Introduction
Children with severe hypodontia have a substantial impairment of their dental health starting early in life. The purpose of this study was to describe types and locations of substitutes for missing teeth in patients with severe hypodontia and to compare the crown and soft tissue morphologies of orthodontic space closure, dental implants, and tooth-supported fixed dental prostheses for replacing teeth in the anterior region.
Methods
Fifty patients missing 6 or more teeth and aged 18 years or older (mean age, 25.6 years) took part in a follow-up study. The patients were examined clinically with panoramic radiographs and clinical photographs. Crown and soft tissue variables (mucosal discoloration, crown morphology, color, and papilla index) were compared for orthodontic space closure, dental implant fixtures, and fixed dental prostheses.
Results
Dental implants, orthodontic space closure, and retaining deciduous teeth were the most commonly prescribed treatments. Persisting deciduous teeth showed a good survival rate at the follow-up examination. Mucosal discoloration was seen only for implant fixtures and was evident for almost all fixtures in the anterior mandible and two thirds of those in the anterior maxilla. The papilla index scored poorer for both implant fixtures and fixed dental prostheses compared with orthodontic space closure.
Conclusions
Dental implants in the anterior region proved to be an inadequate treatment modality in patients with severe hypodontia because of pronounced mucosal discoloration.
Highlights
- •
Fifty children missing 6 or more teeth were surveyed after age 18.
- •
Implants, space closure, and retaining deciduous teeth were the treatments of choice.
- •
Implants in the anterior region were inadequate in patients with severe hypodontia.
- •
Mucosal discoloration or visible metal were most pronounced in the anterior mandible.
- •
Persisting deciduous teeth showed a good survival rate.
Children congenitally missing a substantial number of teeth have a severe impairment of their dental health starting early in life and face a challenging and tedious, even lifelong, treatment regimen. The clinician’s mission is to provide realistic expectations of the treatment course and outcome. Patients and parents expect information on what awaits the patient in the near and distant future. The most demanding task for the clinician is to propose a sensible and feasible treatment plan with a lifelong perspective, based on biologic principles. Severe hypodontia or oligodontia, defined as the congenital absence of 6 or more teeth, is often complicated and requires an interdisciplinary approach at the specialist level, both during the initial evaluation phase and when treatment is provided. The prevalence of hypodontia in the Norwegian population has been reported to be 6.5%, with severe hypodontia affecting less than 0.2% of the general Norwegian and Danish populations.
Although a few studies have investigated hypodontia patients attending interdisciplinary clinics, the observation periods are generally limited. In addition, studies comparing the outcome of various treatment strategies in patients with severe hypodontia are yet to be performed. Hobkirk et al investigated 451 patients referred to a hypodontia clinic and reported missing teeth, spacing, and poor appearance as the most common complaints. Surprisingly, 40% reported “no complaints” related to their condition. The study did not, however, address treatment planning and outcome. A Danish study by Worsaae et al reported experience with a centralized interdisciplinary clinic, focusing on treatment planning and surgical treatment in 112 patients with oligodontia. At the end of the follow-up period (mean, 28 months; range, 1-68 months), 51 had finished treatment. The most common treatment options were orthodontic therapy (97%) and dental implants (90%). Shafi et al collected data retrospectively from the records of 108 patients attending a hypodontia clinic over a 5-year period. Most patients had a suspected family history of hypodontia. Orthodontic therapy was most frequently proposed in treatment planning (49%), and 21% were considered for dental implants. Almost 30% did not complete treatment. Dueled et al compared patients’ and professionals’ evaluations of implant-supported or tooth-supported reconstructions replacing congenitally missing teeth in 129 patients. The esthetic variables were considered acceptable for 92% of the implant-supported reconstructions and 83% of the tooth-supported prostheses. However, mucosal discoloration or visible metal on the buccal side was observed in 57% of the patients with dental implants. A positive correlation was observed between the professional and patient-based evaluations.
Because severe hypodontia is quite rare, opportunities for longitudinal studies with a sufficient number of patients are limited. Several studies dealing with hypodontia did not delineate patients with severe hypodontia as a separate subgroup, and most publications have been case reports or summaries of clinical experience. Consequently, evidence to support treatment decisions in complicated cases is insufficient.
The aims of this study were to compare the resulting crown and soft tissue morphologies of orthodontic space closure, dental implants, and tooth-supported fixed dental prostheses (FDPs) replacing teeth in the anterior region in patients with severe hypodontia. In addition, the treatment performed and the types and locations of substitutes for missing teeth were assessed.
Material and methods
A total of 212 patients with nonsyndromic hypodontia were referred between 1998 and 2010 for an evaluation by an interdisciplinary team at the University of Oslo in Norway. The patients were admitted for clinical and radiographic examinations, and a tentative treatment plan was determined by the specialist team. Patients residing within a practical distance to the university clinic were also offered to complete their entire treatment there. The remaining patients received treatment at their local dentist or specialist clinic.
Starting in March 2013, patients missing 6 or more teeth and aged 18 years or more were contacted by mail or telephone and invited to participate in a follow-up study of treatment outcome. The rationale for the chosen age cutoff was that patients 18 years or over could be expected to have completed the majority of the treatment course. A total of 71 patients met the inclusion criteria, of whom 50 (70%) agreed to take part in the study. Of those not attending, 5 could not be reached, 7 did not wish to participate in the study, and 9 declined for practical reasons. The mean age at inclusion was 25.6 years (range, 18-38 years), and the group consisted of 24 women and 26 men. Nine of the 50 patients were unable to travel to the University of Oslo, and the examinations were performed in cooperation with an orthodontist at the patient’s place of residence. Written information was given before the study, and informed consent was obtained from each participant. The patients were examined clinically, and panoramic radiographs and clinical photographs were taken.
Patient records from the time of first referral (mean age at referral, 13.9 years; range, 7-25 years) were retrieved, and the following information was noted: diagnosis, number and location of missing teeth, and recommended treatment plan.
The following parameters were recorded for all patients at the follow-up examination: number, location, and type of replacements (artificial or moved natural teeth); number and location of persisting deciduous teeth; and treatment performed. Crown and soft tissue morphology were compared for orthodontic space closure, dental implant fixtures (either single or part of an implant-retained prosthesis), and FDPs (tooth-supported conventional or resin-retained prostheses) replacing at least 1 missing tooth in the anterior region (canine to canine). This concerned 42 patients with a total of 187 teeth replaced by any of these 3 means: 97 in the maxilla and 90 in the mandible. The mean observation time from completion of treatment was 4.6 (0-11) years. The following morphologic measures were assessed objectively from standardized photographs for each replacement: mucosal discoloration, crown morphology, color of the replacement tooth, and papilla level.
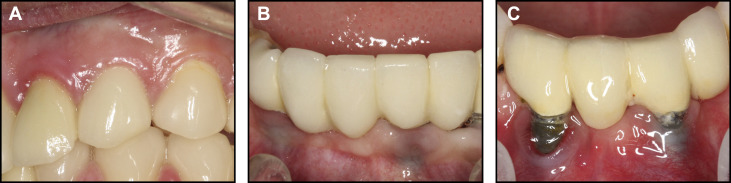
Mucosal discoloration in relation to the replacement tooth was scored as follows: 0, no mucosal discoloration; 1, grayish mucosal discoloration on the buccal side; 2, visible metal on the buccal side ( Fig 1 ). The crown morphology of the replacement tooth was evaluated as previously described by Dueled et al : ie, by comparison with the contralateral tooth or, if this tooth was missing, an ideal morphology for the tooth type in question. As a supplement, expected width-to-length ratios based on published data were considered. The following scoring system was used: 0 (match), the replacement tooth was optimal, with a close match to the natural or the ideal tooth; 1 (deviate), the replacement tooth deviated in at least 1 aspect from the natural or ideal tooth, but the overall impression remained acceptable; 2 (mismatch), the replacement tooth clearly deviated from the natural or ideal tooth, giving an unacceptable end result. The color of the replacement tooth was scored according to the following system, a modification of that described by Czochrowska et al : 0 (match), the replacement tooth appeared to match the shade and translucency of the contralateral tooth or, if this tooth was missing, the nearest natural neighboring tooth; 1 (deviate), the replacement tooth did not match the shade and translucency of the contralateral tooth or, if this tooth was missing, the nearest natural neighboring tooth, and the deviation was within the range of the patient’s tooth shades; 2 (mismatch), the replacement tooth did not match the shade and translucency of the contralateral tooth or, if this tooth was missing, the nearest natural neighboring tooth, and the mismatch was outside the range of the patient’s tooth shades and translucency. The papilla index was modified from the papilla index by Jemt and scored as follows: 0, a papilla corresponding to the original papilla, filling up the entire proximal space; 1, at least half of the height of the papilla was present; 2, less than half of the height of the papilla is present. For each replacement tooth, the papillae on both sides were scored, and the average of these scores was used for the replacement tooth in question.
All measurements were recorded by the same examiner (C.L.H.) after calibration. To evaluate measurement error, 50 replacement teeth were chosen at random and remeasured for each of the 4 morphologic measures, 6 weeks after the first measurement. Cohen kappa values were all above 0.7, indicating low measurement error.
Statistical analysis
Replacements in the maxilla and the mandible were analyzed separately. The replacements were classified into 3 categories: orthodontic space closures, dental implant fixtures, and FDPs. Analyzing the data with the individual tooth replacement as the unit of analysis would not be appropriate, since data from teeth belonging to the same patient are not independent. Instead, the patient was chosen as the unit of analysis; ie, measurements were aggregated by patient and type of replacement. For patients with more than 1 replacement of the same type, the mean of the morphologic score values was calculated and rounded to the nearest integer. When comparing 2 treatments in 2 separate patient groups, we used the chi-square test. When 1 patient had replacements from both categories being compared, we chose only the replacement type used more rarely, ensuring that the compared patient groups did not overlap.
A significance level of 5% was used, and the statistical analyses were carried out using SPSS software (version 22.0; IBM, Armonk, NY).
Results
In total, 571 teeth were congenitally missing among the 50 participants. The mean number of missing teeth per subject was 11.4 (range, 6-23).
The total number of sites with substitutes for a missing tooth was 488 distributed as follows: 216 with implant-supported prostheses (fixture or pontic), 45 with FDPs, 114 with a persisting deciduous tooth, 111 closed orthodontically or spontaneously, and 2 with autotransplantations ( Fig 2 ). In addition, 113 gaps remained without a tooth or replacement. In some cases, multiple interventions were necessary to replace 1 missing tooth: eg, orthodontically moving teeth into a favorable position followed by dental implant insertion.
Classifications of original treatment plans obtained from patient records are shown in Table I . At the follow-up examination, an assessment was made of whether the treatment had been carried out as planned. This was the case for most interventions, except for dental implants, which had not yet been performed in 13 patients.
| Treatment category | Treatment planned (n = 50, % of patients) | Not completed as planned (n) |
|---|---|---|
| Orthodontic appliance therapy | 46 (92%) | 3 |
| Implant-supported prosthesis | 48 (96%) | 13 |
| Retain deciduous tooth | 30 (60%) | 2 |
| Composite restoration | 15 (30%) | – |
| Tooth-supported FDP | 18 (36%) | 3 |
| Veneer restoration | 10 (20%) | 2 |
| Orthognathic surgery | 5 (10%) | 2 |
| Autotransplantation | 1 (2%) | – |
When we compared implant fixtures with orthodontic space closure ( Table II ), implant fixtures scored poorer for mucosal discoloration and the papilla index, and the differences were statistically significant. All implant fixtures in the anterior mandible and 60% in the anterior maxilla had either mucosal discoloration or visible metal. Likewise, when implant fixtures were compared with FDPs ( Table III ), a significantly more pronounced mucosal discoloration was recorded for the fixtures in both jaws. The crown morphology in the anterior mandible was significantly better for the FDPs than the implant fixtures, but the color score was better with an implant fixture than an FDP in the anterior maxilla. For both dental fixtures and FDPs, poor papilla index scores were observed. When we compared space closure with FDPs ( Table IV ), a significantly better papilla index was observed for space closure in both jaws. The crown morphology in the anterior mandible was considered significantly better for the FDPs.
| Anterior maxilla | Anterior mandible | |||
|---|---|---|---|---|
| Implant fixture n (%) |
Orthodontic space closure n (%) |
Implant fixture ∗ n (%) |
Orthodontic space closure n (%) |
|
| Mucosa | ||||
| 0 | 8 (40%) | 11 (100%) | – | 7 (100%) |
| 1 | 7 (35%) | – | 3 (27%) | – |
| 2 | 5 (25%) | – | 8 (73%) | – |
| P <0.01 | P <0.01 | |||
| Crown | ||||
| 0 | 5 (25%) | 4 (36%) | – | 1 (14.5%) |
| 1 | 12 (60%) | 6 (55%) | 11 (92%) | 5 (71%) |
| 2 | 3 (15%) | 1 (9%) | 1 (8%) | 1 (14.5%) |
| NS | NS | |||
| Color | ||||
| 0 | 15 (75%) | 8 (73%) | 7 (58.3%) | 6 (86%) |
| 1 | 5 (25%) | 3 (27%) | 4 (33.3%) | 1 (14%) |
| 2 | – | – | 1 (8.3%) | – |
| NS | NS | |||
| Papilla | ||||
| 0 | 7 (35%) | 10 (91%) | – | 6 (86%) |
| 1 | 8 (40%) | 1 (9%) | 6 (50%) | 1 (14%) |
| 2 | 5 (25%) | – | 6 (50%) | – |
| P <0.01 | P <0.01 | |||
∗ For 1 implant fixture, the gingival margin was not visible on the photographs; this patient was not scored for mucosal discoloration.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


