Masticatory Muscle Disorders
A: Muscle Pain
Case 3.1
Myalgia with Limited Emotional Disturbance
Karina Bendixen and Peter Svensson
A. Demographic Data and Reason for Contact
- A 37-year-old female Caucasian referred from her general dentist due to pain in the jaw and temple.
B. Symptom History
- Pressing, aching, and spreading pain for about 9–10 months in the jaw, the ears, and the temples (Figure 3.1).
- Pain comes and goes.
- Pain 2–3 days per week.
- Pain is worsened when chewing hard foods.
- Pain not affected by stress.
- Pain is described as mild aching and tender. Present pain intensity: 3 (NRS 0–10). Average pain intensity: 4. Worst pain intensity: 6.
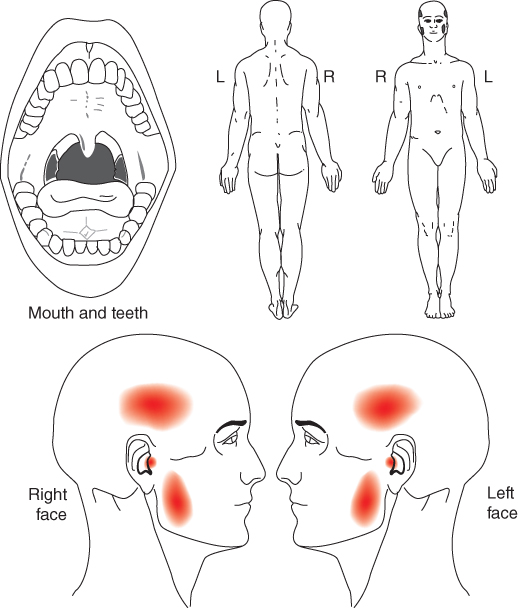
Figure 3.1 Pain drawing by patient.
C. Medical History
- Healthy – no known medical conditions.
- No other pain complaints.
- No known allergies.
- No previous relevant hospitalizations or surgeries.
- No head trauma.
- Regular check-up at her private general dentist.
- Orthodontic treatment with fixed appliances as adolescent.
- No other major dental treatments.
D. Psychosocial History
- Married, two children.
- Secretary in full-time work.
- Middle socio-economic status.
- Rarely sports or exercise.
- Low disability with low pain intensity (GCPS).
- Limitations in chewing tough foods (JFLS).
- Report of some parafunctional activity during daytime (OBCL).
- No symptoms of anxiety, depression, or other physical symptoms (PHQ-9, GAD-7, PHQ-15).
E. Previous Consultations and Treatments
- ENT specialist due to ear pain, but no disorder was detected.
- Medication, analgesics (over the counter): paracetamol (acetaminophen) 2 g three times per week; some pain relief.
- Stabilization splint nighttime use prescribed by general dentist because of bruxism; no effect on pain.
F. Extraoral Status
Face
- Normal appearance and body-mass index (BMI) within normal limits.
- No asymmetries, swelling, or redness.
- No neurological abnormalities upon screening.
- No somatosensory or motor function abnormalities.
Temporomandibular joint
- No noise/sounds on standardized palpation.
- No pain on movements or standardized palpation.
Masticatory muscles
- Bilateral familiar masseter pain on palpation.
- Bilateral familiar temporalis pain on palpation.
Jaw movement capacity
- Open movements: straight. Pain-free opening: 31 mm. Maximum unassisted/assisted opening: 41/43 mm. No pain.
- Lateral movements: right excursion, 10 mm; left excursion, 11 mm. No pain.
- Protrusion: 9 mm. No pain.
Neck and shoulders
- Mild pain on palpation of trapezius muscles.
G. Intraoral Status
Soft tissues
- Moderate tongue scalloping.
- Teeth impressions in buccal mucosa.
Hard tissues and dentition
- Full arch dentition (28 teeth), few composite fillings. Wear grade 1. No dental caries or periodontal disease.
- Neutral sagittal relations. Horizontal overlap: 2 mm. Vertical overlap: 2 mm. No midline deviation.
Occlusion
- Stable.
Saliva
- Normal quantity/quality.
- Good oral hygiene.
H. Additional Examinations and Findings
- Not considered needed.
I. Diagnoses
- Myalgia.
- Subtype local myalgia of masseter and temporalis muscles.
J. Case Assessment
- The physical examination revealed jaw muscle pain and temple headache. The pain is modified by jaw function and fulfills the criteria for the two common pain TMDs: myalgia and headache attributed to TMD. TMD etiology is considered to be multifactorial. Several risk factors are identified, of which in this case the female gender and the age seem to be of main relevance.
- From the history and the physical examination it is apparent that she suffers from a mild type of TMD since the pain level is on average moderate; however, several days a week she has no pain at all. Also, no severe pain comorbidities are present and mild analgesics provides some pain relief. From both physical and psychosocial aspects she is generally healthy.
K. Evidence-based Treatment Plan including Aims
- The overall aims are to eliminate or as a minimum reduce the pain level and numbers of days with pain and also to increase jaw function in a noninvasive manner. This is by low-intensity management and active patient involvement.
- First management steps are information, counselling, and education, including a tailored self-care program and approaches (exercise, awareness of jaw posture, “lips closed – teeth apart,” avoid parafunctional activity, etc.). Discontinue oral splint usage, since no effect on pain. Also, instruction in physiotherapy exercises “self-performed” (jaw stretching, relaxation, heat (diathermy), massage).
- If additional management approaches are needed, pharmacotherapy by the use of topical NSAIDs could also be applied on muscles before massage.
- Monitoring systemic analgesia (paracetamol) usage to avoid medication overuse headaches is indicated.
L. Prognosis and Discussion
- Reversible condition with good prognosis; however, good patient cooperation necessary.
- Based on anamnestic information the patient appears to cope well with minimal influence of and consequence for the psychosocial status.
- Tailored self-care program requires monitoring and adjustments as needed.
- Since the headache is attributed to TMD, the prediction is that management of the TMD will also result in headache remission.
Background Information
- TMD prevalence 3–15%. Peak age 20–45 years. TMD pain prevalence 4.6% (ratio women : men, 2 : 1). Myofascial TMD pain most frequent TMD diagnosis (42%). Myofascial TMD common comorbid conditions (e.g., primary headaches – migraine and tension-type headache) (Ballegaard et al., 2008; Schiffman et al., 2014; Speciali and Dach, 2015; Fernández-de-Las-Peñas and Svensson, 2016).
- Etiology and pathology of TMD are unclear but multifactorial, including some degree of peripheral and central sensitization and also involvement of endogenous modulatory systems. Genetical predisposition to some degree cannot be excluded.
- Occlusion and bruxism are considered as minor risk factors (Michelotti and Iodice, 2010; Fernández-de-Las-Peñas and Svensson, 2016).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


