Abstract
The aim of this study was to evaluate the hard and soft tissue changes after pre-arthroplasty simultaneous maxillomandibular distraction osteogenesis for the correction of post-ankylotic dentofacial deformities. This prospective study included 10 patients with unilateral temporomandibular joint (TMJ) ankylosis who presented with a facial deformity and a maxillary cant. Informed patient consent was obtained for participation. Simultaneous maxillomandibular distraction was planned based on clinical and radiographic examinations. A horizontal mandibular osteotomy was performed in the ramus and the distractor device was fixed. A bilateral Le Fort I osteotomy was then performed and a four-hole straight plate was fixed on the contralateral zygomatic buttress to act as a fulcrum. After a latency period of 5 days, the distractor was activated twice daily by 0.5 mm until the required vertical lengthening was achieved. Intermaxillary fixation was maintained during the entire distraction period. After a consolidation period of 8–12 weeks, the distractor was removed. The TMJ ankylosis was released and a temporal fascia interpositional arthroplasty was performed as second surgery, along with a genioplasty if needed. All patients were followed up for a period of 12–24 months. A marked improvement in the facial asymmetry was noted in all cases. The occlusal cant and mandibular retrusion improved satisfactorily, and the average postoperative inter-incisal opening was 35.6 mm. Pre-arthroplasty simultaneous maxillomandibular distraction offers a good treatment outcome, as it allows improvements in facial aesthetics as well as function.
Temporomandibular joint (TMJ) ankylosis is a joint disorder caused by bony or fibrous adhesion of the anatomical joint components. The most common cause of TMJ ankylosis is trauma (13–100%), followed by local or systemic infection (0–53%) and systemic diseases such as ankylosing spondylitis, rheumatoid arthritis, and psoriasis (28%); it may also occur after any TMJ surgery. TMJ ankylosis not only limits mouth opening and chewing, but may also affect the growth of the mandible as well as the maxilla. When it occurs in children, it can cause secondary dentofacial deformities leading to psychological problems such as low self-esteem and an inferiority complex.
Post-ankylotic facial deformities include micrognathia, reduced facial height, poor jaw–neck definition, chin shift to the affected side, and occlusal discrepancies. In unilateral cases, a cant of the occlusal plane is frequently observed due to mandibular hypoplasia on the affected side, and hence a secondary ipsilateral vertical deficiency in the maxilla. The management of these dentofacial deformities due to TMJ ankylosis remains a challenge for surgeons and a series of operations is often required.
In 1905, Codvilla described distraction osteogenesis as an effective technique for lengthening the mandible. Lopez and Dogliotti stated that they preferred to restore the jaw movements first and address the secondary facial deformities later in paediatric patients with TMJ anklyosis. In contrast, Ortiz-Monasterio et al. and Cho et al. recommended simultaneous bimaxillary distraction osteogenesis using external devices in patients with hemifacial microsomia for the correction of facial asymmetry. Others have advocated simultaneous mandibular distraction and arthroplasty in such patients, but have reported an unstable proximal condylar segment as a remaining problem during the distraction process. Sadakah et al. evaluated the feasibility of transoral bimaxillary distraction osteogenesis before releasing TMJ ankylosis using intraoral mandibular distractors in nine patients and found this to be a feasible and perhaps advantageous technique.
The aim of the present study on post-ankylotic facial deformity was to assess the feasibility of pre-arthroplasty bimaxillary distraction osteogenesis to correct the deformity and also to evaluate the hard and soft tissue changes.
Materials and methods
Ten patients with unilateral TMJ ankylosis presenting with a facial deformity and maxillary cant, ranging in age from 15 to 35 years, were included in this study ( Fig. 1 ); institutional ethics clearance was obtained prior to recruitment. The diagnosis of TMJ ankylosis was based on clinical and radiographic evidence, including a computed tomography (CT) scan. Patients with bilateral TMJ ankylosis, recurrence, who were medically compromised, and those not consenting to surgery were excluded. All patients were informed about the surgical procedure and possible complications, and consent for the treatment was obtained and recorded. All patients were operated on by a single surgeon. A two-stage surgical protocol was followed: the first stage comprised a unilateral mandibular osteotomy with fixation of the distractor device to the ramus and a complete Le Fort I osteotomy, with intermaxillary elastics maintained during the distraction phase; the second stage comprised osteoarthrectomy and a temporal fascia interpositional arthroplasty, which were performed later with removal of the distractor, and a genioplasty if needed.

Preoperative clinical assessment included evaluations of facial aesthetics, function, and occlusion. Panoramic radiographs and CT scans were used to determine the extent of the ankylotic mass and for surgical planning. Radiological evaluation was based on postero-anterior (PA) and lateral cephalograms ( Fig. 2 a–e) .

The vertical and transverse positions of the mandibular angles were assessed by constructing the mandibular triangle on a PA cephalogram using sphenofrontal junction (SF) (where the smaller wing of the sphenoid crosses the medial orbital ridge), M (the inferior-most point on the mastoid bone), gonion (Go; the inferior-most posterior point at the angle of the mandible), cranial base plane (C-plane), occlusal plane, and C (midpoint of the C-plane where geometric midline (GM) crosses) ( Fig. 3 a ). The height of the mandibular ramus was measured as the distance between M and Go. Occlusal cant (°) was measured by the angle formed between the occlusal plane and true horizontal plane. The mandibular triangle was constructed by connecting C–Go–Go bilaterally. The lengths of C–Go were evaluated and GM–Go was compared on both sides to assess the transverse discrepancies ( Fig. 3 a).

The parameters used to observe angular changes were sella–nasion–A-point (SNA), sella–nasion–B-point (SNB), nasolabial angle, and facial convexity angle. Changes in the position of various hard tissue points of the maxilla (anterior nasal spine (ANS), A-point, upper incisor edge (U1E)) and mandible (lower incisor edge (L1E), B-point, pogonion (Pog)), and their corresponding soft tissue points (pronasale (Pn), subnasale (Sn), labrale superior (Ls), labrale inferior (Li), inferior labial sulcus (Si), and soft tissue pogonion (Pog′)), were assessed on lateral cephalograms from the reference in horizontal and vertical planes ( Fig. 3 b). The surgical plan for distraction is demonstrated in Fig. 3 c.
First surgery
All procedures were performed under general anaesthesia. Using a submandibular approach, the vertically deficient mandibular ramus was exposed and the planned osteotomy line was made perpendicular to the lower border of the mandible. A suitable distractor was fixed temporarily in the desired position and then removed prior to completing the mandibular osteotomy. Care was taken not to damage the inferior alveolar nerve. The distractor was then finally fixed, after which it was activated to check for function and then deactivated before closure of the wound ( Fig. 4 a) .

An intraoral maxillary vestibular incision was then made from first molar to contralateral first molar and a sub-periosteal dissection was done to expose the piriform aperture, anterior maxilla, and zygomatic buttress. A complete Le Fort I osteotomy was performed and down-fractured. The maxilla was then gently mobilized and a four-hole titanium straight plate was fixed on the contralateral zygomatic buttress to act as a fulcrum for the maxillary unit ( Fig. 4 b). The wounds were then closed and the patient was placed in intermaxillary fixation (IMF) for the entire distraction period. The mandibular distractor was activated after a latency period of 5 days, twice daily by 0.5 mm.
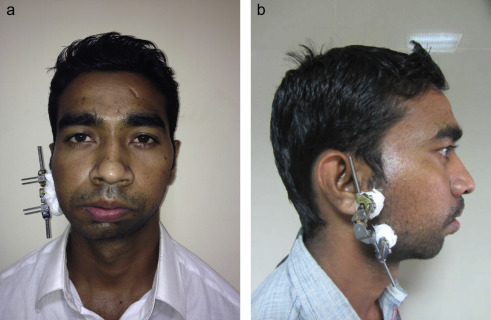
The distractor was activated by the surgeon in the outpatient clinic until the maxillary cant was corrected and the gonial angles were positioned at the same level horizontally ( Fig. 5 a, b ). An overcorrection of 2–3 mm was achieved to compensate for any later relapse. After a consolidation period of 8–12 weeks, and when the existence of new bone was confirmed radiographically, the patient underwent the second surgery ( Fig. 6 a, b ).

Second surgery
A standard Al-Kayat and Bramley incision was made over the temporal region and a layer-wise dissection done to expose the temporalis fascia. A 45-degree incision was made through the superficial layer of the temporalis fascia starting near the root of the zygoma and continued upwards. The ankylosed mass was exposed and the anterior and posterior limits of the mass were identified with the help of a periosteal elevator. An inferior osteotomy cut was made with an oscillating saw to the full depth of the bone. After completion of the inferior cut, a superior cut was made 10–15 mm above the inferior cut and the bony mass was released. Considering that aggressive resection of the ankylotic bone may result in some changes in the position of the mandible and occlusion, the condylar head was reconstructed using a hydroxyapatite collagen scaffold to maintain the vertical height. A temporalis fascia flap was then raised and used as interposition material. A suction drain was inserted and layer-wise closure was done ( Fig. 7 ). All patients were followed for a period of 12–24 months: clinical examinations of mouth opening and aesthetic correction ( Fig. 8 a–d) and radiographic examinations for any recurrence or relapse were performed. The results were analyzed statistically. The paired t -test was used to assess differences between pre- and postoperative values.


Results
With regard to the results of the clinical observations for facial aesthetics and function achieved, the distraction attained met the surgical plan in all cases and the distraction process was uneventful and successful. The facial asymmetry and occlusal canting improved satisfactorily in all cases, with restoration of the lip midline and centralization of the chin ( Tables 1 and 2 ).
| Case No. | Age (years) | Sex | TMJ ankylosis (side) | Type | MO (mm) | Ramus height a , Ipsi., mm | Ramus height a , Contra., mm | Distraction required, mm | C–Go Ipsi., mm | C–Go Contra., mm | GM–Go Ipsi., mm | GM–Go Contra., mm | Occlusal cant b ,° |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 18 | M | Right | III | 10 | 25 | 28 | 3 | 104 | 113 | 40 | 54 | 8 |
| 2 | 20 | M | Left | IV | 8 | 22 | 28 | 6 | 98 | 111 | 45 | 53 | 10 |
| 3 | 17 | F | Right | III | 8 | 26 | 29 | 3 | 96 | 106 | 38 | 54 | 6 |
| 4 | 18 | M | Right | III | 5 | 24 | 29 | 5 | 94 | 109 | 36 | 48 | 8 |
| 5 | 15 | M | Left | IV | 2 | 23 | 28 | 5 | 92 | 102 | 39 | 52 | 7 |
| 6 | 25 | M | Left | IV | 2 | 24 | 29 | 5 | 105 | 114 | 41 | 54 | 9 |
| 7 | 23 | F | Right | III | 6 | 26 | 29 | 3 | 102 | 112 | 38 | 60 | 8 |
| 8 | 35 | M | Left | IV | 2 | 25 | 28 | 3 | 100 | 115 | 36 | 61 | 10 |
| 9 | 20 | M | Left | IV | 2 | 23 | 28 | 5 | 98 | 110 | 40 | 53 | 7 |
| 10 | 28 | M | Left | III | 5 | 24 | 27 | 3 | 104 | 115 | 39 | 52 | 8 |
| Mean | 22 | 5 | 24.2 | 28.3 | 4.2 | 99.3 | 110.7 | 39.2 | 54.1 | 8.1 | |||
| SD | 6.05 | 2.98 | 1.32 | 0.67 | 1.14 | 4.47 | 4.16 | 2.61 | 3.81 | 1.29 | |||
| P -value | <0.05 | <0.05 | <0.05 | ||||||||||
a Ramus height: distance between M and Go.
b Occlusal cant: angle between occlusal plane and true horizontal plane.
| Case No. | MO (mm) | Ramus height a , Ipsi., mm | Ramus height a , Contra., mm | C–Go Ipsi., mm | C–Go Contra., mm | GM–Go Ipsi., mm | GM–Go Contra., mm | Occlusal cant b ,° |
|---|---|---|---|---|---|---|---|---|
| 1 | 40 | 30 | 29 | 116 | 115 | 47 | 47 | 0 |
| 2 | 39 | 29 | 30 | 110 | 112 | 50 | 49 | 0 |
| 3 | 36.5 | 30 | 29.5 | 105 | 106 | 46 | 45 | 1 |
| 4 | 37 | 29 | 30 | 110 | 110 | 42 | 42 | 0 |
| 5 | 28 | 28 | 28.5 | 106 | 104 | 45 | 44 | 0 |
| 6 | 34 | 29 | 30 | 116 | 115 | 47 | 48 | 1 |
| 7 | 36.5 | 30 | 30 | 114 | 114 | 49 | 50 | 0 |
| 8 | 34.8 | 29 | 29 | 115 | 116 | 49 | 49 | 2 |
| 9 | 31 | 27 | 29 | 110 | 110 | 46 | 47 | 0 |
| 10 | 39.2 | 28 | 29 | 116 | 115 | 46 | 46 | 0 |
| Mean | 35.6 | 28.9 | 29.4 | 111.8 | 111.7 | 46.7 | 46.7 | 0.4 |
| SD | 3.79 | 0.99 | 0.57 | 4.18 | 4.13 | 2.31 | 2.49 | 0.7 |
| P -value | <0.05 | >0.05 | >0.05 | >0.05 | <0.05 | |||
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


