White
Red
Ulcers
Raised soft tissue (bumps)
Pigmented
1. Leukoplakia
1. Geographic tongue
1. Squamous carcinoma
1. Pyogenic granuloma
1. Varicosity
2. Lichen planus
2. Desquamative gingivitis
2. Aphthous stomatitis
2. Peripheral giant cell granuloma
2. Amalgam tattoo
3. Leukoedema
3. Candidiasis
3. Herpetic stomatitis
3. Fibroma
3. Macule
4. Cheek/tongue chewing
4. Erythroplakia
4. Traumatic
4. Peripheral ossifying fibroma
5. Candidiasis
5. Mucocele
6. Papilloma
7. Lymphoepithelial cyst
Table 14.2
Hard tissue lesions
|
Radiolucent
|
Radiopaque
|
|---|---|
|
1. Periapical granuloma
|
1. Odontoma
|
|
2. Periapical cyst
3. Dentigerous cyst
|
2. Cemento-osseous dysplasia
|
|
4. Odontogenic keratocyst (keratocystic odontogenic tumor)
|
3. Idiopathic osteosclerosis
|
|
5. Lateral periodontal cyst
6. Ameloblastoma
|
4. Condensing osteitis
|
|
7. Simple bone cyst (traumatic bone cyst)
|
|
|
8. Nasopalatine duct cyst
|
14.2 White Soft Tissue Lesions
14.2.1 Leukoplakia
14.2.1.1 Synonyms
-
Leukokeratosis; erythroleukoplakia
14.2.1.2 Introduction
-
A white lesion of unknown cause which is considered precancerous (Warnakulasuriya 2007).
-
It is a common premalignant lesion of the oral mucosa.
-
Risk factors include consumption of alcohol and tobacco, microorganisms, and trauma.
-
All leukoplakias should be assessed histopathologically and treated vigorously if dysplasia is prominent.
14.2.1.3 Demographics
-
Strong male predilection
-
Female predilection in regional populations where women use tobacco products more than men
-
Seen more frequently in older individuals (average age 60 year)
14.2.1.4 Appearance (Fig. 14.1a–d)
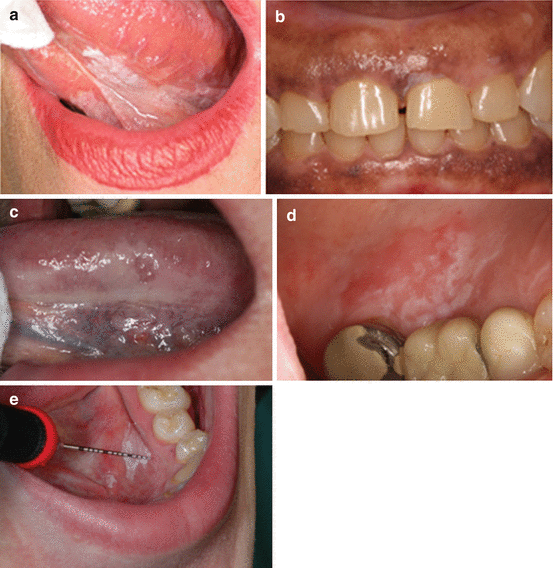
Fig. 14.1
(a) Thick extensive leukoplakia of ventral tongue and floor of mouth in a nonsmoker. Biopsy revealed significant epithelial dysplasia. (b) Small area of somewhat verrucous leukoplakia on the maxillary facial gingiva. Patient is a smoker. No dysplasia detected upon microscopic examination. (c) Thin leukoplakia on the lateral/ventral border of the tongue. Biopsy revealed mild epithelial dysplasia. (d) Irregular erythroleukoplakia of the palatal mucosa. Biopsy revealed epithelial dysplasia. (e) An irregular bordered rough (verrucous) surfaced distinct leukoplakic lesion on the floor of the mouth in a heavy smoker
-
A clinical term defined as a predominantly white lesion of the oral mucosa that cannot be characterized clinically and pathologically as any other disease; a diagnosis of exclusion.
-
The lip vermillion, gingiva, and buccal mucosa are the sites of predilection; the tongue, lip vermillion, and floor of the mouth lesion account for 90 % of leukoplakia dysplasia/carcinoma.
-
Classified as homogenous, nodular (speckled), verruciform, and proliferative verrucous leukoplakia (van der Waal 2010).
-
Homogenous: well-demarcated uniform white plaques with or without fissuring.
-
Nonhomogeneous are predominantly mixed red and white lesions in which keratotic white nodules or patches are distributed over an atrophic erythematous background.
-
Verruciform: presence of thick white lesions with papillary surface; lesions are heavily keratinized and are seen mostly in older adults.
-
Proliferative verrucous: special type of leukoplakia with extensive papillary or verrucous white plaques that tend to slowly involve extensive mucous surfaces with an invariable transformation into squamous cell carcinoma or verrucous carcinoma over a period of several years.
14.2.1.5 Clinical Differential Diagnosis
-
Lichen planus
-
Candidiasis
14.2.1.6 Treatment and Prognosis
-
No current consensus.
-
Repeat follow-up visits and biopsies are essential.
-
Each clinical appearance or phase of leukoplakia has a different potential for malignant transformation.
-
Speckled leukoplakia carries the highest average transformation potential, followed by verrucous leukoplakia.
-
Homogeneous leukoplakia carries the lowest risk.
-
For dysplastic leukoplakia, the clinician must consider the histologic grade when planning treatment and follow-up.
-
In general, the greater the degree of dysplasia, the greater the potential for malignant change.
-
Additionally, multiple factors play a role in determining the optimum management procedure. These factors include the persistence of the lesion over many years, the development of leukoplakia in a nonsmoker, and the lesion’s occurrence on high-risk areas such as the floor of the mouth, the soft palate, the oropharynx, or the ventral surface of the tongue.
-
Non-surgical: carotenoids (beta-carotene, lycopene), vitamins A, C, and K, fenretinide, bleomycin, and photodynamic therapy (Ribeiro 2010).
-
Surgical: conventional surgery, electrocauterization, laser ablation, or cryosurgery.
-
Histopathologic evaluation for dysplasia/carcinoma should be done for nonhomogeneous lesion.
14.2.2 Lichen Planus (LP)
14.2.2.1 Synonyms
-
Lichenoid mucositis
14.2.2.2 Introduction
-
A chronic immunologically mediated mucocutaneous condition of unknown cause resulting from a cell-mediated degeneration of the basal cell layer of the epithelium (Au 2013).
-
Affects 0.1–4.0 % of the general population.
-
Oral lesions may be chronic, remitting, and relapsing with varying degrees of morbidity (Giunta 2001).
-
Lesions range from asymptomatic to severely painful in nature.
-
Genetic involvement is yet to be determined.
-
The World Health Organization’s (WHO) criteria describe lichen planus as a condition predisposed to malignant transformation.
14.2.2.3 Demographics
-
Female predominance seen
-
Most patients between 30 and 60 years of age
14.2.2.4 Appearance (Fig. 14.2a–e)
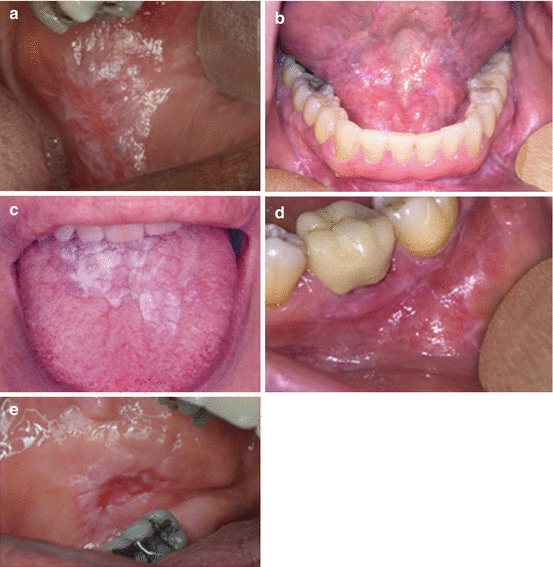
Fig. 14.2
(a) Classic reticular LP on the buccal mucosa. (b) Reticular LP on the buccal vestibule as well as the floor of the mouth. (c) Plaque-like LP on the dorsum of the tongue. (d) Erosive erythematous involvement of the posterior mandibular gingiva with striations is typical of LP. (e) Central ulcerative lesion of the posterior buccal mucosa rimmed by white striations typical of erosive LP
-
Classified into three main forms: reticular, erosive, and atrophic (or erythematous).
-
Reticular: most common type; present as white, slightly raised plaques or papules with interlacing white lines (Wickham striae) on an erythematous background; lesions are asymptomatic; common sites include the buccal mucosa, tongue, gingivae, and vestibule.
-
Erosive: atrophic, with areas of ulceration, erythema, and keratotic white striae; symptoms range from mild to severe pain.
-
Atrophic (erythematous): mucosal atrophy; red, diffuse lesion; pain ranges from mild to severe.
-
Buccal mucosa is the most common sites where lesions are usually bilateral.
-
Other sites include the tongue, vestibule, and gingiva. However, any part of the oral mucosa maybe involved.
-
Lichen planus on the dorsum of the tongue often appears plaque-like.
-
Direct immunofluorescence demonstrates a shaggy band of fibrinogen in the basement membrane zone in 90–100 % of cases.
-
Malignant transformation of lichen planus is highly controversial; malignant transformation is more likely in erosive lesions.
-
The reported incidence of malignant transformation is anywhere from as low as 0.4 % to as high as 1.5 % (Fitzpatrick et al. 2014).
14.2.2.5 Clinical Differential Diagnosis
-
Drug-induced lichenoid reaction
-
Contact mercury hypersensitivity
-
Chronic graft-versus-host disease
-
Erythema multiforme
-
Lupus erythematosus
-
Candidiasis
-
Mucous membrane pemphigoid
-
Squamous cell carcinoma
-
Granulomatous lichenoid mucositis (affects upper lip)
-
Leukoplakia resembling keratotic lichen planus
-
Desquamative gingivitis (erosive LP)
14.2.2.6 Treatment and Prognosis
-
May be difficult to treat.
-
Lesions tend to regress and reappear in an unpredictable fashion.
-
Reticular lesions: No treatment needed.
-
Symptomatic erosive and atrophic lesions: corticosteroids recommended; strong topical corticosteroids usually sufficient (fluocinonide, betamethasone, clobetasol); healing induced within 1–2 weeks; systemic corticosteroids generally not necessary; insufficient evidence that to support the superiority of any specific corticosteroid (Usatine and Tinitigan 2011, Lodi et al. 2012).
-
Recalcitrant cases: topical retinoids, tacrolimus, mycophenolate mofetil, or cyclosporine has been used; side effects and cost may be prohibitive.
14.2.3 Leukoedema
Synonyms: None
14.2.3.1 Introduction
-
A development alteration, of unknown cause, which is considered to be a variation of normal anatomy rather than a disease (Martin and Crump 1972)
14.2.3.2 Demographics
-
Bilaterally on the buccal mucosa.
-
Less frequent sites include the labial mucosa, soft palate, and floor of the mouth.
-
Lesions have been reported in up to 90 % of black adults and 50 % of black children (Canaan and Meehan 2005).
-
The incidence in white persons in different studies is highly variable (10–80 %) possibly due to darker coloration of the mucosa in blacks, rendering the alteration more visible (Bhattacharyya et al. 2003).
-
Similar changes have also been reported on the vaginal and laryngeal mucosa.
14.2.3.3 Appearance (Fig. 14.3)
-
Buccal lesions are poorly defined diffuse, gray-white, opalescent macules which cannot be rubbed off.
-
Occasionally, the lesion may present as fine grooves or folds.
-
Mucosal changes are not usually noticeable until adolescence.
-
Some studies relate the severity of the lesion to smoking.
-
Clinical diagnosis is made easily because the lesion disappears or fades upon stretching the mucosa.
14.2.3.4 Clinical Differences Diagnosis
-
Frictional keratosis
-
Snuff dippers keratosis
-
White sponge nevus
-
Witkop’s disease
-
Clinical stretch test helps distinguish leukoedema from other lesions
14.2.3.5 Treatment and Prognosis
-
No treatment required; it is a benign condition.
-
Does not change significantly even after 20–30 years.
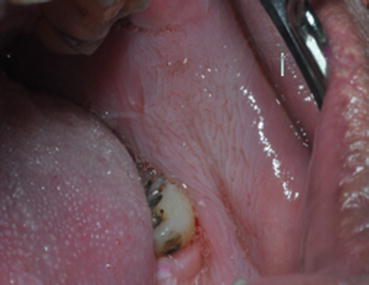 Fig. 14.3Diffuse pale gray-white change of the buccal mucosa in a middle-aged male patient
Fig. 14.3Diffuse pale gray-white change of the buccal mucosa in a middle-aged male patient
14.2.4 Cheek/Tongue Chewing
14.2.4.1 Synonyms
-
Morsicatio mucosae oris; morsicatio buccarum; morsicatio labiorum; morsicatio linguarum
14.2.4.2 Introduction
-
“Morsicatio” represents changes in the mucosa covering the tongue, buccal mucosa, or lips caused by chronic tissue irritation, such as biting, sucking, or friction (Glass and Maize 1991).
-
Etiology unknown (Allen and Camisa 2008).
-
Self-induced injury which may be associated with stress or mental illness (Scully and Hegarty 2010).
14.2.4.3 Demographics
-
Can be seen in any age and gender
-
Increased prevalence in women older than 35 years of age (Woo and Lin 2009)
-
Known occupational association in glassblowers
14.2.4.4 Appearance (Fig. 14.4a, b)
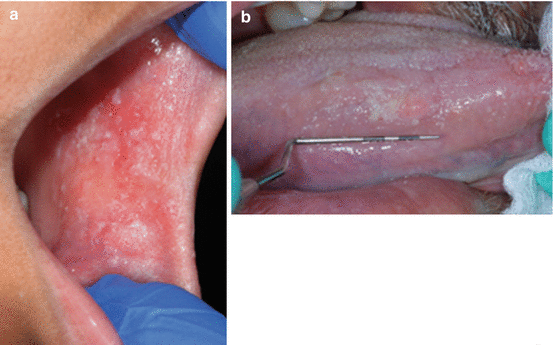
Fig. 14.4
(a) CK Chg. Typical “shredded” appearance of the cheek mucosa in a 10-year-old girl. (b) CK Chg. White rough area on the lateral border of the tongue in a 65-year-old male
-
Thick rough white asymptomatic areas intermixed with red and ulcerated zones of oral mucosa (Woo 2010).
-
Superficial areas may be peeled off or removed by patient.
-
Anterior buccal mucosa is affected most frequently; unilaterally or bilaterally.
-
Lateral border or tongue and lips may also be involved.
14.2.4.5 Clinical Differential Diagnosis
-
Leukoedema
-
White sponge nevus
-
Snuff dipper’s keratosis
-
Chemical keratosis
-
Oral hairy leukoplakia (Tomás Carmona et al. 2000)
14.2.4.6 Treatment and Prognosis
-
If other conditions mentioned above are in consideration, an incisional biopsy may be required.
-
No treatment required, other than mitigation of trauma.
-
Complete resolution takes place upon resolution of chronic trauma.
-
No malignant potential.
14.2.5 Candidiasis (See Candidiasis in Red Lesions)
-
Condensing osteitis presents as a radiopaque/radiolucent lesion between the apex of teeth #29 and 30.
-
Large condensing osteitis between the apex of teeth #30 and 31.
14.3 Red Soft Tissue Lesions
14.3.1 Geographic Tongue
14.3.1.1 Synonyms
-
Erythema migrans; benign migratory glossitis; wandering rash of the tongue; erythema areata migrans; stomatitis areata migrans
14.3.1.2 Introduction
14.3.1.3 Demographics
-
Affects all ages
-
No gender predilection noted
14.3.1.4 Appearance (Fig. 14.5a, b)
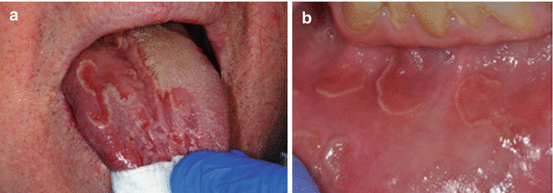
Fig. 14.5
(a) Erythematous zones surrounded by whitish-yellow circinate borders. (b) Patient with erythema migrans of the labial mucosa. He also has classic tongue lesions
-
Multiple well-demarcated asymptomatic erythematous areas surrounded partially or completely by a yellow-white slightly raised serpentine line seen.
-
The erythematous zones on tongue represent atrophy of the filiform papillae.
-
Anterior two-thirds of dorsal surface of the tongue most frequent site.
-
Lesions may also involve the lateral and ventral surfaces of the tongue (Menni et al. 2004).
-
Other oral mucosal surfaces such as labial, buccal, floor of mouth, and palatal areas may be involved in rare cases (Assimakopoulos et al. 2002).
-
Lesions develop in one area, heal in days to weeks, and then develop in a different area,
14.3.1.5 Clinical Differential Diagnosis
-
Pyostomatitis vegetans
-
Stomatitis herpetiformis
14.3.1.6 Treatment and Prognosis
-
No treatment required
-
Symptomatic lesions treated with topical steroids (Menni et al. 2004)
14.3.2 Desquamative Gingivitis
14.3.2.1 Synonyms
-
None
14.3.2.2 Introduction
-
A clinical term common to a wide number of disorders characterized by erythema, desquamation, erosion, and blistering of attached and marginal gingiva (Rees 2011).
-
Most common conditions include lichen planus, mucous membrane pemphigoid, and pemphigus (Endo et al. 2008).
-
Lichen planus and mucous membrane pemphigoid constitute 80 % of cases.
-
Histopathological examination and direct immunofluorescence testing essential to establish a definitive diagnosis.
14.3.2.3 Demographics
-
Seen in adults
-
Greater frequency in women
-
Can affect gingiva anywhere in the oral cavity (Nisengard and Neiders 1981)
14.3.2.4 Appearance (Fig. 14.6a, b)
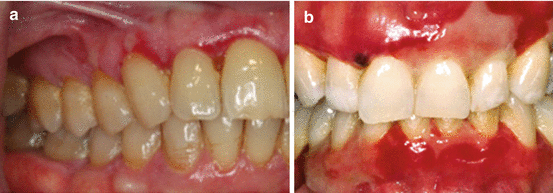
Fig. 14.6
(a) Ulcerative and erythematous areas of the facial gingiva in a 62-year-old male. Biopsy revealed erosive lichen planus. (b) Extensive desquamation of the gingiva on both arches with areas of bloody blisters in a patient with benign mucous membrane pemphigoid
-
Usually involved gingiva appears erythematous and inflamed and exhibits sloughing (Scully and Porter 1997).
-
Pain and discomfort often noted with the condition.
-
Nikolsky sign is often positive (separation of intact superficial epithelium under firm lateral pressure).
14.3.2.5 Clinical Differential Diagnosis
-
Traumatic lesions
-
Thermal burns
-
Plasma cell gingivitis
-
Radiation mucositis
-
Erythroplakia
14.3.2.6 Treatment and Prognosis
-
A definitive diagnosis of the specific disease or disorder is needed to provide adequate treatment (Guiglia et al. 2007).
-
Requires elimination or control of local irritants
-
Many cases respond to topical corticosteroids and plaque control.
-
Lesions tend to wax and wane and may go into remission.
-
Periodic follow-up and long-term care of patients are essential.
14.3.3 Candidiasis
14.3.3.1 Synonyms
-
Moniliasis; yeast infection; thrush
14.3.3.2 Introduction
-
Yeastlike fungal organisms of the genus Candida of which Candida albicans is the most prevalent species in both health and disease (Barnett 2008).
-
Among the most common human pathogens.
-
Infection is more common when individual becomes immunocompromised.
-
Systemic infections are rare but serious when they do occur.
14.3.3.3 Demographics
-
Commensal carriage of this species occurs in approximately 50 % of individuals.
-
Predisposing factors for infection include local host factors (denture use, steroid inhaler use, reduced salivary flow, nutritional deficiencies) and systemic host factors (infants and elderly, diabetes mellitus, immunosuppression, broad-spectrum antibiotics) (Samaranayake et al. 2009, Soysa et al. 2006).
-
Seen across all ages from newborn to older adults.
14.3.3.4 Appearance (Fig.14.7a–e)
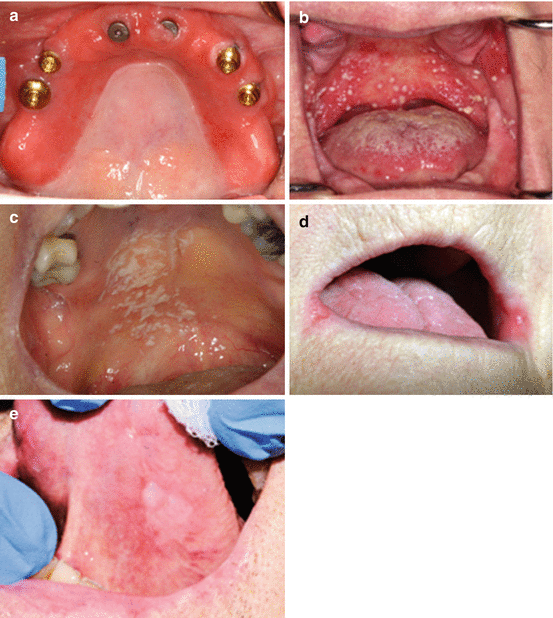
Fig. 14.7
(a) Denture sore mouth. (b) Pseudomembranous candidiasis in an elderly patient with recent history of using antibiotics. (c) Pseudomembranous candidiasis. (d) Angular cheilitis. (e) Hyperplastic candidiasis on the ventral tongue with associated traumatic keratosis
-
Presents clinically in four forms: pseudomembranous, acute erythematous, chronic erythematous, and chronic hyperplastic.
-
Pseudomembranous: characterized by superficial white plaques that are easily removed by gentle rubbing of the lesion (diagnostic feature), leaving a erythematous base; seen in neonates and the elderly at rates of 5–10 % (Rüping et al. 2008).
-
Acute erythematous: aka “antibiotic sore mouth”; results from broad-spectrum antibiotics use; painful lesion.
-
Chronic erythematous: aka “denture stomatitis”; causes include wearing dentures 27/7, ill-fitting dentures, and poor oral hygiene; usually asymptomatic (Webb et al. 2005).
-
Hyperplastic: characterized by white plaques; do not rub off; histological examination needed for a definitive diagnosis; potential for the development of squamous cell carcinoma at lesional sites is of concern; cause of change unclear.
-
Angular cheilitis: commissural erythema; candida along with bacterial infection implicated.
-
Median rhomboid glossitis: erythematous candidiasis involving the dorsal tongue.
14.3.3.5 Clinical Differential Diagnosis
-
Leukoplakia
-
Erythroplakia
-
Traumatic erythema
14.3.3.6 Treatment and Prognosis
-
Traditional antifungal agents: topical (nystatin, amphotericin, miconazole, clotrimazole) and systemic (ketoconazole, fluconazole, itraconazole).
-
Denture care: remove during sleep and immerse in a suitable antimicrobial cleansing agent; hot water-immersed dentures have been of benefit in the treatment of denture stomatitis.
14.3.4 Erythroplakia
14.3.4.1 Synonyms
-
Erythroplasia; erythroplasia of Queyrat
14.3.4.2 Introduction
-
A red lesion of unknown cause which is considered premalignant.
-
Has the highest rate of malignant transformation as compared to other oral premalignant conditions; in one study, 91 % of lesional biopsies showed dysplasia, carcinoma in situ, or carcinoma (Shafer and Waldron 1975).
-
Far less common than leukoplakia (van der Waal 2011).
-
Lesions are frequently overlooked (Reichart and Philipsen 2005).
14.3.4.3 Demographics
-
Typically occurs in the middle aged and the elderly.
-
Most commonly involves the floor of the mouth, ventral tongue, soft palate, and tonsillar fauces (Villa et al. 2011).
-
Etiology is poorly understood (van der Wall 2009).
-
Predisposing factors include tobacco and alcohol.
-
Candida albicans has often been demonstrated as secondary infection; positive correlation between the presence of dysplastic epithelium and candidal hyphae has not been shown.
-
Role of human papilloma virus is controversial.
14.3.4.4 Appearance (Fig.14.8a, b)
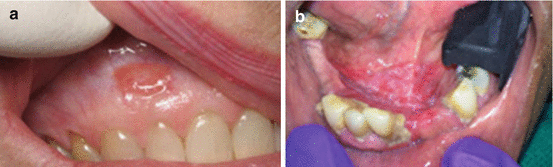
Fig. 14.8
(a) Distinct erythroplakic patch on the maxillary gingiva in a 65-year-old female. Patient is a nonsmoker. Biopsy revealed squamous cell carcinoma. (b) Speckled red and white lesion on the floor of the mouth in a 72-year-old male. Patient is a heavy smoker. Biopsy revealed squamous cell carcinoma
-
A clinical term defined as any lesion of the oral mucosa that presents as bright red velvety plaques which cannot be characterized clinically or pathologically as any other recognizable condition; a diagnosis of exclusion.
-
Classified as homogenous, erythroplakia interspersed with patches of leukoplakia and granular or speckled.
-
Homogenous: smooth and velvety surface.
-
Erythroplakia interspersed with patches of leukoplakia: numerous, small irregular foci of leukoplakia dispersed in the erythroplakic patch.
-
Granular or speckled: irregular, red granular surface interspersed with white or yellow foci.
-
May be multicentric; rarely covers extensive areas of the mouth.
-
Patients in whom carcinoma in situ has been diagnosed generally aware of an alteration in the involved site for at least 2.7 years prior to biopsy.
14.3.4.5 Clinical Differential Diagnosis
-
Fungal infections (oral candidiasis, histoplasmosis)
-
Bacterial infections (tuberculosis)
-
Atrophic lichen planus
-
Lupus erythematosus
-
Pemphigus
-
Pemphigoid
14.3.4.6 Treatment and Prognosis
-
Due to high malignant transformation rate, early detection and treatment are of utmost importance (Yang et al. 2015).
-
Observation for 1–2 weeks following the elimination of suspected irritants is acceptable.
-
Thereafter, prompt biopsy is mandatory for lesions that persist.
-
Epithelial dysplasia or carcinoma in situ warrants complete removal of lesion.
-
Due to high recurrence rates and multifocal involvement, follow-up is mandatory.
14.4 Ulcers in the Soft Tissue
14.4.1 Squamous Cell Carcinoma
14.4.1.1 Synonyms
-
None
14.4.1.2 Introduction
-
It is the most common malignancy of the oral cavity; accounts for more than 90 % of all oral cancers (Chaturvedi 2012).
-
A recent increase in tongue cancer in young females seen (20–44 years); frequently without alcohol or tobacco exposure (Deschler et al. 2014 and Muller et al. 2008).
-
Major risk factors: tobacco, alcohol, combined alcohol and tobacco (synergistic effect), betel quid, and high-risk human papilloma virus (HPV-16).
-
Other risk factors: Candida, Neisseria, and streptococci (role still controversial), dietary factors (vitamin D deficiency implicated), immune status, environmental pollutants (arsenic, chromium, nickel), occupational exposures (construction, painting, carpentry, metalworking), and heritable conditions (Fanconi anemia, dyskeratosis congenita, and Bloom syndrome)
14.4.1.3 Demographics
-
Most often seen in older population (average age 62 years); duration of change approximately of 4–8 months
-
Slight predilection for males in the USA and significant male predominance worldwide
-
HPV-positive tumors
-
Younger white male predilection.
-
Patients approximately 10 years younger than HPV-negative tumors.
-
Patients tend to be in higher socioeconomic group.
-
14.4.1.4 Appearance (Figs. 14.9a–e and 14.10)
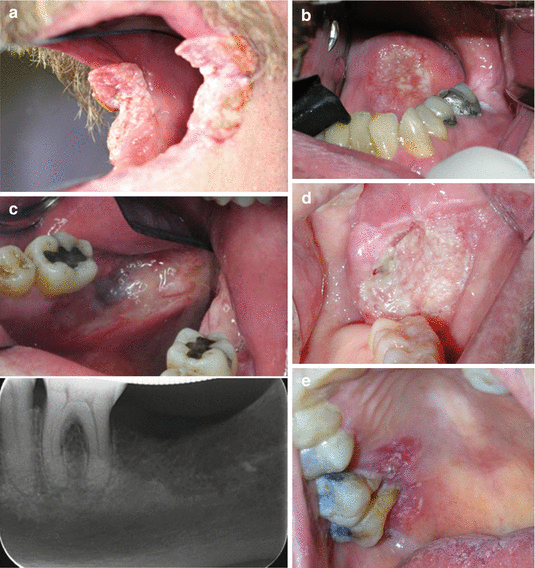
Fig. 14.9
(a) Large fungating exophytic carcinoma of the commissure of mouth encroaching upon the skin. (b) A Large endophytic ulcer with raised borders on the lateral/ventral tongue surface. Biopsy showed a moderately differentiated squamous cell carcinoma. (c) Carcinoma of the alveolar ridge with involvement of the underlying bone. Radiograph demonstrating erosion and irregular radiolucency of the bone. (d) Large fungating exophytic carcinoma of the buccal mucosa. (e) Carcinoma of the palatal gingiva and mucosa resulting in gingival recession. Carcinoma simulating periodontal disease. Destructive ulcerative carcinoma of the mandibular gingiva in 68-year-old female
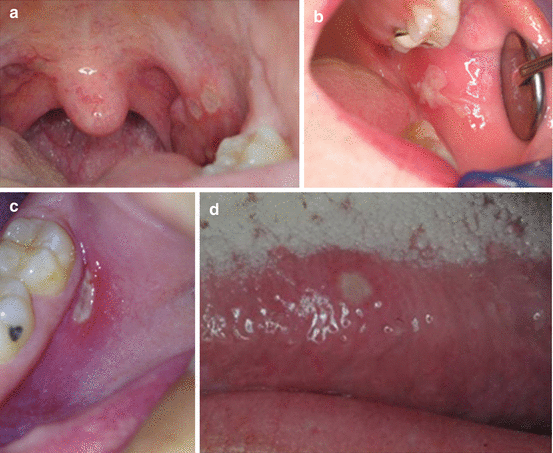
Fig. 14.10
(a) Major aphthous ulcerations on the tonsillar fauces in a 38-year-old female. (b) Major aphthous ulceration on the posterior buccal mucosa. (c) Minor aphthous ulceration on the posterior buccal vestibule in an 18-year-old female. (d) Minor aphthous ulceration on the lateral border of the tongue in a 26-year-old male
-
Often preceded or accompanied by leukoplakia, erythroplakia, erythroleukoplakia, or proliferative verrucous leukoplakia.
-
Most common sites: tongue; accounts for 40–50 % of all cases; majority of cases seen on the lateral or ventrolateral surfaces, rare on the dorsum.
-
The floor of the mouth is the second most common site (35 %); other less common sites include buccal mucosa, gingiva, and palate.
-
Presents as an indurated mass or ulcer.
-
Minimal pain during early growth years.
-
Varied clinical presentations: exophytic, endophytic, leukoplakic, erythroplakic, and erythroleukoplakic.
-
Destruction of underlying bone, if present, may be painless or painful.
14.4.1.5 Clinical Differential Diagnosis
-
Chronic traumatic ulcer
-
Epithelial dysplasia
-
Carcinoma in situ
-
Deep fungal infection
-
Chronic bacterial ulcers
14.4.1.6 Radiographic Features
-
Most oral tumors are favorable to visual examination; imaging is done for tumors that are palpable but not visible.
-
Soft tissue tumors: computerized tomographic (CT) scans, magnetic resonance imaging (MRI), and positron emission tomography (PET) most commonly used; however, stage I tumors (less than 2 cm in size) are not visible on these scans; recently, intraoral ultrasound has been an alternative to MRI in assessing tongue tumor thickness.
-
Tumors invading bone: panoramic and periapical images are of help in assessing mandibular or maxillary invasion. Radioactive isotope-labeled scans also useful in determining extent of tumor.
14.4.1.7 Treatment and Prognosis
-
Almost always requires a multidisciplinary approach (Haddad 2008).
-
Most early and late stage tumors are treated surgically with clear margins (1–2 cm) (Yesuratnam et al. 2014).
-
Neck dissection done when lymph nodes are involved.
-
Apart from surgery, stage III-IV tumors with adjuvant radiation and/or chemotherapy therapy.
-
HPV-positive tumors have a better prognosis than HPV-negative tumors; HPV tumor status should be assessed in appropriate settings.
-
HPV vaccination for prevention of oral carcinomas has not been approved by the US Food and Drug Administration.
-
5-year survival rate is approximately 63 %.
14.4.2 Aphthous Stomatitis
14.4.2.1 Synonyms
Aphthous stomatitis
14.4.2.2 Introduction
-
Most common ulcerative condition of the oral mucosa.
-
1 % of children in developed countries may be affected.
-
Etiology still obscure.
-
Multiple predisposing factors: positive family history, local trauma, nutritional deficiency (iron, folic acid and vitamin, food hypersensitivity (gluten)), immune disturbances, smoking cessation, psychological stress, and others.
14.4.2.3 Demographics
-
Lesions most commonly seen in young adults; 80 % of affected patients report their first ulceration before the age of 30 years.
-
Hereditary is a well-documented predisposing factor; positive family history is seen in 30–40 % of patients (Chavan et al. 2012).
-
Higher prevalence in higher socioeconomic class.
14.4.2.4 Appearance (Fig. 14.11a–d)
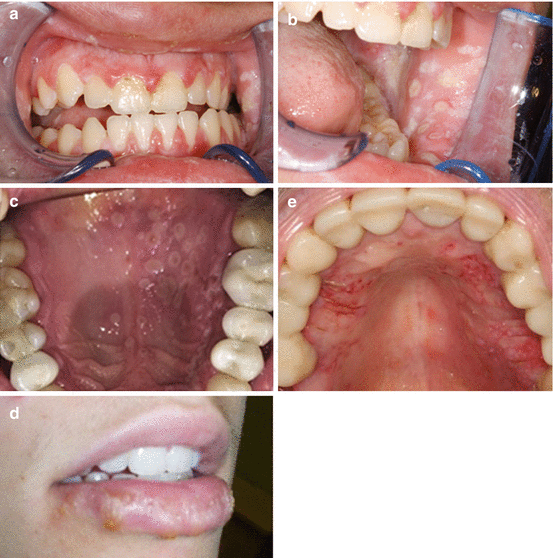
Fig. 14.11
(a) Gingival involvement is evident with enlargement and ulceration. (b) Same patient as Fig. 14.1 exhibiting buccal mucosal involvement. (c) Secondary multiple discrete ulcerations of the palatal mucosa in a 46-year-old. (d) Herpes labialis in a 26-year-old with multiple crusted ulcers and generalized swelling of the lower lip. (e) Secondary herpes on the palatal mucosa in a 76-year-old male. Lesions started within 3–4 days following significant periodontal surgery
-
Lesions characterized by recurrent bouts of single or multiple rounded, flat, painful oral ulcers.
-
Associated with prodromal symptoms of burning, itching, and stinging.
-
Ulcers typically appear with gray-white pseudomembranes surrounded by thin erythematous halos.
-
Occur in the nonkeratinized mobile oral mucosa; keratinized mucosa may be involved in immunocompromised patients.
-
Depending on the size, number, and appearance, they are classified into three clinical forms: minor, major, and herpetiform.
-
Minor aphthous ulcerations: up to 1 cm in diameter; show a variable recurrence rate and heal without scarring in 10–14 days.
-
Major aphthous ulcerations: 1–3 cm in diameter; demonstrate the longest duration per episode; heal in 2–6 weeks and may cause scarring.
-
Herpetiform aphthous ulcerations: 1–3 mm in diameter; numerous lesions; heal within 7–10 days; recurrences closely spaced.
14.4.2.5 Clinical Differential Diagnosis
-
Viral stomatitis
-
Traumatic ulcer
-
Pemphigus
14.4.2.6 Treatment and Prognosis
-
No specific diagnostic test exists.
-
In order to discard the underlying systemic causes, a complete series of laboratory tests should be evaluated (complete blood count, iron, vitamin B12, and folic acid) (Belenguer-Guallar et al. 2014).
-
Biopsy of the lesion is only recommended in the case of diagnostic uncertainty, since the findings only indicate a simple nonspecific inflammatory lesion (Belenguer-Guallar et al. 2014).
-
Refer patient to internist (to rule out malabsorption syndrome, food allergies, gluten sensitivity.
-
Majority of patients spontaneously enter remission.
-
Most common therapy: topical corticosteroids; decreases pain and duration but has no effect on future occurrence of new lesions.
14.4.3 Oral Herpetic Stomatitis
14.4.3.1 Synonyms
-
Cold sore
14.4.3.2 Introduction
-
HSV is a double-stranded DNA virus and is a member of the human herpes virus (HHV) family.
-
Though the virus exists in 2 forms, HSV-1 (or HHV-1) and HSV-2 (or HHV-2), HSV-1 accounts for most oral, facial, and ocular lesions (Usatine and Tinitigan 2010).
-
Transmission occurs primarily through infected saliva or active perioral lesions.
-
The virus must come into contact with a break in the integrity of the mucosa or skin of a susceptible host.
-
Infection includes primary infection, latency, and recurrent infection.
-
Primary infection: initial exposure of an individual without antibodies to the virus.
-
Latent infection: virus is taken up by the sensory nerves and transported to the associated sensory ganglion.
-
Recurrent infection: reactivation of virus.
14.4.3.3 Demographics
-
Crowding and poor hygiene promote exposure to HSV.
-
In developing countries 100 % of the population exposed by 30 years of age.
-
In developed countries 50–60 % of population exposed by 30 years of age.
-
Primary herpes at early age usually results in gingivostomatitis, whereas exposure in adults usually causes pharyngotonsillitis.
-
Acute gingivostomatitis is common in children between 6 months and 5 years of age.
14.4.3.4 Appearance (Fig. 14.12a–e)
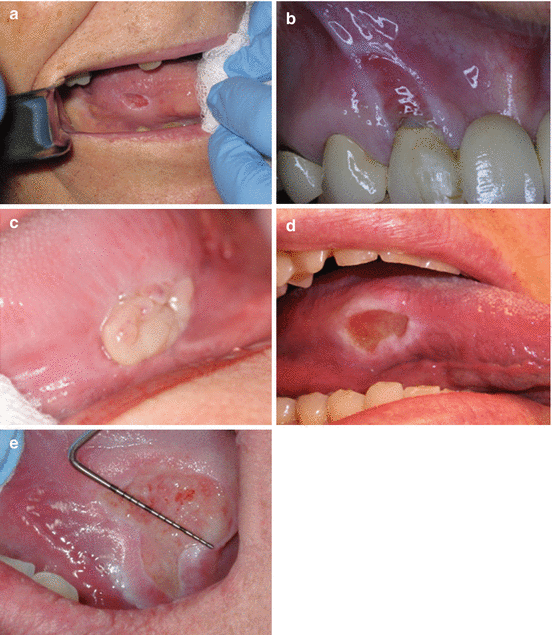
Fig. 14.12
(a) Ulceration of tongue associated with chronic trauma from maxillary molar in a partially edentulous elderly patient. (b) Linear ulcer on the maxillary gingiva associated with tooth brushing trauma. (c) TUGSE on the lateral tongue in a 72-year-old female. The lesion is present for about 3 months. (d) Long-standing ulceration of the lateral tongue. Note thick white borders. (e) Large painful long-standing ulcer of tongue simulating carcinoma. Patient reports chronic trauma. Note thick white borders
-
Age of initial infection affects clinical presentation of primary HSV-1 infection.
-
Primary herpes: early age exposure: gingivostomatitis; late age exposure: pharyngotonsillitis.
-
Acute gingivostomatitis: has an abrupt onset of symptoms and is accompanied by constitutional symptoms such as cervical lymphadenopathy, fever, chills, anorexia, irritability, and sore mouth. Numerous small vesicles that eventually rupture to form ulcers are noted on both attached and movable mucosa affected. The gingiva may be enlarged, erythematous, and extremely painful.
-
Pharyngotonsillitis presents with sore throat, headache, fever, and malaise, and oral lesions are similar to those noted above usually on the tonsils and posterior pharynx.
-
Recurrent infection (secondary herpes) occurs in a healthy host at or near the site of primary infection almost always involving bound down or keratinized mucosa such as lip vermillion and adjacent skin (herpes labialis) and hard palate and attached gingiva.
-
Prodromal signs (tingling, burning, or pain) appear before onset of lesions.
-
In an immunocompromised host, recurrent ulcers appear anywhere on the oral mucosa and may resemble aphthous ulcers when on nonkeratinized mucosa.
14.4.3.5 Clinical Differential Diagnosis
-
Aphthous ulcers
-
Traumatic ulcers
14.4.3.6 Treatment and Prognosis
-
Healing occurs within 7–10 days.
-
Primary infection: Symptomatic support (hydration, pain control, supportive care); antiviral medications are beneficial if administered early (acyclovir suspension, acyclovir or valacyclovir tablets initiated during the first 3 days of symptoms) (Woo and Challacombe 2007; Rahimi et al. 2012; Arduino and Porter 2006).
-
Recurrent infection: best result if antiviral medication administered during the first 3 days of symptoms (acyclovir; penciclovir cream or ointment for herpes labialis) (Woo and Challacombe 2007).
-
Research toward development of a potential herpes simplex vaccination is ongoing (Rahimi et al. 2012).
14.4.4 Traumatic Ulcers
14.4.4.1 Synonyms
-
None
14.4.4.2 Introduction
-
May result from acute or chronic mechanical injury
-
Majority are unintentional; in most cases cause and effect relationship easily established
-
Biopsy is not required in most cases; some may warrant histological investigations to exclude conditions which clinically mimic traumatic lesions
14.4.4.3 Demographics
-
Mechanical trauma related: may occur at any age; no gender predilection
-
Usually occurs on tissues that are prone to accidental biting such as tongue, buccal mucosa and lips
14.4.4.4 Appearance (Fig. 14.13a–e)
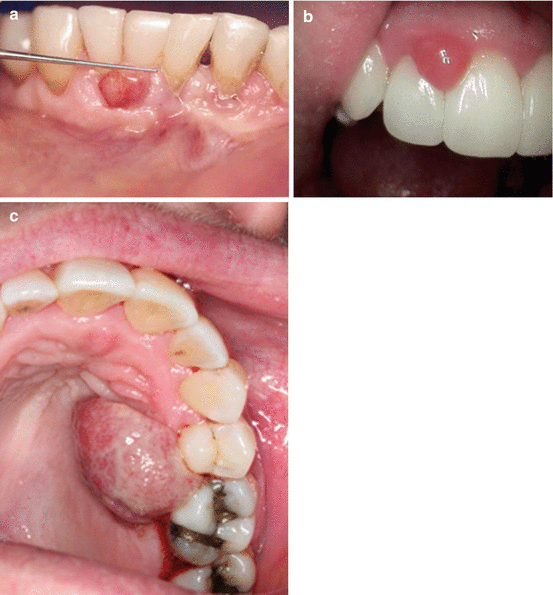
Fig. 14.13
(a) Ulcerated sessile gingival mass. (b) Anterior maxillary gingival mass. (c) Large growth on gingiva that exhibited rapid growth
-
Vary significantly; depending on cause.
-
Acute mechanical trauma: caused by accidental mucosal biting: ulcerated lesion on an erythematous background, covered by a removable, yellowish fibrinopurulent exudate; heal uneventfully with few days.
-
Chronic mechanical trauma: from sharp edges of teeth, restorations and ill-fitting dentures; present as a solitary shallow or deep ulcer with varying degrees of peripheral keratosis; borders of ulcer is indurated in most cases, and the floor is covered by a white or yellowish fibrin clot; may be asymptomatic or painful; common sites include the lips, tongue, and buccal mucosa.
-
Traumatic ulcerative granuloma with stromal eosinophilia (TUGSE) is usually a large ulcer associated with tumefaction; most common site is the tongue; gingiva, the buccal mucosa, alveolar mucosa, and lips may also be affected (Hirshberg et al. 2006).
14.4.4.5 Clinical Differential Diagnosis
-
Squamous cell carcinoma
-
Aphthous ulcers
-
Neutropenic ulcers
-
Medication-induced ulcers
-
Infectious diseases ulcers
-
Autoimmune diseases ulcers
14.4.4.6 Treatment and Prognosis
-
Removal of causative factor is critically important. In addition application of topical anesthetic or protective film provides temporary relief; acute ulcers heal within 1–2 weeks without scarring; recurrence not expected.
-
Biopsy of lesions that do not resolve after 2–4 weeks following mitigation of trauma.
-
TUGSE: many lesions undergo resolution after incisional biopsy (Hirshberg et al. 2006).
14.5 Raised Soft Tissue Lesions (Bumps)
14.5.1 Pyogenic Granuloma
14.5.1.1 Synonyms



