate the presence of swelling, symmetry, sinus tracts, soft tissue abnormalities, periodontal status (probing, mobility), caries, and restorations
Clinical testing: clinical tests for objective information about the chief complaint
-
Thermal tests: Determines vitality and inflammation in the pulp (cold, refrigerant spray on a cotton pellet; heat, gutta-percha stick).
-
Electric pulp tester: Determines vitality of pulp.
-
Percussion: Determines presence of apical periodontitis.
-
Palpation: Determines presence of swelling or inflammation in the periodontium.
-
Probing: Determines presence of pockets or sinus tracts; note that probing to the apex of the tooth in a single spot may mean that there is a vertical root fracture.
-
Mobility: Determines presence of periodontal disease.
Radiographic analysis:
-
Bitewing radiographs of the tooth to determine restorability, proximity of caries, and restorations to the pulp (Fig. 12.1a, b)
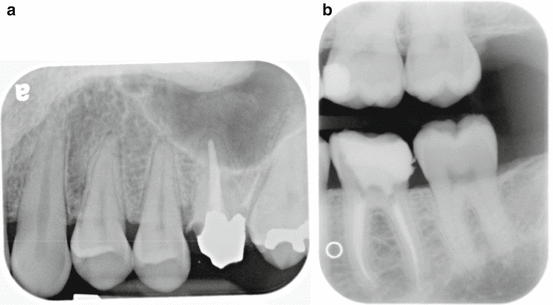 Fig. 12.1(a, b). Determine the restorability of the tooth prior to initiating endodontic treatment by evaluating the amount of tooth structure remaining. See Chap. 6 Restorative Considerations of Endodontically Treated Teeth
Fig. 12.1(a, b). Determine the restorability of the tooth prior to initiating endodontic treatment by evaluating the amount of tooth structure remaining. See Chap. 6 Restorative Considerations of Endodontically Treated Teeth -
Periapical radiographs: two angles for evaluation of periapical pathology, number of canals, presence of calcifications, resorption, etc.
Additional testing: recommended if diagnosis cannot be reached with the above steps
-
Test cavity: Cavity preparation in the suspected tooth with no anesthesia when vitality is in question. Tooth will be sensitive if vital when dentinoenamel junction is reached.
-
Selective anesthesia: Anesthetizing the maxillary or mandibular quadrant to isolate tooth when referred pain to opposing arch is suspected.
12.2 Arriving at the Diagnosis
Arriving at a diagnosis can be very difficult especially in patients with multiple carious lesions. Careful endodontic testing and clinical exam are essential for proper diagnosis (Fig. 12.2).
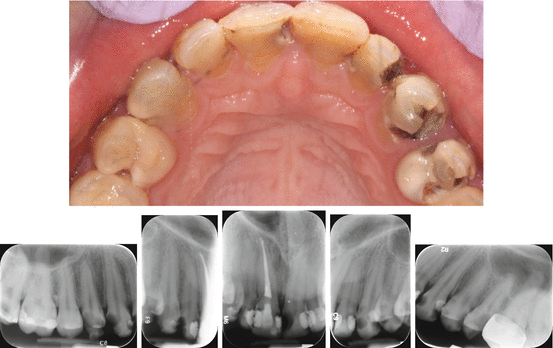

Fig. 12.2
Extensive carious lesions observed clinically and radiographically
The patient’s medical/dental history and subjective and objective information should be combined to arrive at a diagnosis which should include a pulpal and periapical diagnosis. The American Association of Endodontics approved terminology should be utilized for diagnosis (Glickman 2009) (Tables 12.2 and 12.3).
Table 12.2
Presumptive clinical diagnosis of pulpal/periapical conditions
|
Classification
|
Signs/symptoms
|
Test results
|
|---|---|---|
|
PULPAL:
|
||
|
Normal pulp
|
None
|
Normal responses to thermal and EPT – responses are definite and well defined and cease on removal of stimulus
|
|
Reversible pulpitis
|
Requires stimulus to evoke a painful response of short (seconds) duration. Pain is mild and with short lingering sensation. Negative for radiographic changes
|
Hyperresponsive (slightly exaggerated) and/or slightly prolonged (seconds) to cold and/or hot, EPT is within normal limits
|
|
Symptomatic irreversible pulpitis
|
Induced pain – usually more intense and lingers well beyond removal of stimulus (i.e., temperature changes). History of spontaneous pain, usually severe; can be constant or intermittent
|
Hyperresponsive (grossly exaggerated) and prolonged (>10 s) to cold and/or hot. EPT is within normal limits
|
|
Asymptomatic irreversible pulpitis
|
None
|
Clinically and radiographically the caries extends to the pulp. EPT is within normal limits. Thermal tests maybe within normal limits
|
|
Pulpal necrosis
|
Usually asymptomatic. May have history of episodic, prolonged, spontaneous, or provoked pain during irreversible pulpitis stage
|
EPT, no response; thermal tests, no response
|
|
Previously treated
|
Radiographic evidence of root canal filling material in the canal
|
EPT, no response; thermal tests, no response
|
|
Previously initiated
|
Radiographic evidence of access into the pulp cavity
|
EPT, may or may not respond; thermal, may or may not respond
Stay updated, free dental videos. Join our Telegram channel
VIDEdental - Online dental courses
 Get VIDEdental app for watching clinical videos
Get VIDEdental app for watching clinical videos

|