Figure 2.42 Preoperative frontal T1-weighted MRI of right TMJ showing distension of the joint capsule and multiple loose bodies in an intraarticular soft tissue mass (arrows) surrounding the condyle (C).
I. Diagnosis/Diagnoses
Expanded DC/TMD
- Synovial chondromatosis, right TMJ.
DC/TMD
- Degenerative joint disease, right TMJ.
- Masticatory muscle myalgia.
J. Case Assessment
- The minor swelling that was moderately sore to palpation over the right TMJ without any signs of infection, the “bumpy” motion palpated over the joint, and crepitation and occasional clicking in the right TMJ indicated intraarticular changes.
- The somewhat reduced maximal mouth opening and the difference in laterotrusive movements with reduced lateral movement to the left supported the suspicion of a right intraarticular obstacle.
- Medically the patient was healthy except for a moderate hypertension, which could not explain the patient’s actual symptoms.
- Tentative diagnoses could be myalgia because of the painful masticatory muscles on the right side, combined with degenerative condylar changes on the right side indicated by the crepitation in that joint. The slight swelling might further indicate edema in the joint capsule and/or an arthritis with excess of fluid in the joint. In addition, the occasional clicking in the right joint might indicate intraarticular loose bodies. As synovial chondromatosis has been reported to be the most common pseudotumor in the TMJ, with the symptoms exhibited in this patient an extended examination with MRI seemed to be indicated to reveal any intraarticular soft tissue changes.
K. Evidence-based Treatment Plan including Aims
- The aim is to remove the chondroid changes.
- The treatment options for synovial chondromatosis are open or arthroscopic surgery. The aim is to reduce/eliminate pain and normalize reduced mouth opening if present. Open surgery is most frequently used and usually involves exposure of the joint via a preauricular approach. Free fragments should be removed, paying attention to the anterior and medial recess where a number of fragments may hide (Figure 2.43). Synovial areas with evident chronic inflammation may be resected and if the disc is severely deformed or perforated it can be excised
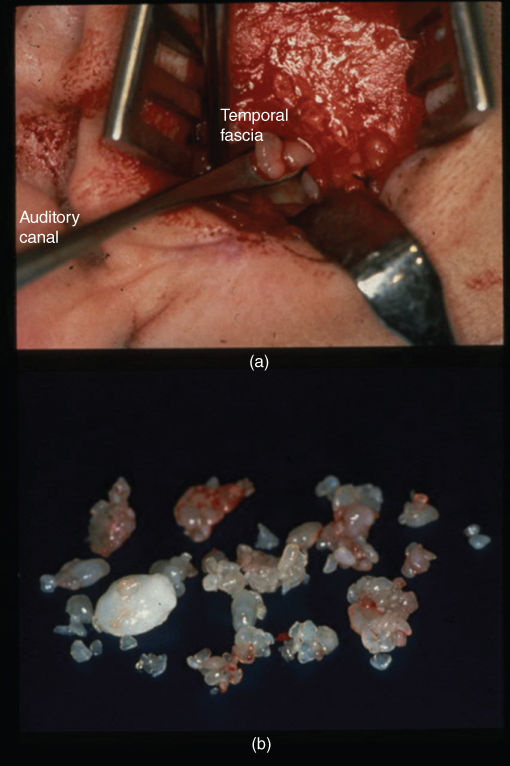
Figure 2.43 Preauricular incison with turned-down lateral joint capsule. Loose bodies (arrow) visible after opening of the upper joint compartment (A). Extirpated loose bodies of varying size and shape all found in the upper joint compartment (B).
L. Prognosis and Discussion
- The prognosis of open surgical removal via a preauricular incision seems to be good, and relapse is very seldom reported. Surgical removal of the pathological changes with arthroscopic technique, which is less invasive, may be used as an alternative to open surgery but a disadvantage with this method is that it is difficult to retrieve major intraarticular loose bodies or a destroyed disc (Lim et al., 2011; Figure 2.44).
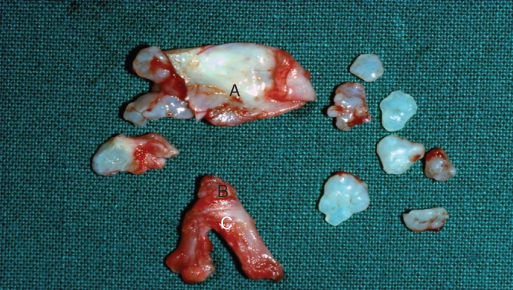
Figure 2.44 A and B indicate two halves of an extirpated surgically divided deformed disc with a major perforation (C) surrounded by loose cartilage bodies.
Background Information
- Synovial chondromatosis is a rare condition that usually affects a single joint; for example, the knee, hip, or elbow, but the TMJ may also be affected. Most cases of synovial chondromatosis occur in middle-aged people, and concerning the TMJ it has been reported to be more common in women than in men (Holmlund et al., 2003). In a review of 285 pseudotumors and tumors of the TMJ published in 181 articles of 15 journals included in Journal Citation Reports the distribution of pseudotumors was clearly the most numerous, representing over two-thirds of the lesions. Synovial chondromatosis accounted for 61.8% of the pseudotumors (Poveda-Roda et al., 2013)
- Two forms of the disease have been recognized: primary and secondary. In the primary form, which is uncommon, the etiology is not known; however, a response to repetitive, low-grade trauma has been proposed. The secondary synovial chondromatosis is more common and arises as a result of an inflammatory or noninflammatory arthropathy (Coleman et al., 2013).
-
Synovial chondromatosis is a non-neoplastic disease characterized by metaplasia of the connective tissue leading to chondrogenesis in the synovial membrane (Matsumura et al., 2012). Part of the chondrified tissue enters the
joint cavity and undergoes chronic calcification, leading to formation of a joint loose body of cartilage tissue (Yokota et al., 2008). Milgram (1977) divided the process into three stages. In stage 1 there is active intrasynovial disease only, with no loose bodies; in stage 2, transitional lesions with both active intrasynovial proliferation and free loose bodies occur; and in stage 3, multiple free osteochondral bodies with no demonstrable intrasynovial disease can be observed. (Milgram, 1977). Even a major single loose body can be formed (Figures 2.45 2.46, and 2.47).
- Concerning the risk of malignancy of synovial chondromatosis, there are somewhat divergent opinions. According to Pau et al. (2013) the disease is considered to be metaplastic and shows no malignant tendencies, but can become locally aggressive, erode the cranial base, and even spread intracranially, whereas according to Coleman et al. (2013), malignancy, even if very rare, can arise in synovial chondromatosis or de novo within the synovial membrane.
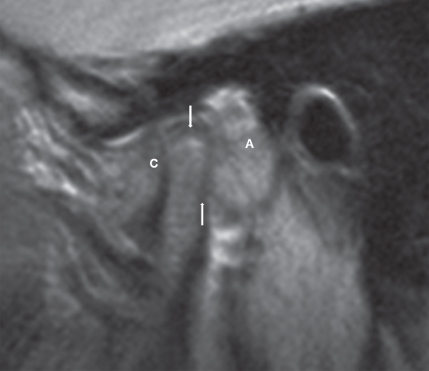
Figure 2.45 Preoperative lateral T1-weighted MRI of a TMJ showing a major intraarticular soft tissue mass (arrows) posterior to the condyle (C) and anterior to the auditory canal (A).
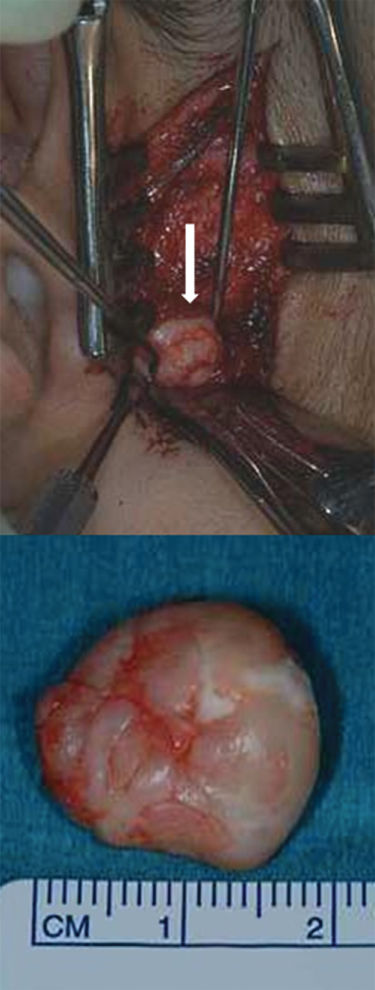
Figure 2.46 Extirpation via a preauricular approach of an intraarticular loose body (arrow) shown in Figure 2.45.
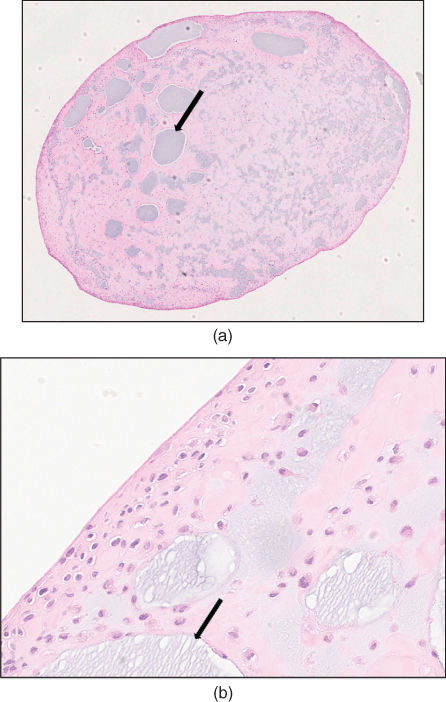
Figure 2.47 (A) Section of a roundish nodule with variable cellularity and pools of fluid (arrow). (B) Section from the periphery of the nodule in (A) showing a hypercellular area with fairly small chondrocytes and pools of fluid (arrow). H&E stain.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


