Key points
- •
The key to good surgery is good access, and the key to good access is good surgery. This is never more true than when dealing with vascular lesions–which demand unrestricted exposure.
- •
Hypervascular tumors or those known to have a high degree of blood loss during surgery may benefit from preoperative embolization.
- •
If embolization is necessary, the embolic agent can be determined by using the following 3-question algorithm:
- ○
Is the vessel to be embolized large or small?
- ○
How long (temporally) is the vessel to remain occluded?
- ○
Is the tissue supplied by the vessel to remain viable after the embolization?
- ○
- •
Surgery is usually performed the day after embolization, although some investigators suggest resection can be delayed up to 8 days.
Introduction
A multidisciplinary team is imperative to the diagnosis and successful management of vascular anomalies of the head and neck. Patients routinely require the services of a radiologist (both imager and proceduralist) and an experienced surgeon. Hematologist-oncologists and dermatologists can also be of assistance. A patient’s history cannot be overemphasized, as it aids the radiologist in deciding on imaging modalities, tailoring studies to the needs of the patient, and making the diagnosis.
This article discusses the classification of vascular anomalies, provides a clinicopathologic review of a few vascular lesions, reviews imaging principles of vascular anomalies and image-guided (interventional) procedures, and concludes with treatment pearls.
Introduction
A multidisciplinary team is imperative to the diagnosis and successful management of vascular anomalies of the head and neck. Patients routinely require the services of a radiologist (both imager and proceduralist) and an experienced surgeon. Hematologist-oncologists and dermatologists can also be of assistance. A patient’s history cannot be overemphasized, as it aids the radiologist in deciding on imaging modalities, tailoring studies to the needs of the patient, and making the diagnosis.
This article discusses the classification of vascular anomalies, provides a clinicopathologic review of a few vascular lesions, reviews imaging principles of vascular anomalies and image-guided (interventional) procedures, and concludes with treatment pearls.
Classification of vascular anomalies
The whole team should share a common lexicon. The International Society for the Study of Vascular Anomalies (ISSVA) provides such a framework for classifying “Vascular Tumors.” These tumors, along with common examples, are listed in Table 1 .
| Vascular Tumors | Vascular Malformations | |||
|---|---|---|---|---|
| Benign | Locally Aggressive or Borderline | Malignant | Simple | Combined |
|
Kaposiform hemangioendothelioma Retiform hemangioendothelioma Papillary intralymphatic angioendothelioma (PILA), Dabska tumor Composite hemangioendothelioma Kaposi sarcoma |
Angiosarcoma Epithelioid hemangioendothelioma |
CM LM VM AVM AVF |
CVM CLM CAMV LVM CLVM CLAVM CVAVM CLVAVM |
In addition to these vascular lesions, this article also considers “vascular-like tumors”: hypervascular neoplasia such as hemangiopericytomas, paragangliomas (carotid body tumors and glomus tumors), and hypervascular metastasis.
Clinicohistopathologic description
Hemangiomas
Hemangiomas are common, comprising 7% of benign pediatric age tumors and affecting 4.5% of children. One-third of hemangiomas are found in the head and neck, and 14% within the oral cavity. Hemangiomas of childhood are divided into infantile and congenital types, based on whether they are fully developed at birth. Hemangiomas that develop in adulthood tend to be small and are often located within the oral cavity or pharynx. Mucosal hemangiomas develop in areas that are often traumatized, such as the lip, buccal mucosa, and tongue ( Figs. 1–5 ).
Infantile hemangiomas
Infantile hemangiomas are the most common vascular neoplasms, and include capillary and cavernous hemangiomas of any organs. These hemangiomas develop more often in infants who are female, Caucasian, premature, or of low birth weight. Most infantile hemangiomas present between 2 weeks and 2 months after delivery, and grow with the child; they present as an erythematous macule, patch, or plaque, but may also be present within deep soft tissues. Most do not require medical or surgical intervention. For those requiring medical intervention, propranolol and glucocorticoids are often the first-line therapy.
Capillary hemangiomas are the most common soft-tissue neoplasm in infants and children, and consist of numerous intertwining capillary-sized blood vessels. These tumors grow rapidly in first year of life, then undergo gradual involution over the next 1 to 7 years. By age 7, 75% to 90% regress.
Cavernous hemangiomas are composed of larger vascular spaces filled with erythrocytes, are generally larger than capillary hemangiomas, and may involve deeper tissue. Although they are usually well circumscribed, they may be locally destructive. Unlike capillary-type infantile hemangiomas, they do not spontaneously regress.
Congenital hemangiomas
Congenital hemangiomas are much rarer than infantile hemangiomas. Unlike infantile hemangiomas they are fully formed at birth, occur equally in males and females, and stain negative for GLUT1 by immunohistochemistry. Congenital hemangiomas occur as solitary lesions on the head or near limb joints, and are categorized by the tendency to spontaneously involute. Rapidly involuting congenital hemangiomas regress completely within 2 years of birth; noninvoluting congenital hemangiomas grow proportionately with the infant and may display partial involution, but not full regression.
Vascular malformations
Vascular malformations are vascular proliferations arising from disordered angiogenesis, either during development or following trauma, and are categorized as either high-flow lesions, which involve an artery, or low-flow lesions, which do not. Vascular malformations may also be categorized by the number of vessel types involved (see Table 1 ). Simple malformations are composed of only a single type of vessel, and combined malformations include any combination of capillary, lymphatic channel, artery, and vein.
High-flow lesions include arteriovenous fistulas (AVFs) and arteriovenous malformations (AVMs). AVFs develop following trauma, and consist of 1 or more shunts between arteries and other vascular structures. AVMs of the head and neck are serious lesions of unclear pathogenesis that are difficult to diagnose, treat, and cure; they may represent a spectrum of diseases rather than a single disease process. Most are present at time of birth, although they may present clinically several years later. Destructive lesions that grow throughout life and may have sudden, dramatic increases in size, AVMs may present clinically as a blush, similar to an early port-wine stain, which may have a pulse and thickening of the tissue, but no fluctuance.
In contrast to AVMs and AVFs, venous malformations ( Figs. 6–10 ) are low-flow vascular malformations consisting of dilated veins. Venous malformations are rare, affecting 1 in 10,000 people, and often occur in the head and neck, involving the mucosa, skin, or muscle. Although most cases arise sporadically, they may arise secondary to an autosomal dominant disorder linked to chromosome 9P, or as part of a syndrome. Clinically they may present with pain or swelling and, unlike lymphangiomas, are compressible.
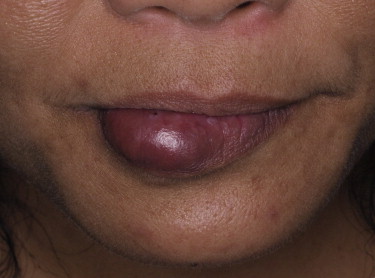
Lymphatic malformations
Lymphatic malformations are congenital dilatations of the lymphatic channels that may be categorized as microcystic, macrocystic, or combined. Macrocystic lesions have a better prognosis, and are easier to treat, than microcystic lesions. The lesions may be focal, multifocal, or diffuse; they typically grow slowly, but may enlarge rapidly during puberty or at times of infection. Three-fourths of lymphatic malformations occur in the head and neck ( Fig. 11 ).
Macrocystic lymphatic malformations (formerly known as cavernous lymphangiomas or cystic hygromas) may arise anywhere, but most often present as a painless, translucent soft mass underlying normal skin, within the posterior and anterior triangles of the lateral neck. Two-thirds of cases are recognized at the time of birth. These lesions may be associated with chromosomal abnormalities, such as Turner syndrome and Down syndrome, or with other anomalies such as thyroglossal duct cyst. Complications include infection, hemorrhage, or compression of adjacent structures, causing difficulties with swallowing or speech. Because they may undergo spontaneous involution in infancy, surgery for infantile cases without complication should be postponed until age 3 to 5 years.
Hemangioendothelioma
Hemangioendotheliomas (HEs) are a group of rare proliferative vascular neoplasms, with behavior and histologic appearance intermediate between benign hemangiomas and malignant angiosarcoma. Of the several subtypes that exist, the most aggressive variety is epithelioid HE. Epithelioid HEs most often arise as a poorly circumscribed mass near medium-sized vessels in young adults, expanding outwardly from the vessels, and obliterating the lumen. Old lesions may ossify and thus can be seen radiographically. Because they are rare tumors, without distinctive clinical or radiographic features, the diagnosis is usually unsuspected until histologic examination. Although they are generally indolent, almost one-third of epithelioid HEs metastasize to regional lymph nodes, lung, or bone, and 15% of patients die of the disease.
Kaposi sarcoma
Kaposi sarcoma (KS) is a rare malignancy of endothelial cells. Four types have been described: classic KS (found in Mediterranean men, involving the skin of the head and neck in 85% of cases, and rarely involving mucosa); human immunodeficiency virus–related KS (a widely invasive sarcoma involving skin in most cases, and involving the upper airway mucosa in nearly one-fifth of cases); endemic KS (seen in sub-Saharan Africa); and iatrogenic KS (found in immunosuppressed organ transplant patients).
Skin lesions range from a solitary pale, erythematous macule, papule, or plaque, to widely disseminated purple-brown nodules. In the oral cavity, early-stage KS presents as erythematous, bluish, or dark brown macules, whereas later-stage disease appears as nodular or ulcerating lesions. Because of high recurrence rates, complete cure may be an unrealistic expectation for many patients. Solitary lesions may be treated by surgical excision, whereas extensive, multifocal lesions demand treatment with radiation and chemotherapy.
Angiosarcoma
Angiosarcoma is a diffusely infiltrative malignant vascular neoplasm with a dismal prognosis. It is the third most common head and neck sarcoma (following malignant fibrous histiocytoma and KS), accounting for 10% of head and neck sarcomas. Although they are extremely rare, comprising less than 1% of all sarcomas, more than half of all angiosarcomas are in the head and neck. Nearly three-quarters of head and neck angiosarcomas involve the skin, subcutaneous tissue, or deep tissue, with the remaining quarter involving the upper aerodigestive tract. Risk factors include history of radiation exposure, trauma, and chronic lymphedema. Most cases arise in patients with no risk factors. Angiosarcomas of the skin or mucosa present clinically as solitary or multifocal, red to blue hemorrhagic nodules. The clinical appearance may be indistinguishable from that of a pyogenic granuloma.
Hemangiopericytoma
Hemangiopericytoma (HPC) is an entity with considerable controversy regarding whether it exists as a distinct entity. The recent trend has been to reclassify tumors previously diagnosed as HPCs as solitary fibrous tumors. HPCs are rare, highly vascular soft-tissue tumors, with spindled to oval cells arranged around prominent, thin-walled blood vessels; they are found in all age groups but occur most often in middle-aged and older adults ( Figs. 12–25 ). Although they may occur at any site, the head and neck is uncommon. Most head and neck HPCs develop in the upper aerodigestive tract, and 28% develop in the neck. Clinically, within the oral cavity HPCs typically present as a soft, rubbery, painless, rapidly enlarging, and well-demarcated red or bluish mass. Most HPCs are clinically benign. A meta-analysis of 116 cases of head and neck HPCs found that following surgery 28% recurred, and 6% recurred more than once. Overall rate of metastasis was 15%, with an average delay of 45 months from treatment of the primary lesion. Seventy-five percent of HPCs in the head and neck had a good prognosis following surgery, and overall 10-year survival rate was 90%. Adverse prognostic indicators include size greater than 5.0 cm, nonsurgical treatment, deep location, and poor histologic differentiation.




