We read with great interest the article entitled: ‘Multiple squamous cell carcinoma of the oral cavity in a young patient with graft-versus-host disease following allogenic bone marrow transplantation’, by M ontebugnoli et al. . The authors described a rare case of oral squamous cell carcinoma (OSCC) involving a patient receiving bone marrow transplantation for beta thalassemia, who had suffered from graft-versus-host disease (GVHD), highlighting the association between oral GVHD and OSCC. It is intriguing that their patient developed multiple OSCC 17 years after hematopoietic stem cell transplantation (HSCT). This case is of particular interest since we encountered a similar transplanted patient with oral GVHD who developed OSCC 11 years after HSCT during close follow-up.
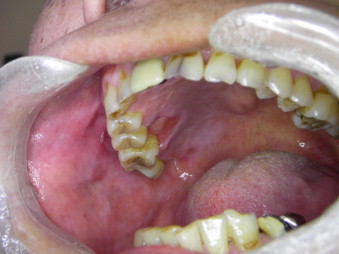
In May 2011, a 61-year-old man with oral GVHD presented at a regular 3-month follow-up and complained of soreness and discomfort of the right maxilla. An oral clinical examination revealed an ulcerated lesion, 10 mm × 25 mm in size, involving the palatal gingiva with indulation ( Fig. 1 ). An incisional biopsy was performed and the specimen demonstrated invasive squamous cell carcinoma histopathologically. On his right palatal gingival, slight lichenoid lesions were still observed. The final staging of the tumour was T2N0M0, and the patient was treated with wide surgical excision of the lesion.
The patient’s medical history was significant for allogenic HSCT from an HLA-matched sibling in March 2000 as treatment for acute lymphoblastic leukaemia.
The conditioning regimen included cyclophosphamide and total body irradiation. The patient received short-term cyclophosphamide and tacrolimus hydrate for postransplant prophylaxis against GVHD, and then continued to receive tacrolimus hydrate. After transplantation, the patient had been seen at our clinic on a 3-week basis for oral evaluation. In January 2001, a follow-up examination detected bilateral red and white lichenoid-type lesions of the bucco-palatal gingival. Hyposalvation was evident. An incisional biopsy of the right palate was performed, and the specimen demonstrated lichenoid changes histopathologically . At that time, a diagnosis of oral chronic GVHD was made. Although the patient did not complain of oral symptoms and no topical therapy was carried out, he had been treated with tacrolimus hydrate until March 2001. The patient had been seen on a monthly basis until April 2002, when the lichenoid lesions and hyposalvation improved. Since then, the patient had been seen every 3 months at our clinic for oral GVHD until he developed oral cancer.
Previous studies have shown that HSCT recipients are at a significantly higher risk of developing secondary cancers than the general population, with a more than 10-fold higher incidence of oral cancer . M ontebugnoli et al. emphasized the relationship between the presence of oral GVHD and devolvement of oral cancer in an HSCT patient . In fact, a review of the literature demonstrated that 15 of the 17 reported cases developing oral sqaumous cell carcinoma in HSCT patients had oral GVHD . Furthermore, according to the literature, the development of secondary solid tumours peaks between 8 and 9 years after HSCT . On the other hand, the case of Montebugnoli et al. developed OSCC 17 years after HSCT. In our case, the patient developed OSCC 11 years after HSCT.
These findings strongly suggest the high-level susceptibility of HSCT patients with oral GVHD to OSCC, and the uncertain time elapsing between HSCT and the development of OSCC. All patients treated with HSCT, particularly those developing GVHD, should therefore undergo a careful examination of the oral mucosa and be closely followed up by physicians long term, with the aim of identifying the onset of secondary tumours as early as possible.
Funding
None.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


