Immediate Implant Placement and Provisionalization of Maxillary Anterior Single Implants
Joseph Y.K. Kan, Kitichai Rungcharassaeng, and Jaime L. Lozada
Loma Linda University School of Dentistry, Loma Linda, California, USA
Introduction
Achieving optimal gingival esthetics around anterior single implants is a challenging procedure,1,2 and maintaining it over time can be an equally demanding task. Despite the high success rates achieved with osseointegrated implants,3 the peri‐implant mucosal response is not clearly understood. For anterior single implants, up to 16% of gingival recession has been reported.3 On the other hand, spontaneous rebound of the receded gingiva has also been observed following a few years of function.4–6 The peri‐implant mucosa changes had been postulated to be an attempt to establish a stable biological dimension.7 An understanding of the dentogingival complex and its implant counterpart (peri‐implant mucosa) allows clinicians to predictably balance the biologic/physiologic requirement and esthetic demand of single implant restorations in the esthetic zone.
The impending loss of a single tooth in the esthetic zone in a patient with an otherwise healthy periodontium can be a distressing experience.1,8–10 An inevitable loss of soft and hard tissue after tooth extraction can be expected in a compromised site for anterior implant esthetics. Various augmentation techniques have been advocated as corrective procedures, but they are time consuming and not always predictable.4,11–13 Therefore, the fundamental concept of site development for an anterior single implant is to preserve the existing gingival and osseous tissue of the failing tooth, if possible.1 Since 1998, when Wohlre14 first demonstrated success with immediate implant placement and provisionalization (IIPP) of single anterior maxillary implants, numerous studies have substantiated the viability of such treatment.9,15–26 One of the most desirable features of IIPP is its efficacy in optimizing esthetic success by preserving the existing osseous and gingival architecture.8,9,14,27
The esthetic success of IIPP procedures is influenced by a number of factors that can be identified as intrinsic or extrinsic.28 Intrinsic factors are patient dependent, and include the relationship between hard and soft tissues, gingival biotype, and sagittal root position in the alveolar bone.29,30 Extrinsic factors, on the other hand, are clinician dependent and include three‐dimensional (3‐D) implant position and angulation, as well as contour of the abutment and provisional restoration.8,29
Diagnosis and treatment planning
Proper diagnosis of the patient’s condition allows clinicians to devise a suitable treatment plan that can be predictably executed. By recognizing unfavorable conditions, adjunctive procedures can be incorporated to avert compromised situations. The following parameters must be evaluated for an IIPP procedure.
- Gingival level of the failing tooth should be: 1) the same as (or more coronal than) that of the contralateral tooth and 2) harmonious with adjacent dentition, as some gingival recession can be expected after the procedure (Figure 6.1).1 Furthermore, it is more challenging to coronally reposition an existing recession for IIPP procedures. Therefore, when the gingival level of the failing tooth is more apical than that of the contralateral tooth, orthodontic forced eruption, if possible, should be implemented prior to IIPP.31
- Osseous–gingival tissue relationship can be evaluated by bone sounding and should measure 3 mm on the facial aspect of the failing tooth and 4.5 mm on the proximal aspect of adjacent teeth (Figure 6.2). There is a propensity for tissue recession after extraction with or without immediate implant placement in low crest situations, in which bone sounding measurements are greater (more than 3 mm mid‐facial pocketing) than those indicative of an optimal relationship.29 Depending on the gingival level, orthodontic and/or periodontal treatment can be used to improve the osseous–gingival tissue relationship.
- Gingival biotype can be assessed during bone sounding and categorized according to the visibility of the underlying periodontal probe (SE Probe SD12 Yellow, American Eagle Instruments Inc., Missoula, MT) through the gingival tissue (visible = thin, and not visible = thick) (Figure 6.2).32,33 Higher visibility corresponds to lower levels of thickness. Thin gingival biotype, which has been shown to sustain more tissue recession after surgical insults than thick biotype, can be enhanced by using a bilaminar subepithelial connective tissue graft (SCTG) at the time of IIPP.28
- Sagittal root position (SRP)30 of the failing tooth in the alveolar bone can be identified via cone‐beam computed tomography (CBCT) and can be categorized as one of four different classes (Figure 6.3):
- class I: the root is positioned against the labial cortical plate;
- class II: the root is centered in the middle of the alveolar housing without engaging either labial or palatal cortical plates at the apical one‐third of the root;
- class III: the root is positioned against the palatal cortical plate;
- class IV: at least two‐thirds of the root is engaging both labial and palatal cortical plates.
- It is important for clinicians to recognize cases that are favorable for IIPP (class I SRP), cases that are more technique sensitive and entail additional attention (class II and class III SRP), and cases that are contraindicated for IIPP, requiring hard and/or soft tissue augmentation prior to implant placement (class IV SRP).30 Buccolingual width and interradicular mesiodistal widths of the failing tooth determine the diameter of the implant to be used and can be evaluated using CBCT and periapical radiographs (Figure 6.4).
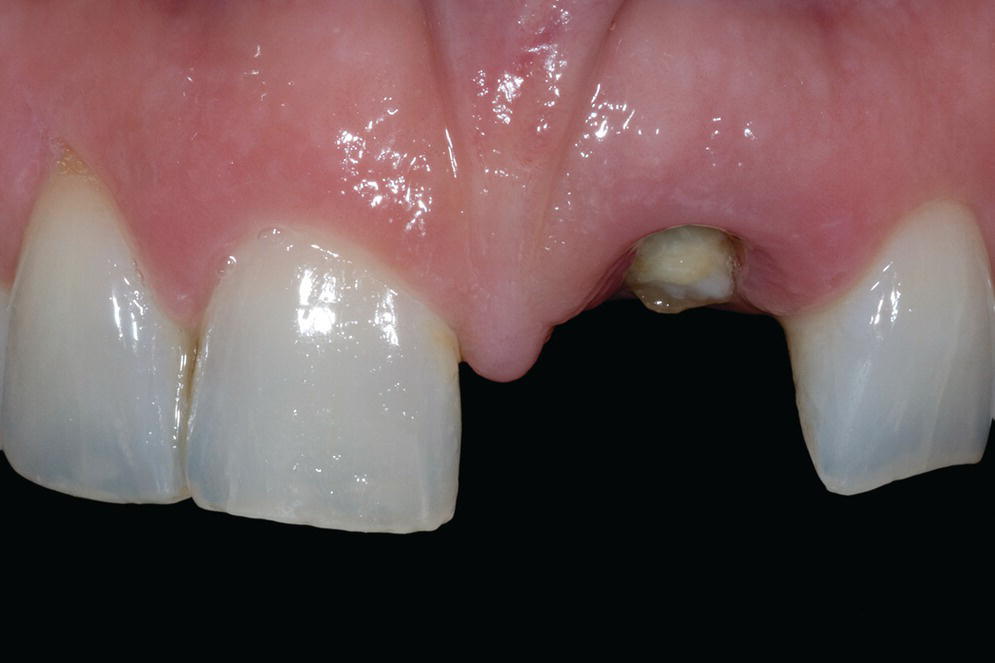
Figure 6.1 Gingival level of the failing tooth (#9) should be (1) the same as (or more coronal than) that of the contralateral tooth and (2) harmonious with the adjacent dentition, as some gingival recession can be expected after the procedure.
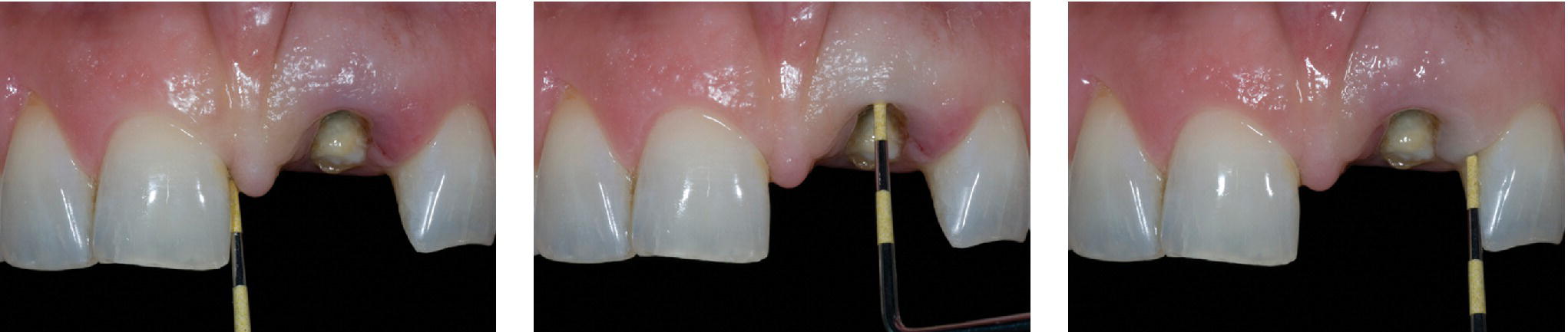
Figure 6.2 Osseous–gingival tissue relationship can be evaluated by bone sounding and should measure 3 mm on the facial aspect of the failing tooth and 4.5 mm on the proximal aspect of adjacent teeth.
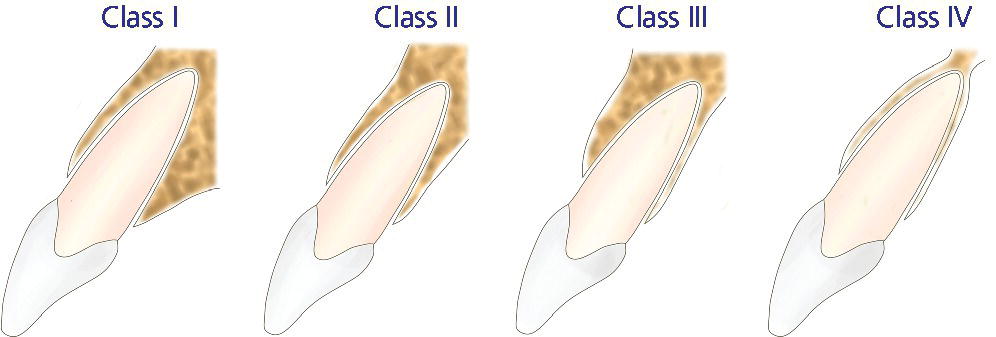
Figure 6.3 Sagittal root position classification. Class I: the root is positioned against the labial cortical plate. Class II: the root is centered in the middle of the alveolar housing without engaging either labial or palatal cortical plates at the apical one‐third of the root. Class III: the root is positioned against the palatal cortical plate. Class IV: at least two‐thirds of the root is engaging both labial and palatal cortical plates.
Source: Courtesy of Jeff Miles.
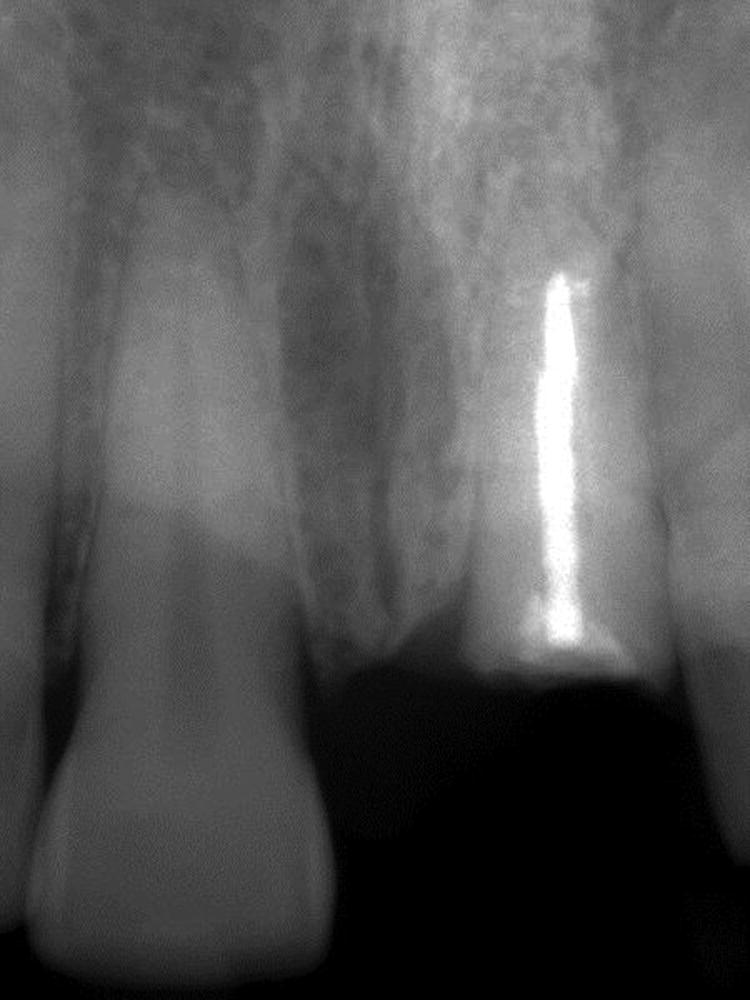
Figure 6.4 Periapical radiograph of the failing tooth.
Clinical procedure
Diagnostic waxing
A diagnostic waxing of the failing tooth on the study cast should: 1) represent, as closely as possible, the definitive restoration; 2) match the contralateral tooth; and 3) be harmonious with the adjacent dentition. Proper diagnostic waxing provides information necessary for treatment planning, especially when adjunctive procedures (orthodontic and/or periodontal intervention) are required. A provisional restoration, as well as implant and soft tissue surgical templates, can be accurately fabricated from a well‐executed diagnostic waxing. It may be possible, before the provisional crown is fabricated, for the patient to preview the intended morphology of the definitive restoration with a smile design using a composite resin replica inside a vacuum‐formed template generated from a cast of the wax‐up. On the other hand, where the crown portion of the failing tooth is intact and esthetically acceptable, it can be modified after extraction to be used as a natural‐looking provisional restoration.
Surgical procedure
Immediate implant placement entails extraction of the failing tooth followed by placement of an osseointegrated implant. The extraction must be minimally traumatic with controlled expansion of the bony socket to avoid soft and/or hard tissue damage. This can be accomplished by first using a periotome (Nobel Biocare, subsidiary of Danaher, Washington DC) to make a sulcular incision with transeptal fiberectomy that extends apically beyond the marginal bone. This incision separates the tooth from the periodontal tissue, facilitating extraction with zero or minimal damage to the usually thin labial bony plate. After the extraction, the integrity of the labial plate must be verified using a periodontal probe. Fenestrations located at least 5 mm apical to the intact facial marginal bone are generally inconsequential to the IIPP procedure, as these defects can be addressed predictably with grafting.
When a facial osseous dehiscence/defect is detected, the predictability of the IIPP in conjunction with guided bone regeneration (GBR) procedures is determined by the shape/size of the defect.34 A V‐shaped defect, which is isolated only to the mid‐facial portion of the facial bony plate, responds favorably to IIPP with GBR (Figure 6.5). It should be noted, however, that significant facial gingival recession after 1 year of function has been reported when IIPP with GBR was attempted on failing teeth with U‐shaped (extends to mesial and/or distal aspect of the failing tooth) or UU‐shaped (extends to the mesial and distal aspect of the immediately adjacent teeth) defects (Figure 6.5).34 Therefore, a failing tooth with a U‐shaped or UU‐shaped defect is contraindicated for IIPP.
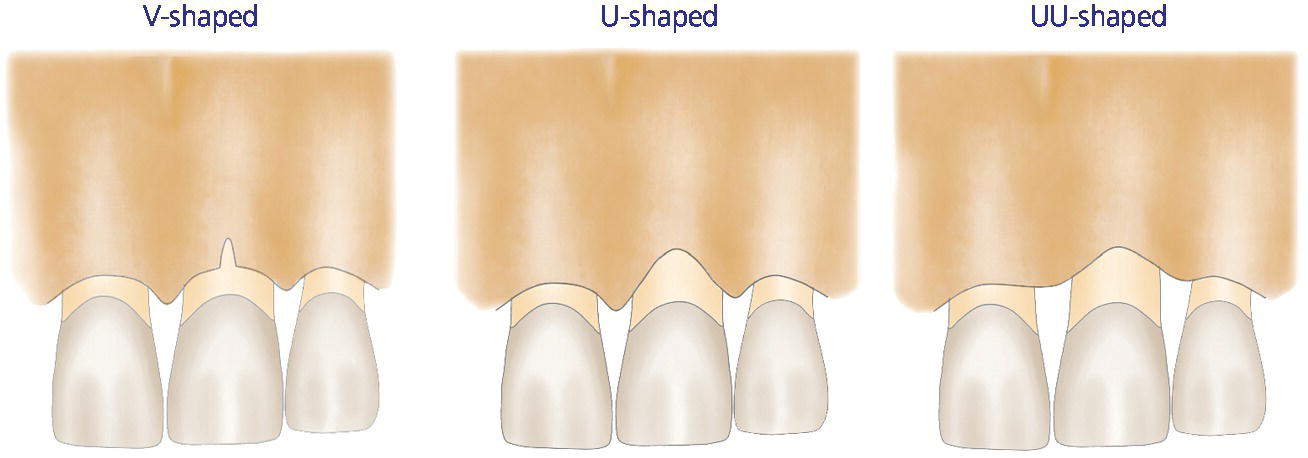
Figure 6.5 Facial bone defect classification. V‐shaped defect: isolated only to the mid‐facial portion of the facial bony plate. U‐shaped defect: extends to the mesial and/or distal aspect of the failing tooth. UU‐shaped defect: extends to the mesial and distal aspects of the immediately adjacent teeth.
Source: Courtesy of Jeff Miles.
Primary implant stability is the prerequisite for IIPP and is usually achieved by engaging the palatal wall and the bone 4–5 mm beyond the apex of the extraction socket. Therefore, class I SRP, with a considerable amount of bone present on the palatal aspect for implant engagement to attain primary stability, is optimal for IIPP. Class IV SRP, with a limited amount of bone for implant engagement, is a contraindication.30 Class II and III SRP present compromised and/or challenging conditions for IIPP.30 In class III SRP, implant stability must rely on its engagement with the available bone on the labial aspect, which can potentially lead to facial fenestration or perforation.30 In class II SRP, as available bone on both the palatal and labial aspects is inadequate, the implant stability relies primarily on the amount of available bone beyond the apex of the extraction socket.30
The final implant diameter should be within the confines of the tooth socket, but should not engage the usually thin coronal portion of the labial plate. This will help to prevent perforation. Furthermore, a minimal distance of 2 mm between the implant and adjacent teeth is recommended to minimize marginal bone loss due to encroachment.35 The final implant position and angulation are in accordance with the following guidelines (Figure 6.6).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


