and Angela J. Yoon1
(1)
Columbia University College of Dental Medicine and Department of Pathology and Cell Biology, Columbia University Medical Center, New York, NY, USA
It is not uncommon to encounter various white or red macules or patches in pediatric patients. These lesions are often transient and of various origins such as thermal insult, trauma, or frictional irritation. It is important to distinguish these lesions from true leukoplakias and erythroplakias which are by definition premalignant lesions. Fortunately true leuko- and erythroplakias are rare in children and adolescents.
|
White and red macules and patches
|
|---|
|
Morsicatio buccarum, linguarum, and labiorum
|
|
Superficial chemical burn
|
|
Oral candidiasis
|
|
Benign migratory glossitis
|
|
Leukoplakia
|
|
Erythroplakia
|
4.1 Morsicatio Buccarum, Linguarum, and Labiorum
Morsicatio buccarum, linguarum and labiorum are also known respectively as chronic cheek, tongue, and lip biting/chewing.
Clinical Appearance
The lesions are white with thickened, ragged appearance to the mucosa. The involved area is often diffuse and loose superficial fragments can sometimes be peeled off.
Etiology
Chronic conscious or subconscious habit of chewing on the cheek, tongue, or lower lip.
Location
Buccal mucosa, lateral tongue, or lower lip mucosa.
Differential Diagnosis
Candidiasis, leukoplakia.
Treatment
The diagnosis is usually made on the clinical appearance. The lesions are harmless and no treatment is required.
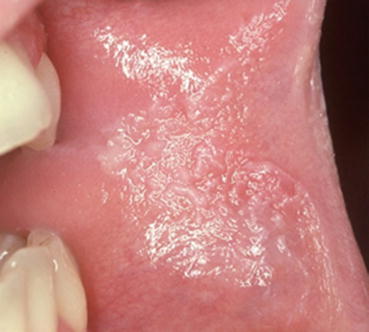
Fig. 4.1
Morsicatio buccarum. White ragged appearance to the anterior buccal mucosa in a teenager who chews on the area when she is studying
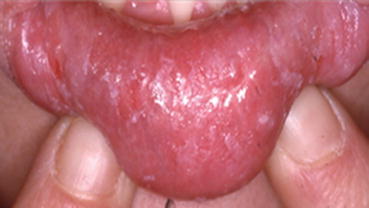
Fig. 4.2
Morsicatio linguarum. Ragged, macerated appearance of the lower lip. The patient has a lip chewing habit and a habit of peeling off the loose “skin”
4.2 Superficial Chemical Burn
Clinical Appearance
Superficial sloughing or peeling of the mucosa. Patients often complain of wiping “stringy” material from mouth in the morning.
Etiology
Superficial chemical burn often from dentifrice.
Location
Mandibular vestibule is the most common location.
Differential Diagnosis
Mucosal pemphigoid, candidiasis, leukoplakia.
Treatment
No treatment is required. The patient can switch to a mild toothpaste and avoid alcohol or peroxide containing mouthwash.
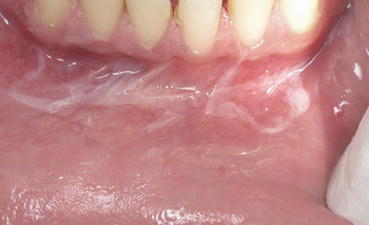
Fig. 4.3
Superficial chemical burn. Transparent white superficial sloughing of the mucosa. The sloughed mucosa is similar to a piece of thin wet tissue paper. Note the lack of any underlying erythema or erosion
Clinical Clue
The superficial slough is transparent white and can be easily wiped away with a cotton tipped applicator; the mucosa underlying the sloughed off tissue is normal appearing and asymtomatic.
4.3 Oral Candidiasis
Clinical Appearance
Commonly referred to as thrush, oral candidiasis can occur in three different clinical variants: pseudomembranous, erythematous, or hyperplastic. The pseudomembranous form is the most common and presents as white removable plaques. Erythematous candidiasis presents with generalized erythema of the oral mucosa and the child might complain of a sore mouth. Hyperplastic candidiasis presents as white adherent plaques and patches. Hyperplastic candidiasis is not commonly seen in children.
Etiology
Opportunistic fungal infection caused by Candida albicans.
Location
Anywhere in the oral cavity. The tongue, palate, and vestibules are common locations.
Differential Diagnosis
Pseudomembranous candidiasis is not often confused with other entities since it is white to cream color and wipeable. Erythematous candidiasis could be mistaken for geographic tongue, contact stomatitis, or allergy. Hyperplastic candidiasis might be mistaken for a leukoplakia or geographic tongue. If a clinical diagnosis of oral candidiasis cannot be rendered, a fungal culture or smear can be performed.



