Key points
- •
The complexity of the revisional facelift or neck lift is directly related to the way the primary procedure was performed.
- •
With so many techniques available to facial cosmetic surgeons, such as subcutaneous facelift, variations of superficial musculoaponeurotic system (SMAS) or extended SMAS procedures, lateral SMASectomy, deep plane and composite ryhtidectomy, subperiosteal facelift, and short scar facelifts, the revisional procedure should be directed to the specific problems that patients exhibit, such as laxity in the upper face, laxity in the neck, jowling, or deepening of the nasolabial folds.
- •
Generally, it is more prudent to restore contour within the deep layer support by the elevation of the SMAS and platysma rather than by rotating skin flaps in an exaggerated manner in a cephalad direction producing a tight unnatural look.
- •
It is extremely important that the posterior hairline and the temporal hairline are correctly aligned at the time of closure.
In the past two decades, cosmetic surgery has become more common and accepted. Facelift and neck lift procedures can be routinely viewed on the Internet or television. With easy access to information and reality shows demonstrating success stories, there has been an increase in demand for these procedures. This increase has given rise to a new generation of patients who have undergone a facelift or a neck lift procedure and, because of the continued effects of aging or residual signs of aging that have not been addressed in a primary procedure, request a secondary operation.
When performing a secondary facelift or neck lift, surgeons need to consider the effects of the primary procedure on the tissues. Despite variations in technique of performing a face lift or a neck lift, the factors that need to be considered when performing a secondary procedure are the same:
- •
Previous incision placement and resulting scars
- •
Amount of skin laxity
- •
Earlobe deformity
- •
Hair pattern changes
- •
Fat irregularities and deficiencies
- •
Fascial laxity leading to deep nasolabial folds and jowls
- •
Cervicomental angle obtusity
- •
Platysmal laxity and banding
- •
Presence of unusual rhytids
- •
The time that has elapsed from the original surgery
- •
Complication associated with secondary/tertiary procedures
Most patients requesting secondary facelifts or neck lifts have some form of laxity and want to improve or maintain their facial appearance. In addition, most of the patients seeking secondary facelifts are older in age and often have other ailments concomitant with aging. Therefore, the preoperative assessment should include a thorough medical history and physical examination. This assessment should include a history of over-the-counter and herbal medicines, because many of the patients who seek a secondary facelift or neck lift take herbal medicines with potential ill effects on surgery. For example, Ginkgo biloba and testosterone can potentially induce hypertension. Many of the herbal products are blood thinners and can affect the coagulation cascade, such as Ginkgo biloba, garlic tablets, ginger, St. John’s wort, and ginseng. Omega-3 fatty acids may also affect the coagulation cascade and additionally may be related to delaying acute wound healing. The authors recommend that patients stop all herbal preparations for at least 2 weeks before and after surgery. When necessary, appropriate referrals to a primary care physician, cardiologist, or other specialist should be made to obtain a clearance and minimize risk of perioperative complications.
In general, the authors’ approach to a secondary procedure is the opportunistic approach and is tailored to patient needs and existing anatomy. Patients present with different skin thicknesses and elasticity, variable amount of subcutaneous tissue, variable amounts of laxity and thicknesses of the superficial fascia, and variable amounts of scarring from primary facelift or neck lift. When evaluating patients, surgeons should look for residual signs of aging that have not been addressed in the primary procedure. It is not uncommon to see a patient who has had a facelift seeking a secondary procedure and on examination most of the laxity is concentrated in the upper face and periocular region, which was not addressed in the primary surgery ( Fig. 1 ). During the secondary facelift, the surgeon can and should address those areas to achieve the best possible result.
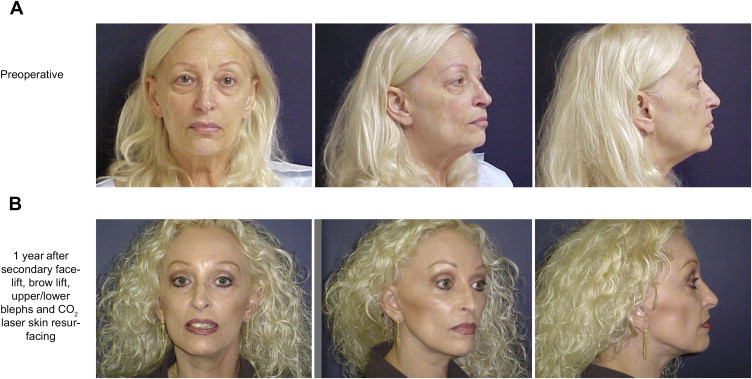
Generally, most patients seeking a secondary procedure have their skin envelope tightened with the primary procedure; therefore, little skin needs to be removed in the secondary procedure. Alternatively, their SMAS and the muscles in the neck are commonly lax compared with the tightened skin envelope. In recent years, the popularity of various forms of short scar facelifts has given rise to an increasing number of patients with this presentation.
Because most of the primary facelifts performed do not involve an extensive sub-SMAS dissection, the secondary facelift benefits from some form of SMAS undermining and tightening. The subcutaneous layer, which is the most common plane of dissection in a facelift, may be thinner after the trauma of the original procedure and facial fat atrophy, creating a challenge in thin patients. In these cases, it may be more prudent to perform a SMASectomy with plication rather than an SMAS elevation.
Incisions and scars
Incision placement during a secondary procedure is largely dictated by the incision line made during the first operation. The authors’ preference is to make a tragal margin incision or a retrotragal incision because it is easier to hide the scar and the scar heals well. In male patients, a pretragal incision may be optimal to prevent transposing hair-bearing skin over the tragus, or laser hair removal can be performed in the area in the future. Before making the incision, careful assessment of the amount of skin laxity present should be made, and, if enough laxity is present, a preauricular incision can be converted to a tragal or retrotragal incision during the reoperation ( Fig. 2 ). On closure of the flap, there should be minimal tension on the tragus. To minimize tension, the skin flap is sutured above and below the tragus with 4-0 Monocryl sutures.
Incisions and scars
Incision placement during a secondary procedure is largely dictated by the incision line made during the first operation. The authors’ preference is to make a tragal margin incision or a retrotragal incision because it is easier to hide the scar and the scar heals well. In male patients, a pretragal incision may be optimal to prevent transposing hair-bearing skin over the tragus, or laser hair removal can be performed in the area in the future. Before making the incision, careful assessment of the amount of skin laxity present should be made, and, if enough laxity is present, a preauricular incision can be converted to a tragal or retrotragal incision during the reoperation ( Fig. 2 ). On closure of the flap, there should be minimal tension on the tragus. To minimize tension, the skin flap is sutured above and below the tragus with 4-0 Monocryl sutures.
Earlobe deformity
Another common stigmata of facelifts is the bat ear or pixie ear deformity ( Figs. 3 and 4 ). This deformity is a result of poor incision placement and excess skin removal caudal to the ear lobe during closure of the primary procedure. The closure of the earlobe cannot be under tension. The deeper structures of the jaw line and neck should be secured to a stable structure, such as the postauricular fascia or the mastoid fascia, and the skin should be closed passively around the earlobe. To correct this deformity, surgeons should incise the earlobe to a more rounded appearance and then inset the earlobe to its proper position. Hanging the cheek on the earlobe during flap redraping should never be attempted. Instead, the skin flap should be secured to the base of the ear lobe with a 3-0 Monocryl or 3-0 Vicryl suture. The skin of the earlobe is then closed with a 4-0 Monocryl suture in a running subcuticular fashion under minimal tension (see Figs. 3 and 4 ).
Hair pattern changes
One of the greatest challenges with incision placement in revisional facelift or neck lift is problems with hairline shifting and bald spots from the primary operation. Another common stigma of facelifts is distortion or the loss of sideburn and temporal hairline. This problem can occur when the cervicofacial flap is advanced too far in the cephalad direction, causing the hairline shift. For example, transposition of the sideburn above the helical rim can leave a bald spot above the ear. This problem is difficult to correct. It is occasionally possible to rotate the temporal hairline inferiorly and partially lower the sideburn. As is commonly the case, avoidance of this problem is the best course of action.
The authors prefer to make the temporal incision in the hairline at the initial procedure and leave the sideburn or 1 cm of hair-bearing skin attached at the base of the helix. This method avoids improper transposition of hair in the temporal region. If skin needs to be removed at that location, it is done in a conservative fashion, bearing in mind not to shift the temporal hairline. Another alternative for correction of this problem is to place the incision along the temporal hairline in the secondary procedure and avoid any additional hairline shifting at the time of flap advancement.
In the postauricular region, there is a potential for visible scars when the incision in the primary procedure was made along the posterior scalp hairline. This scar can become wide and more visible when the neck tissues are suspended to the postauricular scalp skin as opposed to the deeper scalp structures. In the revisional procedure, surgeons have an opportunity to remove some of or the entire scar as long as enough laxity is present. It is the authors’ preference to make the new incision in the hairline cephalad to the old scar in a line that is perpendicular to the vector of pull. If the incision is made in a beveled manner and the dissection is made in a plane to avoid damage to the hair follicles, this incision heals so well that it is almost invisible a year later when the hairs have grown into the scar. When advancing the posterior cervical skin flap in a cephalic direction, the authors place 1 or 2 deep permanent sutures (2-0 Ethibond or Neurolon [Ethicon, San Angelo, Texas]) that secure the deep portion of the skin flap to the deep posterior scalp fascia and/or the periosteum ( Fig. 5 , [CR] ). The excess skin and the old scar are then trimmed, and the incision is closed with staples passively under no tension. Care is taken to align the posterior hairline during closure (see Fig. 5 , [CR] ).




