Fig. 13.1
Clinical photograph showing a “high” left lingual nerve which was injured during extraction of tooth #17, requiring external neurolysis of the nerve
When evaluating patients with LN injuries, the microsurgeon must be prepared for potential patient frustration and anxiety that often accompany these injuries. Patients will question whether it was poor surgical technique or the nature of their anatomy or pathology that contributed to their neurosensory deficit. For instance, in the case of the inferior alveolar nerve (IAN), it is standard of care for most surgeons to obtain a preoperative panoramic radiograph that enables visualization of the course of the inferior alveolar canal (IAC) and its proximity to the area of surgical interest. There are statistically validated radiographic signs that indicate increased risk of IAN injury [11]. If there is radiographic evidence of potential for nerve injury, the surgeon has the option to obtain a preoperative computed tomography (CT) scan or cone beam CT (CBCT). With this technology, the surgeon is able to better visualize the course of the IAC in preoperative planning of extraction of impacted teeth, placement of dental endosseous implants, evaluation of jaw lesions, and designing jaw osteotomies. A major additional advantage of CT is that it allows the surgeon to better educate the patient regarding the potential risk of injury to the IAN and preparing the patient for such an event should it occur. However, with regard to the LN, no practical imaging modality exists for the visualization of the LN and its course other than possibly high-resolution MRI scans. Therefore, the combination of the variant course of the LN and lack of easily obtainable and reproducible imaging of the nerve makes the planning for potential LN injuries more difficult as well as postoperative discussions with patients regarding this potential complication should it occur.
The evaluation and surgical management of patients with LN injuries is a challenging task that requires a sound treatment philosophy based upon experience with careful outcome analysis to refine surgical procedures in order to maximize patient benefit. This chapter shall discuss the anatomy of the LN, microsurgical treatment options, and present a case series.
13.2 Surgical Anatomy
The trigeminal nerve is the fifth and largest cranial nerve that is considered a mixed motor and sensory nerve. The afferent (sensory) component provides general sensation to the skin of the face, teeth, oral cavity, and tongue. The efferent (motor) component provides innervation to the muscles of mastication and other cranial muscles. The ophthalmic (V1) and maxillary (V2) divisions carry only sensory nerves, while the mandibular division (V3) carries both sensory and motor nerves. The LN is a branch of the mandibular division of the trigeminal nerve, and it is formed from afferent branches from the body of the tongue that travel along the lateral surface of the tongue and finally the posterior floor of mouth [1].
As the LN descends into the oral cavity, it is located medial to the mandibular ramus, coursing superior to Wharton’s duct. An understanding of the relationship of the LN to the adjacent Wharton’s duct is critical during a transoral exploration of the floor of the mouth. The LN courses from lateral to medial, and crosses Wharton’s duct in the area of the first and second molars, and lateral to the hypoglossal nerve. Once the LN loops around Wharton’s duct, it then passes upward onto the genioglossus muscle as it enters the substance of the tongue. The position of the LN at the third molar region is dependent upon the flare of the mandible, but generally courses below the lingual alveolar crest and several millimeters medial to the lingual cortex. As described previously, this is an area of anatomic variability that can make the LN susceptible to injury during third molar surgery regardless of the specific surgical technique utilized.
13.3 Indications for Surgical Management
The key to accurate repair of LN injuries is establishing a precise diagnosis. During the initial examination, the surgeon must establish the nature of the sensory disturbance including the affected area, degree of sensory deficit, and presence or absence of any neuropathic pain component [4]. Indications for LN microsurgery are generally accepted to include (1) observed nerve transection, (2) development of pain due to nerve entrapment, (3) no improvement in spontaneous sensory regeneration for greater than 3 months, (4) progressively worsening hypoesthesia or dysesthesia, and (5) hypoesthesia that is intolerable to the patient and amendable to surgical improvement. Of note, some patients seek microsurgical intervention for mild sensory deficits that would not be significantly improved to warrant surgical exploration considering the potential risks of general anesthesia [12]. Contraindications to LN microsurgery can include any of the following scenarios: (1) clinical evidence of spontaneous improving neurosensory function, (2) development of central neuropathic pain, (3) a level of hypoesthesia that is acceptable to the patient, (4) severely medically compromised patient unable to tolerate general anesthesia, and (5) excessive time elapsed since the initial injury based upon current understanding of timing issues as they relate to trigeminal nerve microsurgery [12, 13].
13.4 Surgical Approach and Techniques
Operating magnification is recommended for dissection and mobilization of the proximal and distal portions of the LN, with nasal endotracheal intubation and muscle relaxation to enable unhampered access to the oral cavity to facilitate intraoral surgery. Once the endotracheal tube is secured, a properly sized pharyngeal pack is placed and the patient’s oral cavity is subsequently prepped with 0.12 % chlorhexidine solution or other such solution. The patient is prepped and draped in a sterile fashion consistent with other oral surgical procedures. It is helpful if the patient is placed in slight reverse Trendelenburg position which facilitates venous drainage and results in less intraoperative bleeding. Mouth opening can be accomplished with a rubber bite block or a Molt mouth gag with silicone tips. One must consider undue stress on the temporomandibular joint during these procedures, which can last up to several hours, especially in cases where extensive dissection is needed to identify the proximal and distal portions of the nerve; therefore, the mandible should not be maintained in a fully open position for the duration of surgery [4]. Finally, a local anesthetic with vasoconstrictor is injected in the operative site, allowing adequate time to ensure adequate vasoconstriction. Of note, nerve blocks should be avoided under general anesthesia due to risk of accidental intraneural injection with the patient being unable to respond to this incident resulting in possible additional chemical or mechanical injury to the LN or IAN.
Exploration and repair of the LN can generally be accomplished with a transoral approach using either a paralingual mucosal incision or lingual gingival sulcus incision (Fig. 13.2). The advantages of the paralingual mucosal incision is the direct visualization of the LN it provides with a smaller incision; however, the proximal and distal nerve trunks may have a tendency to retract from the surgical field on exposure and blunt dissection for complete injuries. The lingual gingival sulcus incision requires a larger incision with both distobuccal release and lingual crevicular incision; however, this will not result in retraction of the nerve during surgical dissection or retraction. Furthermore, the lingual gingival sulcus incision is technically more familiar to surgeons with the elevation of a subperiosteal flap that requires a lateral release along the external oblique ridge similar to an extended incision utilized for third molar surgery with extension along the lingual sulci of posterior teeth to approximately the area of the canine tooth. With the lingual gingival sulcus incision, one must handle the gingival tissues gently to prevent gingival recession and/or loss of interdental papilla, especially distal to the second molar, if present, that could result in potential gingival recession and root sensitivity. This flap is then gently elevated in a subperiosteal plane to allow placement of a lateral retractor, preferably an Obwegeser toe-out retractor, and lingual retraction by the assistant with consideration for placement of silk suture to the contralateral rubber bite block to allow passive lingual flap retraction. This surgical approach allows for close inspection of the alveolar ridge and residual dental socket, if applicable. In particular, the microsurgeon should observe the level of the lingual alveolar crest, integrity of the lingual plate, presence of perforations from rotary instrumentation, or any other bony irregularities. These pertinent positive or negative intraoperative findings should be included in the final operative dictation report. In some instances, the surgeon may find a lingually oriented residual socket where the bony lingual ridge was obliterated by the former dental crown of the third molar tooth. This is very relevant in describing the position of the LN relative to where the ridge might have been anticipated if not for the aberrant position of the impacted tooth.
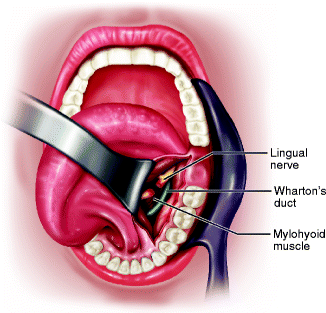

Fig. 13.2
Dashed line depicting transoral approach to lingual nerve using a paralingual mucosal incision, and straight line depicting a lingual gingival sulcus incision (Must Redraw Picture with Tongue Retracted Away from Incision Design)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


